Background:
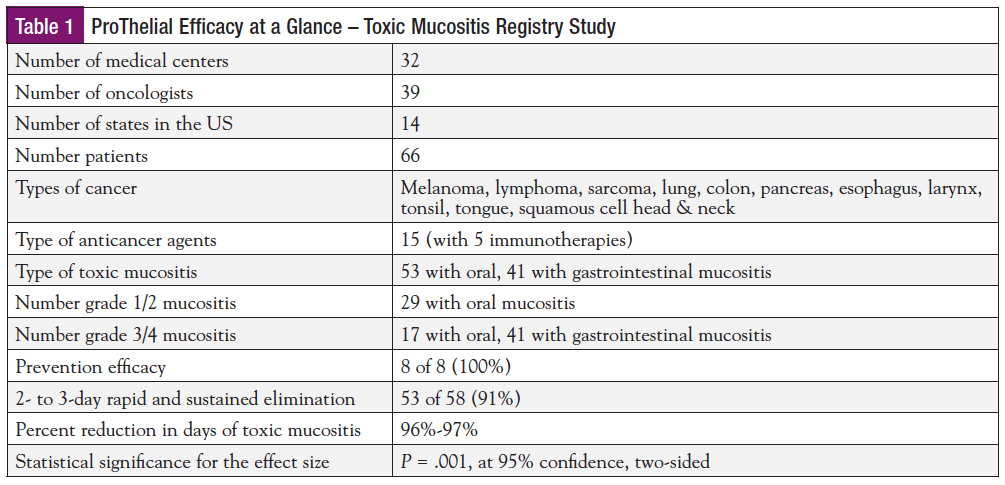
Of the 1.6 million individuals annually diagnosed with cancer, at least 522,166 received chemoradation, with 234,975 developing toxic mucositis and 20% dying within 5 years due largely to mucositis-associated unplanned treatment breaks. In a mucositis registry study of 66 consecutive patients undergoing chemoradiation using 2 different radiation protocols, 5 targeted immunotherapies and 8 nontargeted chemotherapies by 39 oncologists in 32 institutions across 14 states in the United States, high-potency polymerized cross-linked sucralfate (HPPCLS) was prescribed for prevention in 8 patients and for reversal in 58 patients (48 males, 18 females, aged 14-96 years). All 8 patients treated for prevention, 53 patients treated for reversal, with 5 patients lost to follow-up, entered into data analysis. Primary outcomes of patient-reported mouth/throat soreness, clinician-observed WHO grade mucositis, and EORTC/RTOG oral and gastrointestinal mucositis were assessed at days 1, 2, 3, 4, and 7 of use of HPPCLS and at the close of cancer treatment. All 8 patients scheduled for G-tube and expected to develop mucositis never developed mucositis and did not require G-tube placement. All 53 patients had 2- to 3-day elimination of mucositis, sustained throughout treatment as assessed by both primary outcome measures.Objective:
Assess the significance of the HPPCLS data through a statistical analysis of treatment effect compared with historical controls of 351 patients experiencing a mucositis duration of 70 to 84 days.Methods:
Complete a Glasziou rate ratio analysis, a relative risk analysis, and conduct a type I and type II error analysis by using the observed effect size of HPPCLS to determine adequacy of sample size of 66 patients using the P value ≤.001, powered at 95% confidence for no false-negatives.Results:
The Glasziou treatment effect for prevention, rapid reversal, and sustained elimination by HPPCLS was 100%, 96%, and 96%, respectively. This is compared with 0%, 0%, and 0% for generic sucralfate. The type I and type II error with the HPPCLS treatment effect at 0.1%, powered at 95%, predicted that a trial sample size of 3 patients would be required to statistically verify the HPPCLS treatment effect—reducing mucositis duration from the standard 70 to 84 days to 2 to 3 days. The HPPCLS trial had 53 patients with that outcome, far more than the 3 required for statistical proof of effect. The 70- to 84-day duration of mucositis reduced to 2 to 3 days by HPPCLS represented a 96% to 97% reduction in mucositis duration, which is unprecedented. Complete prevention of toxic mucositis by HPPCLS was equally unprecedented.Conclusion:
Statistically significant evidence shows that HPPCLS is associated with complete prevention and rapid sustained elimination of toxic mucositis during chemoradiation. Such outcomes should reduce patient morbidity and improve tolerance of anticancer treatments. Despite the strength of outcome association of a single registry study in a real-world setting, each institution will need to evaluate HPPCLS outcomes for their respective practice.
Tolerance of prescribed chemoradiation treatment is key to survivorship. Mucositis toxicity from chemoradiation lowers tolerance of treatment, which in turn lowers survivorship.1-4 The development of effective antidotes to chemoradiation toxicities has contributed to improved tolerance of optimal chemoradiation dosing. Antiemetics,5 bone marrow (leukocyte) stimulants,6 and hemopoietics (although used less frequently than in the past)7 have served to enhance tolerance to cancer treatment. However, over the past 40 years, effective therapeutic options for chemoradiation toxic mucositis (CRTM) have been lacking, leaving many to question whether anything could be done against mucositis.8,9 Interventions supported by guidelines provide only fractional impact on severity and pain.10-12 Despite evidence-based supported interventions, a significant number of patients newly diagnosed with cancer in the United States continue to develop CRTM at high cost in terms of morbidity,13-15 unplanned office and emergency department visits,16,17 and hospitalizations.18 Of the 1.6 million individuals diagnosed with cancer annually in the United States,19 at least 522,166 require curative doses of chemoradiation, resulting in 234,975 (45%) developing CRTM.20,21 The Agency for Healthcare Research and Quality (AHRQ) has established evidence-based practice centers in the United States to assist public and private sector organizations with improving the quality of healthcare. In an evidence report on the management of cancer symptoms, AHRQ identified toxic mucositis as a leading cause of pain in patients receiving cancer treatment.22 In a separate report on the comparative effectiveness of radiation therapy in head and neck cancer (HNC) patients, the AHRQ recognized CRTM as a dosing-limiting toxicity.23 This was significant because dose limitations impact survivorship by directly being associated with reduced 5-year survival in patients receiving chemotherapy1,2 or radiation.3,4
Toxic Mucositis More Than Oral Ulcers
Although not commonly thought of beyond oral erosions, CRTM is more than painful oral ulcers. The process of mucositis extends throughout the entire gastrointestinal (GI) tract. The clinical presentation for CRTM is determined by the anatomical location of occurrence within the GI tract, and the cytokine production at these sites contributes to systemic symptoms of fatigue, depression, cachexia, and sick behavior.24-27 In the oropharyngeal cavity and esophagus, CRTM gives rise to ulcerated lesions that often begin as a burning sensation (burning mouth syndrome) 4 to 7 days into chemoradiation.13,15 The subsequent loss of taste (ageusia) results from mucositis of the taste buds28 by arresting the replenishment of taste receptors required for the timed senescence of existing receptors. Toxic mucositis of the oropharynx or esophagus disables swallowing and is often managed with a surgical feeding tube.29,30 GI mucositis involves an inflammatory, presumably erosive and/or ulcerative process that gives rise to esophagitis, gastritis, colitis, and cecal enterocolitis.15 In the small intestine, direct cytotoxic damage of enterochromaffin cells (small bowel mucositis) releases serotonin and substance P to give rise to immediate and delayed onset of chemotherapy-induced nausea and vomiting.31 In the colon, apart from the colitis from mucosal erosion, and depending on the dose or type of chemotherapy, unrelenting diarrhea can occur as a form of CRTM,32 often requiring cancellation of the anticancer agent and high-dose steroids and loperamide to control it. In patients undergoing human stem cell transplantation, intestinal (colonic) mucositis is the likely cause of febrile bacteremia rather than neutropenia,33 as have been considered in the past. Because of the serious impairment to the GI tract from CRTM, Medicare defines this toxicity as an emergent medical condition,34 which is supported by data reported to the AHRQ by the Blue Cross and Blue Shield Association Technology Evaluation Center and Evidence-based Practice Center.23
Debility of Toxic Mucositis
The pervasive effects of CRTM can be so debilitating that it dehumanizes the treatment experience for cancer patients, who require additional emotional support by immediate caregivers. Patients find mucositis the single most “distressing”35 experience in receiving chemotherapy, with patient-reported mucositis lasting far longer36 than the commonly stated “2 to 4 weeks.” It is far more disturbing to patients than is reported by physicians37 within any given trial, who may estimate the problem as affecting only 52% of patients, while 90% will report extreme discomfort and disability from CRTM. This disparity between physician-reported and patient-reported symptoms has long been recognized in cancer treatment patients.38-41 The fact that patient-reported CRTM is more important is reflected in the additional hours required by the clinical staff in managing these patients. For HNC patients undergoing treatment, physicians and nurses spent 5.7 and 9.0 additional hours, respectively, per patient to navigate mucositis-related activities from planning to posttreatment.42 Those undergoing successive cycles of chemotherapy report that mucositis severity worsens by 20% to 30% over the previous cycle.43 Consequently, the patient-reported experience of CRTM drives both patient and clinician decisions to interrupt, reduce, or cancel cancer treatment altogether. Patients who develop grade 1/2 toxic mucositis from chemotherapy (with or without radiation) delay or postpone treatment at a rate of 23%, and those with grade 3/4 mucositis at a rate of 21%.15
Unplanned Breaks in Cancer Treatment – Lower Survival
Although not commonly regarded as unsafe, unplanned interruptions of radiation1,2 or chemotherapy3,4 unavoidably lead to a lower 5-year survival due to early recurrence of malignancy, with a 30% increase in mortality for chemotherapy patients1,2 and a 40% to 70% increase in mortality in HNC patients.4,44 Unplanned treatment breaks, for any reason, unavoidably result in reduced dose density of chemoradiation,1,4 that is, a reduced dose quantity per unit time required for a curative treatment course. It is reduced dose density, and not overall dose quantity,1,3 that leads to an early recurrence of neoplastic disease in patients who opt for unplanned treatment breaks. The doubling time for tumor cells surviving the initiation of chemoradiation shortens from 60 days to 4 days,45,46 thus unplanned breaks lowering overall dose density result in reemergence of disease. Early disease recurrence is linked to reduced 5-year survival in patients receiving chemotherapy11 or radiation therapy.3,4 An unplanned treatment break as short as 3 days can reduce 5-year survival from 65% to 18% for certain HNC patients.44 Thus, effective mitigation (and preferably complete elimination) of CRTM will positively impact survivorship.
Guideline-Supported Interventions and HPPCLS
There are many guideline-supported interventions, as will be discussed. Per review criteria, most interventions are recommended from a meta-analysis of randomized controlled trials (RCTs) without regard to the size of the treatment effect in relation to that of placebo or control. As will be discussed later, although the size of the treatment effect may be reproducible and statistically greater than placebo, it may be clinically insufficient to make a difference in a real-world clinical setting of patients, thus overall tolerance to cancer therapy is not improved. High-potency polymerized cross-linked sucralfate (HPPCLS), regulatory and pharmacologically distinct from standard sucralfate, is associated with a substantial treatment effect size, reducing mucositis duration by 96% to 97%. It was approved by the FDA in 2013 and has been associated with complete prevention and rapid sustained elimination of chemoradiation mucositis.47-49 Its data, being derived from an observational registry trial, mistakenly and in conflict with evidence-based medicine recognized by AHRQ,50 are often overlooked. Data from guideline-supported interventions are derived from fixed, controlled clinical settings that are rare in a busy clinical practice. On the other hand, data on HPPCLS are taken from the real-world treatment settings of clinical practice, involving 39 oncologists in 32 different practices across 14 states using 15 different anticancer treatment agents to manage 14 different cancer types in 10 organ systems over an 11-month period. Consistently, HPPCLS reduced mucositis duration by 96% to 97% and completely prevented its onset in patients who opted to avert surgical placement of a gastrostomy tube. This report evaluates the quality of that evidence and provides a plain language review of the statistics regarding the efficacy of HPPCLS as well as the inherent limitation of some guideline-supported therapies.
Methods
Narrative Description of the Mucositis Registry and HPPCLS
In past reports of these data, no narrative description of the registry was published. The presentation of descriptive tables highlighting particulars regarding the prescribing oncologists, their sites of practice, patients’ diagnosis, cancer treatments that gave rise to CRTM, and the severity grade of mucositis and its anatomical location have been reported only in abstract form for poster presentation.51 Tables displaying specific registry information have not been singularly paired to this type of narrative. A descriptive narrative will be instructive and capture the resilience of an intervention with identical and reproducible outcomes in real-world treatment scenarios that are clinically diverse.
Guidelines, Quality of Evidence, and HPPCLS Efficacy
Mucositis guidelines and their criterion for evidence quality are provided. A review of existing comparative effectiveness data on antimucositis therapies will be provided as context to the quality of the evidence reported on the efficacy of HPPCLS. A plain language assessment of the principles governing evidence quality and the statistical assessment of observation data are presented with the perspective of the AHRQ approach and evaluation of such data. Finally, to provide a statistical context of the HPPCLS outcomes from the registry study, this report discusses the relationship between treatment effect size and quality of evidence and the effect that placebo and other biases have on the treatment effect of any given intervention.
Results
A. HPPCLS
HPPCLS is a new polymerized cross-linked formulation of sucralfate recognized by the Center for Devices and Radiological Health of the FDA and licensed for the management of CRTM. Pharmacodynamically, HPPCLS is a more potent form of sucralfate. The 3-hour postadministration potency of a 10% HPPCLS suspension compared with that of a standard 10% sucralfate suspension is depicted in Figure 1. In terms of surface concentration of sucralfate, HPPCLS achieves sucralfate concentrations that are 7-fold (or 800%) greater on normal mucosa and 23-fold (or 2400%) greater on inflamed ulcerated mucosa.52 Sucralfate is nonsystemic, ingested to adhere to the mucosal lining, with 95% to 97% of the ingested dose expelled from the GI tract and the remainder absorbed as aluminum hydroxide and sucrose octasulfate (sulfonated table sugar).53-55 The entire clinical effect for sucralfate is linked to achievable surface concentration. Enhanced sucralfate surface concentration results in enhanced clinical effects.56 Complete prevention with gastrostomy tube aversion and rapid (2- to 3-day) reversal of toxic mucositis sustained throughout ongoing chemoradiation has occurred with HPPCLS.
B. Narrative on the Mucositis Registry Study Design
Table 1 provides a summary of the registry study with HPPCLS outcomes at a glance. The narrative to follow offers specifics to expand the summary and offer a clinical feel of the variety of common cancer treatment scenarios that led to toxic mucositis and that challenges any antimucositis therapy, including HPPCLS.
1. Postauthorization Surveillance by Mucositis Registry
The mucositis registry study was initiated as part of a postapproval requirement of regulatory authorities (FDA). This observation study represents proactive monitoring for unanticipated adverse events, patients’ acceptance of therapy, and real-world treatment outcomes.
2. Other Objectives of Mucositis Registry
Other objectives of the mucositis registry study were to observe patterns of prescribing and in-clinic use of practitioners as well as health outcomes associated with using HPPCLS in an uncontrolled clinical practice setting. Although authorized as a Class I medical device in the United States to be applied, swished, gargled, and then expectorated, the FDA insisted that clinicians be informed that HPPCLS was safe to swallow at up to 4 g daily for 56 consecutive days. This has been true for all sucralfate products since 1982.
3. Performance of Registry Study
- Ethical Approval: This surveillance study was observational, involving no element of intervention outside the licensed use of the product that would require review by an ethics committee. Observations were made within established oncology practices involving the routine management of mucositis with the informed consent of all participants involved. Observations were collected in a manner that did not invoke risks of harm or stigma to any involved.
- Selection of Clinicians and Patients: Clinicians (oncologists, mid-level practitioners, and oncology nurse specialists) voluntarily responded to national outreach efforts of Accredo Specialty Pharmacy of Express Scripts to provide information regarding HPPCLS. Patients with mucositis or those anticipated to develop mucositis were then selected by responding clinicians. Prescribers were not preselected. Besides full 500-mL prescriptions, immediate access to HPPCLS was provided through a physician-assigned patient sample program. Physician-assigned samples of HPPCLS (4- to 7-day 75-mL supply) were provided at no cost to patients or insurers for the initial management of mucositis.
- Inclusion Criteria: Any patient identified by an oncology clinician to receive HPPCLS was enrolled in the registry regardless of type of cancer, its staging, or the cancer treatment regimen. Mucositis at any site within the GI tract caused by or anticipated to be caused by an anticancer therapy was included. This inclusion criterion reflected the uncontrolled real-world clinical setting in which mucositis occurs and through which cancer treatment patients are to be navigated.
- Exclusion Criteria: Patients with any previously known adverse reaction (eg, allergy) to sucralfate were excluded. This exclusion criterion reflected the uncontrolled real-world clinical setting in which mucositis occurs.
- Physician-Assigned Named Samples: Patients identified by oncology clinicians were given a 75-mL 4 to 7-day physician-prescribed professional sample of HPPCLS and received patient instruction sheets accordingly. Patients were maintained weekly on assigned samples at the request of the clinician. Depending on the severity of mucositis or management goal (treatment vs prevention), each patient-administered dose ranged from 2.5 to 10.0 mL of paste per dose.
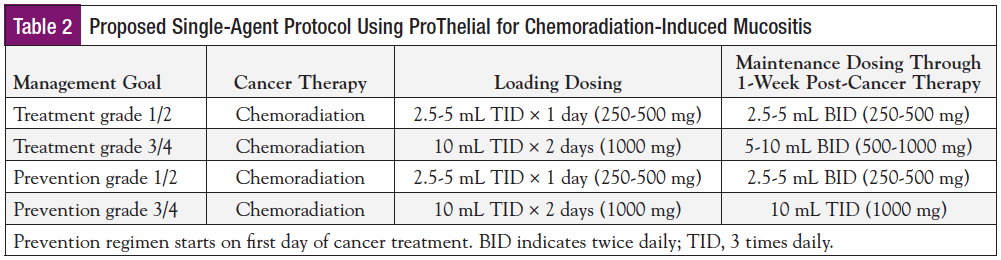
- Instructions for Use and Dosing: The adult dose of HPPCLS administered was determined by both the intent of management (prevention vs reversal) and by the anticipated or known grade of mucositis (discussed in next section). Dosing used is described in Table 2. Patients were instructed to use their tongue to apply the dose to all surfaces inside the mouth, then gargle with it for 10 seconds, hold it in their mouth for 15 seconds, and then expectorate or swallow if so instructed by their oncologist. If tongue application was not possible, then cotton-tipped swabs or a soft-bristle toothbrush were used to apply HPPCLS to all oral surfaces, followed by gargling and holding it in the mouth for 15 seconds. Clinicians explained that HPPCLS was safe to swallow at 1 g 4 times daily for up to 56 continuous days in patients aged ≥12 years. Patients <12 years (not in this report) could use HPPCLS, swish, expectorate or swallow as directed by a pediatric oncologist; generally, not more than 14 mg/kg/dose 2 to 3 times daily depending on severity of mucositis developed or anticipated.
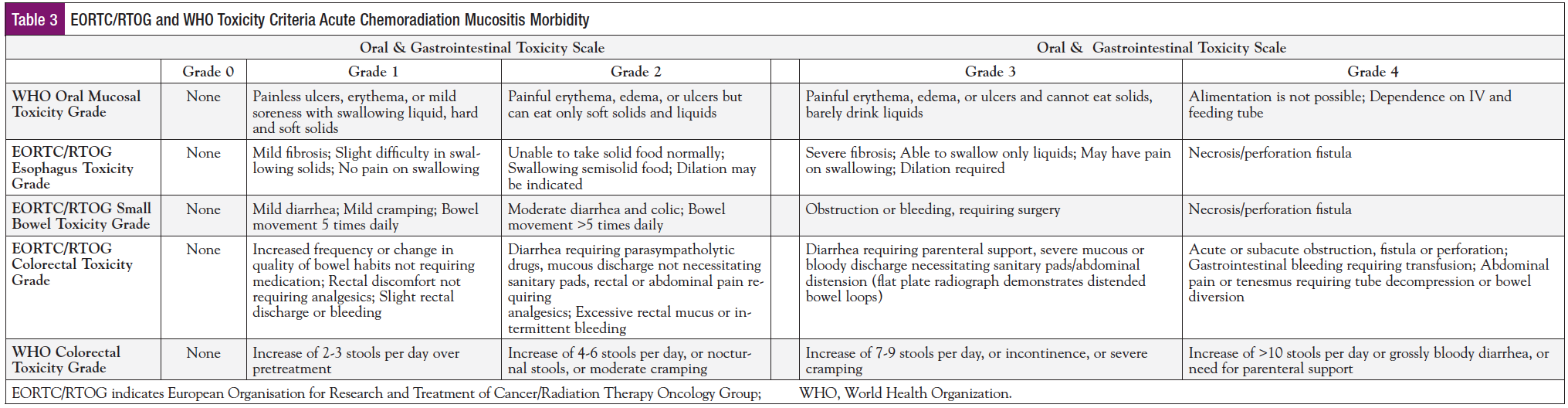
- Assessing Grade of Mucositis: Grade and functions related to difficulty with eating, drinking, swallowing, nausea, vomiting, and diarrhea were identified by the clinical staff prescribing HPPCLS and confirmed by follow-up phone calls of registry attendants. The functional patient-reported scale of the World Health Organization (WHO)57 and the European Organisation for Research and Treatment of Cancer/Radiation Therapy Oncology Group (EORTC/RTOG) grading scale58 were used and are shown in Table 3. Mouth/throat soreness was incorporated in the WHO scale.
4. Registry Characteristics
The mucositis registry was populated from February 10, 2014, through December 30, 2014, and included 66 sequentially enrolled patients, with 55 patients receiving radiotherapy as part of their cancer treatment.
- Registry Clinicians and Institutions: There were 39 oncologists (26 radiation oncologists, 13 medical oncologists) from 32 different oncology institutions across the United States.
- Registry Institutions: There were 32 participating institutions across 14 states in the United States, including Connecticut, Florida, Georgia, Illinois, Kansas, Massachusetts, Maine, Michigan, New York, Pennsylvania, Rhode Island, Tennessee, Texas, and Washington. The type of oncology practices included National Cancer Institute–designated facilities (n = 4), National Comprehensive Cancer Network (NCCN) practices (n = 2), hospital-based institutions (n = 20), and community- based practices (n = 6).
- Registry Patients: Sixty-six consecutive patients were enrolled in the registry: 48 males (aged 46-93 years) and 18 females (aged 14-84 years). Five patients were lost to follow-up, leaving 61 patients represented and reported in the outcome data. All patients had either undergone or were to undergo chemotherapy, radiation, or combined chemoradiation for curative cancer treatment. Of the 61 patients completing follow-up, 53 were prescribed HPPCLS for treatment or reversal of mucositis, and 8 patients were prescribed HPPCLS to prevent it.
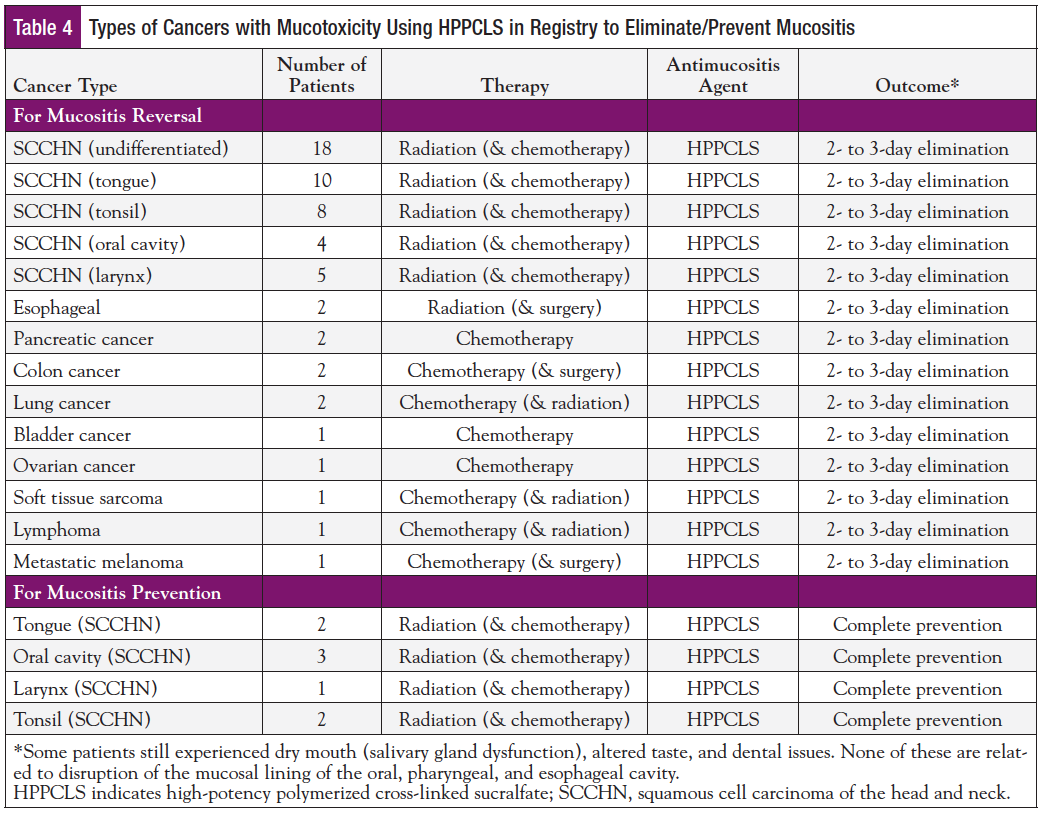
- Types of Cancers in Registry: Table 4 lists the 14 different types of cancers that occurred in 10 different organ systems: head and neck, esophagus, lung, pancreas, colon, bladder, ovary, lymphoma, sarcoma, and skin. The types of cancer under treatment in the registry included unspecified squamous cell carcinoma (SCC) of the head and neck (n = 18), SCC of the tonsil (n = 10), SCC of the tongue (n = 12), SCC of the oral cavity (n = 7), SCC of the larynx (n = 6), esophageal cancer (n = 2), pancreatic cancer (n = 2), colon cancer (n = 2), lung cancer (n = 2), bladder cancer (n = 1), ovarian cancer (n = 1), soft tissue sarcoma (n = 1), lymphoma (n = 1), and metastatic melanoma (n = 1).
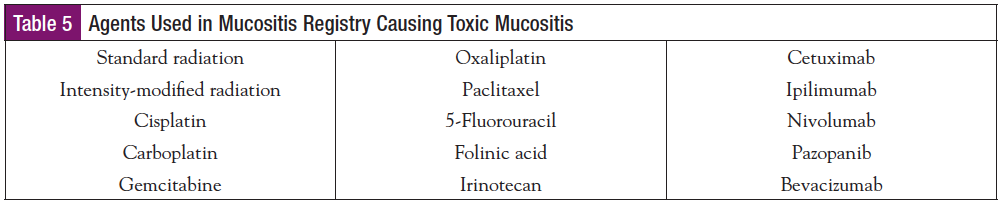
- Type of Anticancer Treatments Associated with Mucositis in This Study: Table 5 shows the antineoplastic agents prescribed by oncologists in the registry. Of the 61 patients reported, 1 received intensity-modulated radiotherapy, and the remainder (n = 60) received standard radiotherapy. All told, toxic mucositis in the oropharynx, esophagus, and small and large intestine were caused by 15 anticancer therapies: standard radiation and intensity-modified radiation in combination with ipilimumab, nivolumab, cetuximab, bevacizumab, pazopanib, folinic acid, 5-fluorouracil, irinotecan, oxaliplatin, carboplatin, cisplatin, paclitaxel, and gemcitabine. Mucositis damage mediated by these agents occurred as follows: Radiotherapy damages cellular DNA, creating reactive oxygen species in cellular cytoplasm with hypoxic and nutrient-starved conditions within normal and tumor cells. The classic chemotherapy agents in this series (carboplatin, paclitaxel, 5-fluorouracil, folinic acid, irinotecan, and oxaliplatin) have mechanisms of action targeting functional elements of the mitotic cycle in all dividing cells, whereas nonclassic immunotherapeutics (cetuximab, ipilimumab, nivolumab, ipilimumab, bevacizumab, and pazopanib) target different cellular elements to cause toxic mucositis. For example, cetuximab is a tyrosine kinase inhibitor antibody targeting the receptor for epithelial growth factor on tumor and normal cells. Ipilimumab is an antibody that targets cytotoxic T-lymphocyte protein 4, an antigen that disables cytotoxic T lymphocytes from engaging foreign tumor cells in the body. By this action, ipilimumab augments T-cell activation and proliferation to attack cancer cells. Nivolumab is an antibody targeting PD-1 ligands known to combine with accessory ligands (PD-L1 and PD-L2) to activate the PD-1 receptor on cytotoxic T lymphocytes. Activation of the PD-1 receptor inhibits the proliferation and cytokine production of anticancer cytotoxic T lymphocytes. Thus, by blocking the inhibitory PD-1 receptor, nivolumab allows cytotoxic T cells to proliferate, generate cytokines, and kill cancer cells. Regardless of the mechanism of action, each agent gives rise to toxic mucositis of the oral and GI tract with symptoms that include painful ulcerations, difficulty swallowing, nausea, vomiting, and diarrhea.
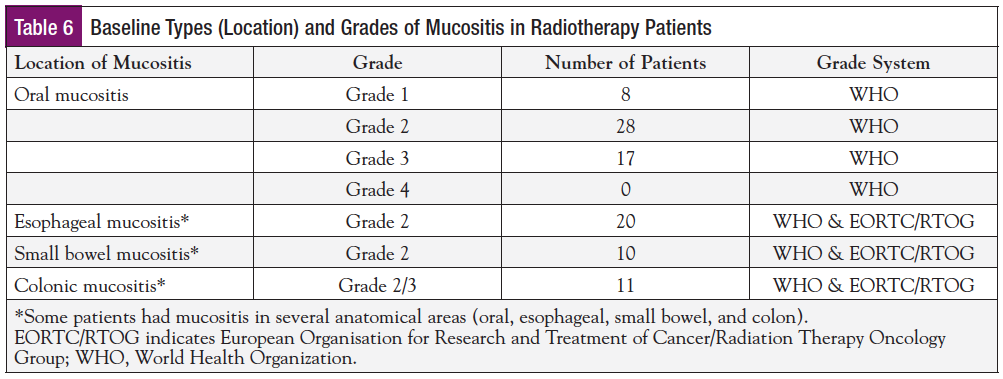
- Baseline Grades of Mucositis: The WHO scale with mouth/throat soreness for oral mucositis and the EORTC/RTOG and WHO Scale for GI Toxicity were used to grade the 53 patients with mucositis. The number of patients per grade and location of mucositis is shown in Table 6.
- Baseline Antimucositis Interventions Used by Clinicians: Historically, 28 of the 39 practitioners of this registry had managed mucositis with mouth rinses (FDA-approved ones and magic mouthwash), antacids, oral hygiene, generic sucralfate suspension, or cryotherapy. The remaining practitioners had no treatment preferences. Dissatisfaction with current interventions drove decisions to prescribe HPPCLS for all 39 practitioners, as patients’ intolerance of persisting mucositis limited the ability to maintain optimal dosing without unplanned interruption. Advanced practice nurse navigators, oncology nurse practitioners, physician assistants, and oncology pharmacists took the initiative in prescribing HPPCLS in both medical and radiation oncology suites.
- Outcomes Collection: Outcomes data were collected by a registry attendant through calls made to both clinical practices and patients. Mouth/throat soreness inquiry of patients incorporated into the WHO grading scale and visual inspection of presence of symptoms/signs of mucositis was noted at day 1 of use of HPPCLS. All information was collected within 4 to 7 days of patients’ initial use of HPPCLS. Staff and patients were specifically asked regarding the timing of clearance of symptoms and signs of mucositis, with a focus on the presence or absence of symptoms or signs on days 1, 2, 3, 4, and 7 and at the end of anticancer treatment.
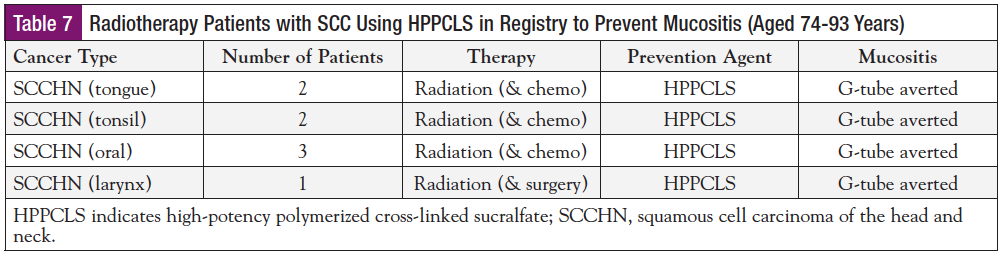
- Mucositis Prevention to Avert Gastrostomy Tube Anticipated Placement: Eight patients without mucositis were prescribed HPPCLS (using the prevention protocols in Table 2) because oncologists anticipated the development of grade 3/4 mucositis in elderly patients (aged ≥74 years), which would necessitate prophylactic placement of a gastrostomy feeding tube. These patients described in Table 7 included 6 males (aged 78-93 years) and 2 females (aged 74 and 84 years) who were assigned baseline grade 0 mucositis pretreatment. Three patients had oral cancer, 2 with tongue cancer, 2 with tonsil cancer, and 1 with cancer of the larynx.
5. HPPCLS Outcomes
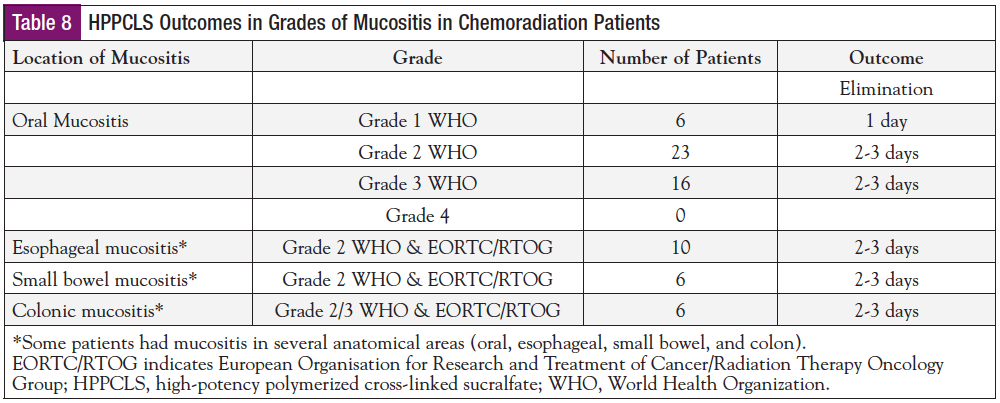
The outcomes of the mucositis registry study reported previously47,48,51 can be seen in Tables 1, 4, and 7, and Table 8. No adverse reactions were encountered, and HPPCLS was well tolerated, which met the main objective of this surveillance study. Forty-eight of the 61 patients (78.7%) reporting outcomes were instructed by prescribers to swallow HPPCLS (an off-label instruction) rather than expectorate following tongue application and gargling. This was done presumably to manage mucositis of the esophagus, small intestine, and colon.
When used with intent to prevent mucositis in 8 patients, HPPCLS was successful in preventing the onset of mucositis in all 8 (Table 8). This had the intended benefit of averting surgical placement of gastrostomy feeding tubes. This outcome represented an unusual prevention rate of 100%, a reproducible treatment effect occurring with 3 oncologists in clinical practices of differing geographical regions.
Table 4 shows that HPPCLS reduces mucositis duration to 2 to 3 days. Table 6 shows that this occurred regardless of the severity of mucositis or its anatomical location. The standard duration of mucositis in HNC patients receiving radiotherapy, 70 to 84 days, has remained stable over the past decade in reports from Elting et al in 200713 with 126 patients, in 200859 with 204 patients, to the report from Franco et al in 2017 with 21 patients.60 Comparing these 351 patients as historical controls for a standard mucositis duration of 70 to 84 days, the reduction of duration to 2 to 3 days using HPPCLS represents a 96% to 97% reduction, a significant treatment effect.
Discussion
A. Mucositis Guidelines and Quality of Evidence
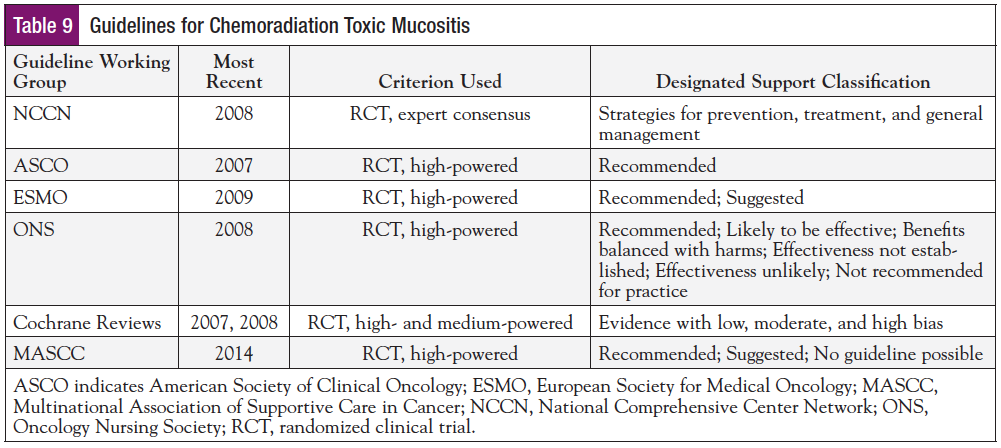
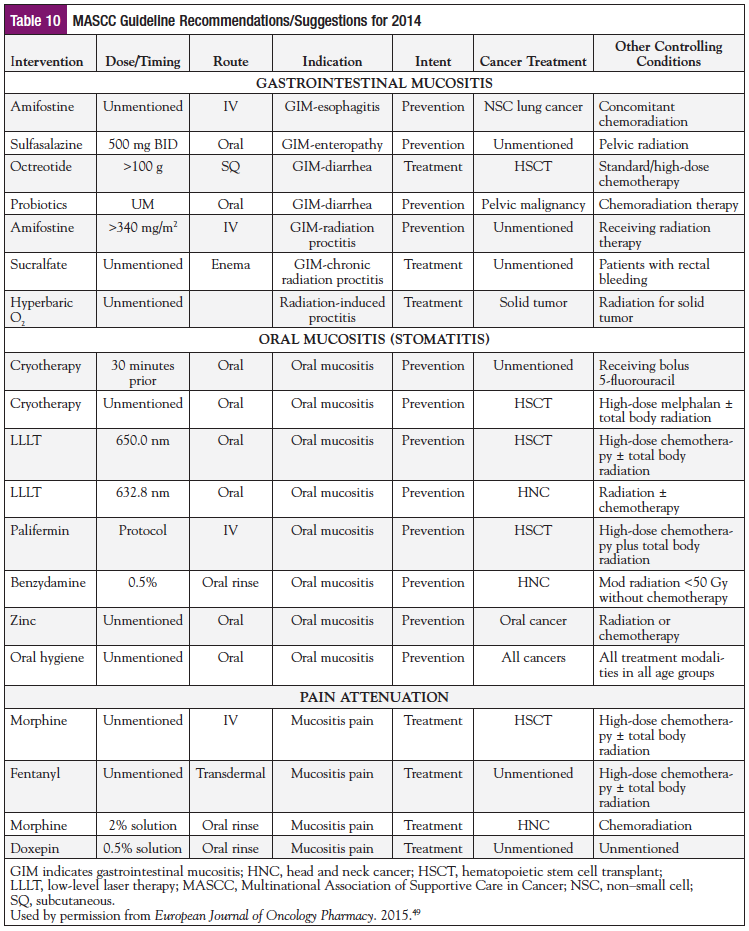
Past and present evidence-based guidelines for the management of toxic mucositis are listed in Table 9. The American Society of Clinical Oncology (ASCO) published the first guideline in 1999 and updated it in 2002 and 2008.61 The NCCN published mucositis guidelines in 2008,12 and the Multinational Association of Supportive Care in Cancer (MASCC) published guidelines in 2004, 2007, 2010, and 2014.11 Mucositis guidelines have been published by the European Society for Medical Oncology (ESMO)62 in 2009 and the Oncology Nursing Society (ONS)63 in 2008. The Cochrane reviews, although not formally viewed as guidelines, are often cited by the other guidelines.64,65 The working group of each guideline utilized slightly different criteria to assess quality of evidence and establish their support or recommendation for any one intervention. Whereas the ASCO guideline limited the 2008 review to 4 select agents (dexrazoxane, amifostine, mesna, and palifermin), the MASCC guideline identified many more interventions, reviewing the literature to select publications in accordance with 5 levels of evidence. In its earlier guidelines, MASCC provided 4 categories for practice guidance: (a) recommended, (b) suggested, (c) not recommended, and (d) no guideline possible. Recently this has been simplified to 3 categories: (a) recommended, (b) suggested, and (c) no guideline possible. Recognizing the lack of comprehensive research on all possible management modalities across all clinical settings (particularly those outside RCTs), the NCCN integrated “expert judgment or consensus” with management strategies from data gleaned from both the Cochrane reviews (which focus on mucositis incidence rather than duration) and the MASCC guidelines. At present, only MASCC has an organized, ongoing working group for mucositis management, and the release of an updated guideline in 2018 is expected. Table 10 lists the 2014 MASCC guideline-supported interventions11 (which have been reviewed elsewhere49) with respect to the intervention’s intent of use, whether for prevention or for treatment (reversal) and other contextual elements that defined their efficacy. Each MASCC-supported intervention provides only fractional or incremental efficacy within rigidly controlled clinical settings.
B. Level of Evidence Used
Each guideline uses some variation of Somerfield’s 5 levels of evidence scheme,66 in which levels IV and V are evidence from nonexperimental observational studies, case reports, and clinical examples. Levels I, II, and III are evidence from investigational trials with an intervention and control group that are either high, low, or insufficiently powered to manage false-positive and false-negative errors.
Of the 14 interventions supported by MASCC with level I and level II evidence, 10 are off-label uses. All MASCC-supported interventions have reproducible, statistically significant treatment effects of modest size in a controlled setting. Generalized application and practicality of guideline-supported therapies have been questioned in the past.49,67 The challenging issue is that modest reductions in mucositis severity and improved palliation of mucositis pain in a controlled setting have not transferred well into clinically meaningful benefits in the real-world practice of oncology. The heterogeneous nature of oncology practice calls for complete prevention, rapid sustained elimination, or both.
C. PEP Guidelines from ONS
In an effort to put evidence into practice (PEP), the 2008 mucositis management guidelines from ONS identified interventions that were within the scope of nursing practice and integral to nursing care. It used a weight-of-evidence classification scheme that modified the Somerfield principles of evidence to include categories of “benefits balanced with harms,” “effectiveness not established,” “effectiveness unlikely,” and “not recommended to practice.” Similar to the MASCC, NCCN, and ESMO guidelines, it reserved categories of “recommended for practice” and “likely to be effective” for interventions deployed in high- to low-powered RCTs involving more than 100 patients. Oral care, cryotherapy, and palifermin were recommended for practice, whereas other nursing accessible interventions were correctly relegated to categories of either “effectiveness not established” or “effectiveness unlikely.”
D. Guidance on Guidelines—Their Strengths, Their Shortcomings, and the AHRQ
The common strength of all mucositis guidelines is the rigor used to identify statistically relevant interventions in RCTs as well as interventions that are clinically irrelevant. Suggested or recommended interventions with statistically relevant outcomes in controlled clinical settings are of limited use for real-world settings. This is because fractional improvements of controlled settings are simply too modest to make a meaningful clinical difference in real-world clinical settings. What’s missing in most guidelines, which has been identified by the AHRQ, is a category of evidence that takes into consideration the overall size of the intervention’s treatment effect.
Because the physical size of the treatment effect of most interventions is relatively small, RCTs with placebo, blinding, and an adequate number of patients are required. The quantitative size of the treatment effect for most interventions is within the order of magnitude of the placebo effect68; it’s merely statistically better than placebo, although only incrementally so. To state it plainly, the effect size from any one intervention is more likely than not to be within 10 to 30 base points beyond the effect size of placebo. Additionally, the treatment effect size may be increased or diminished by 10 to 30 points69 by the presence of bias in patient selection or in nonconcealment (open label) of the interventions from the investigator, patient, or data collector. The latter is known as a bias effect of nonblinding, also referred to as poor allocation concealment. The bottom line is that because the effect size of an intervention is similar (in order of magnitude, within 10-100 base points) to the effect size of placebo, both of which are vulnerable to bias, to identify a true treatment effect of any intervention, trials must be controlled, randomized, and blinded. However, there are interventions with effect sizes that are several orders of magnitude beyond that of placebo. Due to a restricted approach, most mucositis guidelines are blind to this distinction among any one intervention.
The AHRQ, however, recognizes that for some interventions, the treatment effect size is so considerable that it is expected to make a substantial clinical impact on the disease process. Citing the work of Glasziou et al70 of the University of Oxford Centre for Evidence-Based Medicine, the AHRQ recognized that interventions with treatment effect sizes that are at least 1000 base points greater than placebo or other biases are statistically significant, and the sheer size of the treatment effect is evidence of high quality that cannot be improved upon by randomized controlled trials involving that intervention.
E. Treatment Effect Size 10-Fold or Greater Is Evidence-Based Criterion
Treatment effect size of an intervention that is ≥10 times that of placebo or any other confounding bias or of the rate of reversal of disease is known as a positive Glasziou treatment effect.70 Large treatment size is a level of evidence that is, by definition, independent of trial design, whether controlled, poorly uncontrolled, or observational. This makes sense because trials are performed to quantify the magnitude of the treatment effect of an intervention. The quantitative veracity of that effect is bolstered by applying measures that limit or restrict the influence of other factors or biases—biases such as the effect of placebo, patient selection and number, and use of an intervention blinded from the investigator, the patient, or those collecting the data. As mentioned above, because the effect size of a treatment and placebo are of the same order of magnitude,68 both less than 80 to 100, control of nontreatment effects must be extreme. This control does not occur in real-world settings of clinical practice. For most interventions, without applying these restrictions (randomization, placebo/controls, or blinded use of either placebo or the intervention), quantification of a treatment effect cannot be trusted. Without these artificial restrictions, the treatment signal may not be a true signal of efficacy. Thus, MASCC, NCCN, ESMO, and ONS guidelines correctly exclude support for standard interventions tested in uncontrolled real-world settings. However, unlike AHRQ, these guidelines are incomplete, simply because no allowance is made for interventions with rate ratios that are greater than 10 times expected.
F. Illustration of Positive Glasziou Treatment Effect
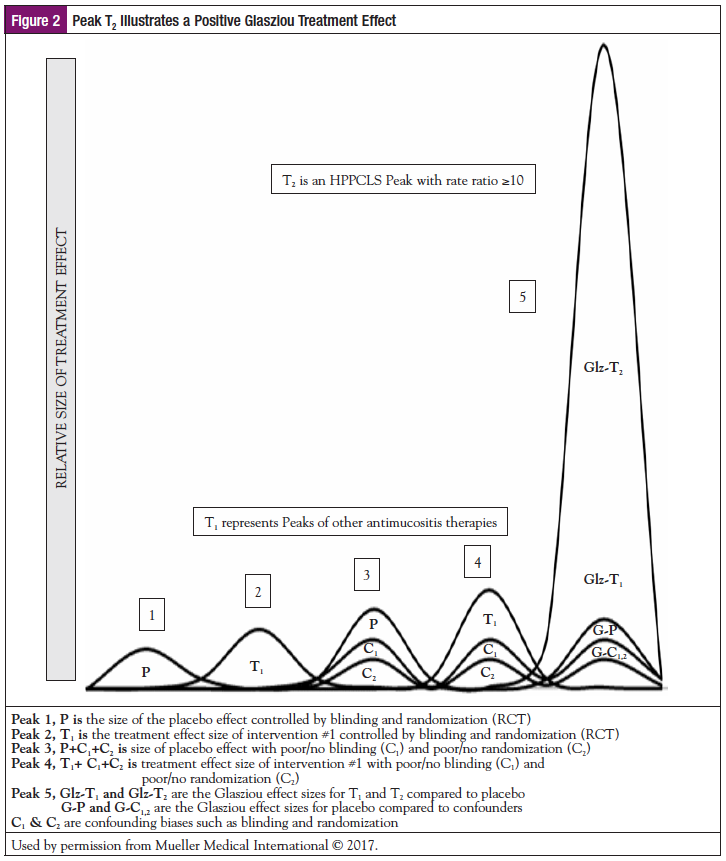
This point is illustrated in the 5 peaks in Figure 2 on the Glasziou treatment effect.
While the caption for Figure 2 provides some detail, it suffices to state that the first 4 peaks demonstrate the effect size of placebo, an intervention, and confounding factors. Peak 5 demonstrates an effect size of an intervention with a positive Glasziou treatment effect. Most mucositis guidelines address interventions with effect sizes similar to Peak 2 and Peak 4. None address interventions with effect sizes similar to Peak 5. From Figure 2 it is plain to see that within Peak 5, even if the effect sizes of placebo and other biases (confounding factors) were never controlled (such as in an observational registry study), the overall effect size of the treatment would not be affected.
Glasziou treatment effects are uncommon but do exist. The use of insulin for hyperglycemia to repeatedly, and thereby predictably, lower blood sugar is a positive Glasziou treatment effect. The use of edrophonium to repeatedly, and thereby predictably, reverse myasthenia gravis (the Tensilon test) is a positive Glasziou treatment effect. The treatment effect size of insulin and edrophonium is far greater than 1000 base points beyond placebo or the natural course of either disease, thus neither require RCTs for investigators to believe their respective effects. In addition, because the size of the treatment is so large, the false-positive and false-negative rates will be very low, and thus the sample size required to verify this treatment effect will be in the order of 3 to 10 people.
G. Application to HPPCLS Outcomes
1. Statistical Significance of HPPCLS Outcomes
In reducing mucositis duration from 70 to 84 days to 2 to 3 days, HPPCLS demonstrates a large treatment effect equal to a 96% to 97% reduction in mucositis duration. It has a Glasziou treatment effect70 that is 6780 base points beyond expected, having a Glasziou rate ratio of 67.8. The treatment outcome is believable, reproducible, and therefore significant. The Glasziou treatment effect is an evidence-based, quantitative statistical method that verifies the veracity (believability) of an observed treatment outcome, defining it as a rate ratio ≥10-fold in the effect of using an intervention versus the effect of not using an intervention to treat a disease process. Strictly speaking, a full evidence-based guideline should include considerations regarding the size of the treatment effect as illustrated in Figure 2. Most, however, do not.
2. HPPCLS Sample Size: 3 versus 51
Using HPPCLS’ treatment effect size, it is possible to calculate the number of patients required to statistically verify a cause-connection of the intervention with this outcome. Powering an RCT at 95% confidence accepting a P value <.001, the number of patients required to verify as real the 97% reduction in mucositis duration by HPPCLS is n = 3. That is, to verify that the observation of 97% reduction in mucositis duration is caused by HPPCLS, at least 3 of 3 patients with this outcome is required. In the HPPCLS mucositis registry study there were 51 such patients. Beyond the 3 consecutive patients statistically required to validate the outcome, this outcome occurred 51 times in 51 consecutive patients. This represented 17 times the number of observations required to ascribe cause-association of outcome to HPPCLS. The intent to treat was the reversal of grade 2/3 mucositis caused by 15 different cancer treatment agents. This angle of analysis supports that the use of HPPCLS for the management of CRTM is credible and statistically sound.
3. HPPCLS Relative Reduction of Risk as a Measure of Evidence Quality
Relative reduction in the risk of persisting CRTM in patients on the 15 anticancer regimens was significant at 0.04. Thus, the likelihood of mucositis-associated treatment breaks in patients on HPPCLS is only 4%. Despite the observation study design, this relative reduction in risk is an additional evidence-based measure of the quality of HPPCLS data. In a general review on the quality of evidence, Guyatt et al71 advised that data from observational studies demonstrating a large reduction in risk of an event are acceptable as high-grade evidence—evidence equivalent to appropriately powered RCTs. For example, a meta-analysis of observational studies showing that bicycle helmets reduce the risk of head injuries to cyclists involved in crashes by 69% was a large effect size for any intervention,72 and thus is proof of outcome. Additionally, Cannegieter et al cited observational studies evaluating the impact of warfarin to prevent thromboembolic events in patients with cardiac valve replacement.73 The relative risk for patients developing thromboembolism on warfarin following cardiac valve replacement was of 0.17. The 83% reduction in risk was evidence of high quality despite the observational study design. The reduction in risk was significant enough to make guideline recommendations, particularly for a certain subgroup of patients at high risk.74
Judging from the work of Guyatt et al71 (who cites Glasziou et al70 in their report), the size of the HPPCLS treatment effect reported in their observational study would be considered statistically credible and of high quality. The relative risk that grade 2/3 oral mucositis will persist in an HNC patient receiving radiotherapy while on HPPCLS is 0.04, far better than 0.17 for warfarin in lowering the risk of thromboembolism following cardiac valve replacement. Additionally, the relative risk of an HNC patient developing toxic mucositis if given HPPCLS preemptively and continued throughout radiotherapy is even less than 0.04 and near zero.
4. Patient Education Required with HPPCLS Use
HPPCLS is a paste with the consistency of yogurt nearly liquefying upon application and requires patient education for maximal benefit. Patient use instructions are always provided (Figure 3). Some patients dose themselves without full application of the HPPCLS to all surfaces of the oral cavity. Full application of HPPCLS to all oral surfaces is particularly important for patients who suffer from chemoradiation-induced dysgeusia or ageusia. Since taste buds are located over the tongue, cheeks, soft palate, and upper esophagus, it is important that HPPCLS be applied to these surfaces to mitigate the effects of mucositis on taste buds. This is best accomplished by using a soft-bristled toothbrush to manually apply half the dose to accessible areas of the oral cavity followed by gargling in the pharynx. The upper esophagus can be reached only by swallowing the gargled dose, which 78% of registry patients had been instructed to do by their oncologist. One patient with radiation-induced pharyngitis, esophagitis, and oral ulceration experienced relief of esophagitic dysphagia and partial relief of pharyngeal ulcerations, but only limited relief of oral ulceration. It was discovered that he had not appropriately applied HPPCLS to the entire oral cavity and did not gargle before swallowing. When corrected by the nursing staff, he experienced rapid reversal of the oral ulcerations and residual pharyngitis. Thus, the appropriate use of HPPLCS falls within the scope of nursing practice and can become integral to oncology nursing care.
Conclusions
As stated by Harris et al, “because mucositis is a systemic process, interventions with the greatest impact are those that exert their effects systemically.” Although indicated for the management of oral mucositis, HPPCLS has been associated with complete prevention and rapid sustained elimination of chemoradiation mucositis throughout the GI tract, specifically in the oropharynx, esophagus, small bowel, and colon of these registry patients. For oral mucositis, the size of the treatment effect was substantial, reducing mucositis duration from the standard 70 to 84 days in HNC patients to 2 to 3 days. It completely prevented mucositis onset in others, thus averting surgical placement of gastrostomy feeding tubes in 8 of 8 patients, all of whom were ≥74 years of age and generally the most vulnerable. A 96% to 97% reduction in mucositis duration qualified for a level of evidence criterion used by the AHRQ. The lack of adopting the Glasziou treatment effect by most guidelines is not a reflection on the phenomenon of outsized treatment effects. Rather, it reflects an analytical blind spot of some mucositis guidelines, noninclusive of the entire science of evidence-based guideline development espoused by academic and government practitioners of the science.50,68,70,71,75
Although guidelines are excellent in identifying which interventions in RCTs work and which do not, their support of recommended or suggested interventions, whether for prevention or reversal, have inexact utility because most interventions provide only fractional benefits even within strictly controlled clinical settings. Transference of benefit into real-world settings of clinical practice has yet to be realized.
On the other hand, the clinical benefits of HPPCLS have been demonstrated in the real-world uncontrolled settings of clinical practice, being challenged by the variety of practitioners (medical and radiation), institutions, regional practice, tumor types, and anticancer agents, including 5 immunotherapies. In addition, the anatomical location of chemoradiation mucositis was equally responsive to HPPCLS. Still, without attentive nursing care directing appropriate oral application of HPPCLS patient by patient, the significant clinical benefits could be entirely missed.
The evidence-based statistics of the benefit of HPPCLS are plain and evident. And where there is no mucositis, there can be no mucositis-associated deaths or unplanned treatment interruptions. Mucositis-associated emergency department visits and emergency hospitalizations should be impacted as well. If its clinical efficacy persists as it gains wide acceptance and use, then HPPCLS may become a potential tool for improved navigation of patients through the cancer treatment experience.
Funding
This article was written without funding from any outside entity.
References
1. Foote M. The importance of planned dose of chemotherapy on time: do we need to change our clinical practice? Oncologist. 1998;3:365-368.
2. Cairo MS. Dose reductions and delays: limitations of myelosuppressive chemotherapy. Oncology (Williston Park). 2000;14(suppl 8):21-31.
3. Rosenthal DI. Consequences of mucositis-induced treatment breaks and dose reductions on head and neck cancer treatment outcomes. J Support Oncol. 2007;5(suppl 4):23-31.
4. Russo G, Haddad R, Posner M, et al. Radiation treatment breaks and ulcerative mucositis in head and neck cancer. Oncologist. 2008;13:886-898.
5. Hesketh PJ, Kris MG, Basch E, et al. Antiemetics: American Society of Clinical Oncology Clinical Practice Guidelines update. J Clin Oncol. 2017;35:3240-3261.
6. Lyman GH, Allcott K, Garcia J, et al. The effectiveness and safety of same-day versus next-day administration of long-acting granulocyte colony-stimulating factors for the prophylaxis of chemotherapy-induced neutropenia: a systematic review. Support Care Cancer. 2017;25:2619-2629.
7. Gawade PL, Berlin JA, Henry DH, et al. Changes in the use of erythropoiesis-stimulating agents (ESAs) and red blood cell transfusion in patients with cancer amidst regulatory and reimbursement changes. Pharmacoepidemiol Drug Saf. 2017;26:1357-1366.
8. Donnelly JP, Blijlevens NM, Verhagen CA. Can anything be done about oral mucositis? Ann Oncol. 2003;14:505-507.
9. Miyamoto CT. Reducing the incidence and severity of oral mucositis – Can it be done? US Oncological Disease. 2007;1(2):18-21.
10. Eilers J, Harris D, Henry K, et al. Evidence-based interventions for cancer treatment-related mucositis: putting evidence into practice. Clin J Oncol Nurs. 2014;18(suppl):80-96.
11. Lalla RV, Bowen J, Barasch A, et al. MASCC/ISOO clinical practice guidelines for the management of mucositis secondary to cancer therapy. Cancer. 2014;120:1453-1461.
12. Bensinger W, Schubert M, Ang KK, et al. NCCN Task Force Report: prevention and management of mucositis in cancer care. J Natl Compr Can Netw. 2008;6(suppl 1):S1-S21.
13. Elting LS, Cooksley CD, Chambers MS, et al. Risk, outcomes, and costs of radiation-induced oral mucositis among patients with head-and-neck malignancies. Int J Radiat Oncol Biol Phys. 2007;68:1110-1120.
14. Murphy BA. Clinical and economic consequences of mucositis induced by chemotherapy and/or radiation therapy. J Support Oncol. 2007;5(suppl 4):13-21.
15. Elting LS, Cooksley CD, Chambers M, et al. The burdens of cancer therapy. Clinical and economic outcomes of chemotherapy-induced mucositis. Cancer. 2003;98:1531-1539.
16. Mayer DK, Travers D, Wyss A, et al. Why do patients with cancer visit emergency departments? Results of a 2008 population study in North Carolina. J Clin Oncol. 2011;29:2683-2688.
17. Barbera L, Taylor C, Dudgeon D. Why do patients with cancer visit the emergency department near the end of life. CAMJ. 2010;182:563-568.
18. Uramoto H, Iwashige A, Kagami S, et al. Prediction of emergency hospitalization of outpatients receiving cancer chemotherapy. Anticancer Res. 2007;27:1133-1136.
19. American Cancer Society. Cancer Facts & Figures 2015. Atlanta, GA: American Cancer Society; 2015. www.cancer.org/acs/groups/content/@editorial/documents/document/acspc-044552.pdf.
20. Kolodziej M, Hoverman JR, Garey JS, et al. Benchmarks for value in cancer care: an analysis of a large commercial population. J Oncol Pract. 2011;7:301-306.
21. McCullough RW. Prevalence, costs, duration of chemoradiation mucositis (CRM) and a prevention/reversal protocol using FDA approved
polymerized cross-linked sucralfate. Supp Care Cancer. 2017;25(suppl 2):S133. Abstract eP192.
22. Carr D, Goudas L, Lawrence D, et al. Management of Cancer Symptoms: Pain, Depression, and Fatigue. Summary. Evidence Report/Technology Assessment No. 61. AHRQ Publication No. 02-E031. Rockville, MD: Agency for Healthcare Research and Quality. July 2002.
23. Samson DJ, Ratko TA, Rothenberg BM, et al. Comparative Effectiveness and Safety of Radiotherapy Treatments for Head and Neck Cancer. Comparative Effectiveness Review No. 20. Rockville, MD: Agency for Healthcare Research and Quality. www.ncbi.nlm.nih.gov/books/NBK45242. May 2010.
24. Kursrock R. The role of cytokines in cancer-related fatigue. Cancer. 2001;92(suppl):1684-1688.
25. Myers JS. Proinflammatory cytokines and sickness behavior: implications for depression and cancer-related symptoms. Oncol Nurs Forum. 2008;35:802-807.
26. Jereczek-Fossa BA, Marsiglia HR, Orecchia R. Radiotherapy-related fatigue. Crit Rev Oncol Hematol. 2002;41:317-325.
27. Smets EM, Visser MR, Willems-Groot AF, et al. Fatigue and radiotherapy: (B) experience in patients 9 months following treatment. Brit J Cancer. 1998;78:907-912.
28. Nguyen HM, Reyland ME, Barlow LA. Mechanisms of taste bud cell loss after head and neck irradiation. J Neurosci. 2012;32:3474-3484.
29. Morton RP, Crowder VL, Mawdsley R, et al. Elective gastrostomy, nutritional status and quality of life in advanced head and neck cancer patients receiving chemoradiotherapy. ANZ J Surg. 2009;79:713-718.
30. Brown T, Hill J. Evidence based review: prophylactic percutaneous endoscopic gastrostomy tube placement in head and neck cancer patients undergoing radiotherapy or chemo-radiotherapy. Allied Health. Queensland Government. Queensland Health. www.health.qld.gov.au/cairns_hinterland/docs/cc_prophylactic_peg.pdf. 2004.
31. Hesketh PJ. Chemotherapy-induced nausea and vomiting. N Engl J Med. 2008;358:2482-2494.
32. Stein A, Voigt W, Jordan K. Chemotherapy-induced diarrhea: pathophysiology, frequency and guideline-based management. Ther Adv Med Oncol. 2010;2:51-63.
33. Hebers AH, de Haan AF, van der Velden WJ, et al. Mucositis not neutropenia determines bacteremia among hematopoietic stem cell transplant recipients. Transpl Infect Dis. 2014;16:279-285.
34. Centers for Medicare & Medicaid Services. Medicare Managed Care Manual. Benefits and Beneficiary Protections. 2016:29-30. www.cms.gov/Regulations-and-Guidance/Guidance/Manuals/downloads/mc86c04.pdf.
35. Chen HM. Patients’ experience and perceptions of chemotherapy induced oral mucositis in a day unit. Cancer Nurs. 2008;31:363-369.
36. McCullough RW. Actual duration of patient-reported mucositis: far longer than 2 to 4 weeks and may be avoidable altogether. Korean Journal of Clinical Oncology. 2016;12:1-6.
37. Fromme EK, Eilers KM, Mori M, et al. How accurate is clinician reporting of chemotherapy adverse effects? A comparison with patient-reported symptoms from the Quality-of-Life Questionnaire C30. J Clin Oncol. 2004;22:3485-3490.
38. Fallowfield L. Why patient recorded outcomes should be mandatory in and outside clinical trials to guide management of patients with metastatic breast cancer. Breast Cancer Res. 2007;9(suppl 2):S7.
39. Williams LA, Bohac C, Hunter S, et al. Patient and health care provider perceptions of cancer-related fatigue and pain. Support Care Cancer. 2016;24:4357-4363.
40. Vogelzang NJ, Breitbart W, Cella D, et al. Patient, caregiver, and oncologist perceptions of cancer-related fatigue: results of a tripart assessment survey. The Fatigue Coalition. Semin Hematol. 1997;34(suppl 2):4-12.
41. Basch E, Iasonos A, McDonough T, et al. Patient versus clinician symptom reporting using the National Cancer Institute Common Terminology Criteria for Adverse Events: results of a questionnaire-based study. Lancet Oncol. 2006;7:903-909.
42. Xu X, Barron RL, Mautner B, et al. Association between respondent- and practice-related characteristics and radiation oncology staff-reported burden on mucositis management for head and neck cancer patients. Journal of The International Society for Pharmacoeconomics and Outcomes Research. 2008;11(6). Abstract PCN96.
43. Chi KH, Chen CH, Chan WK, et al. Effect of granulocyte-macrophage colony-stimulating factor on oral mucositis in head and neck cancer patients after cisplatin, fluorouracil, and leucovorin chemotherapy. J Clin Oncol. 1995;13:2620-2628.
44. Herrmann T, Jakubek A, Trott KR. The importance of the timing of a gap in radiotherapy of squamous cell carcinomas of the head and neck. Strahlenther Onkol. 1994;170:545-549.
45. Withers HR, Taylor JM, Maciejewski B. The hazard of accelerated tumor clonogen repopulation during radiotherapy. Acta Oncol. 1988;27:131-146.
46. Tarnawski R, Fowler J, Skadowski K, et al. How fast is repopulation of tumor cells during the treatment gap? Int J Radiat Oncol Biol Phys. 2002;54:229-236.
47. McCullough RW. ProThelial (Polymerized cross-linked high potency sucralfate): medical device therapy for treatment and prevention of mucositis. European Journal of Research in Medical Sciences. 2014;2:30-58.
48. McCullough RW. A 66 patient multi-institution phase IV post-authorization surveillance of ProThelial (high potency polymerized cross-linked sucralfate) – single agent efficacy for the prevention and rapid reversal of chemo-radiation induced oral, esophageal and intestinal mucositis. British Journal of Medicine & Medical Research. 2015;10:1-17.
49. McCullough RW. Single agent anti-mucositis protocol for oral and gastrointestinal mucositis and other implications on current concepts regarding chemoradiation induced mucositis and its management from a phase IV post-market surveillance of ProThelial – high potency polymerized cross-linked sucralfate (HPPCLS). European Journal of Oncology Pharmacy. 2015;9:1-11.
50. Slutsky J. When should observational studies be used for decision-making, or does the emperor have no clothes? Agency for Healthcare Research and Quality. www.ispor.org/meetings/neworleans0513/releasedpresentations/IP9-Slutsky.pdf. May 2013. Accessed September 5, 2017.
51. McCullough RW. Single agent anti-mucositis protocol now a possibility. 66 patient multi-institution phase IV post-market surveillance of ProThelial (high potency polymerized cross-linked sucralfate). Support Care Cancer. 2015;23(suppl 1):S114-S115. Abstract 10-26-P.
52. Kashimura K, Ozawa K. Sucralfate Preparations. US Patent 5,968,906. October 19, 1999.
53. Giesing D, Lanman R, Runser D. Absorption of sucralfate in man. Gastroenterology. 1982;82:1066. Abstract.
54. Allain P , Mauras Y, Krari N, et al. Plasma and urine aluminium concentrations in healthy subjects after administration of sucralfate. Br J Clin Pharmacol. 1990;29:391-395.
55. Profile: Sucralfate Risk. www.mattilsynet.no/kosmetikk/stoffer_i_kosmetikk/risk_profile_sucralfate_03.11321/binary/Risk%20Profile%20Sucralfate%2003. Accessed April 12, 2017.
56. Kouloulias V, Asimakopoulos C, Tolia M, et al. Sucralfate gel as a radioprotector against radiation induced dermatitis in a hypo-fractionated schedule: a non-randomized study. Hippokratia. 2013;17:126-129.
57. World Health Organization. Handbook for Reporting Results of Cancer Treatment. Geneva, Switzerland: World Health Organization; 1979:15-22. http://apps.who.int/iris/bitstream/10665/37200/1/WHO_OFFSET_48.pdf.
58. Cox JD, Stetz J, Pajak TF. Toxicity criteria of the Radiation Therapy Oncology Group (RTOG) and the European Organization for Research and Treatment of Cancer (EORTC). Int J Radiat Oncol Biol Phys. 1995;31:1341-1346.
59. Elting LS, Keefe DM, Sonis ST, et al. Patient-reported measurements of oral mucositis in head and neck cancer patients treated with radiotherapy with or without chemotherapy: demonstration of increased frequency, severity, resistance to palliation, and impact on quality of life. Cancer. 2008;113:2704-2713.
60. Franco P , Martini S, Di Muzio J, et al. Prospective assessment of oral mucositis and its impact on quality of life and patient-reported outcomes during radiotherapy for head and neck cancer. Med Oncol. 2017;34:81.
61. Hensley ML, Hagerty KL, Kewalramani T, et al. American Society of Clinical Oncology 2008 clinical practice guideline update: use of chemotherapy and radiation therapy protectants. J Clin Oncol. 2009;27:127-145.
62. Peterson DE, Bensadoun RJ, Roila F; ESMO Guidelines Working Group. Management of oral and gastrointestinal mucositis: ESMO clinical recommendations. Ann Oncol. 2009;20(suppl 4):174-177.
63. Harris DJ, Eilers J, Harriman A, et al. Putting evidence into practice: evidence-based interventions for the management of oral mucositis. Clin J Oncol Nursing. 2008;12:141-152.
64. Clarkson JE, Worthington HV, Eden OB. Interventions for treating oral mucositis for patients with cancer receiving treatment. Cochrane Database Syst Rev. 2007;(2):CD001973.
65. Worthington HV, Clarkson JE, Eden OB. Interventions for preventing oral mucositis for patients with cancer receiving treatment. Cochrane
Database Syst Rev. 2007;(4):CD000978.
66. Somerfield M, Padberg J, Pfister D, et al. ASCO clinical practice guidelines: process, progress, pitfalls, and prospects. Classic Papers Curr Comments. 2000;4:881-886.
67. Bhatt V, Vendrell N, Nau K, et al. Implementation of a standardized protocol for prevention and management of oral mucositis in patients undergoing hematopoietic cell transplantation. J Oncol Pharm Pract. 2010;16:195-204.
68. Howick J, Friedemann C, Tsakok M. et al. Are treatments more effective than placebos? A systemic review and meta-analysis. PLoS One. 2013;8:e62599.
69. Wood L, Egger M, Gluud LL, et al. Empirical evidence of bias in treatment effect estimates in controlled trials with different interventions and outcomes: meta-epidemiological study. BMJ. 2008;336:601-605.
70. Glasziou P , Chalmers I, Rawlins M, et al. When are randomized trials unnecessary? Picking signal from noise. BMJ. 2007;334:349-351.
71. Guyatt GH, Oxman AD, Kunz R, et al. What is “quality of evidence” and why is it important to clinicians? BMJ. 2008,336:995-998.
72. Thompson DC, Rivara FP, Thompson R. Helmets for preventing head and facial injuries in bicyclists. Cochrane Database Syst Rev. 2000;(2):CD001855.
73. Cannegieter SC, Rosendaal FR, Briet E. Thromboembolic and bleeding complications in patients with mechanical heart valve prostheses. Circulation. 1994;89:635-641.
74. Bonow RO, Carabello BA, Chatterjee K, et al. ACC/AHA 2006 guidelines for the management of patients with valvular heart disease: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines (Writing Committee to Revise the 1998 Guidelines for the Management of Patients with Valvular Heart Disease); developed in collaboration with the Society of Cardiovascular Anesthesiologists; endorsed by the Society for Cardiovascular Angiography and Interventions and the Society of Thoracic Surgeons. J Am Coll Cardiol. 2007;49:e1-e148.
75. Velentgas P , Dreyer NA, Nourjah P , et al, eds. Developing a Protocol for Observational Comparative Effectiveness Research: A User’s Guide. AHRQ Publication No. 12(13)-EHC099. Rockville, MD: Agency for Healthcare Research and Quality; January 2013. www.ncbi.nlm.nih.gov/books/NBK126190.