There is a growing cancer survivor population in the United States in need of diverse, multidisciplinary healthcare providers competent in addressing their complex healthcare needs. The National Cancer Survivorship Resource Center, a collaboration of the American Cancer Society, The George Washington University Cancer Center, and the CDC launched the Cancer Survivorship E-Learning Series for Primary Care Providers (E-Learning Series) in 2013 to address interprofessional provider learning needs on cancer survivorship. Evaluation of the E-Learning Series showed increased self-reported confidence in learning objectives for every module for primary care and oncology learners. The average change in confidence for primary care providers ranged from 0.61 (SD = 0.77) to 1.10 (SD = 0.90) and for oncology providers from 0.63 (SD = 0.62) to 0.90 (SD = 0.74). Primary care providers had statistically significant differences in confidence improvements compared with oncology providers in modules 1, 2, and 9. Over half of primary care providers (52.3%) reported that they needed more information to implement skills and strategies in practice. Overall, the evaluation showed efficacy of the E-Learning Series in improving both primary care and oncology providers’ confidence in cancer survivorship care and highlighted the need for additional education and training in this area.
The nearly 17 million cancer survivors alive in the United States today have specific healthcare needs that require ongoing communication and care coordination among primary care providers and oncology specialists.1 Yet primary care and oncology providers lack sufficient education and training on cancer survivorship care.2
To address this need, the Cancer Survivorship E-Learning Series for Primary Care Providers (E-Learning Series) was launched in 2013 as part of the National Cancer Survivorship Resource Center, a 5-year collaboration between the American Cancer Society, The George Washington (GW) University Cancer Center, and the CDC. The E-Learning Series is an online, self-paced, 10-module continuing education program available to health professional learners at no cost. Modules cover a variety of topics, including managing late and long-term effects, addressing health behaviors, addressing social and emotional needs, coordinating interprofessional care, and providing evidence-based clinical care management. Each nonsequential module contains two 30-minute presentations delivered by subject matter experts, an audio vignette from a cancer survivor, and resources for the learner.
The development, measures, and initial outcomes of the E-Learning Series have been reported previously.3 Here we evaluate within and between group differences in self-reported confidence gains for primary care versus oncology learners across all learning objectives of the series.
Methods
Study Population
From April 2013 to December 2017, 1656 learners voluntarily enrolled and participated in the E-Learning Series. For this analysis, only learners who self-identified as having an oncology or primary care specialty were included. Eligibility criteria also included fully completing at least 1 module’s pre- and postassessments and practicing within the United States (n = 1138).
Data Collection and Statistical Analysis
At the beginning of each module, learners completed an optional demographic survey followed by a preassessment that asked about confidence in meeting each module’s learning objectives on a 5-point Likert scale (strongly disagree to strongly agree). After completing the module, learners took a required postassessment that repeated the same confidence items and asked additional questions on self-reported learning gains as well as intention to implement new knowledge and skills. SurveyMonkey was used to collect data from 2013 to 2015, and in 2015 data collection moved to a learning management system.
Descriptive statistics and paired samples t tests were examined using STATA/IC 14.2 to compare oncology and primary care provider differences in confidence from pre- to postassessment. Independent samples t tests were performed to assess whether pre- and posttest differences were statistically significantly different between learner groups for each module (P <.05).
Results
A majority of learners (86.6%) practiced in oncology (n = 985), whereas less than one-quarter of learners (13.4%) practiced in primary care (n = 153). The majority of learners identified as female (oncology: 95.5%; primary care: 79.7%), white (oncology: 88.0%; primary care: 73.7%), and non-Hispanic (oncology: 90.3%; primary care: 81.0%). Most learners were nurses (oncology: 85.7%; primary care: 46.3%); however, physicians (primary care: 44.3%; oncology: 2.4%), social workers (oncology: 2.5%; primary care: 0.7%), and healthcare administrators (oncology: 2.4%; primary care: 1.3%) were also included.
Learners in oncology had a much higher frequency of participation for every module. For example, Module 10 oncology specialist participation was n = 181 compared with n = 13 for primary care providers, and Module 1 oncology specialty participation was n = 757 compared with n = 127 for primary care. Since modules were released over the course of several years, it was expected that a greater number of learners from both groups would have completed Module 1 compared with Module 10.
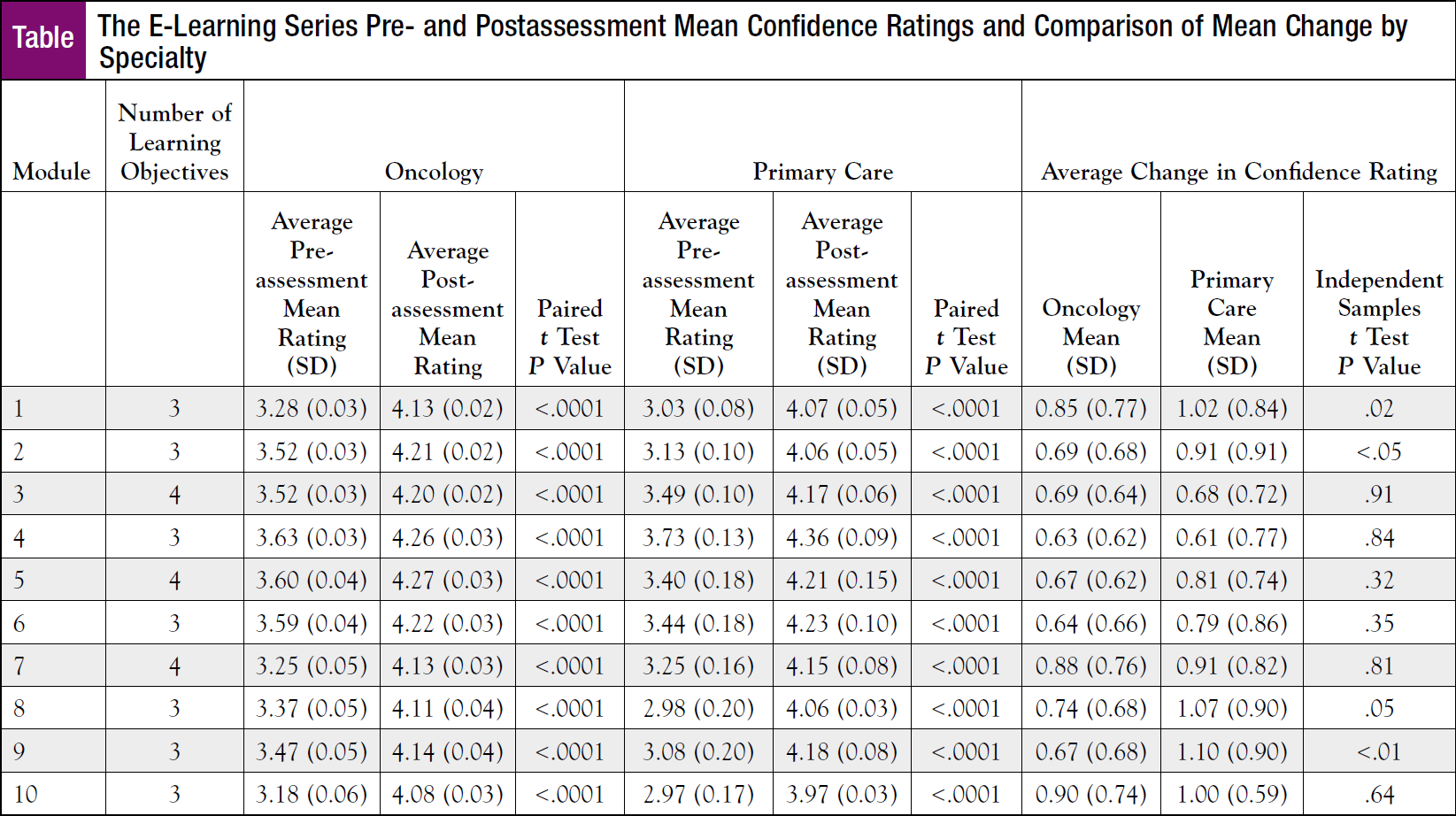
Regarding confidence to meet learning objectives at preassessment, most primary care and oncology providers rated confidence “neutral” (primary care provider means ranged from 2.97 [SD = 0.17] to 3.73 [SD = 0.13]; oncologist means were 3.18 [SD = 0.06] to 3.63 [SD = 0.03]). At postassessment, learners reported confidence in meeting learning objectives (primary care provider means ranged from 3.97 [SD = 0.03] to 4.36 [SD = 0.09]; oncologist means were 4.08 [SD = 0.03] to 4.27 [SD = 0.03]). Mean change from pre- to postassessment was statistically significant (P <.0001) for all modules for both groups.
The average change in confidence ratings for primary care providers ranged from 0.61 (SD = 0.77) to 1.10 (SD = 0.90); the average change for oncology providers ranged from 0.63 (SD = 0.62) to 0.90 (SD = 0.74). Both primary care and oncology providers had the lowest mean increase from pre- to postassessment for “Module 4: The Importance of Prevention in Cancer Survivorship: Empowering Survivors to Live Well.” The largest increase for primary care providers was for “Module 9: Spotlight on Breast Cancer Survivorship: Clinical Follow-Up Care Guideline for Primary Care Providers,” and for oncology providers, “Module 10: Spotlight on Head and Neck Cancer Survivorship: Clinical Follow-Up Care Guideline for Primary Care Providers.” Primary care providers had statistically significant self-reported higher confidence to meet learning objectives for “Module 1: The Current State of Survivorship Care and the Role of Primary Care Providers” (P = .02), “Module 2: Late Effects of Cancer and Its Treatments: Managing Comorbidities and Coordinating with Specialty Providers” (P <.05), and “Module 9: Spotlight on Breast Cancer Survivorship: Clinical Follow-Up Care Guideline for Primary Care Providers” (P <.01). No other statistically significant differences were observed. All pre- to postassessment means by specialty and comparison of confidence ratings are presented in the Table.
At postassessment, most oncology (91.9%) and primary care providers (90.9%) either agreed or strongly agreed that their knowledge was enhanced, that they gained new skills/strategies they could apply to practice (85.4% oncology, 84.3% primary care), and that they planned to implement skills/strategies into practice (77.5% oncology, 79.1% primary care). Yet, more than half (52.3%) of primary care providers indicated they needed additional information before being able to implement skills/strategies into practice compared with almost one-third (30.2%) of oncology providers.
Discussion
The E-Learning Series reached diverse types of healthcare professionals from all regions of the United States. Strategies are needed to reach community health centers, rural settings, racial/ethnic minorities, and male participants. Also, despite the intended audience of primary care providers, most learners came from an oncology specialty. This suggests substantial interest in survivorship care from the oncology community as well as challenges in promoting disease-specific education to primary care providers.
Providers in both oncology and primary care settings reported statistically significant gains in confidence across all modules. Learners of both groups had the lowest preassessment confidence rating for the module on head and neck cancer survivorship (Module 10), a rarer cancer type that comes with complex survivorship late and long-term effects. Primary care providers had lower preassessment ratings at baseline for the module on breast cancer (Module 9) but statistically significantly greater gains in confidence compared with oncology counterparts at posttest. This makes sense because oncology providers would have greater curricular exposure and experiential knowledge in breast cancer than their primary care counterparts. The increase in primary care learner confidence in this area suggests that the E-Learning Series met a critical learning gap in survivorship knowledge for this high-prevalence cancer.
It is unsurprising that oncology specialists had higher preassessment ratings across most modules compared with primary care providers. The one exception was Module 4 on prevention and wellness behaviors: primary care providers had higher preassessment ratings. The statistically significantly higher change scores among primary care providers compared with oncology counterparts for modules 1 and 2 indicate that the E-Learning Series narrowed confidence gaps between specialties in understanding survivorship care basics, the role of primary care providers, and late effects of cancer.
More than half of primary care learners indicated that more information was needed to implement new knowledge in practice. Adult learning requires ongoing education through mixed modalities. Mixed media, interactive in-person education, peer-to-peer learning, and interprofessional role-play for shared care of cancer survivors could be strategies to further explore to help further bridge the learning gap in cancer survivorship care for diverse healthcare professionals.
There were several limitations of this study. First, there was high potential for selection bias by the following factors: motivation to learn, connectedness to professional networks, and degree of computer savvy. Second, confidence ratings are by nature subjective. Responses could be influenced by social desirability. Third, we did not control for covariates outside of professional role. Finally, all findings should be interpreted with caution given the small sample size of primary care providers, particularly for modules 5, 8, 9, and 10.
Conclusion
The E-Learning Series generated confidence gains in cancer survivorship topics among learners across specialties and professions. It also highlighted gaps in knowledge and training among interprofessional providers in cancer survivorship care. The results support the ongoing need for education in survivorship care training for interprofessional healthcare providers.
Acknowledgments
The Cancer Survivorship E-Learning Series for Primary Care Providers (E-Learning Series) was developed through the National Cancer Survivorship Resource Center, a collaboration between the American Cancer Society (ACS), The George Washington University (GW) Cancer Center, and the CDC, funded by a 5-year cooperative agreement (#5U55DP003054) from the CDC. The E-Learning Series and the resulting evaluation is currently supported through a cooperative agreement (#5NU58DP006461-01) from the CDC. The GW Cancer Center would to like to thank the ACS and the CDC for their ongoing partnership.
Funding details: This work was supported by the CDC under cooperative agreements #5U55DP003054, #5U38DP004972 and #5NU58DP006461-01.
References
- Institute of Medicine and National Research Council. From Cancer Patient to Cancer Survivor: Lost in Transition. Washington, DC: The National Academies Press; 2005.
- Lester JL, Wessels AL, Jung Y. Oncology nurses’ knowledge of survivorship care planning: the need for education. Oncol Nurs Forum. 2014;41:E35-E43.
- Harvey A, Zhang Y, Phillips S, et al. Initial outcomes of an online continuing education series focused on post-treatment cancer survivorship care. J Cancer Educ. 2020;35:144-150.
You can access the Cancer Survivorship E-Learning Series at gwccacademy.org.




