Breast cancer remains the most feared disease by all women, unrelated to their race, ethnicity, or age. Among major cancers, cancer of the breast is the most common cancer in women in the United States. It is the second most common cause of death and the third most frequent cancer in the world, after lung and stomach cancer, but it is by far the most common type of cancer among women worldwide.1 Globally, there are 1.3 million women diagnosed with breast cancer annually. More than 11 million of them over the next 20 years will die of this disease.2 This equates into someone being diagnosed every 29 seconds and a woman dying every 69 seconds. These statistics may actually be underreported since not all countries have tumor registries for reporting the incidence of cancers that occur within their population. There is consensus that in developing countries most breast cancer patients present at a younger age and with a more advanced stage of the disease compared with patients in developed countries.3,4 Certain difficulties and barriers to treatment are found specifically in developing countries. Resources for breast cancer treatment may be incredibly limited.5 Solutions will need to be country specific. The estimated mortality incidence ratios are generally lower in developed countries. More than 55% of breast cancer–related deaths occur in the middle- and lower-income countries.6 Educational, cultural, and logistical issues and other barriers can prevent the availability and delivery of high-quality care to underserved patients.7 Race, ethnicity, and socioeconomic status are social factors that also shape cancer outcomes.8 This article provides an in-depth look at the need for patient navigation specifically within low- and middle-income countries as it relates to having women educated, screened, diagnosed, and treated for breast cancer. Given that breast health and breast cancer patient navigation began in the United States in the early 1990s targeting underserved women, we can learn from several decades of experience and see what components may apply to other countries confronting delays in diagnosis and treatment that result in high morbidity and mortality rates.
Background, Definition, and Goals of Patient Navigation Performed by Laypeople and/or Oncology Nurse in the United States
We know from our experience in the United States that the burden of cancer is not equally distributed with respect to factors such as race and ethnicity, socioeconomic status, and nativity. These social factors can and do directly influence morbidity and mortality since they have an impact on the disease stage at diagnosis, prognosis, and clinical outcomes. A disproportionate burden of disease falls upon racial and ethnic minorities, especially those medically underserved and disadvantaged.8,9 Patient navigation in cancer care refers to individualized assistance offered to patients, families, and caregivers to help overcome healthcare system barriers and facilitate timely access to quality medical and psychosocial care. Cancer patient navigation works with a patient from prediagnosis through all phases of the cancer experience.10 Understanding the history of navigation and how it has evolved over time provides information as to how it can best be applied to the middle- and lower-income countries today. Navigators differ from other cancer support personnel in their orientation toward flexible problem solving to overcome perceived barriers to care rather than the provision of a predefined set of services.7
In the late 1970s and early 1980s, the prospective payment system (PPS) was implemented to help reduce healthcare costs related to inpatient stays.11 Each day of a patient’s hospitalization had to be medically justified for it to be a covered (ie, reimbursable) service by insurers such as Medicare, Medicaid, and other third-party payers. Utilization review (UR) nurses were employed by insurers to review medical records retrospectively and identify any days of hospitalization that lacked (apparent) medical necessity. Such days would be “carved out” of the covered services for inpatient hospital stays, causing concerns for hospitals regarding reimbursement for care. Because people other than physicians were scrutinizing the necessity of healthcare interventions, including length of hospitalizations, relationships among UR nurses, physicians, and hospitals often were adversarial.12 This process was not related to the underserved patient, yet it provided the roots and foundation for nurse navigation 2 decades later.13
By the late 1980s, the process of medical record review changed to concurrent chart review and was renamed utilization management (UM). The objective of concurrent review was to identify delays in treatment or discharge from the hospital because of inefficiencies within the healthcare system. Hospitals across the country employed their own teams of UM nurses to review medical records during patients’ hospital stays and communicate with physicians and healthcare teams when more documentation was necessary to justify additional hospital days. The UM nurses, employed by the hospitals, identified specific inefficiencies and worked with healthcare teams to improve care delivery and subsequent reimbursement by insurers for hospitalizations. These “barriers to treatment or barriers to discharge from the hospital” became the sole focus of this work.14
During the 1980s and 1990s, another type of UM nurse, hired by third-party payers, was also in hospitals. These nurses conducted independent chart reviews and evaluated care delivery and length of hospital stays. They interacted with hospital-based UM teams rather than contacting physicians directly. The most common reasons for delays in discharge and prolonged hospital stays were difficulties obtaining patient transfers to facilities with lower levels of care (eg, a skilled nursing facility or rehabilitation hospital) or delays in scheduling ancillary tests (eg, radiology tests being unavailable on weekends). Although some improvements in the efficiency of care delivery were achieved, they were not systematically applied to benefit all patients. Also, relationships among independent UM nurses, attending physicians, and hospital management often remained adversarial.15
In the early 1990s, the concept of “case management” was introduced as another way to increase the efficiency of healthcare delivery. The philosophy and application of case management were quite different from UR and UM. Case managers most often were nurses who worked directly with healthcare teams caring for specific patient populations (eg, cardiovascular accidents, oncology care, diabetes care, cardiac bypass surgery). The specific populations were identified as requiring complex or expensive care or requiring coordination of care over time. The goals of case management were to improve efficiency, increase adherence to treatment recommendations, provide links for patients to needed resources within the hospital and the local community, and ensure that care was effective, safe, and patient centered.13 Prevention of readmissions was key. Prevention of overutilization of healthcare resources in any setting was a primary goal.
Most physicians viewed nurse case managers as critical team members and the first “navigator,” keeping patients on a clinical pathway. Finally, the case manager and patient were participating with the care team. The responsibilities of oncology nurse case managers included addressing barriers to timely care delivery, facilitating communication among members of the healthcare team and the patients and families, educating patients about their illnesses and treatments, addressing psychosocial and financial issues that could impact or delay care, arranging for timely consultations, promoting adherence to cancer surveillance and medications associated with cancer treatment, and planning for the next phase of care (eg, discharge, additional services such as rehabilitation, transfer to a facility with a lower level of care, self-management at home, and/or home care).
At the same time hospitals were implementing the case manager role, third-party payers were also using case managers to ensure that care was provided in a timely and costeffective manner. Subsequent studies validated the effectiveness of case management, and the role is still in place for many insurance companies and hospitals.16 During the implementation of case management in patient care delivery, a physician at Harlem Hospital, Dr Harold Freeman, coined the phrase “patient navigation.”17 He saw that an individual, commonly a layperson from within a community, could serve as a patient navigator whose efforts could help address disparities in healthcare and improve access to care for underserved people. For example, patient navigators could help improve access to mammography for African American women and facilitate earlier diagnosis of breast cancer.17 Additionally, Freeman saw patient navigators as responsible for educating the community about the importance of cancer screening. The goal of patient navigation was to facilitate timely access to high-quality cancer care in a culturally sensitive manner for all patients.18 Concerned about the high mortality rate among breast cancer patients being seen at Harlem Hospital, he developed the concept of patient navigation, striving to reduce breast cancer mortality due to myths, cultural barriers transportation barriers, financial barriers, fear, etc. Case workers, referred to as patient navigators, were trained to do community outreach, such as arranging for transportation and eliminating other barriers to accessing screening mammograms, which proved successful in reducing mortality and morbidity from breast cancer. This approach was also replicated for other common cancers that were deemed survivable if diagnosed at an early stage.19 The use of patient navigators has continued to grow and evolve over time and still does to this day. The training and competencies for performing navigation have also developed, going beyond the lay navigator concept originally created and expanding into the fields of social work and nursing. So, though from a historical perspective patient navigation began with a focus on gaining access to screening and care among the underserved population, oncology nurse navigators—previously known as case managers, breast health educator nurses, or UM nurses—began addressing the barriers to diagnosis and treatment and eventually expanded into community outreach to help provide easier access to screening and subsequent care and treatment. This resulted in the 2 navigation processes dovetailing with one another in the early 2000s (Table).
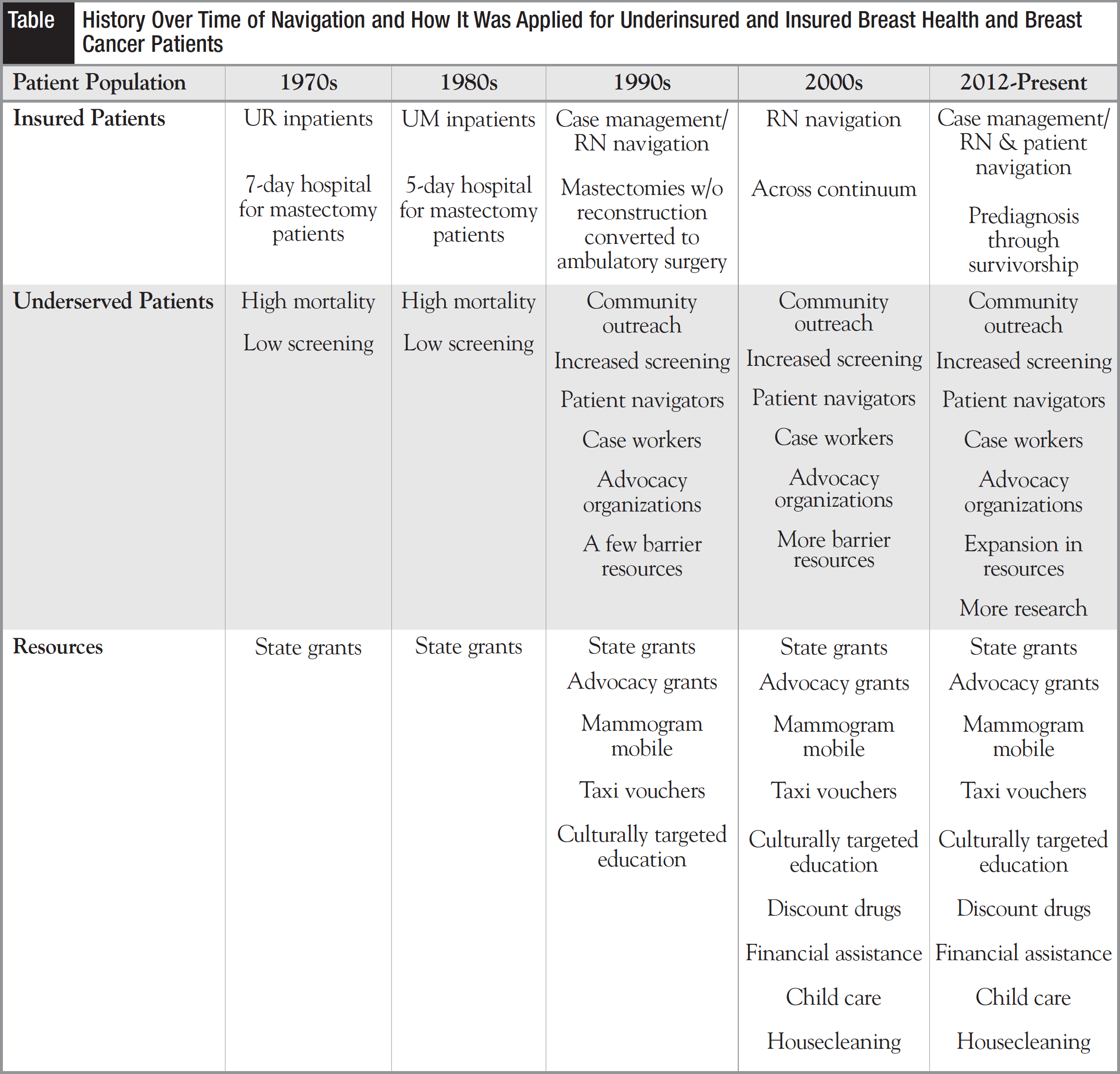
There is no universally agreed upon definition of navigation today. Most definitions and actual functions of someone performing the job have concentrated on barrierfocused identification and resolution.7 For a navigation program to be successful in fulfilling its goals, it must encompass the navigation processes beginning with community outreach and awareness, screening, prediagnosis, diagnosis, all phases of treatment, survivorship, surveillance, healthy lifestyle promotion, and for those who succumb to this disease, end-of-life issues. As it specifically relates to middle- and lower-income countries where resources are limited, navigation must include some components of UM, case management, education, community outreach, barrier assessment, resource referral, and psychosocial support.13 Not all of these functions, however, need to be performed by 1 person, such as a nurse. Different individuals may be employed to perform specific servicefocused tasks, based on their training, knowledge, and expertise. This means that UM also needs to be a core component of identifying the correct individual to fulfill specific role(s), being watchful to not overutilize or underutilize healthcare resources, including manpower resources. There may be case managers, nurse navigators, lay navigators, counselors, community health workers, doctors, nurse practitioners, and others, including volunteers from the community.7 It is of importance to note, too, that particular services provided by navigators depend on the barriers they identify and the strategies they use to eliminate or reduce those barriers.7,19,20 Community outreach workers (laypersons) may focus on adherence to screening or the practice of certain lifestyle behaviors to reduce cancer risk, whereas a nurse navigator may be directly involved in the care of the patient and take a proactive role in assessing her needs and helping to ensure that she receives treatment.
The navigation program Dr Freeman established at Harlem Hospital focused specifically on high volumes of stage III and IV breast cancer patients with a known poor prognosis who were part of a community with low-income and medically underserved minorities. That program, developed in the early 1990s, targeted perceived barriers caused by mistrust as well as healthcare system complexity by training lay people to provide one-on-one follow-up and case management.19
Over time and with the support of grant funding, others have also taken on the charge of addressing disparities as a way to increase early detection and therefore increase breast cancer survival. Some programs have focused on educational outreach and screening referrals as a way to improve access for patients. Other programs have utilized bilingual and bicultural navigators to address perceived barriers associated with language and culture.21 What has been learned from the various navigation models in the United States is that navigation is associated with improved rates of screening and follow-up, lower clinical stage at presentation and initial diagnosis, and greater patient satisfaction.22
The Importance of a Comprehensive and Tailored Navigation Program
Cancer patient navigation can and should take on different forms in different communities, as dictated by the needs of the patients, their family, and their community. Within each patient navigation program, the healthcare system, community system, navigators, consumers, and related entities should ensure that they have agreed upon how patient navigation will be defined and operationalized.23
Patient navigation needs to be provided by culturally competent professionals or peers in a variety of settings, depending on the complexity of the situation. The navigator can work within the healthcare system or outside the healthcare system but in close collaboration with providers and the community. The design of the cancer patient navigation system is engineered to be directed by, and to meet, the needs of the patient and the family in the context of the community and the healthcare environment.23
As there were evolving efforts implemented to reduce overutilization of medical resources of insured patients while still helping to ensure that patients received the care they needed in the right and most cost-effective medical setting, there were also efforts taking place to focus on health disparities with a goal to promote earlier detection that would save more lives. As we look at the needs of middle- and low-income countries, both processes, case management and patient navigation, will be needed for a program to be successful. Given the limited resources for screening, diagnosis, and treatment currently available in many low- and middle-income countries, it is critically important to develop a breast cancer program that encompasses education about breast cancer awareness and promotes early detection, as well as helps ensure appropriate utilization of medical resources. Ironically, this combines the theories of utilization management, case management and community outreach, patient education, barrier assessment, resource referrals, and psychosocial support together into 1 navigation program.
A report by the Trans-Health and Human Services Cancer Health Disparities Progress Review Group identified patient navigation programs as an important resource for the elimination of cancer health disparities in the United States.20 The goal of patient navigation to reduce health disparities in the United States was adopted by the National Cancer Institute in 2006. The Cancer Patient Navigation Act was created to help ensure that patients with cancer received high-quality, coordinated care. Navigators (without the Act defining training or educational requirements to serve in these roles) were to guide patients through the physical, emotional, and financial challenges that come with a cancer diagnosis. Although the actual Cancer Patient Navigation Act became law in 2005, funds were not invested into the development and implementation of navigation programs until 2009. What cancer centers saw as most important was to provide a navigation process to all patients, unrelated to their socioeconomic status.10 At a global level, similar navigation acts are needed to further help launch improvements in breast cancer diagnosis and treatment around the world.
The Navigator Role in Breast Cancer Care Today
The mission of patient navigation in breast cancer care has extended beyond addressing the needs of underserved populations or facilitating screening and diagnosis; its goal is to navigate all patients throughout the cancer continuum. Begining in the mid to late 1990s, funding for breast cancer patients came from cancer organizations and other advocacy groups (eg, Avon Foundation, American Cancer Society, Susan G. Komen for the Cure, National Breast Cancer Foundation). Through grant-supported navigation programs, increased numbers of underserved patients have been reached and navigated through their diagnosis and treatment of breast cancer.24,25
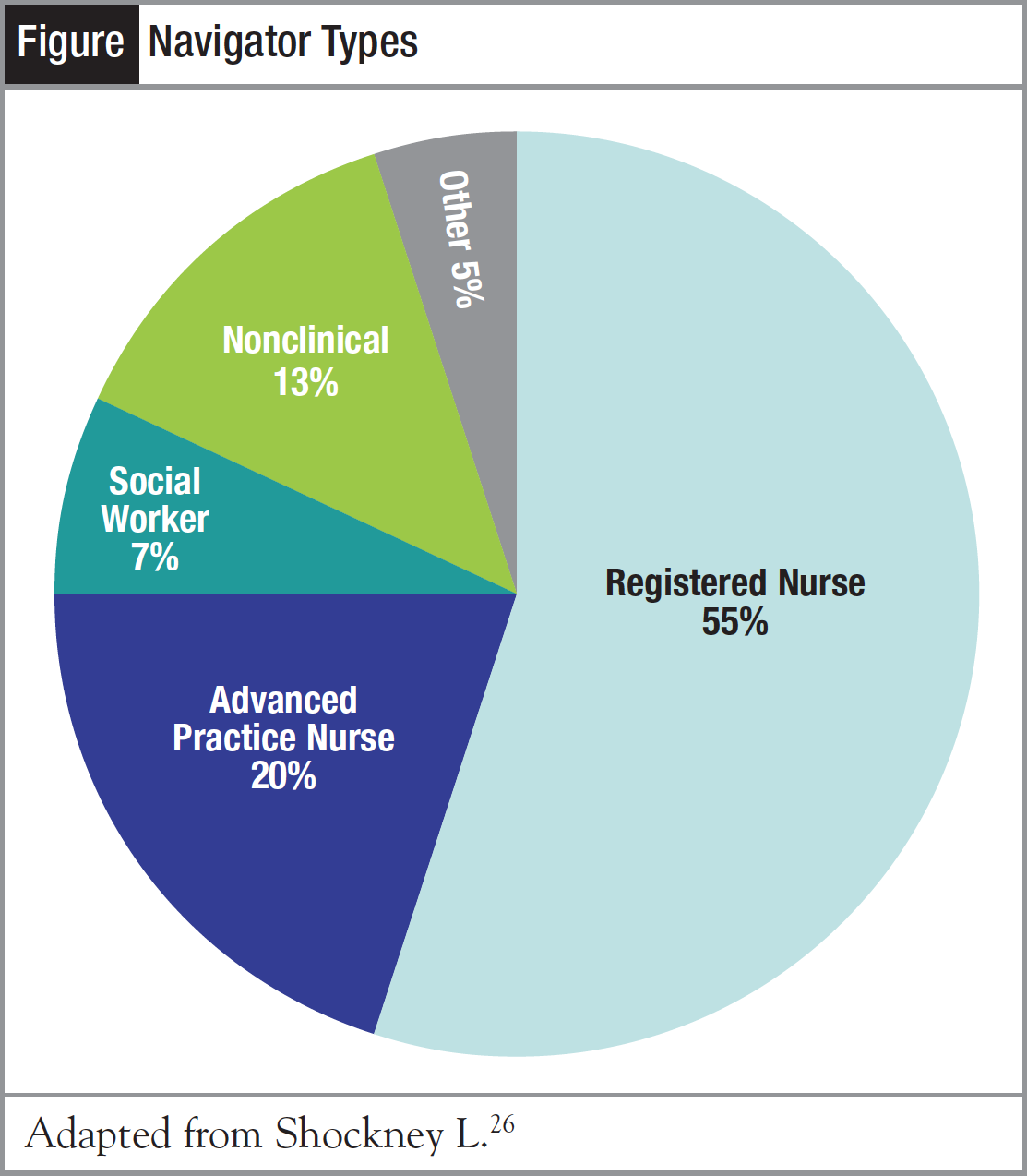
In most cases, the role of patient navigator has been filled by nurses, but in some cases, by social workers and/or laypeople (Figure).26 In some settings, the roles of case manager and patient navigator are blended into 1 job. Due to fragmentation in care, driven greatly by third-party payers and where they do or do not approve diagnostics and treatment to be delivered, the need for coordination of cancer care continues to be a priority for nurse navigators. Without this process, breast cancer patients may not receive treatment in keeping with the National Comprehensive Cancer Network (NCCN) treatment guidelines, which describe the most evidence-based treatment aligned with good clinical outcomes. Treatment in keeping with the NCCN guidelines is achievable for underserved patients in the United States when they are given access to cancer centers for their diagnosis and treatment. When we look at the needs of underserved women in middle- and low-income countries, however, it may not be realistic to expect them to receive treatment that matches the evidence-based standard of care. We need to look at what is feasible and determine how effective treatment may be achieved based on the resources currently available, as we strive to obtain or create the resources needed to help develop appropriate treatment in the future.
Learning from Navigation Efforts Conducted in the United States with the Undeserved Population
When we are discussing minorities in the United States, we are usually referring to African American, Hispanic/ Latino, and the American Indian/Alaska Native in our society. And underserved women are those who have a decreased income and socioeconomic status, lower education level, commonly lack health insurance, and have limited access to healthcare in general. These patient populations are particularly challenging when facing the diagnosis and treatment of breast cancer.
Although it is known that underserved women continue to present with later stage breast cancer (stages III and IV), it has become apparent through laboratory research that not all breast cancers, even when comparing stage for stage, are alike.27 There are biological differences among subsets of breast cancer patients from various cultures and ethnicities that warrant further research so that personalized treatment plans, based on targeted biologic therapies, can improve survival for minority and underserved women. Couple this issue with cultural differences and it’s clear that the navigation needs of these specific patient populations require special navigation skills and knowledge, with the goal for women diagnosed with breast cancer to become long-term survivors who are living a healthy and happy life.
Barriers that prevent optimal breast cancer treatment for minority and underserved populations have been studied with some consistency and depth over the last 3 decades. Low rates of adjuvant therapy being successfully administered to patients as well as long delays in initiation of treatment contribute to higher mortality rates for these women.28
A review of the literature regarding barriers for these patient groups indicates that barriers are related to 3 categories—patient; physician; healthcare system. Let’s look at each category.29
Patient-Related Barriers
These barriers include low socioeconomic status, lower level of education, limited or no access to healthcare, and cultural or belief systems issues. A low socioeconomic status has been noted to directly and independently contribute to a higher mortality rate.28 Among African American women who have breast cancer, the percentage of patients who live at the poverty level is more than twice as high as that of white women who have this disease (29% vs 12%).8,30 Similar data have been noted among Hispanics, Native Americans, and women living in rural areas of the United States.31
Women who did not complete high school have a lower compliance rate with screening mammography than those who did graduate from high school. Also, the need to maintain a steady job, take care of children, and minimize any unnecessary expenses (such as a copayment) all factor into the problems navigators experience with getting patients to do the right thing for themselves.
We should never underestimate the unique cultural and belief systems that prevent a timely diagnosis and subsequent treatment. There are women who believe that by ignoring the problem (a breast mass), the symptoms will go away on their own. Spiritual beliefs can steer a patient into feeling convinced that a higher power will heal her, therefore she believes she does not need cancer treatment. It is common in Hispanic and African American communities to feel that family comes before all other things. This too can result in delays in diagnosis and treatment. And of course language barriers are a hindrance when we are not able to explain to the patient why early diagnosis and completion of treatment are so important.
Physician-Related Barriers
Communication, personal bias, limited education—these barriers are a little less obvious. Cultural differences can make the communication process difficult and frustrating. Some physicians don’t recommend mammography screenings due in part to assumptions that these patient populations are so noncompliant that it isn’t worth the time to try to persuade the patients to comply. Physicians in rural areas may not be up to date regarding treatment (ie, lumpectomy is equal to mastectomy from a survival perspective).32,33
Healthcare System–Related Barriers
The biggest barrier is having to deal with patients who are uninsured or underinsured. Lower income (poverty level) limits the access to needed resources for receiving routine cancer screening and wellness care. If a patient can schedule a screening mammogram, the wait time may be long. The patient, who may have been willing originally to come in for screening, may change her mind and lose the inspiration to use healthcare access.29
The Challenge for Navigating Women for Breast Health and Breast Cancer Care in Middle- and Low-Income Countries
The role of the cancer patient navigator is to identify and eliminate barriers that prevent individuals from getting the right care, at the right time, and by the right person. Whether that involves educating a person about the need for timely screening, reducing fear and nullifying myths about breast cancer, helping someone access health insurance or low-cost screenings, finding transportation to treatment, arranging alternate child care while a parent receives care, helping a person access information about treatment options, or connecting to a support group, the navigator helps patients find and get the care they need.23 By reducing or eliminating barriers to care, navigators help individuals receive the screening and diagnostic tests they require. With early identification of a cancer, and early treatment, morbidity and mortality can be reduced.23
When we consider applying this concept in middle- and low-income countries, we must recognize that the right care, at the right time, and by the right person may need to be altered initially until the needed resources are created or provided. Lower levels of health literacy or education that may contribute to fears of cancer screening or diagnosis, cultural orientations that contribute to lack of trust of doctors or medical institutions, attitudes of fatalism about cancer, logistical barriers, and other cultural barriers can be difficult to surmount.7 Navigation programs seek to reduce these disparities 1 barrier at a time, individually for each patient as well as systematically for the population seen and treated.
It is known from our experience in the United States that a variety of barriers impede prevention, screening and early detection, follow-up of suspicious findings, and aggressive treatment of disease among the underserved population. Lower levels of education or health literacy, fears of screening or diagnosis, cultural orientation or fatalistic views of cancer, logistics associated with access to care and lack of transportation, child-care needs, clinic schedules, living in a rural setting, and other barriers, as well as not reporting a warning sign of a breast health problem they self-identify, result in women not getting screened.34
The most common barriers experienced by underserved patients relate to10:
- Finances and economics
- Language and culture
- Communication
- Healthcare system complexity and/or fragmentation
- Transportation
- Bias based on culture/race/age
- Fear
Case Study: Barriers to Treatment in South Africa
A study conducted in Capetown, South Africa, demonstrated some of the various barriers described above.35 Only 6% of black breast cancer patients accepted and received treatment. There were several different barriers identified that included cultural, religious, and social factors. Specific reasons given for refusing treatment included (1) The patient believes that she has been poisoned by an evil sorcerer and that she requires special indigenous African medicines. She believes that Western treatment such as surgery will cause the cancer to spread and kill her; (2) Decision-making may involve various family members, including older, more conservative family members; (3) There are financial barriers. Patients are not keen to be viewed as sick because it will impact their ability to work and take care of their children. They don’t want to be labeled by the community as being a person with cancer.4,35
Case Study: Nigeria's Challenges in Managing Breast Cancer
A team of researchers set out to investigate the challenges, severity, and other factors that influenced the clinical outcomes of breast cancer patients.36 They focused specifically on a teaching hospital within Nigeria. The study took 8 years to complete (1996-2003) and provided some key information that served as baseline data from which to measure improvements in the care delivery system. The mean duration of symptoms a woman noted was 11.2 months (9 days-7 years). Pain in patients (47%) was reported as the most common symptom bringing them into the healthcare system. Localized cancer was found in the upper outer quadrant of the breast 40% of the time, whereas whole breast involvement occurred 26% of the time. Advanced breast cancer (defined as having loco-regional features) was present 74% of the time. Thirty-nine percent of women had fungating tumors, and metastatic disease was clinically evident 13% of the time. Eighty percent of patients had stage III or IV breast cancer at the time of initial diagnosis. Treatment compliance was poor with the majority of patients dead or lost to follow-up within a year of diagnosis.36
In determining the causes of late presentation, it was learned that the problem was multifactorial in nature and included religious beliefs, prolonged denial, lack of awareness, and ill-informed perceptions about breast cancer. Some patients utilized alternative means of treatment, most specifically herbal and spiritual treatment options that were readily available to them. There was also lack of knowledge among the healthcare providers about breast cancer and an environment within the hospital itself that was not inviting and caring. The number 1 barrier however was fear of mastectomy surgery.36,37
It was confirmed as an outcome of this study that extensive staging workups, including bone scans, CT scans, xrays, and MRIs, did not contribute to changing the management of patients with early stage or advanced stage breast cancer. This was an important utilization management issue to discover. Advanced breast cancer posed a huge clinical management problem due to the extensiveness of the lesions, which oftentimes were not operable and commonly were infected and necrotic. The conclusion these researchers drew was that early detection of breast cancer may be quite difficult in developing counties as it requires early diagnosis through screening or women reporting symptoms very early on when tumors are small. The Nigerian doctors reported that the prerequisite for early diagnosis would be the implementation of appropriate support for women seeking care that would include appropriate and easy access to affordable diagnostic tests and treatments, which are commonly lacking. Culturally sensitive and appropriately targeted education about breast cancer, tailored to the specific needs of the population, was required and considered to be a woman’s right to receive.36
Steps and Issues to Consider When Designing and Implementing a Breast Cancer Navigation Program in Developing Countries: Start with a Needs Assessment and Gap Analysis
A needs assessment is an important activity to perform before an effective and efficient navigation program can be implemented. It identifies for the oncology team the specific needs of patients while providing a sense of direction and a set of priorities. A needs assessment will provide baseline information needed before the team embarks on the construction of a comprehensive navigation program to serve the needs of women in these environmental and cultural settings. This can be challenging, as there may be limited information available. Knowing the population base and some information about them is useful however. This includes information about the current incidence of breast cancer; some volume information by stage, age distribution, and treatment options currently available; as well as treatment options actually utilized. The gap analysis provides information regarding where there are holes in the system that need to be filled, whether they be in screening, treatment, barriers to care, or other resources missing or limited currently.
Although it is oftentimes difficult to perform a comprehensive needs assessment, remembering that cancer impacts a patient’s life will enable the people conducting the needs assessment to include a variety of issues associated with patient support needs. Unaddressed needs result in adverse outcomes.38
Understanding the culture and belief systems is part of the information needed from the outset and provides the beginning steps to identification of the barriers to screening, diagnosis, and treatment. What do women value? (eg, making sure they are there for their children and have food to feed them).What do men value? (eg, being able to provide shelter for their families).
There are a variety of validated needs assessment tools available. They include but are not limited to the following38:
- Cancer Care Monitor
- Concerns Checklist
- Needs Evaluation Questionnaire
- Needs Near the End-of-Life Care Screening Tool
- Oncology Clinic Patient Checklist
- Patient Needs Assessment Tool
- Problems and Needs in Palliative Care Questionnaire
- Problem Checklist
- Supportive Care Needs Survey
- Sheffield Profile for Assessment and Referral to Care
- Symptoms and Concerns Checklist
- Psychosocial Needs Inventory
Recruit a trained, experienced breast cancer nurse navigator to take a leadership role in overseeing the development and implementation of the navigation program.
Formulate a list of barriers to diagnosis and treatment and what resources, if any, currently exist or are needed to overcome these barriers (eg, transportation, healthcare myths, no radiation facilities, no mammography equipment, outdated equipment, no one trained in reading the results of screening or diagnostic tests).
What current method of communication is available to reach people within each community and across the country? How effective have these methods been in reaching women to date about any issues of importance (ie, other health-risk issues)? What social gatherings occur and when? What telecommunications methods are available?
What screening is currently available and how accessible is it for women? If transportation is a major barrier, is it possible to offer a mobile screening and diagnostic program?
What methods are currently used for diagnosing breastcancer (eg, excisional biopsies vs core biopsies vs large fungating tumors that are obvious to diagnose)?
What pathology services are available and what is the completion time? Also, what is the level of accuracy and specificity?
Identify what breast cancer medical personnel exist, where they are located, and what their specialties are. Is there adequate staffing of these medical personnel? Are they clustered in 1 area of the country? Do they work currently as a multidisciplinary team or as totally independent disciplines? What volume of patients are they currently seeing? Are they trusted individuals within the community? Something that has also been learned from exploring the needs in developing countries is that simple technology transfer is not very useful and that different treatment protocols will likely need to be developed. These eventual treatment protocols will need to come from research initiatives. Referral guidelines and clinical care guidelines must be developed in a way to be auditable. Most breast cancer treatment does not require a high-level physician specialist; the best example perhaps being treatment with hormonal therapies.39
Identify what treatments are available and where and to what degree treatment is currently utilized. This includes surgical options, chemotherapy drugs, radiation equipment, reconstruction/flap coverage options, hormonal therapies, biologic targeted therapies, pain medications, rehabilitation services, nursing care, and palliative care. What financial barriers exist to obtaining treatments?
Identify locations where treatment can be administered. In countries with limited resources, chemotherapy can be administered in a centralized infusion center, for example, by nurses given approval to prescribe supportive drugs.39 And although there may be a preference for certain chemotherapy drugs (such as taxanes and anthracyclines), from a utilization management perspective it may not be cost-effective to provide them. A decision may be made to employ more affordable chemotherapy regimens that are still valid from a treatment perspective, such as cytocan, methotrexate, and fluorouracil (CMF). Hormonal therapy, specifically tamoxifen, is considered the single most effective anticancer therapy available in the world for breast cancer. A challenge, however, is being able to perform the needed hormone receptor tests on the breast cancer specimen to determine this prognostic factor so that only those patients who would benefit from it (those with hormone receptor–positive tumors) would be receiving it. These are examples of tailored treatment made possible by research. Aromatase inhibitors are likely too expensive for use in these settings. In some situations, surgical or radiation oophorectomy may be an affordable option in poorer countries. Radiation, which can require many weeks of treatment, must also be assessed in regard to its availability and need. Research should be conducted to determine if shorter courses of radiation therapy may suffice, making this treatment available for more patients. Last but not least is the need for palliative care, including medications and palliative radiation therapy, with priority given to those with locally advanced and metastatic disease.35
Identify individuals within the community who are trusted—people of faith, local doctors or nurses, or other community leaders. Recruit their help in identifying potential breast cancer survivors doing relatively well posttreatment (if they exist) as well as families who have lost family members to breast cancer.
- Provide certification classes for laypeople to become certified breast health educators, modifying the American Cancer Society training content to fit the needs of the community being served (ie, statistics, screening methods, diagnostic methods available, how to access care, what treatments are available). These individuals become the core of lay navigators for community outreach and awareness.
- Develop a core group of breast cancer survivors to speak, spreading the word about the importance of early detection as well as raising awareness of resources available for diagnosis and treatment; family members who have lost a loved one should speak to promote the importance of earlier detection and treatment. These individuals are 1 component of community outreach being conducted by lay navigators.
Identify what resources remain needed (transportation is the number 1 barrier to cancer care globally). Identify ways to create these needed resources or alternatives to eliminate these barriers. For example, if a patient can’t come for dressing changes, teach the family how to do this at home. Identify what treatments can be “taken to” the patient. Mammography mobile for screening works well in some rural areas. An alternative for formal exercise is hanging laundry on a clothesline.
What funding sources are accessible to obtain needed supplies for diagnosis and treatments? Where are they located and how much in dollars and equipment is available?
Identify a champion within the country for support of reducing mortality and morbidity from breast cancer. This may require meeting with a health minister to present needs. In reviewing the problems of breast cancer in middle- and low-income countries, it appears that oncologists can play a vital role through international associations by pressuring governments to supply resources and equipment and by insisting on training programs for medical personnel. Oncologists can also be fundamental to the creation of research initiatives to further learn about breast cancer physiologically and from a needs assessment perspective.4,5,40
Think creatively when considering obtaining supplies for specific needs. Work with advocacy organizations, and “alternative” companies (ie, a disposal diaper company might provide diapers to use for dressings for women with locally advanced fungating tumors).
Create educational materials that are clear, culturally appropriate, and at the correct educational level for those who will be reading or hearing (via video or audio) the information. This includes providing information that explains the role of navigators in supporting women with breast abnormalities during diagnosis and treatment.
Develop measures that will help to determine if you are making a difference as intended. These measures should reflect back to your goals for the breast health/breast cancer program. We cannot manage what we do not measure. So measurement is key. Clinical outcome measures and process as well as structure measures are helpful to consider here. Are you seeing more women diagnosed at an earlier stage of breast cancer? Are you recruiting more women to come for screening mammograms? How many women were taught how to perform a breast self-exam compared with the past? How many women received completion of treatment? What barriers were identified and what resources were provided for each specific case? Do you have written goals and objectives that have measurable outcomes? Are there clear job descriptions and measurable outcomes for each person involved in the navigation process?
Identify cancer organizations you can learn from and partner with so that you are not reinventing the wheel. These include the Academy of Oncology Nurse Navigators (AONN), The Breast Health Global Initiative (BHGI), and Union for International Cancer Control (UICC), as well as Susan G. Komen for the Cure International. Collaboration can facilitate accomplishments happening sooner when there are shared goals. Training and education of those who will be involved with the navigation program can be readily learned from affiliating with the AONN.
What Additional Challenges Do We Face in the Future?
As more targeted drugs are developed for the treatment of breast cancer, more expense will be incurred because these new drugs, though exciting and promising in saving and extending more lives, are going to be much more costly than treatments used to date. There will also likely be more oral medication usage, which can simplify the administration process by eliminating intravenous treatments. However adherence to oral medications will likely be a major barrier to treatment.
We are experiencing a shortage of oncology specialists and primary care physicians in the United States. Such shortages also occur in other parts of the world. And until there is a cure or true prevention, we need to anticipate the incidence of the disease continuing to increase globally.
Conclusion
It can appear to be a mammoth task to take on the early diagnosis and treatment of breast cancer in countries with limited resources and low- to middle-income status. However, by applying what we have learned through navigation efforts established in the United States over the past 4 decades, we likely will be able to make successful headway globally in improving the experience for women diagnosed with breast cancer. Creating a needs assessment and gap analysis; identifying the barriers specific to the women at risk for breast cancer; developing and implementing a comprehensive step-by-step action plan that is measurable and supported by evidence-based research; and forming a navigation team, led by a breast cancer nurse navigator and supported by a champion for breast cancer (such as an oncologist) can provide the tools and help to develop the resources needed in each country to make a difference for women diagnosed in the future. Navigation is truly a multifaceted process that includes patient education, community outreach, early diagnosis, utilization management, case management, appropriate treatment, survivorship, psychosocial care, and end-of-life needs. Bringing together the right people at the right time and in the right manner, all focused on the same goal, will enable more developing countries to achieve successes like those that have been achieved in the United States over the past several decades. And even in the United States, our work is far from done. It is likely that by working collegially with other organizations, we can learn from the work of developing countries as well.
Disclosure: Lillie D. Shockney, RN, BS, MAS, is AONN Program Director.
Corresponding author: Lillie D. Shockney, RN, BS, MAS Johns Hopkins University 600 North Wolfe Street, Carnegie 683 Baltimore, MD 21287 E-mail This email address is being protected from spambots. You need JavaScript enabled to view it.
References
- Gilani GM, Kamal S, Akhter AS. A differential study of breast cancer patients in Punjab, Pakistan. J Pak Med Assoc. 2003;53(10):478-481.
- Our global reach. Susan G. Komen for the Cure Web site. http://ww5.komen.org/AboutUs/GlobalReach.html. Accessed February 6, 2013.
- Malik AM, Pathan R, Shaikh NA, et al. Pattern of presentation and management of ca breast in developing countries. There is a lot to do. J Pak Med Assoc. 2010;60(9):718-721.
- Murray EM. Medical and radiation oncology for breast cancer in developing countries with particular reference to locally advanced breast cancer. World J Surg. 2003;27(8):924-927.
- Jones SB. Cancer in the developing world: a call to action. BMJ. 1999;319(7208):505-508.
- Jakesz R. Breast cancer in developing countries: challenges for multidisciplinary care [editorial]. Breast Care (Basel). 2008;3(1):4-5.
- Dohan D, Schrag D. Using navigators to improve care of underserved patients. Cancer. 2005;104(4):848-855.
- Lannin DR, Mathews HF, Mitchell J, et al. Influence of socioeconomic and cultural factors on racial differences in late-stage presentation of breast cancer. JAMA. 1998;279(22):1801-1807.
- Smedley BD, Stith AY, Nelson AR, eds. Unequal Treatment: Confronting Racial and Ethnic Disparities in Health Care. Washington, DC: National Academy Press; 2003.
- Shockney L. Becoming a Breast Cancer Nurse Navigator. Sudbury, MA: Jones & Bartlett; 2011.
- Sloan FA, Morrisey A, Valvona J. Effects of the Medicare prospective payment system on hospital cost containment: an early appraisal. Milbank Q. 1988;66(2):191-220.
- Feldstein PJ, Wickizer TM, Wheeler JR. Private cost containment. The effects of utilization review programs on health care use and expenditures. N Engl J Med. 1988;318:1310-1314.
- Shockney L. Evolution of patient navigation. Clin J Oncol Nurs. 2010;14(4):405-407.
- Wang TJ, Mort EA, Nordberg P, et al. A utilization management intervention to reduce unnecessary testing in the coronary care unit. Arch Intern Med. 2002;162(16):1885-1890.
- Restuccia JD. The evolution of hospital utilization review methods in the United States. Int J Qual Health Care. 1995;7(3):253-260.
- Goodwin JS, Satish S, Anderson ET, et al. Effect of nurse case management on the treatment of older women with breast cancer. J Am Geriatr Soc. 2003;51(9):1252-1259.
- Freeman HP, Chu KC. Determinants of cancer disparities: barriers to cancer screening, diagnosis, and treatment. Surg Oncol Clin N Am. 2005;14(4):655-669.
- About us. Harold P. Freeman Patient Navigation Institute Web site. http://www.hpfreemanpni.org/about-us/. Accessed February 26, 2013.
- Freeman HP, Muth BJ, Kerner JF. Expanding access to cancer screening and clinical follow-up among the medically underserved. Cancer Pract. 1995;3(1):19-30.
- Trans-HHS Cancer Health Disparities Progress Review Group. Making cancer health disparities history. US Department of Health and Human Services; 2004. http://planning.cancer.gov/library/2004chdprg.pdf. Accessed February 26, 2013.
- Centers for Medicare and Medicaid Services. Evidence Report and Evidence-Based Recommendations. Cancer Prevention and Treatment Demonstrations for Ethnic and Racial Minorities. US Department of Health and Human Services; 2003. http://www.cms.gov/Medicare/Demonstration-Projects/DemoProjectsEvalRpts/downloads/CPTD_Brandeis_Report.pdf. Accessed February 26, 2013.
- Frelix GD, Rosenblatt R, Solomon M, et al. Breast cancer screening in underserved women in the Bronx. J Natl Med Assoc. 1999;91(4):195-200.
- C-Change Web site. http://www.cancerpatientnavigation.org/index. html. Accessed January 28, 2013.
- The Avon breast cancer crusade. Avon Foundation for Women Web site. http://www.avonfoundation.org/causes/our-impact/breast-cancer-2012/. Accessed February 12, 2013.
- Patient navigator program. National Breast Cancer Foundation Web site. http://www.nationalbreastcancer.org/breast-cancer-patient-navigator. Accessed February 12, 2013.
- Shockney L. The role of patient navigation in improving breast cancer diagnosis and treatment. http://portal.bhgi.org/GlobalPortfolio/globalsum mit/Documents/Presentations/SHOCKNEY.pdf. Accessed March 8, 2013.
- Hunter CP, Redmond CK, Chen VW, et al. Breast cancer: factors associated with stage at diagnosis in black and white women. Black/White Cancer Survival Study Group. J Natl Cancer Inst. 1993;85(14):1129-1137.
- Kerner JF. Breast cancer prevention and control among the medically underserved. Breast Cancer Res Treat. 1996;40(1):1-9.
- Shockney L. Navigating the underserved and minority breast cancer patients—the challenges and solutions. Journal of Oncology Navigation and Survivorship. http://www.aonnonline.org/education/clinical-commentary/ 655-navigating-the-undeserved-and-minority-breast-cancer-patients-challenges- and-solutions#.UUxfZ-hqZV [subscription required]. Accessed March 22, 2013.
- Hurd TC, James T, Foster JM. Factors that affect breast cancer treatment: underserved and minority populations. Surg Oncol N Am. 2005;14(1):199-130.
- Hiatt RA, Pasick RJ. Unsolved problems in early breast cancer detection: focus on the underserved. Breast Cancer Res Treat. 1996;40(1):37-51.
- Hatzell TA, Ricketts TC, Tropman SE, et al. Rural physicians’ understanding of the state-of-the-art in breast, colon and rectum cancer treatment. Cancer Causes Control. 1999;10(4):261-267.
- Ayanian JZ, Guadagnoli E. Variations in breast cancer treatment by patient and provider characteristic. Breast Cancer Res Treat. 1996;40(1):65-74.
- Breen N, Kessler LG, Brown ML. Breast cancer control among the underserved–an overview. Breast Cancer Res Treat. 1996;40(1):105-115.
- Wright SV. An investigation into the causes of absconding among black African breast cancer patients. S Afr Med J. 1997;87:1540-1543.
- Adesunkanmi ARK, Lawal OO, Adelusola KA, et al. The severity, outcome and challenges of breast cancer in Nigeria. Breast. 2006;15(3):399-409.
- Ajekigbe AT. Fear of mastectomy: the most common factor responsible for late presentation of carcinoma of the breast in Nigeria. Clin Oncol (R Coll Radiol). 1991;3(2):78-80.
- Shim EJ, Lee KS, Park JH, et al. Comprehensive needs assessment tool in cancer (CNAT): the development and validation. Support Care Cancer. 2011;19(12):1957-1968.
- Sikora K. Developing a global strategy for cancer. Eur J Cancer. 1999;35(1):24-31.
- Cavalli F. The Djerba statement: just another declaration, or a new beginning [editorial]? Ann Oncol. 1995;6(10):963-964.





