Introduction
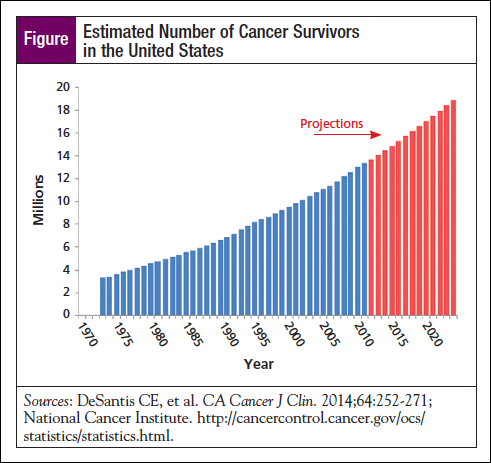
As of January 2014, nearly 14.5 million Americans were living with a history of cancer.1 Within 10 years, that number is expected to climb to nearly 19 million (Figure).2,3 Although these statistics may seem alarming, they actually represent longer survival of patients with cancer, which is the result of early diagnosis and advances in treatment over the past 4 decades. Data from the American Cancer Society reveal that the 5-year relative cancer survival rates have increased from 49% (1975-1977) to 68% (2004-2010), marking a significant improvement (P <.05). 1 With the advent of novel cancer drugs and diagnostic technology, these survival rates are projected to continue to increase.4
Defining Survivors
The term “cancer survivor” has a variety of definitions, but was originally used to describe family members who survived the loss of a loved one due to cancer at a time when the disease was considered incurable.5 This definition next evolved to describe individuals with cancer whose disease did not recur in the 5 years after their diagnosis or treatment.5 In 1986, the National Coalition for Cancer Survivorship aimed to redefine cancer survivorship, to capture the broad experience patients faced following a diagnosis of cancer that continued throughout their disease trajectory and for the balance of life.6,7 Although this definition of survivorship has been widely adopted as the norm throughout the oncology community, it has since been expanded to encompass family, friends, and caregivers as well.6-8
Survivorship Care
Although rising survival rates are a testament to the significant strides researchers and healthcare professionals have made on the frontlines of treatment, patients living with cancer often lack the necessary tools and resources to effectively navigate the healthcare system, particularly after they have completed their therapy.9 Once treatment ends, many cancer survivors continue to experience physical, emotional, and practical concerns, but may not receive the assistance they require.9 Posttreatment survivorship care is an evolving area of clinical practice and research that aims to address these needs.9 Given the increase in cancer survival rates, healthcare professionals today must recognize the ongoing needs of these patients and offer management strategies via survivorship care, which is key to minimizing disease- and treatment-related effects on a patient’s quality of life (QoL).9
One of the greatest challenges facing the cancer survivorship community is how best to design and deliver high-quality survivorship care.9 Because healthcare providers may sometimes differ in their approach to this care, building consensus is important to effectively respond to the myriad of challenges cancer survivors face during the posttreatment period.9
In 2011, LIVESTRONG assembled the Essential Elements of Survivorship Care meeting in Washington, DC, which included more than 150 community leaders, stakeholders, cancer survivors, and cancer survivor advocates. At the forefront of this effort was a series of consensus-building activities designed to establish a list of elements that are essential to the care of cancer survivors following treatment.9
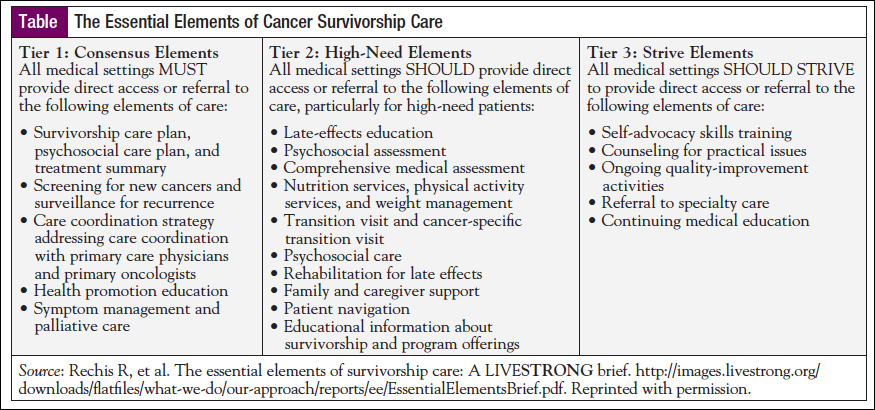
Meeting participants prioritized 20 essential elements of survivorship care, which were grouped into 3 tiers based on their ranking scores.9 As shown in the Table, Tier 1 includes elements of care that all medical settings must provide; Tier 2 includes elements that all medical settings should provide; and Tier 3 includes elements that all medical settings should strive to provide.9
Following the LIVESTRONG meeting, researchers at The George Washington University further examined patient-prioritized needs in survivorship care through a national comparative effectiveness study funded by the Patient-Centered Outcomes Research Institute. Results will be forthcoming in 2017.10
Survivorship Care Plans
According to the Institute of Medicine (IOM) and the National Comprehensive Cancer Network, the central components of survivorship care include: (1) prevention of new and recurrent cancers and other late effects; (2) surveillance for cancer spread, recurrence, or second cancers; (3) assessment of late psychosocial and physical effects; (4) intervention for consequences of cancer and treatment; and (5) coordination of care between primary care providers and specialists to ensure that all of the survivor’s health needs are met.8,11
In 2005, the IOM released From Cancer Patient to Cancer Survivor: Lost in Transition, an instrumental report that underscored the importance of using survivorship care plans to help preserve the continuity of care between primary care providers and oncologists.8,11 Critical to the success of any plan is the transfer of patient information between these clinicians, since they constitute a team working on behalf of the patient.8
In addition to improving the continuity of care for patients, survivorship care plans may help clinicians identify psychosocial distress, detect cancer recurrence and secondary cancers in a timely manner, manage bothersome symptoms, avoid preventable conditions, and avert potentially fatal late effects.11 Accordingly, the following components should be included in the comprehensive summary of a survivorship care plan11:
- Results of any diagnostic tests performed
- Characteristics of tumors (ie, site[s], stage/grade, hormone receptor status, relevant marker information)
- Complete dates of treatment initiation and completion
- Comprehensive list of treatment—including surgery, chemotherapy, radiotherapy, transplant, hormonal therapy, or other therapies provided. Additional information should include agents used, treatment regimens, total dosage, identifying number and title of clinical trials (if applicable), indicators of treatment response, and toxicities experienced during treatment
- Psychosocial, nutritional, and supportive services that have been provided
- Complete contact information of clinicians and institutions providing treatment
- Identification of a key point of contact and coordinator of continuing care.
Furthermore, once a patient with cancer is discharged from treatment, a documented follow-up care plan that incorporates evidence-based standards of care should be made available to every patient and his or her primary healthcare provider. At a minimum, this should include a likely course of recovery from any treatment-related toxicity, the need for continued health maintenance or adjuvant therapy as indicated, and any recommendations for cancer screenings or other periodic examinations, with instructions given on when they should be performed and who should conduct them.11
In its report titled Cancer Program Standards 2012: Ensuring Patient-Centered Care, the Commission on Cancer (CoC) stipulated that, to receive and maintain cancer program accreditation, all cancer programs should establish survivorship care plans for their patients by 2015.12 To fulfill this requirement, the plan should be prepared by the principal provider(s) responsible for coordinating the patient’s oncology treatment, with input from other care providers. It is to be distributed to the patient once treatment is completed and must include a record of care that the patient received, important details on disease characteristics, and a follow-up care plan that incorporates recognized evidence-based standards of care, when available. The program must be implemented, monitored, and evaluated, with documented results presented annually to the cancer committee.12
Addressing Psychosocial Distress in Patients with Cancer
Patients with cancer may experience a myriad of psychosocial concerns throughout the course of their disease, including psychological, social, financial, and behavioral challenges, all of which can have a profound effect on their health and treatment plan.12 In an effort to address these issues, the CoC requires that cancer programs develop a process to incorporate screening for distress into the standard of care for patients with cancer and provide resources and/or referrals designed to meet any attendant psychosocial needs that patients with distress may experience.12
According to the CoC, screening for distress should be offered at least once per patient during a pivotal medical visit, such as at time of diagnosis, presurgical and postsurgical visits, first visit to discuss chemotherapy, routine visit with a radiation oncologist, or a postchemotherapy follow-up visit.12 No particular mode of administration is specified by the CoC (eg, patient questionnaire, clinician-administered questionnaire); the selection may be made at the discretion of the cancer program. The program may also choose its own tool for screening patients for distress. However, the CoC gives preference to validated instruments with established clinical cutoffs.12
Survivorship Care Programs
Survivorship care has been implemented in different ways by different programs; however, most programs are run by either physicians or advanced practice clinicians such as nurse practitioners.8 Each program approach has its own advantages and disadvantages.8 For example, some survivorship care programs focus on treating the impact of cancer and emphasize care for long-term and late effects of treatment, whereas other programs emphasize wellness and the importance of psychological support.13
Two main considerations when developing a survivorship care program are the patient population and the level and type of resources available in the practice setting.13 The experiences and needs of patients with cancer may vary throughout their disease trajectory, ranging from few long-term effects related to treatment to chronic conditions or significant treatment-related health issues.13
Using Communication to Foster Patient-Centered Survivorship Care
Effective communication between the patient with cancer and the healthcare provider (or team) is a cornerstone of patient-centered care. In addition to educating patients on aspects of their disease, it may help providers identify patients with needs that are likely to affect their health or their care. One such example is monitoring the effectiveness of treatment through feedback and then determining whether adjustments are needed. Good communication serves patients by providing referrals to appropriate psychosocial services, coordinating psychosocial and biomedical healthcare, and enhancing follow-up on care delivery. It also provides emotional support to patients to assist them in managing their disease and making shared decisions regarding treatment.14,15 According to the National Cancer Institute, key aspects of effective patient–clinician communication include: (1) fostering healing relationships, (2) exchanging information, (3) responding to emotions, (4) managing uncertainty, (5) making decisions, and (6) enabling patient self-management.16
Because family members are often the primary caregivers for patients with cancer, effective communication between caregivers and clinicians is equally important, especially if the caregiver is responsible for an individual with limited communication skills, including language barriers or cognitive deficits.16
Evidence indicates that effective clinician–patient communication is associated with favorable patient outcomes.15 Studies have shown that patients whose physicians involved them in their treatment decisions during office visits had better health outcomes or improved overall satisfaction compared with those who were uninvolved in their own care.15,17,18 To set the stage for effective communication, clinicians should prepare themselves for an optimal exchange by devoting their full attention to patients and not interrupting them while they are speaking. The clinician can create an environment that enhances a true connection by making eye contact, sitting near a patient, or reassuring a patient through appropriate touch. During the exchange, it is important to provide information and confirm understanding. Finally, clinicians should ask patients for feedback on their communication styles.19 Establishing a clear connection with patients from the beginning allows patients to open up, be less frightened, and focus on the information being provided to them.19
Addressing Quality-of-Life Issues
Maintaining a cancer survivor’s QoL is an important component of survivorship care, especially for patients who experience long-term and late effects of cancer and its treatment.20 As it pertains to cancer care, QoL is defined as a personal sense of well-being, encompassing physical, psychological, social, and spiritual domains.20
Physical well-being involves the control or relief of symptoms—either acute symptoms related to treatment, such as hair loss, nausea, and vomiting, or late effects such as pain and fatigue—and the maintenance of function and independence. Psychological well-being refers to the ability to cope with a life-threatening illness that may evoke emotional distress, altered life priorities, and fear of the unknown, and may be accompanied by a corresponding desire to make positive life changes. Social well-being involves the effort to deal with the impact of cancer on individuals, their roles, and relationships. Spiritual well-being refers to the ability to maintain hope and derive meaning from the cancer experience, which is often characterized by uncertainty.20
Long-Term and Late Effects of Cancer Treatment
Although many patients with cancer function normally after completing treatment and go on to live symptom-free lives, others may experience persistent lingering effects or effects that appear long after treatment has ended.21 Long-term effects may emerge during or after treatment and persist chronically, whereas late effects may not emerge until months or years later.21
The types of long-term and late effects that patients with cancer experience will vary, depending on the type of treatment they received.22 For example, lymphedema may be experienced by patients who have undergone surgery to remove their lymph nodes or who have had radiation therapy to lymph nodes, whereas patients with Hodgkin lymphoma who have had their spleen removed are at increased risk for contracting serious infections compared with their counterparts who did not undergo this surgery.22
In other instances, patients who have received chemotherapy and radiation therapy to the chest may experience heart and lung problems, whereas chemotherapy and high doses of radiation to the head may lead to learning impairments, memory problems, or attention deficits.22 In addition, chemotherapy and high-dose radiation therapy in the head and neck region may lead to problems related to dental and oral health, whereas the use of steroid medications may lead to vision problems such as cataracts.22 Other common long-term and/or late effects of cancer treatment include fatigue, sexual dysfunction, infertility, and pain.23-25
Conclusion
Nurse navigators play a critical role in the delivery of quality survivorship care in the posttreatment setting. They must have a strong understanding of the specific risks related to various treatment modalities and must be able to triage survivors to specialty care based on those risks. Nurse navigators also connect patients to critical resources and facilitate patient-centered communication and care coordination among providers. Given the growing survivor population and the shrinking oncology workforce, these professionals will be critical to the provision of cancer survivorship care for the foreseeable future.
References
- American Cancer Society. Cancer Facts & Figures 2015. www.cancer.org/acs/groups/content/@editorial/documents/document/acspc-044552.pdf. Accessed July 15, 2015.
- DeSantis CE, Lin CC, Mariotto AB, et al. Cancer treatment and survivorship statistics, 2014. CA Cancer J Clin. 2014;64:252-271.
- National Cancer Institute. Statistics. http://cancercontrol.cancer.gov/ocs/statistics/statistics.html. Accessed July 15, 2015.
- Mariotto AB, Yabroff KR, Shao Y, et al. Projections of the cost of cancer care in the United States: 2010-2020. J Natl Cancer Inst. 2011;103:117-128.
- Leigh SA. Defining our destiny. In: Hoffman B, ed. A Cancer Survivor’s Almanac: Charting the Journey. Minneapolis, MN: Chronimed Publishing; 1996:261-271.
- National Coalition for Cancer Survivorship. Defining cancer survivorship. www.canceradvocacy.org/news/defining-cancer-survivorship/. Published July 24, 2014. Accessed July 15, 2015.
- National Coalition for Cancer Survivorship. The National Coalition for Cancer Survivorship. www.canceradvocacy.org/about-us/our-history/. Accessed July 15, 2015.
- National Comprehensive Cancer Network. NCCN Clinical Practice Guidelines in Oncology (NCCN Guidelines®): Survivorship. Version 1.2015. February 27, 2015. www.nccn.org/professionals/physician_gls/pdf/survivorship.pdf. Accessed July 15, 2015.
- Rechis R, Beckjord EB, Arvey SR, et al. The essential elements of survivorship care: A LIVESTRONG brief. http://images.livestrong.org/downloads/flatfiles/what-we-do/our-approach/reports/ee/EssentialElementsBrief.pdf. Accessed July 15, 2015.
- The Patient-Centered Outcomes Research Institute. Evaluating Cancer Survivorship Models. www.pcori.org/research-results/2013/evaluating-cancer-survivorship-care-models. Accessed October 30, 2015.
- Institute of Medicine. Hewitt M, Greenfield S, Stovall E, eds. From Cancer Patient to Cancer Survivor: Lost in Transition. Washington, DC: The National Academies Press; 2005.
- American College of Surgeons Commission on Cancer. Cancer Program Standards 2012: Ensuring Patient-Centered Care. V1.2.1. www.facs.org/~/media/files/quality%20programs/cancer/coc/programstandards2012updates.ash. Accessed July 15, 2015.
- American Society of Clinical Oncology. Providing High Quality Survivorship Care in Practice: An ASCO Guide. www.asco.org/sites/www.asco.org/files/survivorcompendium2014_web.pdf. Accessed July 15, 2015.
- Institute of Medicine. Delivering High-Quality Cancer Care: Charting a New Course for a System in Crisis. Washington, DC: The National Academies Press; 2013. www.nap.edu/catalog/18359/delivering-high-quality-cancer-care-charting-a-new-course-for. Accessed July 15, 2015.
- Institute of Medicine. Cancer Care for the Whole Patient: Meeting Psychosocial Health Needs. Washington, DC: The National Academies Press; 2008. www.nap.edu/catalog/11993/cancer-care-for-the-whole-patient-meeting-psychosocial-health-needs. Accessed July 15, 2015.
- Epstein RM, Street RL Jr. Patient-Centered Communication in Cancer Care: Promoting Healing and Reducing Suffering. National Cancer Institute, NIH Publication No.07-6225. Bethesda, MD; 2007.
- Gattellari M, Butow PN, Tattersall MH. Sharing decisions in cancer care. Soc Sci Med. 2001;52:1865-1878.
- Hack TF, Degner LF, Watson P, Sinha L. Do patients benefit from participating in medical decision making? Longitudinal follow-up of women with breast cancer. Psychooncology. 2006;15:9-19.
- Planetree, Inc. and Picker Institute. Patient-Centered Care: Improvement Guide. planetree.org/wp-content/uploads/2015/03/Patient-Centered-Care-Improvement-Guide-10.10.08.pdf. Accessed July 15, 2015.
- Ferrell BR, Hassey Dow K. Quality of life among long-term cancer survivors. Oncology (Williston Park). 1997;11:565-571.
- Stein KD, Syrjala KL, Andrykowski MA. Physical and psychological long-term and late effects of cancer. Cancer. 2008;112(11 suppl):2577-2592.
- Cancer.net. Long-term side effects of cancer treatment. www.cancer.net/survivorship/long-term-side-effects-cancer-treatment. Accessed July 15, 2015.
- American Cancer Society. Fatigue in people with cancer. www.cancer.org/acs/groups/cid/documents/webcontent/002842-pdf.pdf. Accessed July15, 2015.
- Schover LR, van der Kaaij M, van Dorst E, et al. Sexual dysfunction and infertility as late effects of cancer treatment. EJC Suppl. 2014;12:41-53.
- Moynihan T; for Mayo Clinic staff. Cancer pain: relief is possible. www.mayoclinic.org/diseases-conditions/cancer/in-depth/cancer-pain/art-20045118. Accessed July 15, 2015.