Objectives: The objectives were to evaluate the LIVESTRONG Cancer Navigation Services program, which was developed to address cancer survivors’ psychosocial needs from diagnosis through posttreatment survivorship, and to discuss its implications for the provision of care for survivors occurring outside the clinical setting.
Methods: We conducted a longitudinal study to track cancer survivors who received navigation services, surveying participants at intake and at 2 weeks and 6 weeks postintake. We examined changes in (1) the perceived impact of cancer-related concerns; (2) self-efficacy related to getting support and coping with emotional health; and (3) emotional distress, plus the impact of receiving counseling from an emotional support navigator.
Results: The most common need among the cancer survivors was for emotional support, followed by insurance, financial, and employment concerns. The numbers and types of needs differed by age at diagnosis, stage in treatment, and other individual characteristics. As a whole, the study participants’ self-efficacy increased over time, and the impact of cancer-related concerns and emotional distress decreased. Survivors referred to an emotional support navigator had increased self-efficacy and reduced emotional distress and concerns about the impact of cancer. Overall, the participants reported high levels of satisfaction with navigation services, which were higher among survivors with more needs, who finished treatment <5 years ago (vs ≥5 years ago), and who had more interactions with a navigator.
Conclusions: These findings highlight the importance of navigation services throughout the cancer journey and the value of the LIVESTRONG model, which augments community-based and clinic-based services. Because adequate psychosocial care is not available across many oncology care settings, services outside the clinical setting can help meet cancer survivors’ needs.
When patients are faced with a cancer diagnosis, they often experience emotional distress and feelings of uncertainty. They must deal with complex medical information, make difficult and often life-altering decisions, and navigate a fragmented healthcare system. Patient navigation programs can help patients, as well as family members and other loved ones, throughout the cancer journey by providing tangible assistance and emotional support. A growing body of research finds that patient navigation services improve screening rates, time from screening to diagnosis, timeliness of care, and patient satisfaction with the navigation services; reduce patient distress; and improve other outcomes.1
Patient navigation services typically are based in clinical or hospital settings, and patients with cancer are referred to the navigation program by physicians or by other clinic-based staff.2,3 Initially, patient navigation focused on getting patients into treatment in a timely manner and supporting them in active treatment.1,4 Patient navigation services have not traditionally focused on cancer survivors who have completed active treatment, although there is growing recognition of the importance of continuing navigation support for patients at this stage.5 In fact, it was very recently that the oncology accrediting program of the American College of Surgeons—the Commission on Cancer—established standards for patient navigation services and psychosocial screening and care, which are to be implemented in 2015.6 Furthermore, although cancer clinics are increasingly following the 2003 National Comprehensive Cancer Network Distress Management Guidelines, studies indicate that many patients do not receive the coping resources and psychosocial support services they need.7,8
Recognizing that cancer survivors’ myriad needs were not being comprehensively met within the clinical setting, the LIVESTRONG Foundation created a navigation service program in 2004 to fill this gap. These services act as a community-based complementary system for clinical models of navigation, and for communities without existing local navigation and psychosocial screening and support. LIVESTRONG Cancer Navigation Services program (henceforth, LIVESTRONG Navigation) provides services independent of any clinic or hospital, and the program is designed to address the needs of patients with cancer and survivors across their cancer journey from diagnosis through posttreatment survivorship. Other nonprofit organizations, including the Cancer Support Community, the National Coalition for Cancer Survivorship, and the American Cancer Society, also provide support services to individuals affected by cancer, using different models.9-11
The purpose of this article is to describe the LIVESTRONG Navigation program, to present findings from an evaluation of its unique model of services, and to discuss the findings’ implications for the provision of care for cancer survivors that can occur outside the clinical setting.
The goal of LIVESTRONG Navigation is to provide free, comprehensive, one-to-one support to all people affected by cancer, including those who currently have or who were ever diagnosed with cancer, caregivers, family, friends, and healthcare providers. This article focuses on navigation services for patients who have been diagnosed with cancer (ie, cancer survivors). The program provides services by phone, e-mail, or in-person (in the LIVESTRONG office in Austin, TX) in 6 main areas: (1) addressing insurance, financial, and employment concerns; (2) education and matching for clinical trials; (3) locating and accessing local resources; (4) educating on and providing financial discounts for fertility preservation services; (5) coping with emotional concerns through counseling and support groups; and (6) providing education about a cancer diagnosis and treatment decision-making.
Soon after starting LIVESTRONG Navigation, the LIVESTRONG Foundation recognized that cancer survivors had considerable emotional support needs. To address these needs, LIVESTRONG created the Emotional Support Navigation program. Specially trained emotional support navigators (ESNs) are licensed social workers who provide professional short-term counseling by telephone (and in person in the Austin office). ESNs help cancer survivors set goals, such as depression management, improving self-care, and improving communication with health professionals, family, and other loved ones. ESNs also help survivors to identify strategies to reach their goals (eg, for depression, strategies may include cognitive reframing, journaling, and mindfulness meditation).
LIVESTRONG Navigation is able to provide this robust range of services for people affected by cancer because of the national partnership model that acts as the program’s underpinning. LIVESTRONG Navigation acts as the convener of organizations that partner to create a coordinated service delivery system that is intended to reduce service redundancy and create a seamless experience for survivors. Partner organizations and the type of support provided at the time of the study include:
- Patient Advocate Foundation: insurance, debt management, and employment concerns
- EmergingMed: clinical trials education and matching
- NavigateCancer Foundation: understanding a diagnosis and making informed treatment decisions
- Imerman Angels: connecting with peers who have had a similar cancer experience.
The LIVESTRONG Foundation promotes navigation services via community outreach, community partnerships, and advertising through various media. Based on intake data of the navigation program with the LIVESTRONG Foundation, cancer survivors most frequently learn about LIVESTRONG from healthcare providers (34%), community partners (24%), word of mouth (15%), and the Internet (12%).
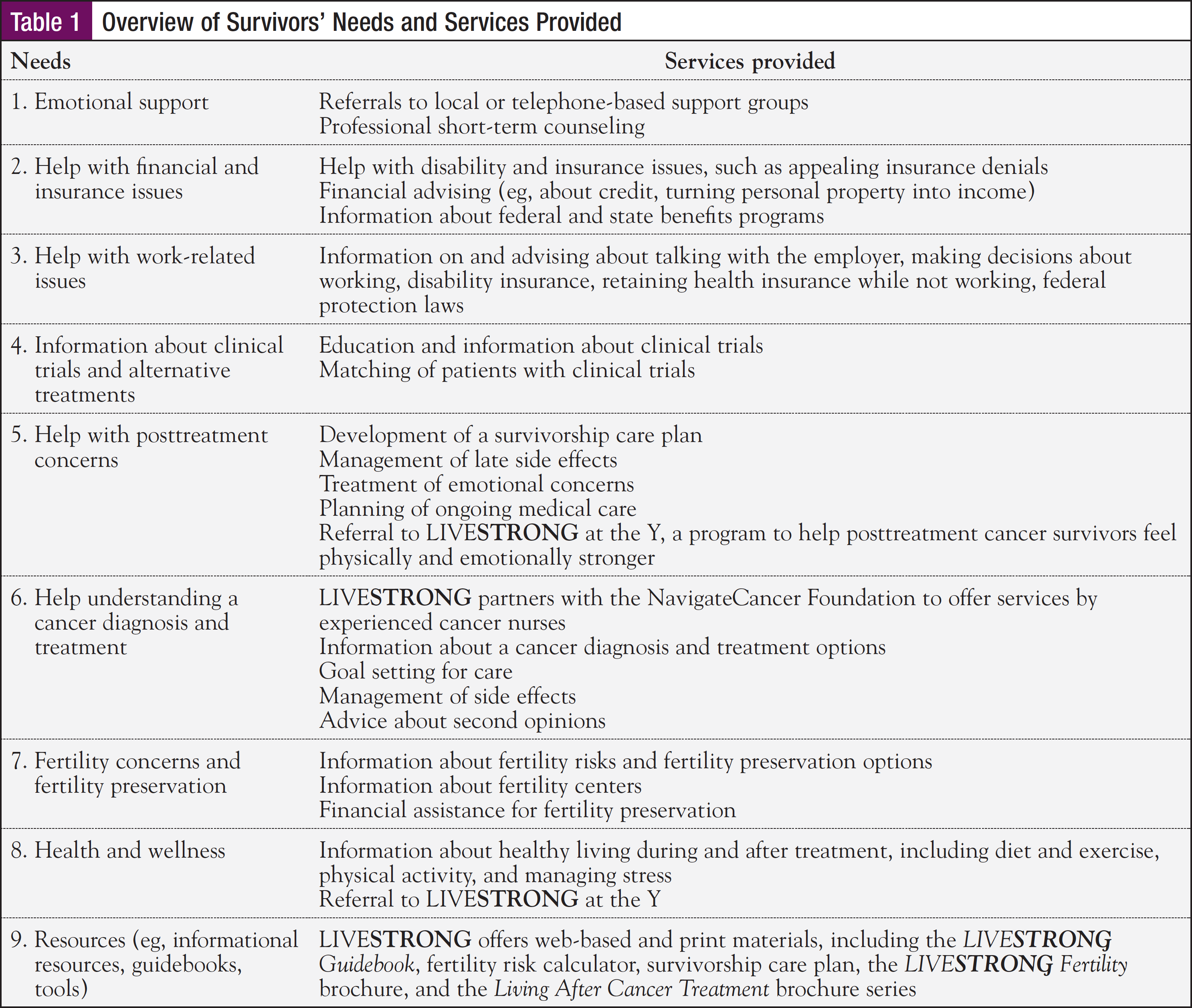
During the first communication between a LIVESTRONG navigator and a survivor, the navigator conducts a distress screening using a stress thermometer and assesses the survivor’s needs. The navigator then connects the survivor to the appropriate LIVESTRONG services and resources (including the LIVESTRONG at the Y program, the LIVESTRONG Care Plan, the LIVESTRONG Guidebook, or the Living After Cancer Treatment brochure series) and to partner organizations as appropriate. LIVESTRONG also provides emotional support services, fertility assistance, and referrals to community resources and psychosocial support programs. LIVESTRONG navigators coordinate each survivor’s care, provide appropriate follow-up, ensure that the survivor’s needs are met, and identify future needs that may arise (Table 1).
To determine the model’s impact, LIVESTRONG designed an evaluation study that focused on service delivery and survivor-reported outcomes.
Methods
Study Design
LIVESTRONG conducted a longitudinal study to track cancer survivors who received LIVESTRONG Navigation services. The study participants were surveyed at 3 time points—during intake (Survey 1 = T1); 2 weeks after intake (Survey 2 = T2); and 6 weeks after intake (Survey 3 = T3). The survivors completed the intake survey (Survey 1) using the mode by which they initially contacted LIVESTRONG (ie, in person, by telephone, or online); the remaining surveys (Surveys 2 and 3) were sent by mail or by e-mail.
Enrollment
Cancer survivors who contacted LIVESTRONG Navigation between March 2011 and October 2012 and met the age eligibility criteria (aged ≥18 years) were invited to participate in the study. Of 1162 cancer survivors who participated in the navigation study, 761 completed the baseline survey and at least 1 follow-up survey; another 401 cancer survivors did not complete a follow-up survey and were therefore excluded from the analysis.
Data Collection Instruments
The intake form, which was created as a basic needs assessment tool, includes questions to gather demographic, contact, and minimal medical information, such as diagnosis and stage of treatment. Also, questions are included to help assess the patient’s emotional, practical, and financial needs. The form is used to determine appropriate LIVESTRONG resources and referrals to partner organizations, as well as to provide some data for evaluation.
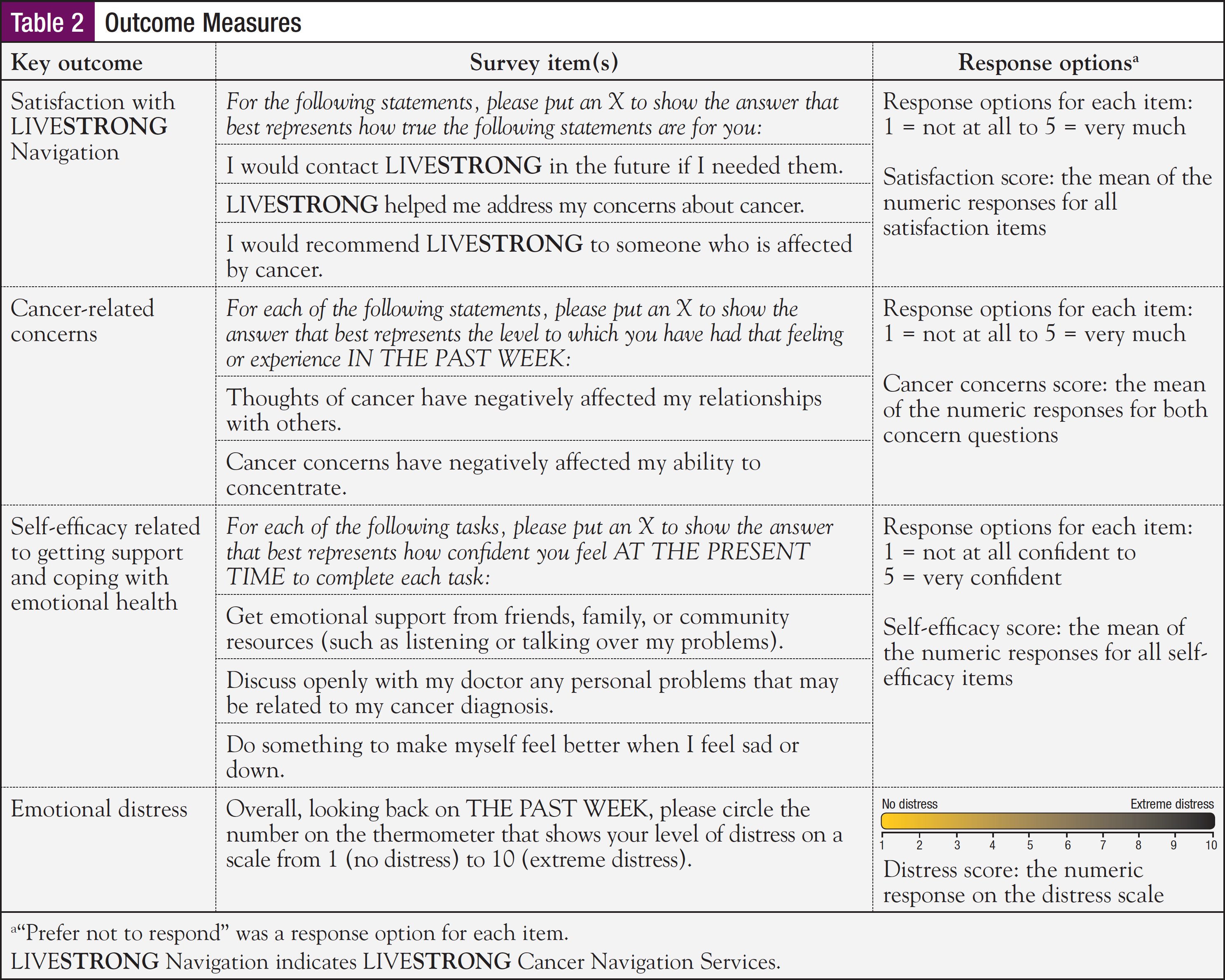
The intake form also assessed baseline levels for key outcomes, such as cancer-related concerns, emotional distress, and self-efficacy related to getting support for cancer-related needs. Surveys 2 and 3 also assessed these outcomes, as well as satisfaction with LIVESTRONG Navigation (Table 2). We included measures that are relevant to LIVESTRONG’s main areas of service; for example, the results from assessing cancer-related concerns before and after counseling inform these services.
Data Analysis
We examined the outcomes by first computing descriptive statistics (means and standard deviations) of the outcome measures at each time point for all participants and for subgroups. We then fit a series of models to examine the impact of LIVESTRONG Navigation on the participants’ outcomes. Two variables captured service delivery—(1) number of interactions with LIVESTRONG navigators, and (2) number of services provided.
We conducted a linear regression model examining the relationship between LIVESTRONG Navigation services and participant-reported satisfaction with the services at the end of the study. Satisfaction was based on the T3 survey measures, but T2 scores were used for participants with missing satisfaction scores at T3. The model controlled for the number of service needs, sex, race, age at diagnosis, the number of interactions with an ESN, marital status, and the stage of treatment.
Because of the large number of missing values for age at diagnosis, marital status, and stage of treatment, we included an unknown (ie, missing) category for each of these variables to allow for the inclusion of as many participants as possible in the analyses.
We then examined changes over time from intake to 6-week follow-up in (1) perceived impact of cancer-related concerns, (2) self-efficacy related to getting support and coping with emotional health, and (3) emotional distress. Multilevel models were conducted to account for measurements repeated over time.
In addition to examining the impact of services and interactions with navigators on outcomes, we also tested for an interaction between time and referral to the LIVESTRONG ESN to determine whether survivors who received ESN support experienced greater or lesser improvements in outcomes over time than those who did not receive this service. Similar control variables were included in these models. We ran all models with and without participants who had missing values for age at diagnosis, marital status, and stage of treatment and found no differences.
Results
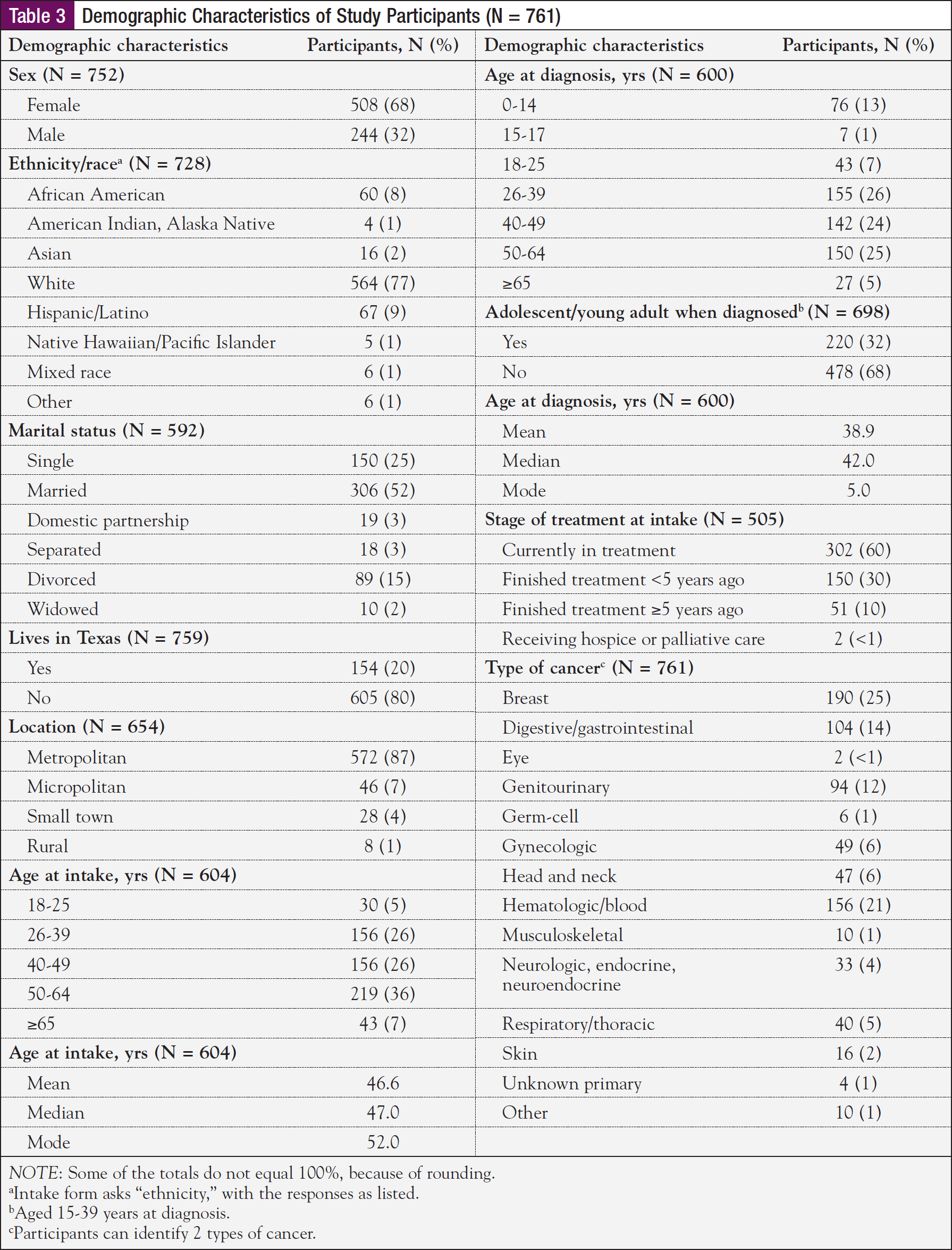
Table 3 presents the characteristics of the study sample (N = 761). The majority of study participants were female (68%), white (77%), married (52%), and currently in treatment (60%). We found no significant differences between the study participants and those who were excluded from the analyses (who did not complete a follow-up survey) in terms of age at diagnosis, stage of treatment, or cancer type.
Participant Needs
At intake, the navigators assess the participants’ needs and connect them with the appropriate services, resources, and partners. Table 4 shows the types and numbers of services that were needed and received by the participants (mean, 7.0 needs).
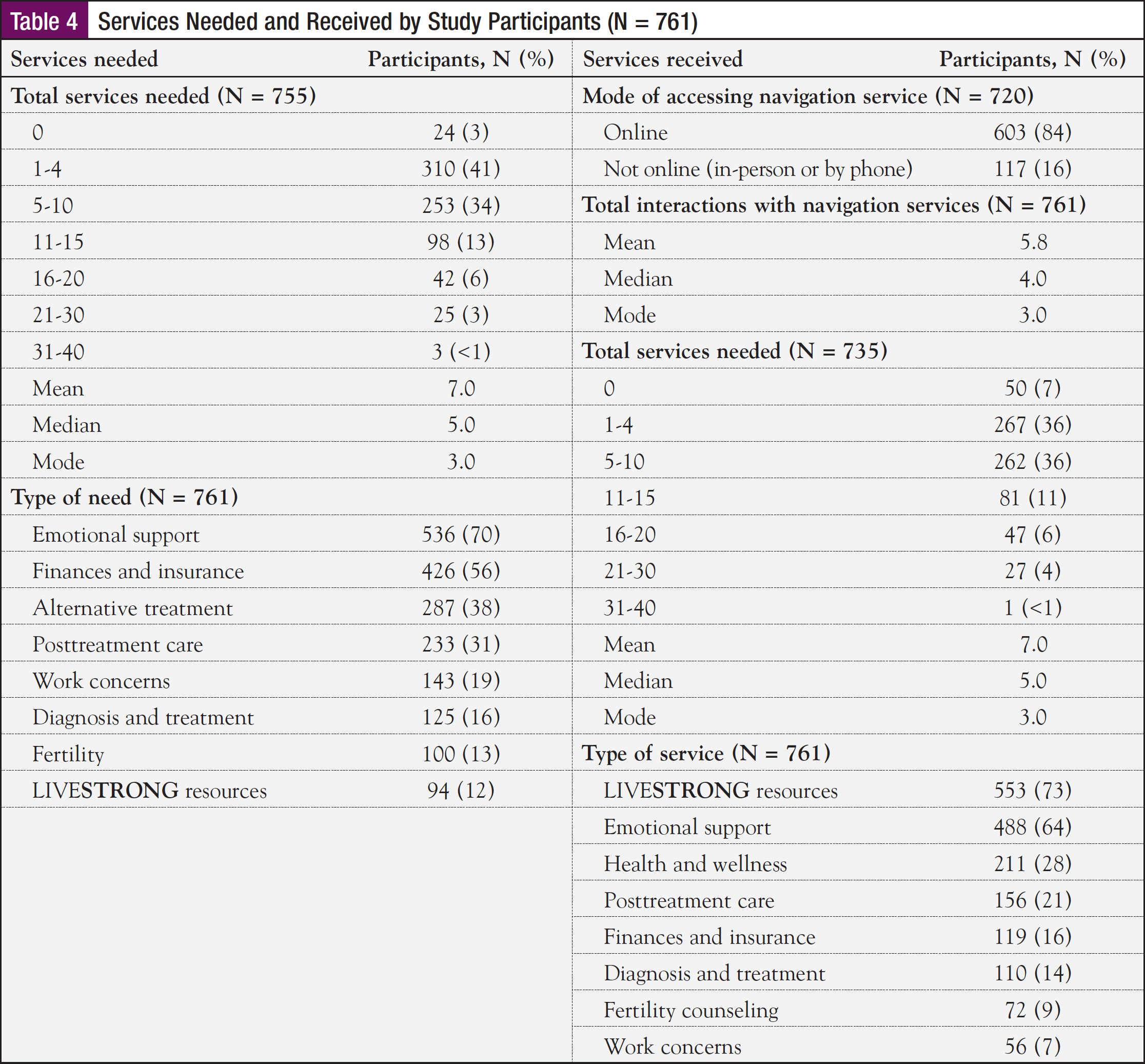
Overall, the most frequently reported needs were emotional support (70%), followed by financial and insurance needs (56%). Emotional support was the most frequently reported need for all age-groups, for men and women, and across all stages of survivorship. However, among nonwhite participants, financial and insurance needs were greater than emotional support needs, and there were marked differences between white and nonwhite participants (71% of white participants had emotional needs vs 59% of nonwhite participants, P <.05; and 55% of white participants had financial and insurance needs vs 70% of nonwhites, P <.05).
Participants with neurologic, endocrine, neuroendocrine, gynecologic, or digestive/gastrointestinal cancers had the most needs (mean, 8.0); those with genitourinary and other cancers (including skin, musculoskeletal, germ-cell, eye, and unknown) had the lowest number of needs (mean, 6.0 needs).
Participants who were diagnosed with cancer as adolescents and young adults (aged 15-39 years) had a significantly higher number of needs (mean, 8.6) than those who were aged 40 to 59 at diagnosis (mean, 6.8), aged ≥60 years at diagnosis (mean, 6.8), and aged ≤14 years at diagnosis (mean, 7.6; P <.009).
Participants who were currently in treatment were more likely to have financial and insurance needs (65%) compared with participants who had finished treatment (49% for those who had finished <5 years ago and 56% for those who had finished ≥5 years ago; P = .004).
Services Provided
Overall, the participants interacted with LIVESTRONG Navigation an average of 5.8 times and were provided, on average, 7 different services (Table 4). The most common types of services were LIVESTRONG resources (73%), ESN (64%), health and wellness (28%), and posttreatment care (21%).
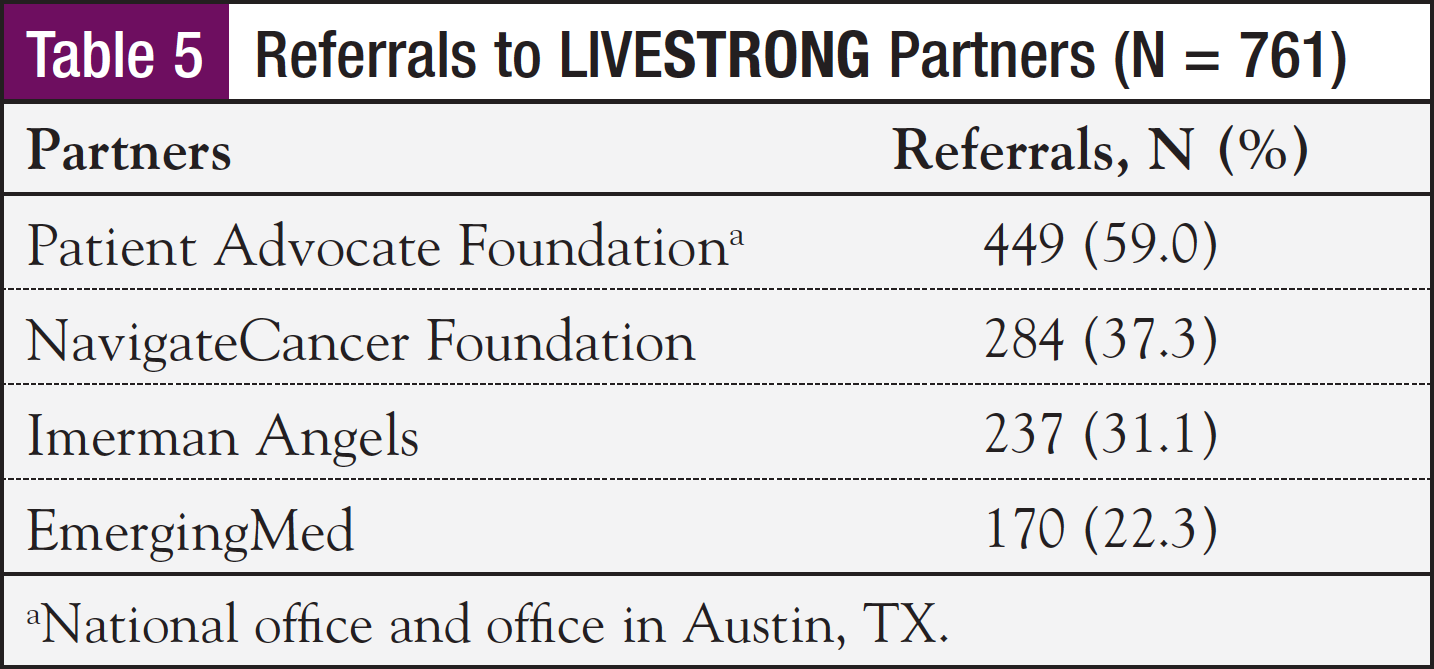
The participants were also referred to partner organizations for specialized services (Table 5).
Outcomes
Overall, the participants’ self-efficacy (related to getting support and coping with emotional health) increased over time, and the impact of cancer-related concerns and distress decreased over time (Figures 1, 2, and 3).
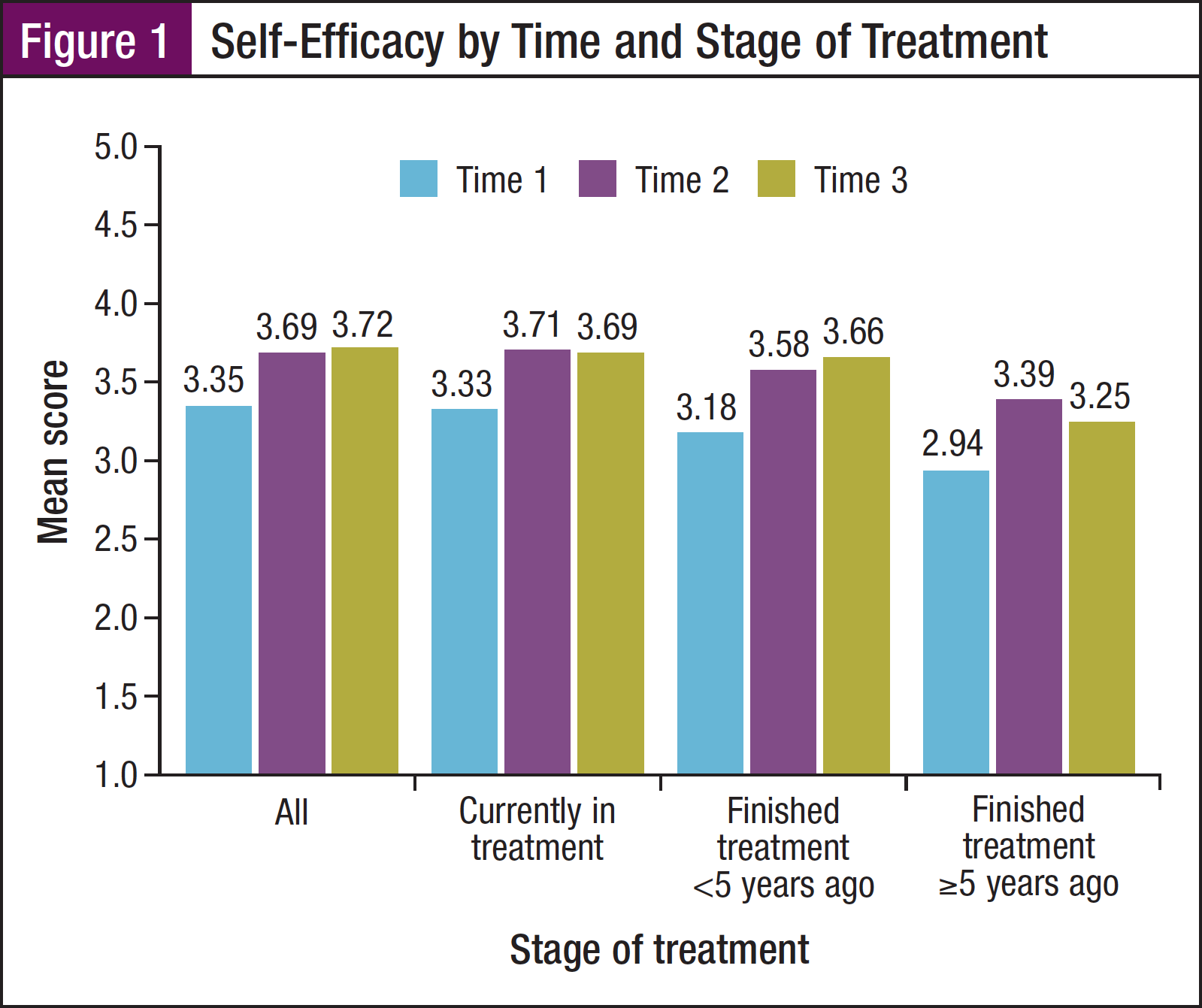
Self-efficacy. The mean self-efficacy scores increased over time, from 3.35 at T1 to 3.69 at T2 and 3.72 at T3 (increases were significant for T1 vs T2 and T1 vs T3; P <.05; Figure 1). At all 3 time points, self-efficacy was lowest among the survivors who finished treatment ≥5 years ago, although the differences were significant only at T1 and T3. At all 3 time points, self-efficacy also was lowest among survivors who were diagnosed at age 0 to 14 years; however, the differences were significant only at T2. Those diagnosed at age 0 to 14 years had lower self-efficacy (mean, 3.39) than survivors who were diagnosed at age 40 to 59 years (mean, 3.71) or at age ≥60 years (mean, 3.85; P <.05). There were no significant differences in self-efficacy by sex or by race/ethnicity.
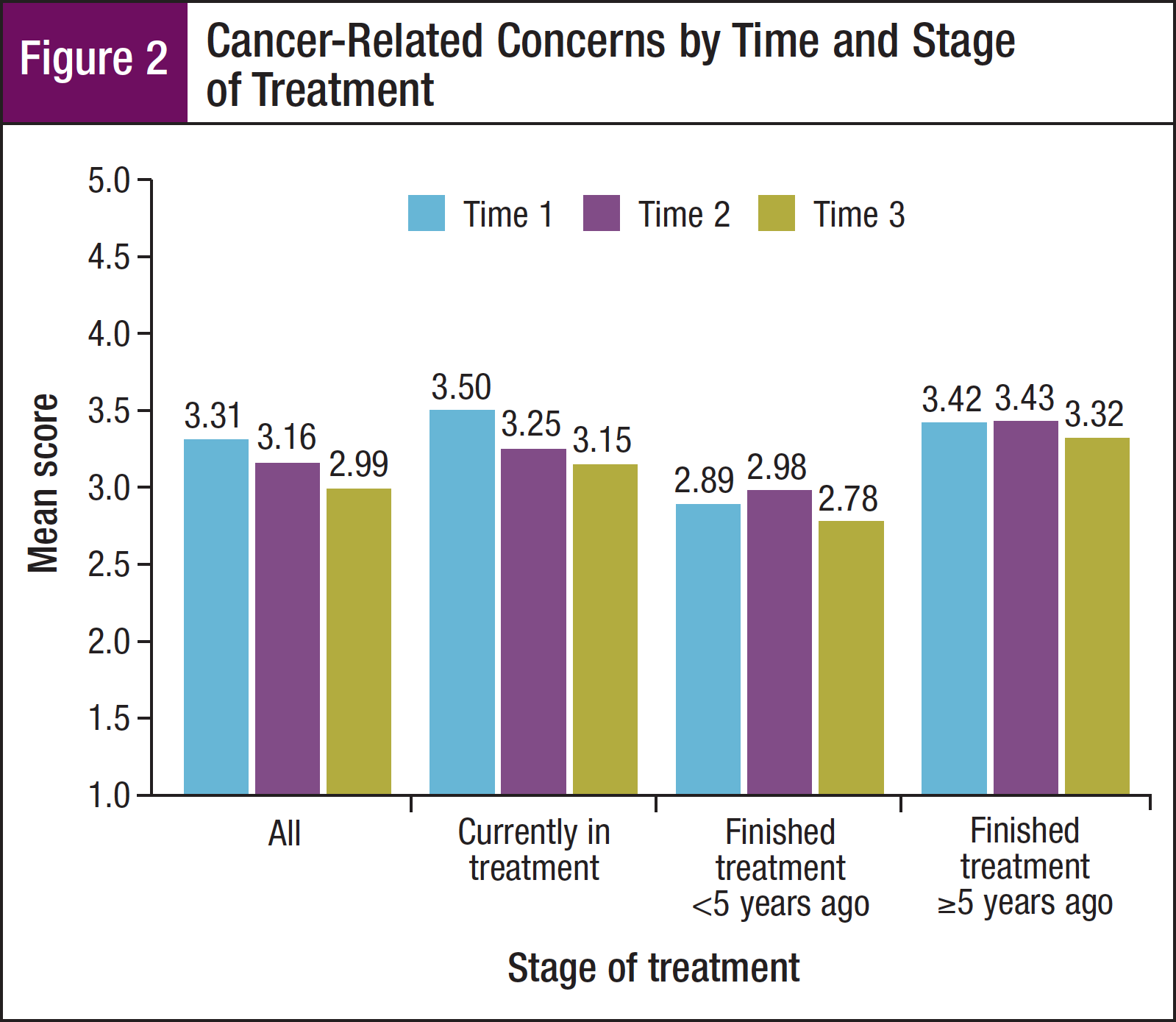
Perceived impact of cancer-related concerns. Survivors’ mean cancer-related concerns scores decreased significantly over time, from a mean of 3.31 at T1 to 2.99 at T3 (P <.05; Figure 2). At all 3 time points, survivors diagnosed with cancer <5 years ago had the lowest cancer-related concerns scores; the differences were significant only at T1 and T3. Similarly, survivors who were diagnosed at age ≥60 years had lower cancer-related concerns scores than those diagnosed at a younger age (P <.001 at T1; P = .07 at T2; P <.05 at T3).
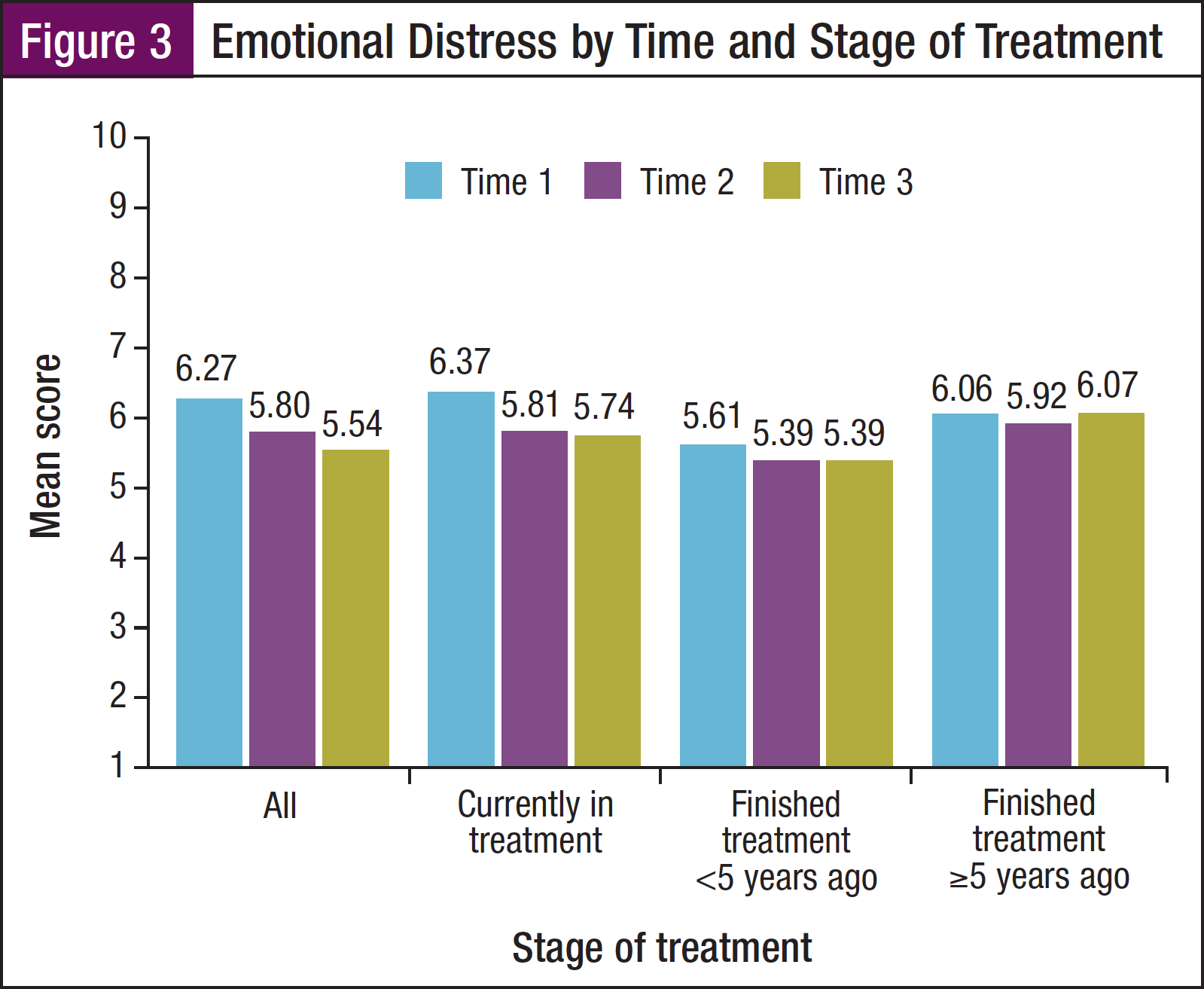
Emotional distress. Overall, the mean distress scores significantly decreased over time, from T1 (mean, 6.27) to T2 (mean, 5.80) and to T3 (mean, 5.54; P <.05; Figure 3). In addition, the distress scores varied significantly by stage of treatment at T1 (P <.001) and T3 (P = .014). At both time points, the distress was lowest among the participants who were diagnosed <5 years ago. Males had significantly higher mean distress scores than females at all 3 data collection points (mean, 6.49 vs 5.82 at T1, P <.001; 6.01 vs 5.39 at T2, P <.005; and 5.81 vs 4.96 at T3, P <.001).
Satisfaction with LIVESTRONG Navigation Services
Overall, participants were highly satisfied with LIVESTRONG Navigation. For the study participants as a whole, the mean satisfaction score was 4.22 (standard deviation, 1.06) of a maximum score of 5. Participants who were diagnosed at age 15 to 39 years were more satisfied (mean, 4.32) than participants who were diagnosed at age 40 to 59 (mean, 4.13; P = .05). Participants who finished their treatment <5 years ago were significantly more satisfied than those who finished their treatment ≥5 years ago (mean, 4.25 vs 4.17 for patients who are currently in treatment and 3.88 for those who finished treatment ≥5 years ago; P <.05).
We also conducted regression analyses to understand predictors of satisfaction at T3. Controlling for other factors, the participants who had more interactions with LIVESTRONG reported greater satisfaction (B = 0.013; standard error, 0.01; P = .013). In addition, participants who received support from an ESN reported greater satisfaction (B = 0.29; standard error, 0.10; P = .004).
Impact of Emotional Support Navigator
The changes in self-efficacy over time varied significantly according to whether cancer survivors had an ESN (Wald X2[2] = 8.33; P = .016). Although they started out at T1 with poorer self-efficacy, participants who had an ESN experienced consistent increases in self-efficacy over time and at T3 had similar scores to the participants who did not have an ESN.
We also found that having an ESN was associated with significant reductions in the impact of cancer-related concerns over time (Wald X2[2] = 13.40). Cancer survivors who had an ESN reported a greater impact of cancer-related concerns at T1 and T2, but this impact was reduced over time, and at T3, those who had an ESN reported similar levels of impact to those who did not have an ESN.
Finally, there is a general trend of differences in distress over time based on receiving ESN services (Wald X2[2] = 5.60; P = .061). Participants who had an ESN reported lower distress at T1 and T3, but higher-stress at T2, than those who did not have an ESN, although their T2 values were lower than their T1 values, suggesting a reduction in distress over time.
Discussion
LIVESTRONG Navigation has developed a model of patient navigation that addresses cancer survivors’ needs outside the clinical setting. The services encompass areas that are often not addressed within traditional oncology care settings, including employment, insurance, and financial issues; emotional counseling; and fertility preservation assistance. These findings augment the growing body of evidence about the benefits of patient navigation services, highlight the importance of navigation support for cancer survivors outside the clinical setting, and suggest that the partnership model used by LIVESTRONG is effective in meeting cancer survivors’ diverse needs.
We assessed the impact of navigation services on outcomes of interest, specifically self-efficacy, perceived impact of cancer-related concerns, and distress of cancer survivors. As a whole, survivors’ self-efficacy increased over time, and cancer-related concerns and distress concerns each decreased over time. In addition, participants had an enormous need for emotional support; it was the most frequently reported need among the survivors as a whole and across all the subgroups examined, with the exception of nonwhites, for whom insurance and financial issues were the top concerns.
Participants who had an ESN benefited from increased self-efficacy, specifically confidence in their ability to get emotional support, to talk with healthcare providers about personal problems related to their diagnosis, and to take action to make themselves feel better. These participants also had lower levels of distress and cancer concerns after receiving emotional support services. Because psychosocial care is not a standard service across oncology care settings, LIVESTRONG Navigation services can help to meet the needs for emotional support among cancer survivors.
These findings showed that the participants who finished their cancer treatment more recently (<5 years ago) were more satisfied with LIVESTRONG Navigation and had greater self-efficacy than those who finished their cancer treatment ≥5 years ago. We also found differences in satisfaction with LIVESTRONG Navigation and self-efficacy by age at diagnosis. Participants who were diagnosed with cancer as adolescents or as young adults had the highest satisfaction levels.
Participants who were diagnosed with cancer as a child had the lowest self-efficacy. LIVESTRONG Navigation has a special focus on adolescents and young adults; therefore, these findings suggest that efforts to meet the needs of young survivors have been effective.
These findings have led LIVESTRONG to review the services it provides to support longer-term cancer survivors and pediatric cancer survivors, and to conduct additional research to understand their needs.
Overall, the participants reported high levels of satisfaction with LIVESTRONG Navigation. Participants with more needs and who had a higher number of interactions with a navigator reported greater satisfaction, suggesting that multiple “touch points” are often needed to meet survivors’ varied needs, and for navigators to build a trusting and supportive relationship with survivors.
Limitations
These results should be considered in light of the study’s limitations. Because the study did not involve a control group, we must consider the findings about impact on outcomes of interest to be suggestive.
Another limitation is that some of the data collection instruments were developed primarily for programmatic rather than for evaluation purposes. For example, survivor needs and services delivered did not use the exact same categories, making it difficult to definitively say that the program delivered the service that was needed.
Finally, we were unable to assess the impact of LIVESTRONG’s partners, because there was no way to isolate the impact of the partner organizations’ services over and above the services provided directly by LIVESTRONG.
To address these limitations, LIVESTRONG plans to implement a new case management system that will facilitate the assessment of how partner organizations meet survivor needs, and whether unmet needs remain, and is developing follow-up surveys that are specific to the types of services provided. LIVESTRONG is also considering the viability of using an experimental design and a more refined approach to examine the level of services received (eg, beyond the number of interactions with a navigator) and the impact of various services.
Conclusion
Overall, the findings highlight the importance of patient navigation services at all points of a patient’s cancer journey and the value of the LIVESTRONG model, which augments community-based and clinic-based navigation services. LIVESTRONG is using these findings to guide further development and evaluation of its navigation services.
Support services outside the clinical setting can help to meet the needs of cancer survivors and should be considered by clinical care providers to ensure the best outcomes for survivors. LIVESTRONG is positioned to partner with hospitals and physicians to provide psychosocial screening and care that meet the Commission on Cancer standards.
Author Disclosure Statement
The authors have no conflicts of interest to report. This study was funded by the LIVESTRONG Foundation.
For information about partnering with LIVESTRONG, contact: Emily Eargle, MSSW, Director, Navigation Services, LIVESTRONG Foundation, 2201 E. 6th St, Austin, TX 78702, phone: 512-279-8431, This email address is being protected from spambots. You need JavaScript enabled to view it..
References
- Paskett ED, Harrop JP, Wells KJ. Patient navigation: an update on the state of the science. CA Cancer J Clin. 2011;61:237-249.
- Battaglia TA, Burhansstipanov L, Murrell SS, et al; for the Prevention and Early Detection Workgroup from the National Patient Navigation Leadership Summit. Assessing the impact of patient navigation: prevention and early detection metrics. Cancer. 2011;117(15 suppl):3553-3564.
- Guadagnolo BA, Dohan D, Raich P. Metrics for evaluating patient navigation during cancer diagnosis and treatment: crafting a policy-relevant research agenda for patient navigation in cancer care. Cancer. 2011;117(15 suppl):3565-3574.
- Wells KJ, Battaglia TA, Dudley DJ, et al; for the Patient Navigation Research Program. Patient navigation: state of the art or is it science? Cancer. 2008;113:1999-2010.
- Willis A, Pratt-Chapman M, Reed E, Hatcher E. Best practices in patient navigation and cancer survivorship: moving toward quality patient-centered care. J Oncol Navig Surviv. 2014;5(2):8-14.
- Commission on Cancer; American College of Surgeons. Cancer program standards 2012: ensuring patient-centered care. Version 1.2.1. 2012. www.facs.org/cancer/coc/programstandards2012.pdf. Accessed April 30, 2015.
- Allen JO, Zebrack B, Wittman D, et al. Expanding the NCCN guidelines for distress management: a model of barriers to the use of coping resources. J Community Support Oncol. 2014;12:271-277.
- Carlson LE, Waller A, Mitchell AJ. Screening for distress and unmet needs in patients with cancer: review and recommendations. J Clin Oncol. 2012;30:1160-1177.
- Esparza A. Patient navigation and the American Cancer Society. Semin Oncol Nurs. 2013;29:91-96.
- Sharpe K, Perocchia RS, Wiatrek DE, Shaw B. Milestones in mission: the work of the American Cancer Society’s mission delivery. J Cancer Educ. 2013;28:4-8.
- Printz C. Not at any cost: organizations help patients cope with costs of cancer care. Cancer. 2011;117:879-881.






