Background: Fear of cancer recurrence (FCR) is one of the most reported unmet needs of cancer survivors, including gynecologic cancer survivors. Greater perceived risk of cancer recurrence has been found to be associated with increased cancer worry among gynecologic cancer survivors. A better understanding of FCR in cancer survivors can help clinicians manage this problem effectively.
Objective: The objective of this study was to describe the similarities and differences in FCR experienced by gynecologic cancer survivors.
Methods: A secondary data analysis was conducted on the data collected by the author for her dissertation. The original data were collected using a web-based survey among the survivors of cervical, ovarian, and uterine cancer. Descriptive statistics, Pearson correlation coefficient, t test, and Mann-Whitney U test were used for data analyses.
Results: FCR was not significantly different between cancer types. Survivors of younger age and shorter disease-free interval reported more FCR. As age and survivorship duration increased, the FCR decreased. A lower FCR score was noted in nonwhite participants. The number of disease-free years (survivorship duration) was significantly correlated with FCR only in white participants.
Conclusion: This study concluded that FCR differs based on the cancer survivor’s age. Although there are inconsistencies in the literature, this study found that FCR decreased as the disease-free interval increased. The result showed only a marginal difference in the FCR between ethnic groups; however, some previous studies found no difference, whereas others reported a difference in FCR based on ethnicity. Results based on ethnicity in this study should be viewed with caution due to the small number of nonwhite participants.
Cancer recurrence is defined as the return of cancer after treatment completion and after a length of time during which the cancer could not be detected.1 Fear of cancer recurrence (FCR) is a known problem for many cancer survivors that interfere with their quality of life.2-4 FCR is defined as the experience of worry and concern that cancer might return to the same organ or spread to another part of the body.5 FCR causes significant emotional burden in cancer patients.6 A higher perceived risk of cancer recurrence is found to be associated with increased cancer worry among gynecologic cancer survivors and breast cancer survivors.7,8 Studies indicate that high FCR may be correlated with posttraumatic stress disorder in long-term survivors.9 A better understanding of FCR in cancer survivors can help clinicians manage this problem effectively. The objective of this study was to describe the similarities and differences in FCR experienced by gynecologic cancer survivors.
Methods
The data for this study were previously collected by the author for her dissertation. The original data were collected between March 23, 2013, and May 17, 2013. The University of Texas Medical Branch at Galveston provided the internal review board approval. The data collection was done using a web-based survey. The sample consisted of English-speaking women who were survivors of cervical, uterine, and ovarian cancer, aged ≥21 years, and disease-free for at least 2 years following treatment completion.
This study defined “cancer survivors” as those who have completed treatment at least 2 years prior to data collection and remained disease-free since completion of cancer treatment. The participants who were disease-free for 2 to 5 years from treatment completion were considered early survivors, and those who were disease-free for over 5 years were considered long-term survivors. For the current study, participants’ responses to the Fear of Relapse/Recurrence Scale and demographic information, including participant’s age, diagnosis, ethnicity, and disease-free interval, were included.
Fear of Relapse/Recurrence Scale
The Fear of Recurrence/Relapse Scale was used to measure FCR.10,11 This scale consists of 5 items that measure patients’ belief and anxiety concerning their disease recurring relevant to cancer survivor populations. All items on this scale were rated on a 5-point Likert scale (1 = strongly agree, 2 = agree, 3 = not certain, 4 = disagree, and 5 = strongly disagree). Items 1, 2, 3, and 4 were reverse-coded and summed so that higher scores indicated a greater fear of recurrence. In the current study, this instrument had a good internal consistency, α = .845.
Data Analysis
Descriptive analysis of the data was performed using frequency distribution. To examine the FCR between groups, 2 groups were created based on the age (younger vs older) using mean split (age 57 years). Based on disease-free interval (survivorship status), the sample was again divided into 2 groups: early survivor (2-5 years) and long-term survivor (>5 years). Ethnicity was divided into whites and nonwhites (Table 1). Pearson correlation coefficient was used to evaluate the relationship between variables. Mann-Whitney U analyses and t tests were performed to examine the differences in the FCR between groups.
Results
A total of 632 women responded to the original survey; 352 women who completed all questionnaires were included in the final analyses. The mean age of participants was 57.07 years (SD, 10.12; range, 29-80 years). The mean disease-free interval was 5.65 years (SD, 4.71; range, 2-30 years). Women from 5 different ethnicities represented the sample: non-Hispanic white (88.9%), Hispanic white (3.7%), African American (1.4%), Hispanic (2.3%), and Asian (3.7%). The ethnicity was again divided into 2 groups for subsequent analysis: white (92.6%) and nonwhite (7.4%). All ethnic groups except non-Hispanic white were combined to form 1 group of nonwhites. The diagnoses included ovarian cancer (59.7%), uterine cancer (31.3%), and cervical cancer (9.1%). The sample consisted of younger survivors (47.2%) and older survivors (52.8%). There were more early survivors (2-5 years; 65.6%) than long-term survivors (>5 years; 34.4%).
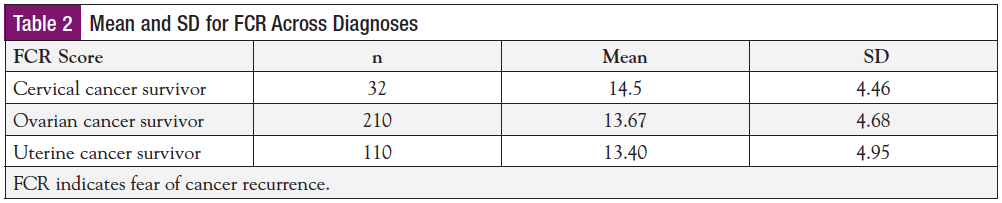
Nonwhite gynecologic cancer survivors reported a lower FCR than white survivors. The FCR score was only slightly higher in the younger age-group than in the older age-group. A higher FCR score was seen among early survivors than long-term survivors, which suggests that less time since treatment completion may be associated with higher FCR in early survivors. The significance of the difference in FCR within each group will be described in the subsequent analyses. The FCR mean score was similar among cervical, ovarian, and uterine cancer survivors (Table 2).
Pearson correlation coefficient analysis was performed to explore the relationship of FCR with age and survivorship duration (number of disease-free years) within the ethnic groups (Table 3).
A negative correlation was noted between FCR and age and FCR and survivorship duration in both whites and nonwhites, indicating that as age and survivorship duration increased, the FCR decreased. Age and FCR showed a stronger correlation in whites and nonwhites, which shows that age is a determining factor for FCR for both white and nonwhite cancer survivors. The result indicated that for white participants, the number of disease-free years (survivorship duration) had a significant association with FCR, but for nonwhite participants, the disease-free years did not demonstrate a significant impact on FCR (Table 3).
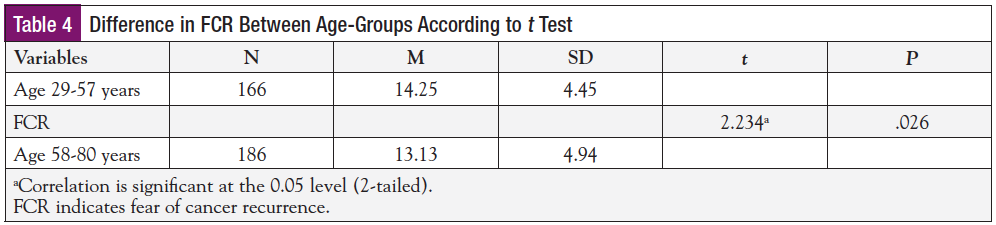
The current study also explored the difference in FCR based on age, ethnicity, and disease-free interval. The FCR score was slightly higher in the younger age-group than the older age-roup. Examination of the differences in FCR between younger and older survivors using t tests (Table 4) showed a significant difference between the age-groups, suggesting that the younger age-group experienced more FCR than the older age-group (P = .026).
To examine the difference in FCR between ethnic groups and based on survivorship status, a nonparametric statistical test (Mann-Whitney U) was used (Table 5). A lower mean score of FCR was noted in nonwhites compared with whites. However, the difference in FCR between the ethnic groups was only marginally significant (P = .065), which suggests that ethnicity may not have a significant impact on FCR. Early survivors reported a higher FCR mean score compared with long-term survivors. The difference in FCR between early versus long-term survivors was statistically significant (Table 5), indicating that early survivors experienced greater fear of recurrence than long-term survivors (P <.001).
Discussion
Studies indicate that cancer survivors experience FCR.4-6,12 In the current study, the FCR score was similar among ovarian, uterine, and cervical cancer survivors. The results from this study indicated that as age increased, the FCR recurrence decreased. Examination of the differences in FCR between younger and older survivors showed a significant difference between the age-groups, indicating that the younger survivors experienced more FCR than the older survivors. This difference in FCR between younger and older survivors is consistent with other studies.13-15 In a study of 1128 long-term breast cancer survivors 3 to 8 years following a cancer diagnosis, it was found that younger women experienced more FCR than older women.14 Similarly, another study with 252 breast and endometrial cancer survivors also found that younger cancer survivors scored poorly on FCR score.13 A 2-year follow-up study of breast cancer survivors also found that younger age was consistently associated with higher FCR.15 In contrast to these findings, another study involving 153 postmenopausal women with early-stage breast cancer taking adjuvant endocrine therapy found no significant difference in FCR between younger and older participants.16 The difference in the findings could be related to the diagnosis or time since diagnosis. However, findings from a majority of the studies support the fact that FCR differs based on the age of the cancer survivors, and it is consistent with the result from the current study.
This study also showed that as survivorship duration (number of disease-free years) increased, FCR decreased. An evaluation of the longitudinal trends of FCR in 189 posttreatment head and neck cancer survivors showed that approximately 50% did not experience significant levels of FCR; approximately 20% experienced significant levels of FCR intermittently; and approximately 30% experienced significant levels of FCR over time.17 Similarly, an evaluation of FCR in prostate cancer patients undergoing treatment reported fairly constant FCR over time.18 Another study that assessed the predictors of FCR in breast cancer survivors over a period of 18 months after surgery found that younger survivors had higher FCR during the first 1.5 years after breast surgery, but older survivors reported stable levels of FCR during the first 6 months after surgery, after which the FCR declined.19 These findings are different from the findings in the current study. The differences could be related to the type of cancer, type of treatment, or other factors such as age or ethnicity. In fact, the number of disease-free years was significantly correlated with FCR in white participants in this study.
A lower score of FCR was noted in nonwhite participants compared with whites in the current study. However, the difference in FCR between the ethnic groups was only marginally significant (P = .065), suggesting that ethnicity may not have a significant impact on FCR. A study that evaluated FCR in patients treated with surgery for pancreatic and periampullary neoplasms showed a clinically significant level of FCR associated with nonwhite ethnicity (P = .012).20 However, a 2-year longitudinal study following surgery for breast cancer found no difference in FCR based on race.15 Although not supported by findings from this study, it is possible that the difference in FCR could be related to the cancer type.
Conclusion
FCR is one of the most reported unmet needs of cancer survivors, including gynecologic cancer survivors. A study with long-term early-stage ovarian cancer survivors found a significant amount of distress related to FCR (22%) and fear of a second cancer (36%).21 In a similar study, 56% of early-stage ovarian cancer survivors reported to have FCR.12 Another evaluation of 199 gynecologic cancer survivors found that FCR was the most endorsed need among this group (24%).22 In summary, gynecologic cancer survivors do experience FCR, and the literature supports the fact that FCR in this group of cancer survivors ranges from at least 22% to 56%, and this is of great concern.12,21,22
This study supports the fact that gynecologic cancer survivors experience FCR. Although there are some differences in the results compared with the existing literature, this study found that younger age and shorter interval from treatment was associated with increased FCR. A lower FCR score was noted in nonwhite participants, whereas the difference between ethnic groups was not significant. The disease-free years was significantly correlated with FCR only in white participants. However, the findings based on ethnicity should be viewed with caution because of the small number of nonwhite participants. Differences in the findings are believed to be related to the type of cancer, type of treatment, or other factors such as age or ethnicity.
Implications for Research and Practice
As revealed by the results, FCR is a problem among the gynecologic cancer survivors. Screening for FCR and development of appropriate interventions to address this issue are recommended. It is also suggested to undertake a future research study using direct data collection to control participant demographics.
Limitations
The sample had an overrepresentation of ovarian cancer survivors and white participants. This study was limited to English-speaking women. Self-selection and self-reporting bias are other limitations. Another limitation is that this study did not assess FCR over time.
References
1. American Cancer Society. What is cancer recurrence? www.cancer.org/treatment/survivorship-during-and-after-treatment/understanding-recurrence/what-is-cancer-recurrence.html. 2016.
2. Bradley S, Rose S, Lutgendorf S, et al. Quality of life and mental health in cervical and endometrial cancer survivors. Gynecol Oncol. 2006;100:479-486.
3. Cimprich B, Ronis D, Martinez-Ramos G. Age at diagnosis and quality of life in breast cancer survivors. Cancer Pract. 2002;10:85-93.
4. Urbaniec OA, Collins K, Denson LA, Whitford HS. Gynecological cancer survivors: assessment of psychological distress and unmet supportive care needs. J Psychosoc Oncol. 2011;29:534-551.
5. Vickberg SM. The Concerns About Recurrence Scale (CARS): a systematic measure of women’s fears about the possibility of breast cancer recurrence. Ann Behav Med. 2003;25:16-24.
6. Hong YM, Hu JC, Paciorek AT, et al. Impact of radical prostatectomy positive surgical margins on fear of cancer recurrence: results from CaPSURE. Urol Oncol. 2010;28:268-273.
7. Goncalves V. Long-term quality of life in gynecologic cancer survivors. Curr Opin Obstet Gynecol. 2010;22:30-35.
8. Phillips KM, McGinty HL, Gonzalez BD, et al. Factors associated with breast cancer worry 3 years after completion of adjuvant treatment. Psychooncology. 2013;22:936-939.
9. Mehnert A, Berg P, Henrich G, Herschbach P. Fear of cancer progression and cancer-related intrusive cognitions in breast cancer survivors. Psychooncology. 2009;18:1273-1280.
10. Kornblith AB. Psychosocial adaptation of cancer survivors. In: Holland JC, ed. Psychooncology. New York, NY: Oxford University Press; 1998:223-254.
11. Greenberg DB, Kornblith AB, Herndon JE, et al. Quality of life of adult leukemia survivors treated on clinical trials of Cancer and Leukemia Group B during the period 1971-1988: predictors for later psychological distress. Cancer. 1997;80:1936-1944.
12. Matulonis UA, Kornblith A, Lee H, et al. Long-term adjustment of early-stage ovarian cancer survivors. Int J Gynecol Cancer. 2008;18:1183-1193.
13. Kornblith AB, Powell M, Regan MM, et al. Long-term psychosocial adjustment of older vs younger survivors of breast and endometrial cancer. Psychooncology. 2007;16:895-903.
14. Ziner KW, Sledge GW, Bell CJ, et al. Predicting fear of breast cancer recurrence and self-efficacy in survivors by age of diagnosis. Oncol Nurs Forum. 2012;39:287-295.
15. Liu Y, Pérez M, Schootman M, et al. Correlates of fear of cancer recurrence in women with ductal carcinoma in situ and early invasive breast cancer. Breast Cancer Res Treat. 2011;130:165-173.
16. Corter AL, Findlay M, Broom R, et al. Beliefs about medicine and illness are associated with fear of cancer recurrence in women taking adjuvant endocrine therapy for breast cancer. Br J Health Psychol. 2013;18:168-181.
17. Ghazali N, Cadwallader E, Lowe D, et al. Fear of cancer recurrence in patients undergoing definitive treatment for prostate cancer: results from CaPSURE. Psychooncology. 2013;22:807-813.
18. Mehta SS, Lubeck DP, Pasta DJ, Litwin MS. Fear of cancer recurrence in patients undergoing definitive treatment for prostate cancer: results from CaPSURE. J Urol. 2003;170:1931-1933.
19. Starreveld DEJ, Markovitz SE, van Breukelen G, Peters ML. The course of fear of cancer recurrence: different patterns by age in breast cancer survivors. Psychooncology. 2017;27:295-301.
20. Petzel MQ, Parker NH, Valentine AD, et al. Fear of cancer recurrence after curative pancreatectomy: a cross-sectional study in survivors of pancreatic and periampullary tumors. Ann Surg Oncol. 2012;19:4078-4084.
21. Wenzel LB, Donnelly JP, Fowler JM, et al. Resilience, reflection, and residual stress in ovarian cancer survivorship: a Gynecologic Oncology Group study. Psychooncology. 2002;11:142-153.
22. Hodgkinson K, Butow P, Fuchs A, et al. Long-term survival from gynecologic cancer: psychosocial outcomes, supportive care needs and positive outcomes. Gynecol Oncol. 2007;104:381-389.