Patient navigation has been shown to improve patient engagement and enrollment in clinical trials1,2 and increase utilization of supportive cancer care.3,4 However, oncology patient navigation is not universally provided5 or measured. Patient navigation in cancer care refers to specialized assistance for the community, patients, families, and caregivers to overcome barriers to receive care and facilitate timely access to clinical services and resources. Navigation processes encompass prediagnosis through all phases of the cancer experience.6 The navigation services implemented will depend on the particular type, severity, and complexity of the identified barriers.6
A national subcommittee was formed by the Academy of Oncology Nurse & Patient Navigators (AONN+) in 2016 called the Navigation Metrics Subcommittee. One of its goals was to support the work of the AONN+ Evidence into Practice Committee and the Navigation Metrics Project, which spearheaded the team that developed the 35 evidence-based standardized metrics in the areas of patient experience (PE), clinical outcomes (CO), and return on investment (ROI) utilizing navigation core competencies, national guidelines, and value-based cancer care metrics to support our present healthcare landscape in oncology. The end goal was to provide standardized national evidence-based navigation metrics that could be utilized by any model of navigation to ensure program success and sustainability.
Evidence into Practice Committee
Navigation Metrics Subcommittee
The objective of this initiative was to develop standardized metrics in the areas of PE, CO, and ROI using the AONN+ DOMAINS for certification. These domains contain a comprehensive list of all areas in which navigators practice to provide quality patient care and financial stability for their organizations.
The Navigation Metrics Subcommittee was inspired by a discussion at the Evidence into Practice Committee at the AONN+ annual conference in November 2015. The committee members reviewed how each navigation program was collecting different metrics—and some programs failed to collect any data—to determine efficacy and satisfaction. Because programs were collecting different metrics (or not collecting any data), and data were inconsistent, there are no established benchmarks for navigation programs nationally. The conclusion was that the AONN+ members needed to take the lead on creating evidence-based navigation metrics in the categories of PE, CO, and ROI. The chairs of the Evidence into Practice Committee, Elaine Sein, BSN, RN, and Danelle Johnston, MSN, RN, ONN-CG, OCN, reviewed the analytics and determined that we should talk with the AONN+ and The Lynx Group leadership to get their approval and discuss next steps. The leadership team requested a proposal and outline to provide detail on the scope of the navigation metrics project. The proposal was completed and approved. This work was developed by the navigation metrics project team and would become the ongoing goal of the Navigation Metrics Subcommittee to support additional initiatives that support the AONN+ metrics.
AONN+ Navigation Metrics Subcommittee Members
The Navigation Metrics Subcommittee meets on a regular basis, develops and ranks the goals to prioritize the work for the year. The team meets monthly, virtually, and goals are listed on the monthly agendas. New work teams are created to support the goals and report back to the committee on a regular basis. Sixteen team members have been selected for their expertise in specific yet unique areas. The team boasts participation from diverse institutions across the United States, such as Chartis Oncology Solutions; The University of Arizona; HonorHealth Research Institute; Miami Cancer Institute; Hendricks Regional Health; Olcott Center, Indiana University Health Bloomington; Northside Hospital Cancer Institute; Capital Health Cancer Center; Baylor Scott & White Health, Baylor University Medical Center Dallas; Saint Joseph Hospital, Cancer Centers of Colorado; Greenville Health System Cancer Institute; Native American Cancer Research Corporation; University of South Alabama Mitchell Cancer Institute; University of Vermont Cancer Center; and Saint Luke’s South Hospital Goppert Breast Center.
Program Objectives
The program included the following objectives: To describe a novel AONN+ Navigation Metrics Subcommittee team designed to support the AONN+ evidence-based standardized metrics in multiple areas for nurse navigation programs to facilitate quality coordinated patient care and financial stability for their institutions. Documents have been created by the team to meet this objective.
Methods
The purpose of the AONN+ Navigation Metrics Subcommittee is to support through tool development the standardized metrics for the population of national navigators in the United States. This has involved designing items for an online assessment tool that will comprise quantitative data (survey; Likert-type responses) and potentially some open-ended items (qualitative data), thus employing a mixed methods approach.
Navigation Goals for 2018-2019
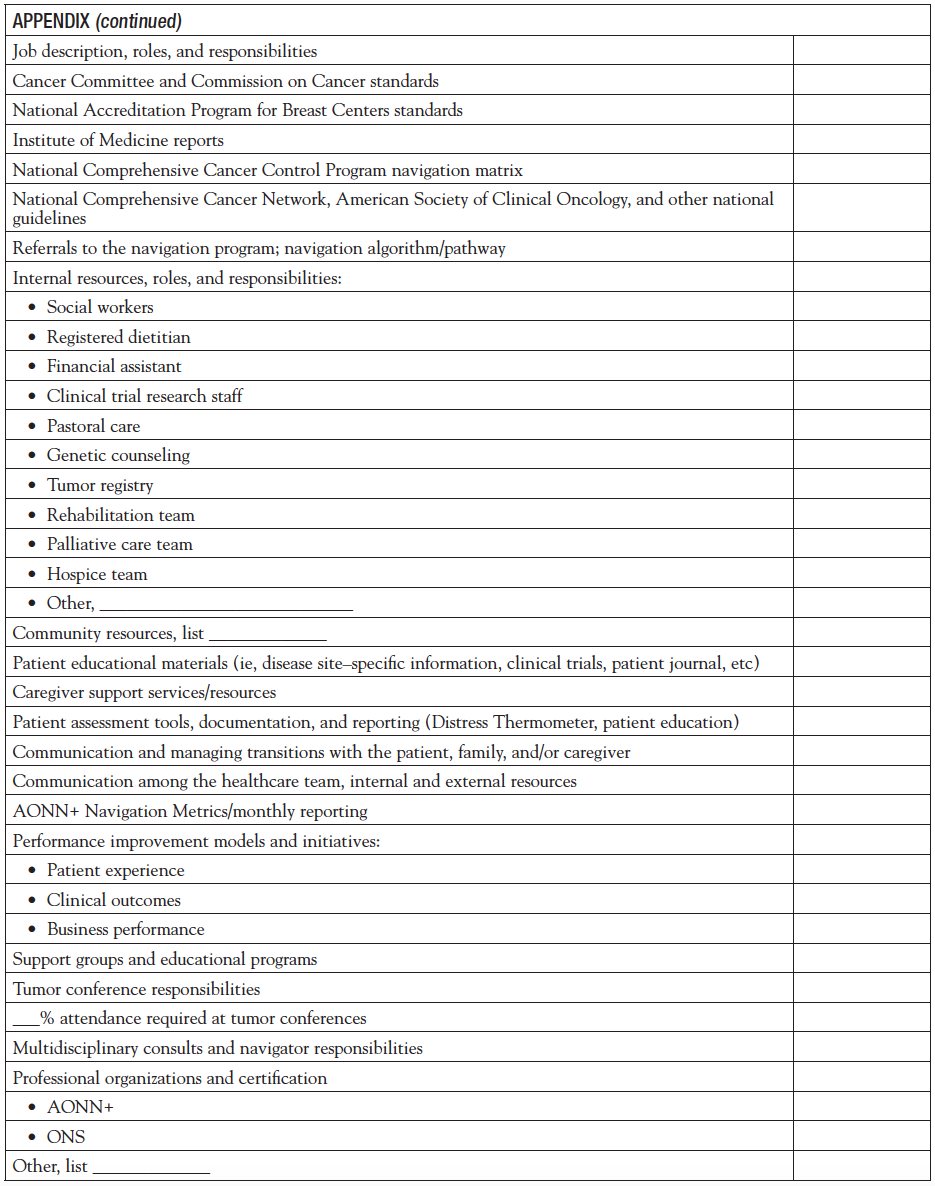
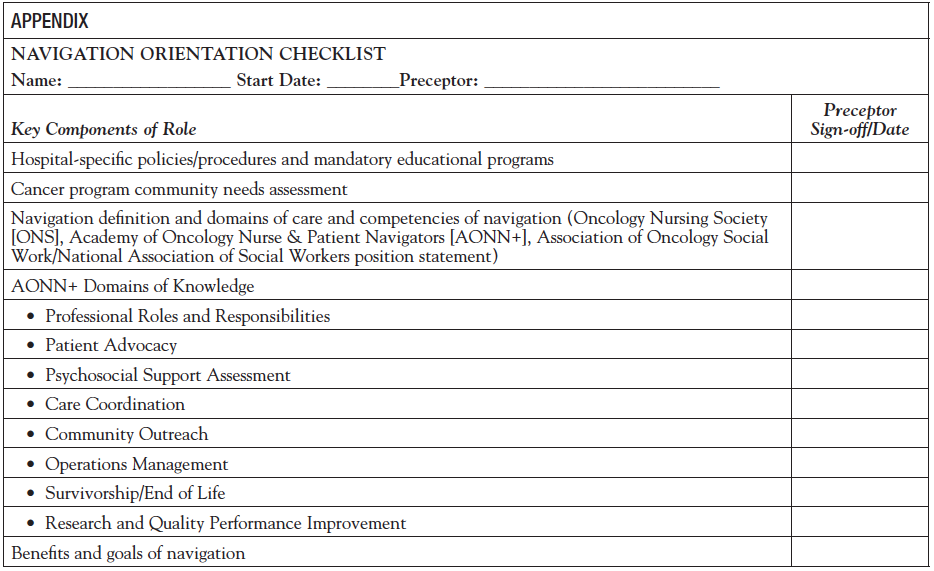
During the team meetings, members suggested and approved several goals and objectives for the following years. They included developing a navigation acuity tool and providing value-based cancer care education to navigators, administrators, and providers. The navigation acuity tool was initially discussed by the Navigation Metrics Subcommittee but transitioned to a larger initiative of AONN+ that included 10 national experts who would participate on the team to work on the AONN+ evidenced-based navigation acuity tool. The Navigation Metrics Subcommittee members created some very important tools that would support navigators and the committee goals, which included patient and provider experience surveys, navigation orientation and annual competencies, and a provider fact sheet to help educate physicians and their office staff on the role of the navigator (Appendix).
The Patient and Provider Navigation Experience Survey
An important AONN+ navigation metric measures PE as it relates to the navigator. Navigators deserve to receive this important feedback on their role as well as to utilize the feedback from patients and their caregivers to enhance the navigation program. This metric falls under the AONN+ Research, Quality, and Performance Improvement domain. The navigation patient experience survey was based on the results from the CAHPS Cancer Care Survey sponsored by the Agency for Healthcare Research and Quality and the Patient-Centered Care Research Program of the Outcomes Research Branch of the National Cancer Institute. The California Healthcare Foundation provided seed money, and the design and research were carried out by the American Institutes for Research and Mayo Clinic. The summary of findings was published in 2013. The questions that were incorporated included the categories of shared decision-making, treatment information, effective communication, and enabling patient self-management; these components were extremely different from the typical patient satisfaction questions.
It is essential that we also keep our providers engaged in the navigation program development and enhancement. The metrics team members discussed and created a provider experience survey to measure the effectiveness of the navigator and support staff, as well as to request feedback on how to further enhance the navigation program and identify future goals of the program.
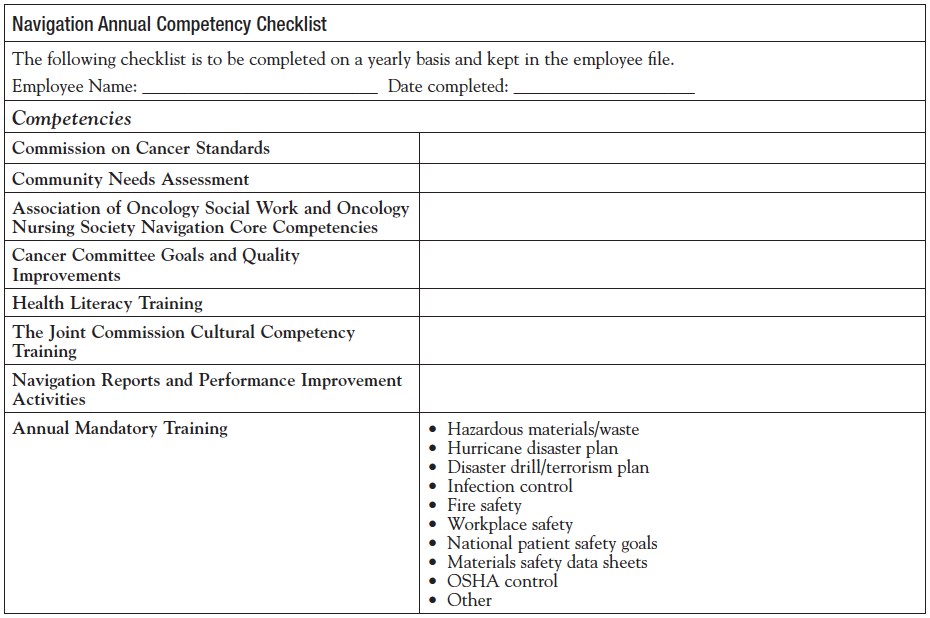
Navigation Orientation and Annual Competencies
Within the domain of Professional Roles and Responsibilities, navigators receive orientation and an annual review of national standards, core competencies for the navigator, internal and external resources, guidelines, policies, and procedures, etc of the navigation program. The team discussed that many sites do not have a formal orientation checklist and annual competency checklist for onboarding new staff members. The orientation and annual competencies include national navigation core competencies and knowledge domains for the navigator, changes in national standards (ie, Commission on Cancer, National Accreditation Program for Breast Centers), new processes or resources, revisions of the community needs assessment, new cancer committee goals, health literacy and cultural competency training, summary of reports, metrics and performance improvement initiatives, as well as cancer program–specific mandatory educational programs (Appendix).
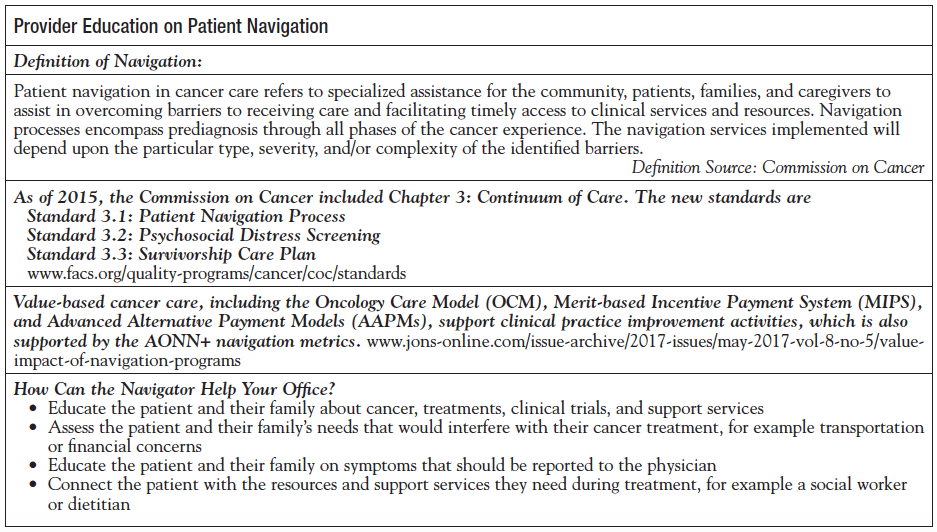
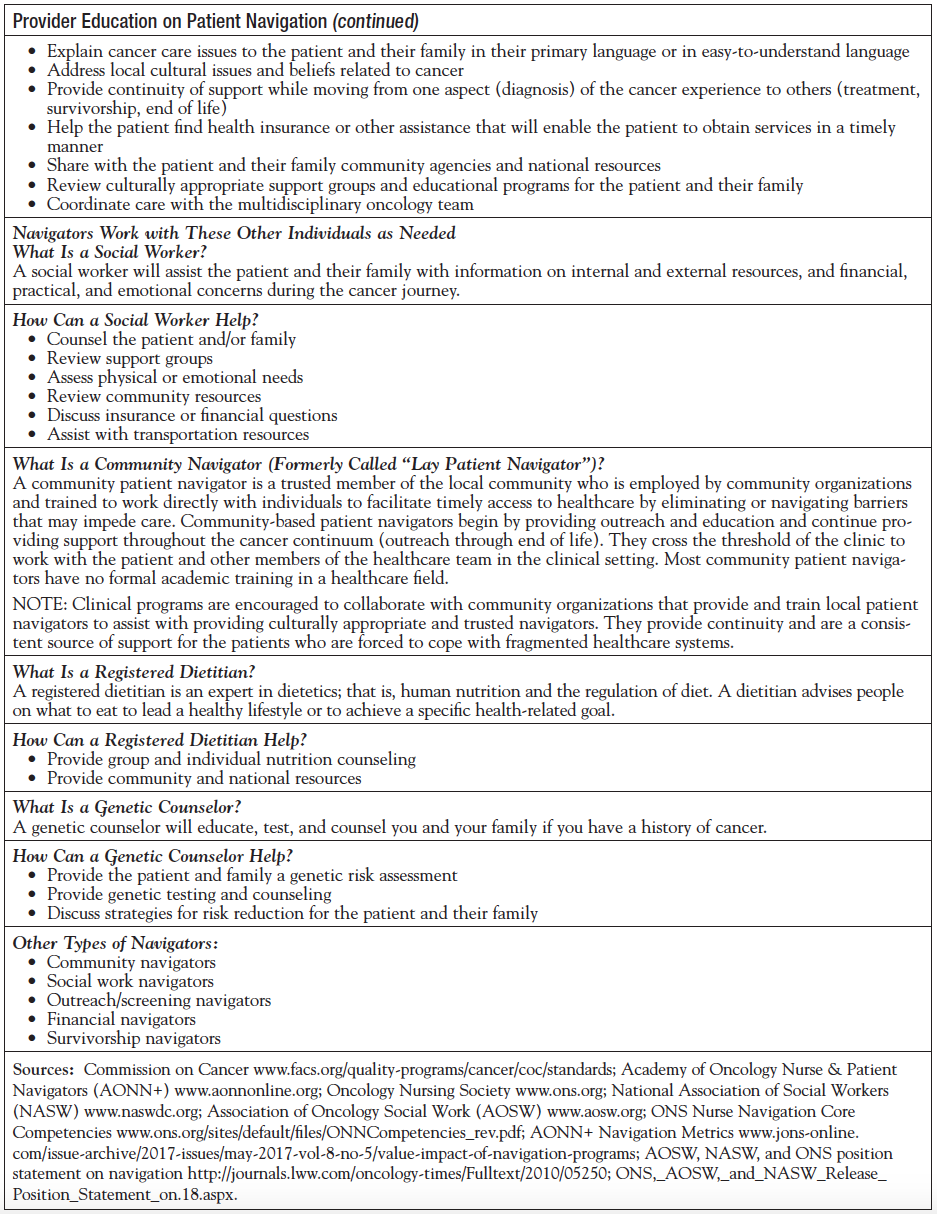
The Provider Fact Sheet for a Navigation Program
A stumbling block for navigators at times is how to explain their role as navigators to the providers in a concise, easy-to-understand manner. A navigator may state, “I coordinate care for my patients and their caregivers,” and although this is true, it does not clearly define the details of the role. We wanted to provide a short “elevator speech” that the navigators could utilize to clearly present their role and responsibility. This tool has been successfully tested and is now utilized by many cancer programs to educate not only the providers but also their staff and other departments. The document includes the definition of navigation, Commission on Cancer standards on navigation, and the core competencies and knowledge domains of a navigator (Appendix).
Next Steps and Results
The team discussed sharing the accomplishments of the Navigation Metrics Subcommittee and these documents at the AONN+ annual conference in 2018. The team created an abstract that was accepted, and the poster was created by the entire team. The poster abstract included the yearly goals, accomplishments, and deliverables/documents created (Appendix).
The Navigation Metrics Subcommittee was formed to gain feedback and participation from all models of navigation and include all the different disciplines; included are nurse navigators, social work navigators, lay navigators, administrators, and statisticians, to name just a few. The committee has been developing diverse assessment tools, and a current and future goal will be to conduct a pilot test to yield data. Data collection and analysis will be ongoing.
Other AONN+ Nationally Highlighted Projects
Early in 2018, AONN+ opened an exploratory first of its kind study titled, National Evidence-Based Oncology Navigation Metrics: Multisite Exploratory Study to Demonstrate Value and Sustainability of Navigation Programs to “assess the reliability and validity of 10 key navigation metrics” and “gain insight into the barriers and challenges navigation programs encounter during the implementation of navigation metrics.”8 This study, which is ongoing as of this writing, and future studies on navigation metrics are expected to further demonstrate the value of the work products coming out of the Navigation Metrics Subcommittee.
The second most noteworthy endeavor of AONN+ is the current undertaking focused on navigation-specific acuity. The Acuity Workgroup has been tasked to review the literature and come to an understanding of what navigation-specific acuity means, how it can be measured, and how an acuity score can be used within a larger acuity system to determine other relevant factors. These include navigation productivity, triaging for navigation protocols based on scoring, and monitoring acuity across disease sites to aid in determining additional supportive care needs, staffing, and delineation of roles. This work will lead to additional research studies, which will again move the needle even farther toward solidifying navigation as a necessary and important profession.
Conclusion
Since its inception, barely 3 years ago, the Navigation Metrics Subcommittee has proved to be a highly productive group as evidenced by the large body of work summarized in this article. Delivering quality products of this volume was possible due to the dedication and commitment of the experienced AONN+ leaders and team members of the subcommittee. This group’s desire to further the development of the navigation role through support of the AONN+ navigation metrics and the creation of other practical tools has resulted in the advancement of the navigation profession. Additionally, the team’s effort to disseminate these tools and to educate all AONN+ members has led to a stronger, more unified, and knowledgeable professional organization overall. Programs, nationally and internationally, now have a dedicated resource and team to help troubleshoot their unique program needs in the form of posing questions and getting guidance on a wide spectrum of topics, including how to start a navigation program, what data elements to incorporate when starting a program or working within an electronic system, how to track the basics for the financially scarce environment, tools to utilize throughout the navigation continuum, and the list goes on. Benchmarking and data established by the committee will aid in the difficult conversations with administrators and financial bodies as it relates to showing value, equating practice to downstream revenue, and the overall oncology navigation ROI in our already financially challenged healthcare environment. The Navigation Metrics Subcommittee members are fully engaged in improving AONN+ as an organization. By developing and providing resources, the committee, as an extension of AONN+, is providing support for navigators of all types and in all practices. By networking with attendees at the AONN+ national and midyear conferences, the committee is not only promoting their work and educating their colleagues, they are also demonstrating the value of belonging to an organization that is “dedicated to improving patient care and quality of life by defining, enhancing, and promoting the role of oncology nurse and patient navigators.”9
References
- Guadagnolo BA, Dohan D, Raich P. Metrics for evaluating patient navigation during cancer diagnosis and treatment: crafting a policy-relevant research agenda for patient navigation in cancer care. Cancer. 2011; 117(15 Suppl):3565-3574.
- Holmes DR, Major J, Lyonga DE, et al. Increasing minority patient participation in cancer clinical trials using oncology nurse navigation. Am J Surg. 2012;203:415-422.
- Steinberg ML, Fremont A, Khan DC, et al. Lay patient navigator program implementation for equal access to cancer care and clinical trials: essential steps and initial challenges. Cancer. 2006;107:2669-2677.
- Dohan D, Schrag D. Using navigators to improve care of underserved patients: current practices and approaches. Cancer. 2005;104:848-855.
- Braun KL, Kagawa-Singer M, Holder AE, et al. Cancer patient navigator tasks across the cancer care continuum. J Health Care Poor Underserved. 2012;23:398-413.
- Guthrie Robert Packer Hospital. Commission on Cancer. www.guthrie.org/patient-services/cancer/commission-cancer.
- Academy of Oncology Nurse & Patient Navigators. Academy of Oncology Nurse & Patient Navigators Announces Standardized Navigation Metrics. www.aonnonline.org/education/articles/10-aonn-announces-standardized-navigation-metrics. March 10, 2017.
- Academy of Oncology Nurse & Patient Navigators. National Evidence-Based Oncology Navigation Metrics: Multisite Exploratory Study to Demonstrate Value and Sustainability of Navigation Programs. https://aonnonline.org/education/standardized-metrics/navigation-metrics-quality-study. February 21, 2018.
- Academy of Oncology Nurse & Patient Navigators. About AONN+. https://aonnonline.org/about.