Addressing compassion fatigue in the oncology healthcare setting is an integral component of any oncology navigation program. Oncology navigators spend countless hours caring for patients, removing barriers, and ensuring they have resources available to remain compliant with their physician-prescribed treatment plan, all while providing emotional support to patients and their caregivers. It is important that organizational leaders recognize symptoms of compassion fatigue in the workplace such as high absenteeism, inability to work well with the team or complete assignments, and a negative attitude. To decrease the risk, the navigation program leadership must promote well-being in the workplace.
Compassion Fatigue vs Compassion Satisfaction
Compassion fatigue is displayed when a person feels exhausted due to multiple encounters of helping someone in distress. It has been described as the psychoemotional distress that develops when self-sacrificing behavior accompanied by ongoing exposure to difficult situations occurs.1 Navigators may feel numb and disconnected from their patients and caregivers during this period. Compassion fatigue often leads to burnout and secondary trauma. As oncology healthcare professionals, navigators are caring for patients and caregivers who are going through one of the most difficult journeys they will face in their lifetime. The emotional toll on an oncology navigator can be tremendous.
Compassion satisfaction refers to the pleasure a person feels from performing their work:
- It is characterized by people feeling invigorated by work they like to do
- They feel they can keep up with new technology and protocols
- They experience positive thoughts, feel successful, are satisfied with the work they do, want to continue to do it, and believe they can make a difference
Organizational leaders can also help optimize compassion satisfaction in the workplace by distributing tools, having vital conversations, promoting the importance of well-being, and incorporating resiliency skills training into the organization.
Compassion Satisfaction Tools
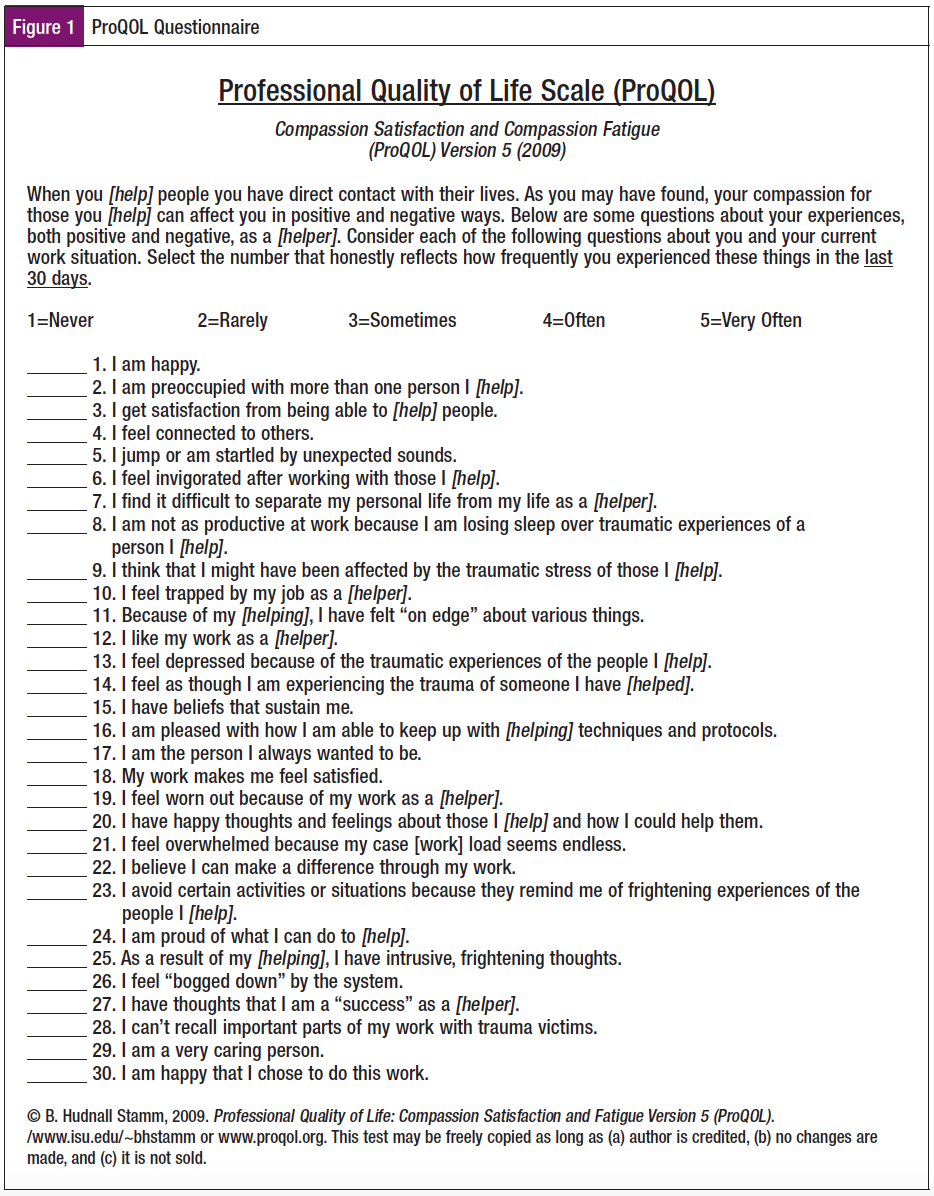
The Professional Quality of Life Scale (ProQOL) is an evidence-based system of measuring levels of compassion satisfaction, burnout, and secondary traumatic stress (Figure 1). The ProQOL is a 30-item self-report measure of the positive and negative aspects of caring. It reviews one’s work-related experiences over the past 30 days. The score enables an individual to assess if they are at risk for compassion fatigue episodes, as well as to compare results with average scores. Leaders can distribute this in a team meeting and promote discussing results together. Based on the outcome, managers can take the lead by scheduling a team event that promotes well-being. A yoga class, lessons in mindfulness, chair massages, and healthy cooking classes are just a few examples of team events that promote well-being.
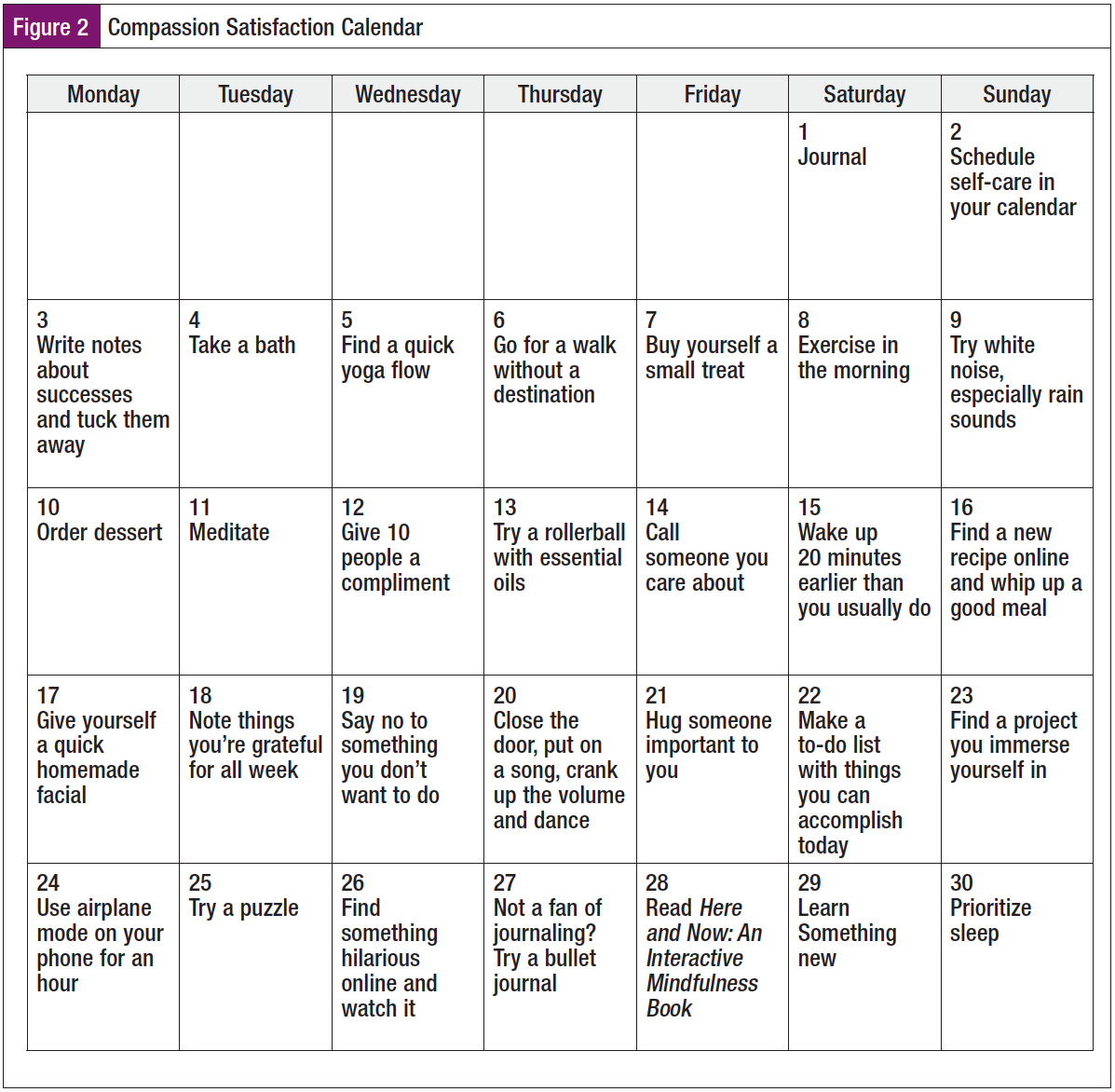
Leaders can also enable and promote compassion satisfaction by utilizing a calendar that outlines ways to prioritize one’s self (Figure 2). Encouraging the activity of journaling, coupled with the calendar, supports learning about and implementing self-care activities into the daily life of the navigators.
Navigators must be equipped with resources that can help reduce the risk of developing compassion fatigue. Navigators need to be encouraged to establish healthy boundaries, make self-care and self-compassion priorities, and practice self-reflection and mindfulness. The ability to reduce compassion fatigue is greater when leaders and navigators are aware of the symptoms and institute measures to prevent it.2
References
- Zhang YY, Han WL, Qin W, et al. Extent of compassion satisfaction, compassion fatigue and burnout in nursing: a meta-analysis. J Nurs Manag. 2018;26:810-819.
- Sheppard K. Compassion fatigue: Are you at risk? American Nurse Today. www.americannursetoday.com/compassion-fatigue.