Background: Cancer patients in Nigeria have reported psychological distresses, anxiety, and depression. These concerns stem from lack of information and social support and lead to poorer health outcomes and higher mortality. The impact of stigma against cancer patients has not been adequately explored in Nigeria. The community-driven patient navigation programs in Abia and Akwa Ibom states were established to guide patients through cancer screening to survivorship and address psychosocial issues while eliminating barriers to care.
Objective: This study explored self-reported psychosocial outcomes of cancer management and the pattern of stigma against cancer patients in both states.
Methods: This was a mixed-methods cross-sectional study of a sample of consenting cancer patients aged 18 years and older. The revised Edmonton Symptoms Assessment System was used to evaluate pain, anxiety, and depression. Perceptions of cancer stigma were also evaluated using a validated tool. Data analysis involved descriptive statistics, chi-square tests, Pearson correlation coefficient, and deductive thematic analysis.
Results: About 88% of the participants (N = 66) had been diagnosed with breast cancer. Most patients (56.06%, N = 66) reported moderate to severe anxiety, while 57.58% (N = 66) had moderate to severe depression. The proportion of patients with high stigma scores (ie, mean score ≥2.5) in each domain were cancer perception 25.76% (N = 66), stereotype perception 46.97% (N = 66), and discrimination experience 18.18% (N = 66). There was a moderate positive correlation (r = 0.403, P <.001) between the perception of cancer and anxiety. Qualitative themes regarding opportunities for improvement included “need for support,” “creating awareness,” and “hope.”
Conclusion: Psychosocial issues and stigma were common among cancer patients in the study. Stigma was correlated with anxiety and depression. There is a need to educate patients, their families, and the community about cancer stigma in the Abia and Akwa Ibom states.
Cancer patients in Nigeria and other places often deal with a myriad of psychosocial issues. More than 78% of cancer patients in Nigeria were reported to be psychologically distressed,1 about 37% reported moderate to severe anxiety, and 14% to 25% were diagnosed with depression.2,3 Common predictors of these psychosocial issues for cancer patients in Nigeria include lack of information regarding the disease spectrum, low income, pain, and social support.1-3 Psychosocial issues are linked to poorer patient outcomes in terms of quality of life and overall morbidity.4 Given the increasing prevalence of cancers in Nigeria,5 it is expected that the burden due to psychosocial issues will rise. Unfortunately, there is a dearth of adequately trained professionals who can attend to the diverse psychosocial needs of Nigerian cancer patients.6
Stigma, which is defined as a “social process, experienced or anticipated, characterized by exclusion, rejection, blame, or devaluation that results from experience, perception, and adverse social judgment regarding a person/group,” is a common experience for cancer patients.7 Although there have been no prevalence studies regarding stigma among Nigerian cancer patients, the effects of stigma and discrimination have been reported to include the concealment of cancer diagnosis and the fear of seeking early treatment. In the Nigerian society, it is common for a cancer diagnosis to be concealed from family members and social circles to avoid having a cancer patient labeled as a witch.6 There is widespread misconception about cancers in Nigeria, such as “cancers are not diseases to be treated in hospitals”; “witchcraft can be used to transmit cancers to people”; and that “people can get cancers from mystical sources.”8 The fear of stigma and associated stereotypes are associated with feelings of worthlessness and depression.9,10
A patient navigation program (PNP) is a systematic approach to guiding patients through the complexities of healthcare systems and removing the barriers to access to healthcare services.11 These programs are run by patient navigators who follow patients from screening, through treatment, and into survivorship.11,12 PNPs help ensure that patients get the most efficient care available locally, without increasing their financial burden. Evidence shows that PNPs improve patient outcomes, satisfaction, and quality of life.13,14 They also improve the quality of service provided by physicians.15 Although the importance of local PNPs has been reported,16,17 there have been no studies to examine their role in meeting the psychosocial needs of patients. The purpose of this study was to evaluate the psychosocial aspects of cancer care and perceptions of cancer stigma among patients receiving navigation services. Specifically, the study evaluated self-reported anxiety, depression, and perceptions of stigma among breast and cervical cancer patients using a PNP in the Abia and Akwa Ibom states in Nigeria.
Methods
This was a mixed-methods cross-sectional study of patients diagnosed with breast and cervical cancers participating in a patient navigation service in the Abia and Akwa Ibom states in Nigeria. It was a part of the larger clinical pathway implementation project.
Study Setting and Participants
Sixty-six patients participated in the study. The study population was drawn primarily from the Abia and Akwa Ibom states in Nigeria. Abia state is in southeastern Nigeria with an estimated population of 4 million spread across 17 local government areas (LGAs).18 Akwa Ibom state borders Abia state to the southeast and has an estimated population of 5.4 million people living in 31 LGAs.19 Both states have strong sociocultural and geographical connections.
Study participants included patients aged 18 years and older diagnosed with cancer before the end of 2020 and were receiving navigation services. New patients who were diagnosed through cancer screening activities that were coordinated by trained patient navigators in 2021 were also recruited into the study. This study was advertised at local hospitals and promoted on local social media, as well as with advertisement in churches and at community events, including patient support group meetings. Individuals interested in the study volunteered to participate. Patient navigators explained the study to potential participants and obtained consent. A sample of consecutive individuals who provided consent to the navigators were entered into the study.
Delivery of Patient Navigation and Support
Trained patient navigators (n = 4; 2 registered nurses and 2 community health workers) were recruited to manage the project. Their duties included:
- Identifying and connecting with local hospitals and clinics that managed cancer patients
- Working collaboratively with the hospitals to identify and recruit cancer patients
- Supporting patients through the care process
- Encouraging patients to join and participate in the cancer support groups
- Organizing monthly cancer support group meetings and addressing patients’ barriers to care
- Promoting early cancer detection in the community by working with community-based groups, churches, and health institutions to organize cancer screening events
Through these core tasks, the navigators were able to work with a diverse group of patients. As there was no existing patient navigation service for cancer patients in Abia state before the launch of this project, the navigators extended their services beyond cancers of primary interest to include other cancers (eg, ovarian and prostate cancer). They connected people who had suspicious cancer screening results with the relevant healthcare providers, such as surgeons and gynecologists. The navigators also performed periodic screening for barriers and psychosocial aspects of cancer care. Patients who presented with psychosocial issues were offered counseling by the navigators with support from trained counselors. Data from patient evaluation regarding psychosocial needs were entered into an online electronic medical record (EMR) system that was locally developed for patient navigation using OpenEMR technology.20 The EMR was customized to evaluate patient barriers to care using the framework developed by George Washington University’s PN-BOT program.21 The Edmonton Symptoms Assessment System22 was included in the EMR to record patients’ psychosocial outcomes.
Meanwhile, the navigators also organized monthly support group meetings in both states. Cancer patients who joined the support groups were encouraged to elect local executives, while the patient navigators served as coordinators. This led to the establishment of the Abia Cancer Support Group, based in Aba, and the Ibom Cancer Support Group, based in Uyo. The monthly meetings of these support groups were rotated among hospitals in the area to facilitate the involvement of patients who were hospitalized. Through the monthly support group meetings, counselors were able to identify mental health issues and to provide group counseling on anxiety and depression to the patients. The meetings were also used to provide education on practical strategies to cope with some of the symptoms of cancer and its treatment. The meetings were publicized using posters at hospitals and through posts on social media. Due to the challenges of hosting in-person events during the COVID-19 pandemic, Google Meet was used to hold online meetings. This attracted participants from outside the Abia and Akwa Ibom states. In addition to hosting monthly meetings, the support groups provided greeting cards to encourage patients who were undergoing cancer treatments at local hospitals.
Data Collection, Sample Size, and Analysis
Data were collected through an online questionnaire that included open-ended questions. Patients with limited Internet access participated in a phone interview conducted by volunteers. In addition to demographic information, data were collected to evaluate patient-reported outcomes, including pain, anxiety, and depression. These were based on the revised Edmonton Symptoms Assessment System (ESAS-r).22 The ESAS-r is a validated tool with 9 items that is used for symptom screening and longitudinal evaluation of patients in oncology, palliative care, and other disciplines irrespective of the care setting. Each of the 9 items were rated using a 10-point Likert-like scale.22 The ESAS-r scores were categorized into high symptom burden (ESAS-r ≥7), moderate burden (ESAS-r 4-6), and low symptom burden (ESAS-r 0-3).
The survey also evaluated perceptions of cancer stigma among the patients using a previously validated tool by Yılmaz et al.7 The tool was validated in a developing country like Nigeria. The stigma survey was divided into 3 domains—the impossibility of recovery, stereotypes, and discrimination experience. The impossibility of recovery domain related to the feelings that cancer was a death sentence and that the patient would most likely die of the disease, whereas the stereotypes domain alluded to how people in the community perceived cancer patients. Discriminatory experiences were those incidents that made patients feel that they were unfairly treated due to their cancer diagnosis. Survey responses by the patients were scored as follows: strongly disagree = 1, disagree = 2, agree = 3, and strongly agree = 4. Mean and total scores were calculated for each patient and each domain. Stigma scores ≥2.5 represent high stigma, and scores <2.5 represent low stigma.7 The patients were also requested to provide comments regarding the psychosocial outcomes, cancer stigma, or their perceptions regarding the care they received, using a 10-point Likert scale, with 10 being the worst rating. The scores were regrouped as great (1-3), fair (4-6), and poor (≥7). Due to the COVID-19 pandemic, this survey was largely completed online and through phone interviews administered by the patient navigators.
Quantitative data were abstracted from the patient navigation software to show the patient demographics, barriers encountered, psychosocial measures, and care/services provided. Surveys administered by an online interviewer were also used to evaluate perceptions of cancer stigma; issues about stigma were identified during the support group meetings. Qualitative data included interviews that were conducted with patients to understand the impact of the navigation program. Quantitative data were analyzed using descriptive statistics, chi-square, and t tests. Qualitative data were organized into codes that were developed a priori based on the themes that were structured to mirror the quantitative data. These codes were used to perform thematic analysis.
A minimum sample size of 74 patients was required to compare the prevalence of high stigma score (≥2.5) that was reported in Iran10 with the scenario in Nigeria, with a precision of 0.1 at 95% confidence level. The quantitative sample size was calculated using the formula: [n = (Z2 × P × (1 - P))/e2]. Where:
– Z = value from standard normal distribution corresponding to desired confidence level (Z = 1.96 for 95% CI)
– P is expected true proportion
– e is desired precision (half desired CI width)
P value <.05 was considered to be significant. Qualitative data were collected from all participants while the survey was administered.
Ethical Consideration
Ethics approval was obtained from the Abia State Ministry of Health Human Research Ethics Committee (AB/MH/AD/904/T.190). The privacy of participants was ensured as data were stored in a secure, electronic cabinet provided by the University of Saskatchewan. Only participants who provided informed consent were recruited into the data. Their identity was masked using alternate identifiers (for qualitative data) and the use of aggregate data for reporting quantitative data. Participants were informed of their right to withdraw from the study at any point without consequences until all the data were aggregated and deidentified for analysis.
Results
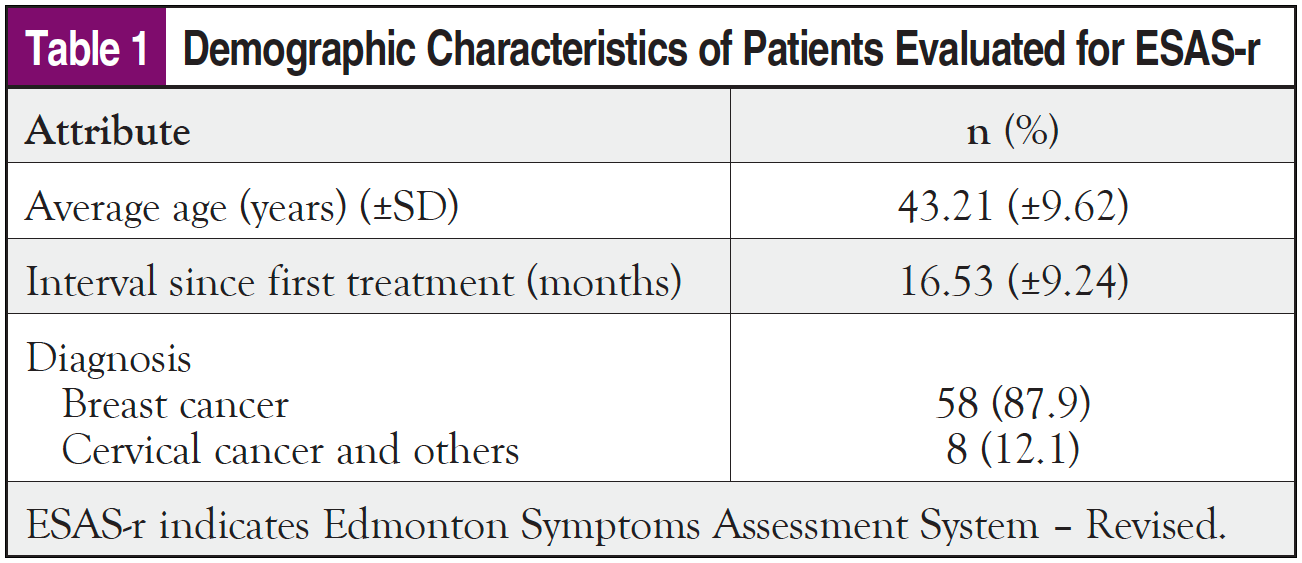
A total of 66 consenting patients completed the survey, with an average age of 43.21 (±9.62) years. Most of the patients (87.9%, N = 66) had been managed for breast cancer. Table 1 shows the demographic characteristics of the patients.
The Pattern of Patient-Reported Psychosocial Symptoms
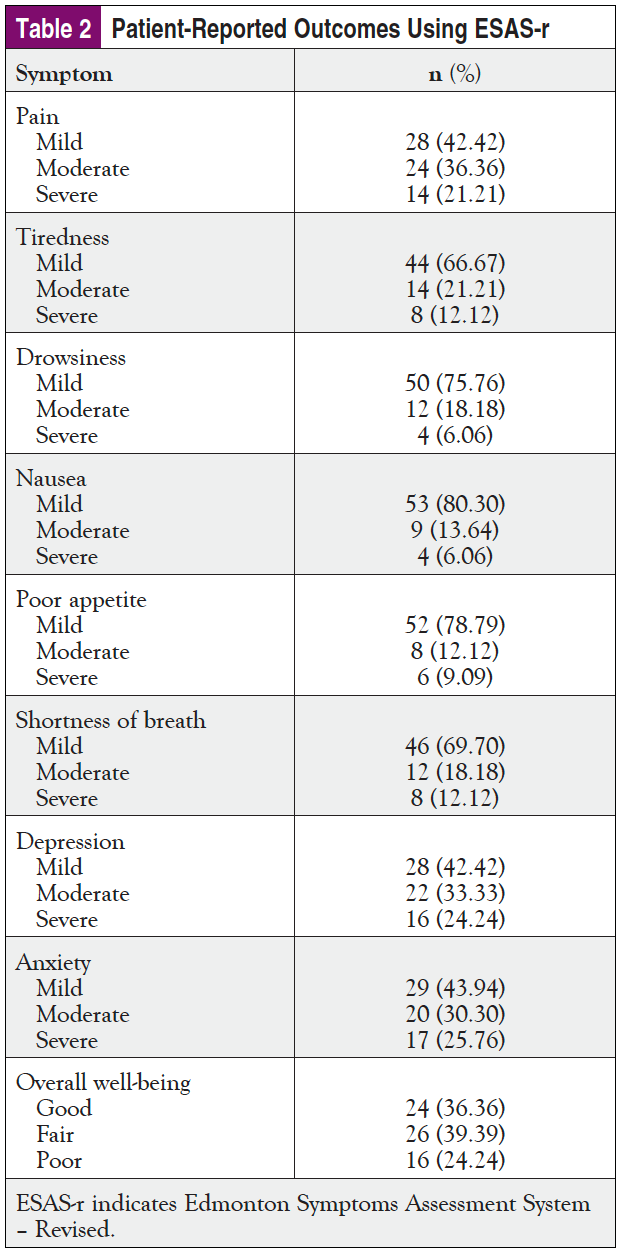
The ESAS-r scores were categorized into high symptom burden (ESAS-r ≥7), moderate burden (ESAS-r 4-6), and low symptom burden (ESAS-r 0-3), as previously described. Table 2 shows the distribution of the patient-reported symptoms.
Perceptions of Cancer Stigma
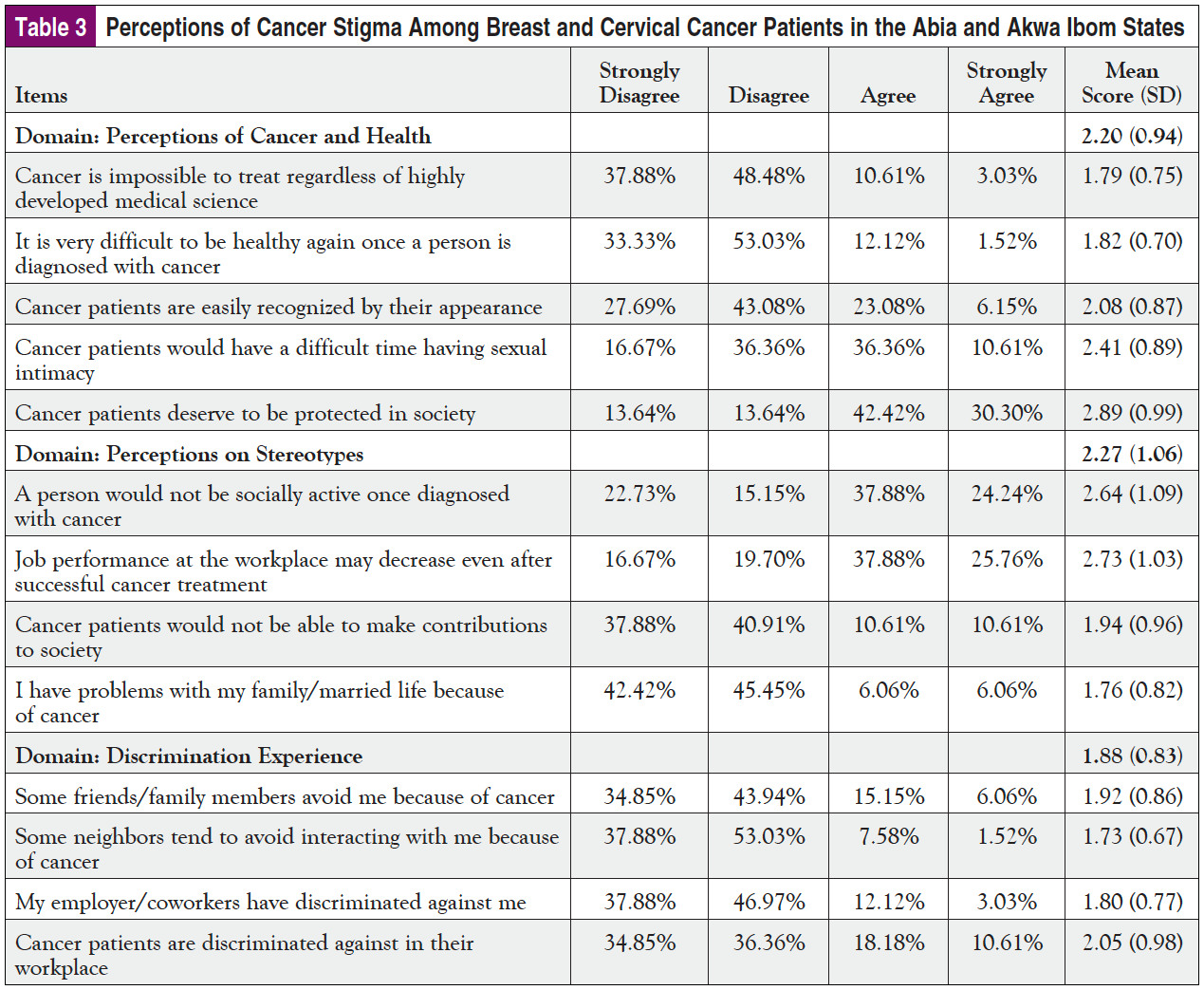
Issues with high stigma scores (ie, mean scores ≥2.5) included protection of cancer patients (2.89 ± 0.99), social activity for cancer patients (2.64 ± 1.09), and posttreatment job performance (2.73 ± 1.03). Table 3 shows the results of the stigma scores by domain.
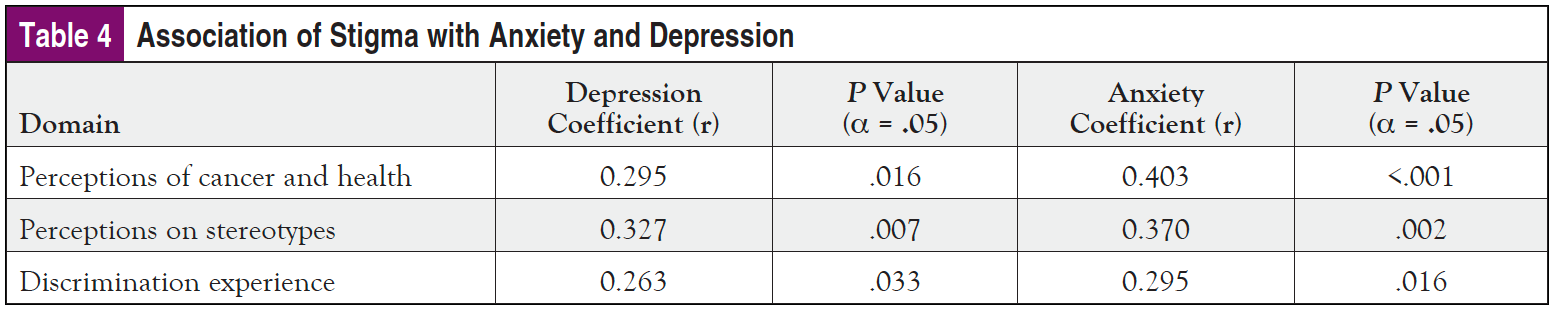
The proportion of patients with high stigma scores (ie, mean score ≥2.5) in each domain was cancer perception, 25.76% (N = 66); stereotype perception, 46.97% (N = 66); and discrimination experience, 18.18%. Further analysis was conducted to examine the strength of association (Pearson correlation coefficient) between the mean scores in each of the domains with the patient-reported anxiety and depression based on ESAS-r scores (Table 4).
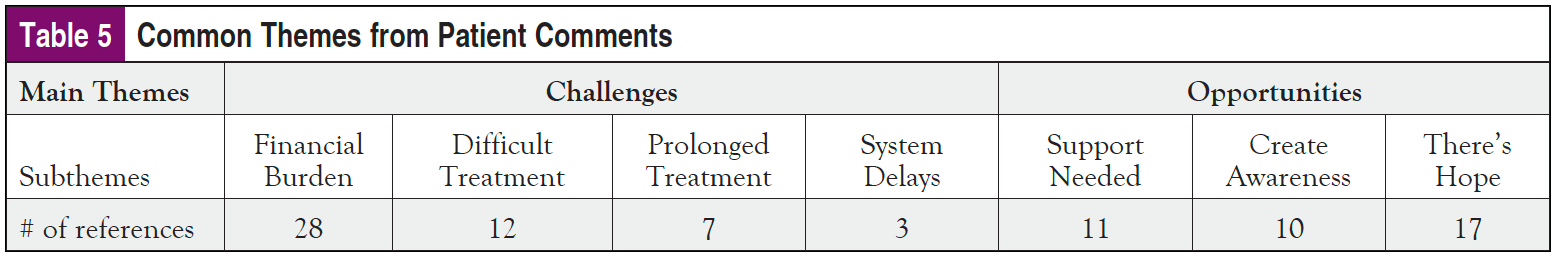
Inductive thematic analysis was used to explore the comments made by the patients regarding cancer treatment and stigma. The emergent themes were broadly categorized into challenges (depicting negative experiences) and opportunities (representing positive experiences/expectations), with the following subthemes, as shown in Table 5.
The following comments illustrate each of the themes and subtheme.
Main Theme: Challenges
This theme described the challenges that patients experienced while undergoing treatment and accessing the navigation service. The subthemes reflected the financial burden that patients faced while undergoing treatment (financial burden), the physiological and psychological difficulties associated with treatment (difficult treatment), and the delays within the health system that affect cancer care (system delays).
Subtheme: Financial burden—“Treatment is expensive, and it takes time due to lack of finance.”
Subtheme: Difficult treatment—“I have seen that the treatment is not so easy but possible.”
Subtheme: Prolonged treatment—“It takes time and money to cure it.”
Subtheme: System delays—“I am on treatment, but strike is not helping us.”
Main Theme: Opportunities
The main theme “opportunities” showed comments that spoke to methods of coping used by patients and strategies for improving cancer care generally. The subtheme “need for support” talked about the value of the support group, while “hope” spoke to the feeling that the next day would be better. The “need for awareness” reflected participants’ expectations on how to improve their care experience.
Subtheme: Need for support—“I was hard on myself at the initial stage. The support group has been of great help in this regard.”
Subtheme: Need for awareness—“[Create] more awareness of stigma and to support patients.”
Subtheme: Hope—“God is in control.”
Patient Suggestions on Improving Cancer Stigma
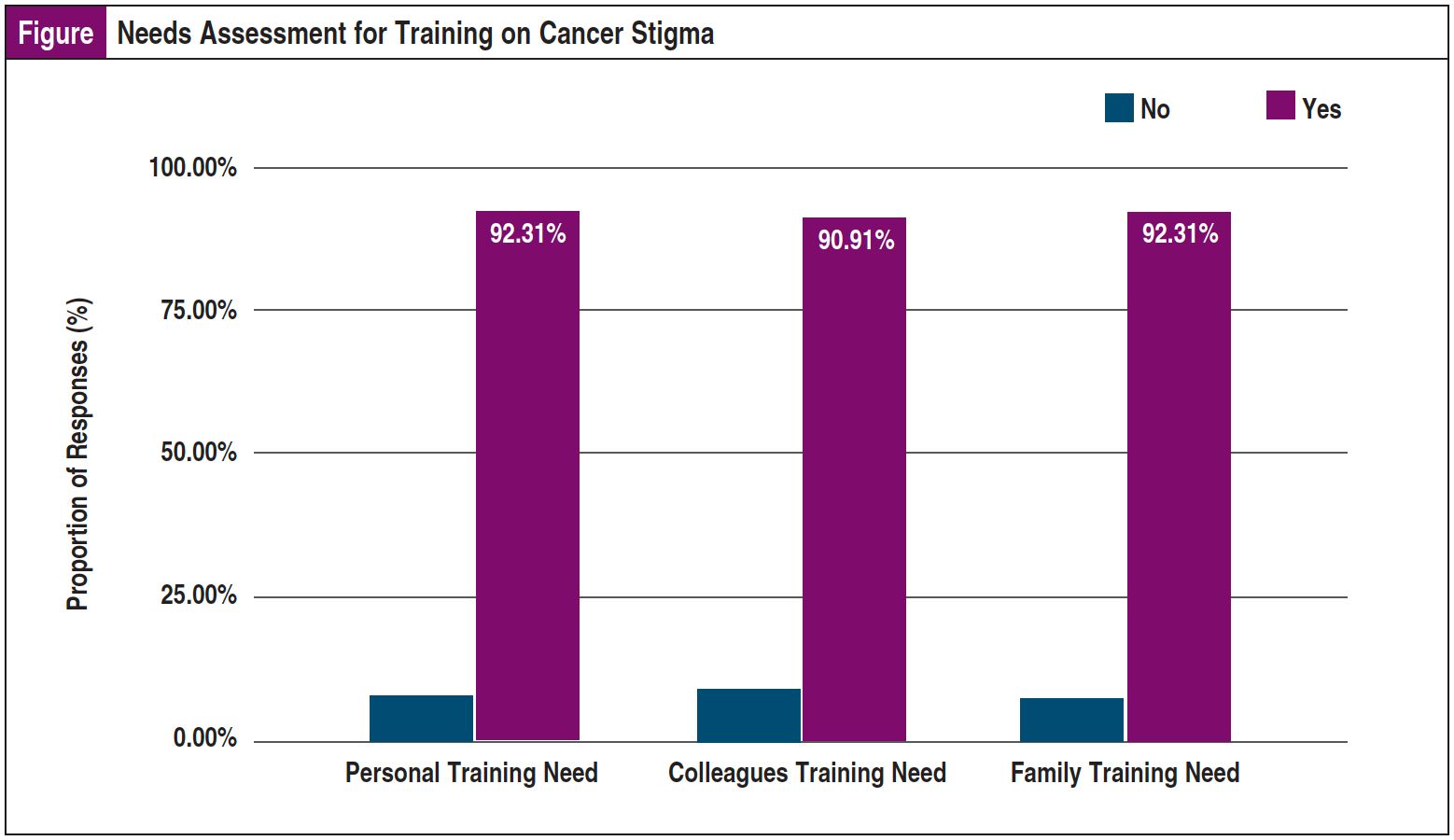
Patients were requested to express their interest in further training and services regarding cancer stigma. More than 90% of respondents indicated an interest in having themselves, colleagues at work, and family members trained on cancer stigma (Figure).
Discussion
This project was initiated to strengthen the community-driven approach to strengthening cancer control services in Abia state and environs. It built on previous interventions that improved the clinicians’ competence in early cancer detection, diagnosis, treatment, and the development of clinical pathways.23,24 The average age of patients in this study (43.21 years ±9.62) was comparable to those reported in similar studies.2-4
Although 36% (N = 66) of the patients assessed their health to be “great,” at least 55% reported having moderate to severe pain (Table 2). This finding could reflect a gap in the management of cancer pain in the study setting. Previous research had also highlighted the need for improving the competence of clinicians in the management of cancer pain and other symptoms.25,26 It will be important to further train the clinicians in pain management for cancer patients. Almost 60% of the patients (N = 66) had moderate to severe anxiety or depression. This is higher than the prevalence of moderate to severe anxiety (37%) and moderate to severe depression (14%-25%) that was reported in the literature.2,3 The higher prevalence of anxiety and depression in this study might be due to the use of a different grading system, as the previous studies used Beck’s Depression Inventory,2 whereas this study used the ESAS-r.22 Regardless of the scoring system, this study highlights the need to provide more mental health support to cancer patients in Nigeria.6 Qualitative data showed that financial challenges and poor perceptions of cancer might be among the stressors. These findings have also been reported in other jurisdictions.27,28 It will be necessary to explore ways to mobilize local support to fund cancer services in the area.
Furthermore, this study found that the proportion of patients with high stigma scores (ie, mean score ≥2.5) was mostly in the stereotype perception domain, 46.97% (N = 66), followed by the cancer perception domain (25.76%, N = 66). This pattern of high stigma score was lower than what was reported in Iran.10 Although no previous Nigerian studies have used this approach to analyze cancer stigma, the effects of stigma and discrimination have been reported to include the concealment of cancer diagnosis and the fear of seeking early treatment. The fear of stigma and associated stereotypes have been associated with feelings of worthlessness and depression.9,10 In Nigerian society, it is common for a cancer diagnosis to be concealed from family members and social circles to avoid having a cancer patient labeled as a witch.6 As shown in the Figure, there is a need to develop educational interventions for patients and their families regarding cancer stigma.
The generalizability of this study is limited by the fact that the sample size (N = 66) was less than the 74 patients required to compare the prevalence of a high stigma score (≥2.5) with what was reported in Iran.10 The findings could be different if more patients were recruited, especially those who did not receive navigation service. Although 55% (N = 66) of patients reported having poor pain management, this finding is limited as the study did not evaluate the clinical pain management of each patient (eg, adequacy of pain control). Also, because the sample was recruited from patients who were already receiving navigation services, the findings regarding psychosocial symptoms (eg, anxiety and depression) may be different from what might be reported by patients who did not use such a service.
Conclusion
This study showed that psychosocial issues and stigma were prevalent among cancer patients in the Abia and Akwa Ibom states of Nigeria. Perceptions of stigma were significantly related to anxiety and depression. It will be important to create a training program for patients and their families regarding cancer stigma and ways to handle it. Such training would potentially reduce the perceptions of stigma while equipping patients with coping skills.
Funding Acknowledgment
This research project was funded by Pfizer Inc. The funders did not have any role in the design or execution of the project. The authors declare no conflict of interest.
References
- Ojewole FO, Madu AM, Nwozichi CU. Association between psychological distress and unmet information needs among female cancer patients in two selected teaching hospitals in South-West Nigeria. CHRISMED J Health Res. 2018;5(1):11-17.
- Asuzu C, Adenipekun A. Correlates of depression and anxiety among the cancer patients in the radiotherapy clinic in Uch, Ibadan, Nigeria. African Journal for the Psychological Study of Social Issues. 2015;18(2):10-13.
- Lebimoyo A, Ola B, Adewuya A, et al. Mental health and quality of life among patients with gynaecological cancers in Lagos, Nigeria. Malaysian Journal of Psychiatry. 2020;29(2):1-17.
- Fatiregun OA, Olagunju AT, Erinfolami AR, et al. Relationship between anxiety disorders and domains of health related quality of life among Nigerians with breast cancer. Breast. 2017;31:150-156.
- Jedy-Agba E, McCormack V, Adebamowo C, Dos-Santos-Silva I. Stage at diagnosis of breast cancer in sub-Saharan Africa: a systematic review and meta-analysis. Lancet Glob Health. 2016;4:e923-e935.
- Agha AA, Onalu C, Chidebe R. Bridging the gap: investigating the role of social workers in supporting metastatic breast cancer patients in Nigeria. Soc Work Public Health. 2021;37:244-257.
- Yılmaz M, Dişsiz G, Demir F, et al. Reliability and validity study of a tool to measure cancer stigma: patient version. Asia Pac J Oncol Nurs. 2017;4:155-161.
- Sarki AM, Roni BL. This disease is “not for hospital”: myths and misconceptions about cancers in Northern Nigeria. Journal of Global Health Reports. www.joghr.org/article/12012-this-disease-is-not-for-hospital-myths-and-mis conceptions-about-cancers-in-northern-nigeria. 2019.
- Nwozichi CU, Musah KT, Madu AM, et al. Contextualizing the cultural factors associated with cancer care in Nigeria: an ethnonursing study. J Transcult Nurs. 2021;32:382-388.
- Shiri FH, Mohtashami J, Nasiri M, et al. Stigma and related factors in Iranian people with cancer. Asian Pac J Cancer Prev. 2018;19:2285-2290.
- Weber J, Mascarenhas D, Bellin L, et al. Patient navigation and the quality of breast cancer care: an analysis of the breast cancer care quality indicators. Ann Surg Oncol. 2012;19:3251-3256.
- Okon K, Eguzo K, Ekanem U, Udo I. Impact of an innovative patient navigation project in Nigeria: preliminary results. Journal of Global Oncology. 2018;4(2):113s.
- Pittathankal A, Davidson T. Care pathways for patients with breast cancer. Trends in Urology, Gynaecology & Sexual Health. 2010;15(2):10-13.
- Zon R, Frame JN, Neuss MN, et al. American Society of Clinical Oncology Policy Statement on Clinical Pathways in Oncology. J Oncol Pract. 2016;12:261-266.
- Cui Q, Tian J, Song X, et al. Effectiveness of clinical pathway in breast cancer patients: a meta-analysis. Global Journal of Oncologists. www.savvyscien cepublisher.com/downloads/gjov2n1a3/. 2014.
- Eguzo K, Kremzier M, Nnah K, et al. Expanding the role of Nigerian primary care providers in cancer control through continuing education: findings from government-led collaborative intervention. Journal of Clinical Research in Oncology. 2018;1(2):1-6.
- Eguzo KN, Ekanem US, Chukwuemeka O, et al. Using multiple perspectives analysis to propose state cancer control policy in Abia State, Nigeria. J Clin Oncol. 2020;38(suppl):e14132.
- Governor’s Office. The Official Website of Abia State Government. God’s Own State. Abia State Government. https://abiastate.gov.ng/.
- Akwa Ibom State Government. Ministry of Information and Strategy. About Akwa Ibom. https://akwaibomstate.gov.ng/about-akwa-ibom/.
- Eguzo K, Lawal A, Oluoha C, et al. Clinical pathway and patient navigation: research protocol on the appropriateness, timeliness and support of women diagnosed with breast cancer in Abia state. Asian Pacific Journal of Cancer Care. 2021;6(3):367-371.
- The George Washington University Cancer Center. Patient Navigation Barriers and Outcomes Tool (PN-BOT). Version 1.1 Quick Start Guide. http://bit.ly/AboutPNBOT. 2016.
- Hui D, Bruera E. The Edmonton Symptom Assessment System 25 years later: past, present, and future developments. J Pain Symptom Manage. 2017;53:630-643.
- Eguzo KN, Ismaila N, Akpanudo U, et al. Using blended learning to improve education on clinical pathways for breast cancer management in Nigeria: preliminary results. J Clin Oncol. 2019;37(suppl):10539.
- Eguzo K, Ismaila N, Oluoha C, et al. Using blended-learning approach to improve education on clinical pathways for breast cancer management in Nigeria: a research protocol. J Clin Res Oncol. 2018;1:1-5.
- Olakulehin OA, Akanbi OO, Adeoti ML, et al. A cross sectional study of newly qualified doctors’ knowledge on pain management in South Western Nigeria. Journal of Advances in Medicine and Medical Research. 2017;21(10):1-10.
- Nwogu C, Mahoney M, George S, et al. Promoting cancer control training in resource limited environments: Lagos, Nigeria. J Cancer Educ. 2013;29:14-18.
- Chan RJ, Gordon LG, Tan CJ, et al. Relationships between financial toxicity and symptom burden in cancer survivors: a systematic review. J Pain Symptom Manage. 2019;57:646-660.
- Ver Hoeve ES, Ali-Akbarian L, Price SN, et al. Patient-reported financial toxicity, quality of life, and health behaviors in insured US cancer survivors. Support Care Cancer. 2021;29:349-358.