Kathleen Sweeney, DNP, RN, ACNS-BC, AOCNS, NE-BC
Director, Cancer Center Hematology & Transplant Services
Froedtert & the Medical College of Wisconsin Cancer Center
Milwaukee, WI
Darlene A. Showalter, DNP, RN, CNS
DNP Program Coordinator & Clinical Associate Professor
The University of Alabama in Huntsville, AL
Background: Cancer mortality and incidence in the United States has decreased each year from 1991 through 2017. The decline is credited to increased cancer prevention efforts, increased cancer screening, early detection of cancers, and higher-quality treatments. Although cancer diagnoses and deaths have been declining in the United States, COVID-19 has impacted cancer screening rates, and the concern is this will lead to increases in late-stage diagnoses and increases in cancer mortality.
Population and Setting: The project took place at a Federally Qualified Health Center located in a primarily African American neighborhood in a large Midwestern city. The target population consisted of women aged 40 to 69 years who qualified for mammography screening and received care at the clinic.
Objectives/Project Design: This was a quality improvement project aimed at increasing the number of women scheduling and receiving mammograms after implementing a lay navigation program in person and via phone.
Methods: Each woman who qualified received scripted navigation services, including education, written materials, and help to overcome barriers to screening mammography.
Results: One hundred fifty-eight women received education on mammography. Of those, 128 went on to receive additional navigation, including written education and help overcoming barriers so they could receive screening. Forty-three women who met with the navigator received screening mammography.
Conclusion and Implications: There were multiple clinically significant pieces of this project, including the number of women who did receive mammograms, the number of women who received education about mammography, the number of women who had never received a mammogram in the past, and the number of uninsured women who received information on how to get a mammography screening with no out-of-pocket cost. Navigation can decrease barriers for women and increase the number of women who get screening mammography. Navigators have the potential to draw women back to routine mammography screening after the recent COVID-19 pandemic.
Cancer mortality in the United States has decreased each year from 1991 through 2017, which means there have been 2.9 million fewer deaths from cancer during those years.1 Overall cancer incidence has decreased each year since 1991.2,3 The decline in both cancer-related death and incidence of cancer is credited to increased cancer prevention efforts, increased cancer screening, early detection of cancers, and better quality treatments. Although mortality is decreasing, cancer is still the second-highest cause of death in the United States.4 Siegel et al estimated there would be 1,918,030 new cancer diagnoses and 609,360 cancer deaths in 2022.5
Along with lung and colorectal cancer, breast cancer is 1 of the 3 most common cancers in the United States affecting women.1 These 3 cancers account for 50% of all new cancer diagnoses in women. Breast cancer alone accounts for 30% of all female cancers,1 as it is the most common cancer among women,6 and it is the second leading cancer cause of death in women after lung cancer.1,6 Siegel et al estimated that in 2022 there would be 290,560 breast cancer diagnoses and 43,780 deaths.5
In the United States, mammography screening has been shown to decrease mortality from breast cancer by 40% if women begin screening at age 40.7 While mortality can be decreased by screening, less than half of eligible women receive a yearly mammogram. Although cancer diagnoses and deaths have been declining over the past 2 decades, there are significant racial and ethnic disparities in cancer screening rates,8 cancer incidence, and cancer mortality.3,9 Barriers to cancer screening among minority women include competing priorities, loss of privacy, lack of knowledge about cancer screening, perceived good health, fear of pain, fear of a cancer diagnosis, family discouragement to screen, lack of physician recommendation, awareness of someone who was hurt by cancer screening, cost, lack of transportation, and language barriers.10 In 2018, it was reported that for women aged 50 to 74 years, only 71.7% had a recent mammogram.11 Factors that decreased the likelihood of women receiving a mammogram include age range of 50 to 64 years, income less than 139% of the federal poverty level, no primary care provider, lack of insurance, government insurance, non-Hispanic Asian race and ethnicity, women without a recent physician visit, lower education levels, younger age, and those without an obstetrics and gynecology provider.11
Cancer disparities have been further affected by COVID-19. Since the pandemic began in 2020, studies have begun to show that women living in high poverty areas are less likely to receive a mammogram screening.12 The COVID-19 pandemic has increased preexisting fears and mistrust among the African American population toward the government and healthcare institutions. This mistrust is due to historical experiences like the Tuskegee Syphilis Study. COVID-19 has created additional barriers to screening, including issues with work schedules, lack of reliable childcare,13 financial concerns, fear to seek care,13,14 transportation challenges,13-15 difficulty accessing screening care, loss of insurance, and increased anxiety.15 COVID-19 has emerged as a new barrier to cancer screening particularly among underserved and minority populations.13 Young women living in poverty, without health insurance, those who needed an interpreter or had a long distance to travel were least likely to receive screening. All of this has led to increased delays in cancer diagnosis and treatment, which may lead to a short-term decrease in cancer incidence and then an increase in advanced cancers and mortality in the future.4 COVID-19 is expected to impact the number of new cancer diagnoses and deaths over the next few years, possibly impacting disadvantaged populations hardest.
COVID-19 has greatly impacted the number of people receiving cancer screenings. During 2020, the screening deficit was 9.4 million people for all cancers.16 Mammography screening rates fell similarly by 89% to 90% from 2019 to 2020.16,17 This decrease means that worldwide there were 3.9 million women who were not screened for breast cancer during 2020.16 A modeling study from the United Kingdom estimates that this decrease in screening will increase deaths from breast cancer by 7.9% to 9.6%.18 There are little to no data available evaluating how to get women back into mammography screening after COVID-19.
How can this trend be reversed so women are encouraged to have routine mammogram screening again? Navigation might be an option. In a 16-week project, a lay navigator was embedded into a Federally Qualified Healthcare Center (FQHC) in a Midwestern city with the goal of educating women about breast cancer, breast health, and mammography, as well as navigating eligible women to get mammogram screening. A lay navigator is a trusted nonclinical member of the healthcare team who assists patients, families, and caregivers to overcome barriers in the healthcare system and access available resources.
Conceptual Framework
The conceptual framework used for this project was the Health Belief Model (HBM) (Appendix). Developed in the 1950s by the US Public Health Service, the HBM has been utilized to explain and forecast the of use preventive health services, including screenings and immunizations.19 The HBM has 6 main concepts: perceived susceptibility, perceived seriousness, perceived benefits, perceived barriers, cues to action, and self-efficacy.19 The HBM has the greatest success when it is applied to prevention programs like cancer screening.20 The concept behind the model is that there are factors that may change the likelihood of someone participating in health promotion activities like screening mammography. The concepts that predict participation in health promotion activities vary in intensity for each person.19

Health Belief Model and Mammography Screening
The HBM has been widely used in studies assessing breast cancer screening. The elements of the HBM can be associated with the health action and breast cancer screening in both positive and negative ways.21 Susceptibility to breast cancer, breast cancer severity, and the benefit of screening are positively related to obtaining mammography, while any barrier a woman faces is negatively related to the woman receiving screening. Benefits must outweigh the barriers for a woman to engage in breast cancer screening. The goal of navigation, in this instance, was to decrease the barriers to mammography so the benefits would outweigh them and women would schedule and receive screening.
The goal of the program was to increase the number of underserved women scheduling and receiving mammography screening. The navigator’s role included educating women about breast cancer and the myths surrounding breast cancer and mammography, making women aware of specific cancer risks based on their racial and ethnic backgrounds, and discussing how to employ independence concerning their health. These navigation offerings focused on each woman’s perceptions of breast cancer and her feelings about the magnitude of breast cancer. The navigator had resources available to help women overcome barriers that kept them from receiving mammography, including help with scheduling appointments, following up via phone if they missed an appointment, arranging transportation, sharing how mammograms feel to decrease fears, and access to multiple resources that provide funding and/or insurance coverage for breast cancer screening. Based on the education and navigation services that were offered and provided, women should have had an increased understanding of their susceptibility to breast cancer, increased perception of the benefits of mammography screening, and a decreased perception of barriers to receive a mammogram. The navigator also provided cues to help encourage women to schedule and complete mammography screening. These cues included a recommendation for a mammogram, verbal education, written education materials, and help to schedule their appointment if desired. The goal was that these services would help increase the number of underserved women receiving mammography screening.
Design
In this administrative quality improvement project, a navigation intervention was implemented at an FQHC to take place over 16 weeks. The project consisted of in-person and phone navigation interactions to increase the number of underserved women who schedule and receive screening mammography. The navigator was available at the FQHC on Monday, Wednesday, and Friday, when mammography services were available. The navigator tried to engage all women either immediately before or after their appointments. Staff and providers at the FQHC also referred women to the navigator, and women self-referred for navigation services.
Exclusion criteria included women who spoke English as a second language, women with a history of breast cancer, or women who had mammogram screening in the past year. Data were collected in aggregate as well as individually. The navigator followed a navigation script or algorithm so each woman received the same information. Initially, each woman received mammography and breast cancer education. Next, as part of the script, the navigator assessed what barriers women were experiencing that keep them from receiving mammogram screening. These barriers were tracked in aggregate and individually. Based on the barriers that were identified for each woman, the navigator developed an individualized plan to help decrease their barrier(s) to mammogram screening. The navigation services offered included a connection to insurance or copay assistance, education, support at mammogram appointment, transportation resources, childcare resources, assistance scheduling, reminder calls, follow-up phone calls, introduction to mammography staff, help establishing with a primary care provider, discussion of fears, and connection to social work services. The number and type of navigation services provided to each woman was documented. Each encounter consisted of 1 or multiple services.
Multiple studies have shown that navigation needs to be tailored to the cultural needs of the community.22,23 Navigation services must be culturally relevant,24 and if possible the navigator should be from a diverse background and live in the community.23 The person who was trained as a navigator and placed at the FQHC was an African American female who lived within the city. She has multiple family members who had been diagnosed with breast cancer, and she works within the community. The navigator received training on navigation, breast cancer, ways to help women overcome barriers, and use of the project materials. The navigator was integrated into the FQHC before navigation began through education sessions for staff and providers about cancer disparities, navigation, and the navigation project. The goal was that the clinic staff would get to know her and trust her so they would refer patients to navigation.
Lack of knowledge about breast cancer and breast cancer screening using mammography is widespread in underserved communities.24 To overcome this, education was an integral part of the navigation intervention. The navigator, although not a medical professional, has a degree in community education and over 9 years of experience delivering cancer education and outreach to underserved areas in the city. Using 1 navigator, rather than various navigators, ensured women received consistent messaging and services during the project.
Cost is one of the most frequently mentioned barriers that keeps women from receiving screening mammography.23,25 The navigator had multiple ways to decrease costs for women, including access to financial navigators available through the FQHC by referral. Financial support to fund mammograms was procured from the Susan G. Komen Foundation, Well Woman Medicaid, and as a last resort, use of the sliding scale fee at the FQHC. These options were implemented to help buffer the barrier of prohibitive cost.
Evidence-Based Procedure
The navigator was trained using the online George Washington Cancer Institute Oncology Patient Navigator Training: The Fundamentals.26 Upon completion of the training, the navigator then started working at the FQHC. Each woman accepting navigation received scripted interventions. These interventions included education, assessment of barriers, individualized interventions based on identified barriers, navigation to mammography screening, and follow-up calls.
Data Collection
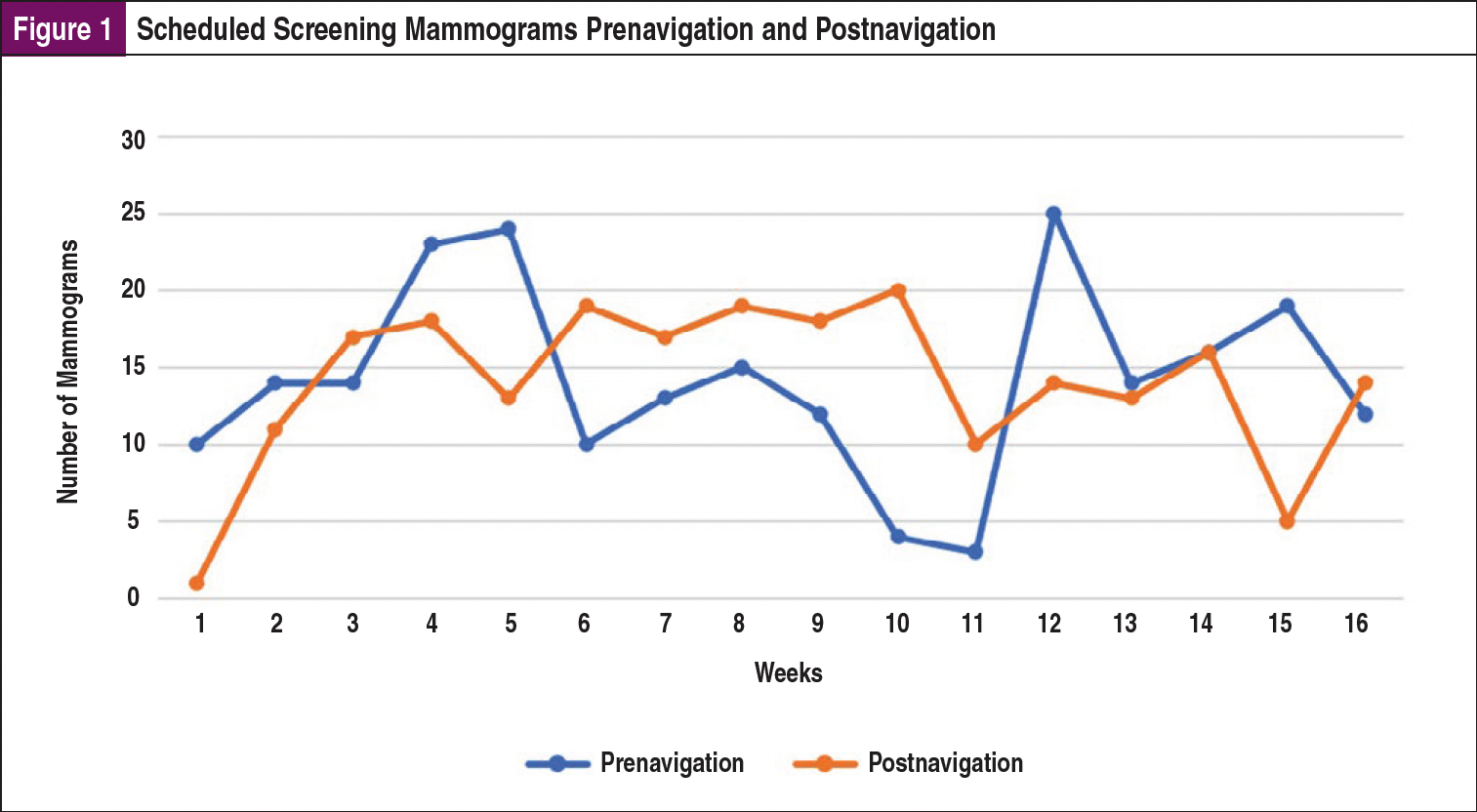
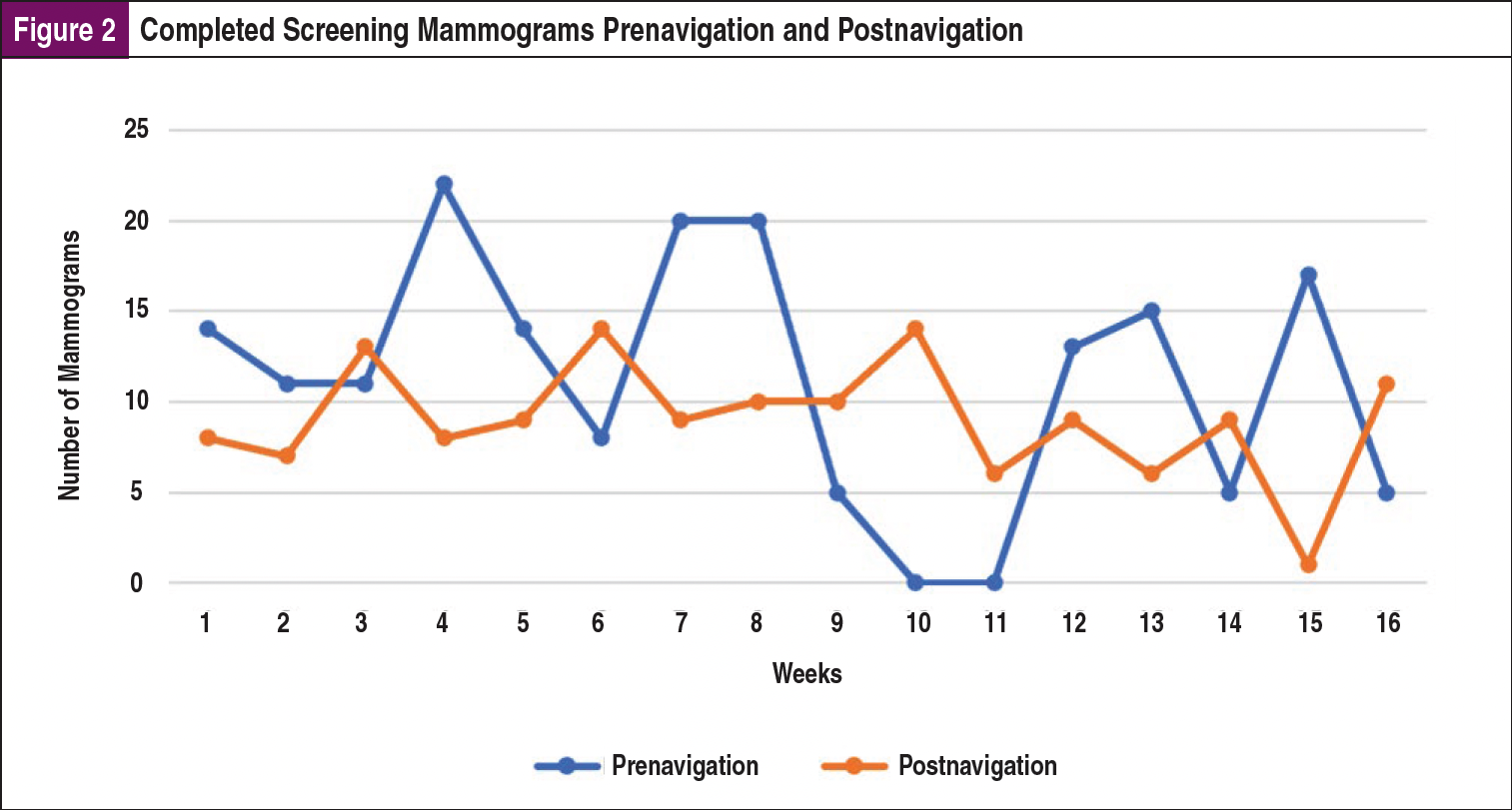
The principal outcome measures for this project were the number of women scheduling screening mammography and the number receiving mammography after navigation was implemented. Once the navigator was in place, data were collected and compared with a comparable period prenavigation to show the difference between the 2 time periods (Figure 1 and Figure 2). The project ran for 16 weeks beginning in February 2021.
Demographics
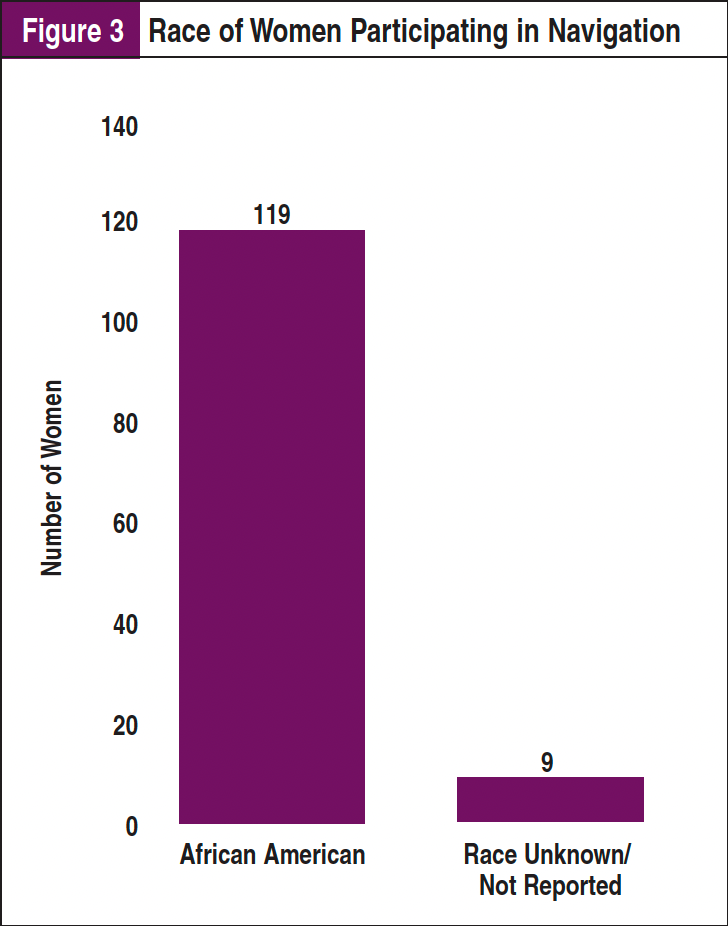
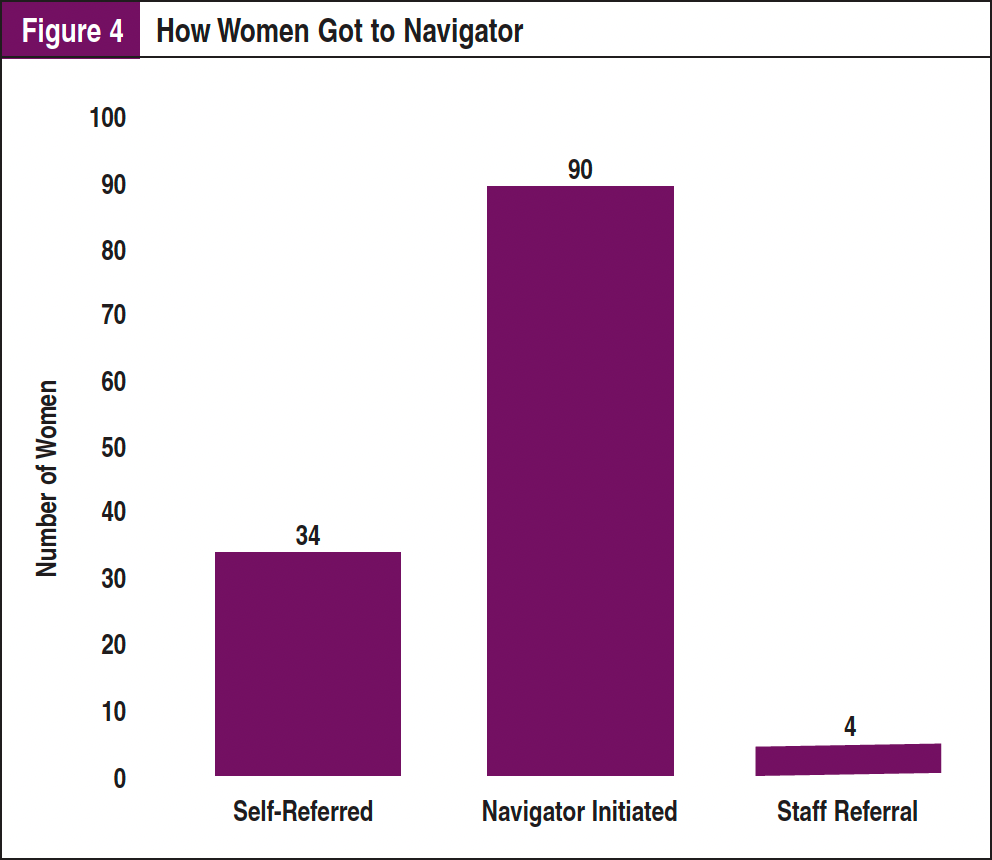
Throughout the 16 weeks of navigation, the navigator was on-site 43 days, which constituted 271 hours. During this time, 160 women were approached for navigation, and 158 agreed to participate. Of those, 128 qualified to participate in the program. Of those who did not qualify, 1 spoke English as a second language, 16 had a history of breast cancer, and 13 had a mammogram screening within the past year. Eight women who did not know if they had a screening mammogram in the past year were included in the project. Of the 128 women who participated, 119 (93%) were African American, and the remaining 9 (7%) chose not to state their race (Figure 3). Ninety (70%) of the women were approached by the navigator to participate, 34 approached the navigator, and 4 were referred by staff of the clinic (Figure 4). Eighty-three women (65%) had insurance, 20 (16%) were uninsured, and 25 (20%) were unaware if they had insurance (Figure 5).

Barriers
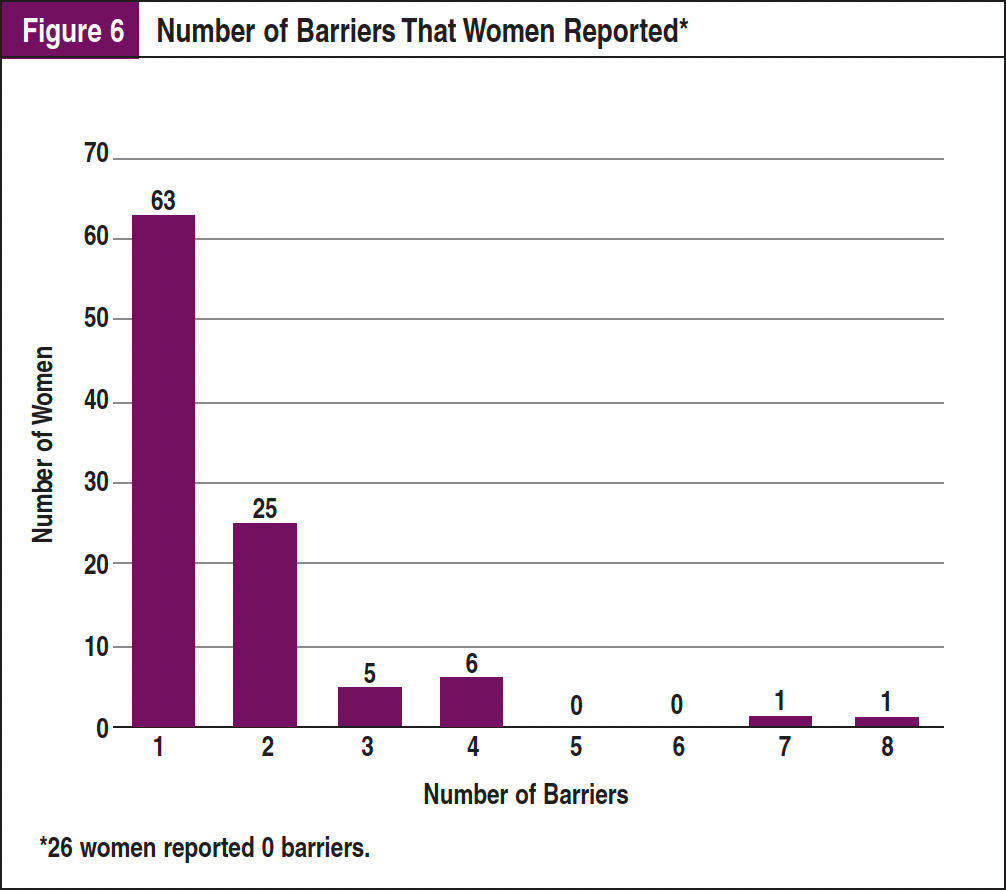
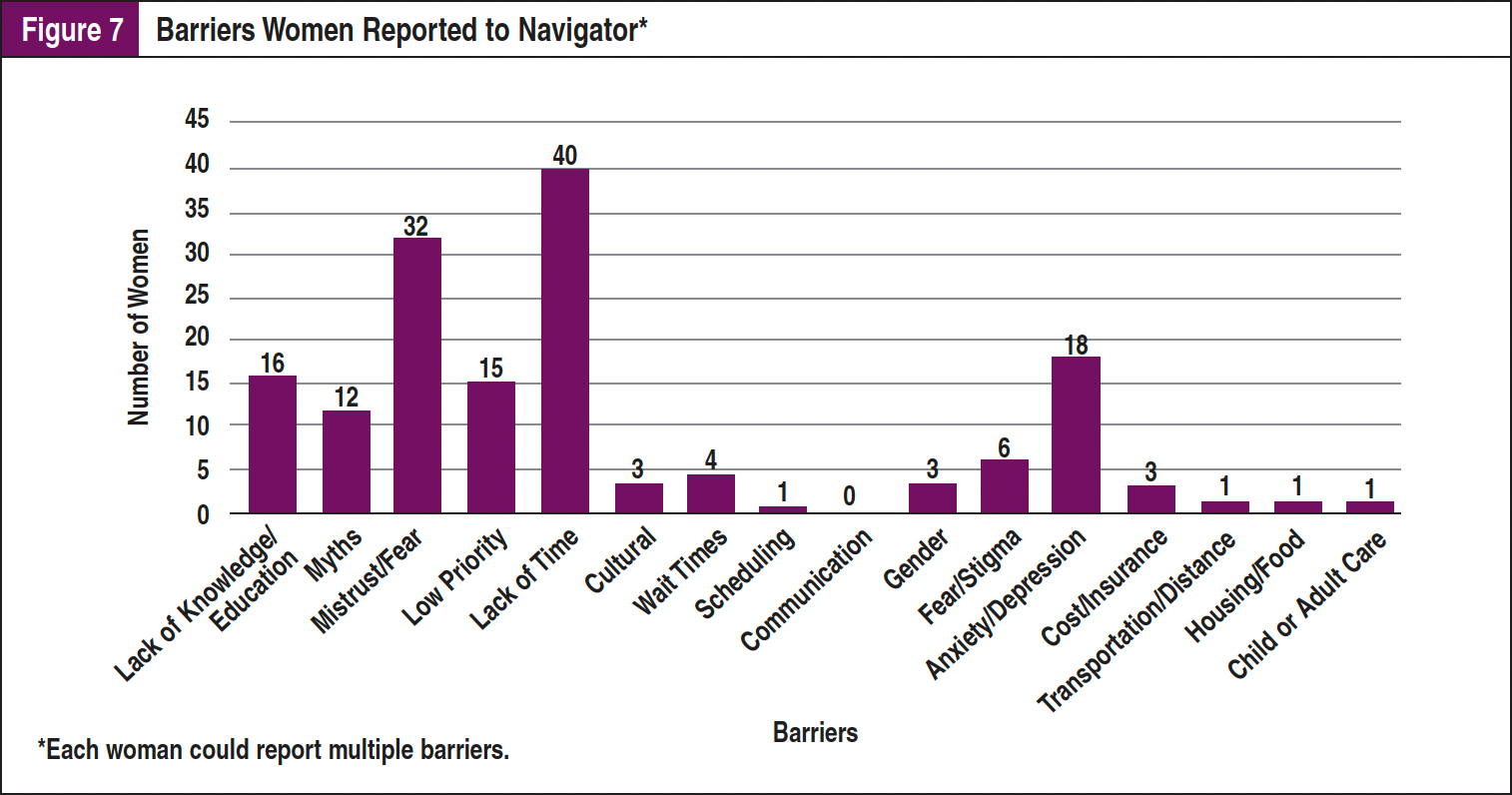
Women reported between zero and 8 barriers to receiving screening mammography. There were 168 total barriers identified, with 26 (20%) women reporting no barriers to mammography and 38 (30%) reporting more than 1 barrier to the navigator. The number of barriers reported by women is reported in Figure 6. The 4 most common barriers were lack of time (n = 40), mistrust and/or fear of the medical community (n = 32), mental health issues (n = 18), and lack of knowledge about screening mammography (n = 16). All barriers are reported in Figure 7.
Interventions
One hundred percent of the women received at least 1 intervention from the navigator. The most common intervention was education about mammography, with 100% of women receiving education. This education included information about the process and length of time a mammogram takes. This intervention was helpful in addressing the participants’ concerns about the time commitment required for screening. Ninety-six percent received education about breast cancer, 31% were introduced to the mammography staff, and 17% had a discussion about their fears about mammography with the navigator. All interventions were provided based on the women’s needs and requests (Figure 8).

Results
Two hundred twenty-eight women were scheduled for a screening mammogram prenavigation compared with 226 postnavigation. Detailed data by week are reported in Figure 1. The results of the Mann-Whitney U test for the number of mammograms scheduled prenavigation versus postnavigation had a P value of .76 (ie, not a statistically significant difference).
One hundred eighty mammogram screenings were completed prenavigation compared with 144 mammogram screenings for the same number of weeks postnavigation. Detailed data by week are reported in Figure 2. The P value for the number of mammograms completed prenavigation versus postnavigation was .29 (ie, not a statistically significant difference).
Limitations
There were multiple possible limitations to this project. COVID-19 had the ability to decrease the effectiveness of this project. COVID-19 shut down preventive cancer screening in most areas, with screening numbers for breast cancer decreasing by 89.2% in 2020.17 The FQHC closed their mammogram suite for 3 months from May 2020 until late July 2020. COVID-19 increased existing fears and mistrust in the African American population about medical care, which may have long-term effects on preventive cancer screening like mammography.13 Fear of COVID-19 may have decreased the number of women going to receive healthcare and participating or following through on mammograms. As both the prenavigation and postnavigation data collection times were after the start of COVID-19, it is difficult to ascertain what numbers would have been before the pandemic. Another pandemic-related limitation was a specific initiative implemented by the FQHC staff to schedule mammogram screening for women who were overdue or had an appointment during the closure of the mammogram suite. This push to get women scheduled may have inflated the prenavigation number of screening mammograms scheduled and completed.
The second limitation was associated with the days and times the navigator was on-site at the FQHC. The navigator was available 3 half days a week for navigation—Monday morning, Wednesday afternoon, and Friday morning. The navigator missed having contact with women who were coming to the clinic on the days and times she was not available on-site. Mammography is only available 3 days a week, but the navigator could have educated women on Tuesdays and Thursdays. It is possible that if the navigator had been on-site longer hours and/or more days, she could have had a higher volume of contacts with candidates for screening mammograms.
The third limitation relates to the characteristics of the population that reside near the FQHC. Some of the neighborhood is transient, with people moving into and out of houses or apartments regularly. There were multiple women who did not have a phone during their first contact with the navigator at the clinic, so the phone follow-up was not possible. There were also additional women who had phones shut off after they met with the navigator, so she could not contact them for the scheduled follow-up. To help overcome these issues, the navigator had set times and days she was available at Progressive Health and provided that schedule on preprinted cards with her phone number. This ensured that participants knew when they could find the navigator on-site, although this effort may not have overcome the limitation of hours.
The educational level and health literacy of the women receiving care at the FQHC may also have been a limitation. Existing written breast cancer and mammography education was used for the project. For women with low health literacy or those unable to read, the written information may not have been helpful, which means they missed a key piece of the navigation intervention.
Time could also have been a limitation, as the goal of the project was to show an increase in the number of women receiving breast screening via mammography after the implementation of navigation. A navigator who is on-site for a longer period of time and builds up relationships with women and the community may show more of an impact over a longer period. Because there is a lot of mistrust in the African American community toward healthcare, a longer project could have increased the number of women receiving screening mammograms because the navigator would have had more time to create positive, trusting relationships with the women coming to the clinic.
Discussion
While the results of this project were not statistically significant, there were multiple clinically significant pieces of the project. Forty-three women who met with the navigator got a mammography screening. One hundred fifty-eight women received education on mammography. Of those, 128 went on to receive additional navigation, including written education and help overcoming barriers so they could receive screening. The navigator noted this was the first time someone had spoken to many of the women about the importance of breast cancer screening. There were more than 20 women in their 50s who had never received a screening mammogram. There were also multiple women who had no idea they qualified to receive screening at age 40. These women benefited from hearing about the importance of breast cancer screening and knowing when they should get screened, and each had the additional benefit of working with someone who could help them to overcome individual barriers like fear, mistrust, lack of insurance, and multiple other barriers.
Thirty-six percent of women were uninsured or unaware if they were insured. The navigator was able to share with these women multiple ways they could get a mammography screening without any out-of-pocket cost to them. Cost has been noted to be a large barrier in other navigation projects, and being able to present options to decrease or remove out-of-pocket costs for women is vital. Without the navigator on-site, those women would not have received that information.
Of the women who the navigator screened for the project, 76% did not have a screening mammogram in the past year. This is very high compared with the average national mammography screening rate of 50%.7 The navigator was able to educate these women on the importance of screening and help them receive screening if they were ready. Educating these women and getting 43 to screening mammography may help decrease the late-stage diagnoses and high mortality among African American women in this area.
Lay navigators can be used to help the clinical team by assisting with patient education, assessing barriers to care, and helping patients get into cancer care. This takes pressure off the clinical team and lets them concentrate on the medical aspects of care. These partnerships of nonclinical and clinical staff will continue to be a way to provide all the care a patient needs in 1 space.
There is a lot of evidence that navigation is efficacious within multiple aspects of cancer care. There is no need to reinvent the wheel; there are multiple tool kits that share how to develop a navigation program. Future projects can be structured to examine navigation of underserved women, but extend the time frame of the project and the amount of time the navigator is available on-site. New studies can be done in other locations and populations to see if navigation can increase the number of women getting mammogram screenings within different populations. These studies should look at larger populations to increase the power of the study. They should also provide navigation services for a longer period. Any navigation project would need to have the navigation interventions created to fit the needs of the population in that area.
Now that the United States is out of its pandemic response to COVID-19 and people are seeking healthcare more regularly, navigation may provide the support women need to get screened. Navigation can be used to educate women about breast cancer and cancer screening, encourage them to schedule screening, and help decrease barriers that keep women from getting a mammogram screening. With the large decrease in cancer screening that has occurred since the start of the pandemic, it is possible that navigation is a way to increase the number of women receiving breast cancer screening. This may be especially true in underserved and minority populations that have preexisting barriers to cancer screening.
References
- Siegel RL, Miller KD, Jemal A. Cancer statistics, 2020. CA Cancer J Clin. 2020;70:7-30.
- McCanney J, Winckworth-Prejsnar K, Schatz AA, et al. Addressing survivorship in cancer care. J Natl Compr Canc Netw. 2018;16:801-806.
- Olaku OO, Taylor EA. Cancer in the medically underserved population. Prim Care. 2017;44:87-97.
- Siegel RL, Miller KD, Fuchs HE, Jemal A. Cancer statistics, 2021. CA Cancer J Clin. 2021;71:7-33.
- Siegel RL, Miller KD, Fuchs HE, Jemal A. Cancer statistics, 2022. CA Cancer J Clin. 2022;72:7-33.
- DeSantis CE, Ma J, Gaudet MM, et al. Breast cancer statistics, 2019. CA Cancer J Clin. 2019;69:438-451.
- Monticciolo DL. Current guidelines and gaps in breast cancer screening. J Am Coll Radiol. 2020;17:1269-1275.
- Singh GKJ, Jemal A. Socioeconomic and racial/ethnic disparities in cancer mortality, incidence, and survival in the United States, 1950-2014: over six decades of changing patterns and widening inequalities. Journal of Environmental and Public Health. 2017;(138):1-19.
- Siegel RL, Miller KD, Jemal A. Cancer statistics, 2019. CA Cancer J Clin. 2019;69:7-34.
- Ogedegbe G, Cassells AN, Robinson CM, et al. Perceptions of barriers and facilitators of cancer early detection among low-income minority women in community health centers. J Natl Med Assoc. 2005;97:162-170.
- Hall IJ, Tangka FKL, Sabatino SA, et al. Patterns and trends in cancer screening in the United States. Prev Chronic Dis. 2018;15:E97.
- Miller MM, Meneveau MO, Rochman CM, et al. Impact of the COVID-19 pandemic on breast cancer screening volumes and patient screening behaviors. Breast Cancer Res Treat. 2021;189(1):237-246.
- Price-Haywood EG, Burton J, Fort D, Seoane L. Hospitalization and mortality among black patients and white patients with Covid-19. N Engl J Med. 2020;382:2534-2543.
- Fisher-Borne M, Isher-Witt J, Comstock S, Perkins RB. Understanding COVID-19 impact on cervical, breast, and colorectal cancer screening among federally qualified healthcare centers participating in “Back on track with screening” quality improvement projects. Prev Med. 2021;151:106681.
- Schifferdecker KE, Vaclavik D, Wernli KJ, et al. Women’s considerations and experiences for breast cancer screening and surveillance during the COVID-19 pandemic in the United States: a focus group study. Prev Med. 2021;151:106542.
- Chen RC, Haynes K, Du S, et al. Association of cancer screening deficit in the United States with the COVID-19 pandemic. JAMA Oncology. 2021; 7:878-884.
- London JW, Fazio-Eynullayeva E, Palchuk MB, et al. Effects of the COVID-19 pandemic on cancer-related patient encounters. JCO Clin Cancer Inform. 2020;4:657-665.
- Maringe C, Spicer J, Morris M, et al. The impact of the COVID-19 pandemic on cancer deaths due to delays in diagnosis in England, UK: a national, population-based, modelling study. Lancet Oncol. 2020;21:1023-1034.
- Janz NK, Becker MH. The Health Belief Model: a decade later. Health Educ Q. 1984;11:1-47.
- Fulton JP, Buechner JS, Scott HD, et al. A study guided by the Health Belief Model of the predictors of breast cancer screening of women ages 40 and older. Public Health Rep. 1991;106:410-420.
- Yarbrough SS, Braden CJ. Utility of health belief model as a guide for explaining or predicting breast cancer screening behaviours. J Adv Nurs. 2001;33:677-688.
- Kamaraju S, DeNomie M, Visotcky A, et al. Increasing mammography uptake through academic-community partnerships targeting immigrant and refugee communities in Milwaukee. WMJ. 2018;117:55-61.
- Wallington S, Oppong B, Dash C, et al. A community-based outreach navigator approach to establishing partnerships for a safety net mammography screening center. J Cancer Educ. 2018;33:782-787.
- Nonzee NJ, Ragas DM, Ha Luu T, et al. Delays in cancer care among low-income minorities despite access. J Womens Health (Larchmt). 2015;24:506-514.
- Drake BF, Tannan S, Anwuri VV, et al. A community-based partnership to successfully implement and maintain a breast health navigation program. J Community Health. 2015;40:1216-1223.
- George Washington Cancer Institute. Oncology Patient Navigator Training: The Fundamentals. https://aonnonline.org/education/navigation-tools/gw-cancer-center-opn-training-the-fundamentals.



