Patrick J. Dineen, MD, MBA; Liana Orduna; Sara Hansen; Angela Tejeda; Robert Alejo
Stony Brook Cancer Center, Mobile Mammography
Ronkonkoma, NY
Background: As part of Stony Brook University, a flagship university of the State University of New York system, the Stony Brook Cancer Center provides a full spectrum of services from primary to tertiary care across both inpatient and outpatient sites. The county has 3 federally designated medically underserved areas and many geographically isolated areas on the rural east end of Long Island. As one travels east from New York City, the accessibility of public transportation becomes exponentially limited. A county needs assessment data analysis concluded that women in underserved areas were most likely to forego breast cancer screening. Despite the substantial number of women not receiving recommended screening services, there were no mobile mammography units (MMUs) serving the county.
Objective: To determine the effectiveness of the mobile healthcare clinic (MHC) removing barriers to screening vulnerable populations, and to prove that the mobile MMU benefits the health of our community through prevention services while saving on healthcare resources that can be reinvested into the community. Furthermore, we would like to prove a positive return on investment (ROI) and a decreased dependence on emergency department visits for the populations we screen. Finally, we will compare the patient population served on the MMU with that of the same hospital’s brick-and-mortar breast center to show the increased diversity screened on the MMU, all while determining the effectiveness of the MMU’s screening procedures by comparing its callback rate with 2 of the same hospital’s stand-alone breast screening facilities.
Methods: Using the data collected from the MMU program from its inception in October 2018 and entering the data into the Harvard Medical School’s Mobile Health Map tool, program impact measures were calculated, including quality-adjusted life years (QALY), money saved from prevention system impact (emergency department visits avoided), and the bottom-line impact (ROI, total cost savings to date). The patient population at the brick-and-mortar breast center in the same healthcare system was used to compare patient demographics between the breast center and the MMU. Radiology summary reports were used to tabulate the recall rate of screening mammograms from 2 stand-alone facilities under the same healthcare banner, comparing the callback calculations with that of the MMU.
Results: The Mobile Health Map tool with our collected data from over 5000 patients showed the following for 4 successive years: 1167 total emergency department visits avoided, ROI up from 12:1 to 20:1, and QALY ranging from 73 to 103 annually. The demographics of patients screened on the MMU compared with the brick-and-mortar facility showed that 71% of the patient population on the MMU were minorities, compared with just 22% at the brick-and-mortar facility. The comparative analysis of recall rates between the MMU and 2 stand-alone screening facilities showed that all 3 screening sites shared an equal recall rate of 15%.
Conclusion: The MMU, along with other MHCs across the country, is a proven superior service since the program(s) is providing lifesaving preventive cancer screenings to underserved populations who do not have access to a primary care physician and would otherwise use the emergency department as their medical home. This MMU decreases the dependence on local emergency departments while offering preventive services free of charge for the uninsured, alleviating the fear of high medical costs while granting lifesaving measures. The MMU eliminated many of the barriers to healthcare that the underserved populations are facing, including a lack of transportation, lack of health insurance, and inability to speak English, among others. Our findings proved that this patient population sees the MMU as a safe space and has now relied on its services for repeat screenings, education, and as their point of contact in the medical field for them, friends, and family members.
There are more than 2000 mobile health clinics (MHCs) operating in the United States. These MHCs offer services ranging from primary care to cancer screenings. A growing body of literature supports MHCs as a successful and cost-effective model of healthcare delivery.1 Because MHCs can overcome many healthcare barriers, especially for minorities, immediate benefits are obvious, including preventive services offered on Stony Brook Cancer Center’s Mobile Mammography program. This program and similar ones around the country improve individual health outcomes, advance population health, and reduce healthcare costs compared with traditional clinical settings.1 These specialty vehicles fulfill the needs of underserved populations by not only engaging on a personal level but also by gaining the trust of vulnerable populations by delivering much-needed services directly into each community. The most recent data released by the CDC reveal that after skin cancer, breast cancer is the most common cancer among women in the United States. The average risk of a woman developing breast cancer in her lifetime is 13%.2
In 2018, the latest year for which incidence data are available, over 254,000 new cases of female breast cancer were reported, with 42,465 women dying of this cancer.3 For every 100,000 women, 127 new breast cancer cases were reported, making it the highest rate of new cancer cases among all races and ethnicities.3 Furthermore, the state with the highest rate of diagnosed cancers in the United States is New York.3 A county needs assessment data analysis for Long Island, NY, concluded that women in underserved areas were most likely to forego breast cancer screening. Despite the substantial number of women not receiving recommended screening services, there were no mobile mammography units (MMUs) serving the county. The purpose of this paper is to prove the effectiveness of the MHC in removing barriers to screening vulnerable populations, treat a more diverse population than brick-and-mortar facilities, and decrease the dependency on local emergency departments, all while showing the money saved on healthcare resources that can be reinvested into the community.
Methods
Data collected from over 5000 MMU patients from 2018 to 2022 were interpreted to show the impact that the program has on its local community, its own medical system, as well as the downstream effect on the healthcare system’s government funds. Metrics calculated include quality-adjusted life years (QALY), emergency department visits avoided per year, and the program’s return on investment (ROI). Furthermore, MMU data from our same healthcare system’s brick-and-mortar breast center were collected to compare the demographics screened, including ethnicities and insurance status of each client, along with a metric to measure the effectiveness of the MMU by comparing the recall rates with those of 2 other stand-alone facilities within the same healthcare system.
Harvard Medical School’s Mobile Health Map brings the visualization of the collected data to life. This tool was created for MHCs to enter collected data into an interactive dashboard to assess the effectiveness and impact of one’s program for each year of operations. The data collected from the Mobile Health Map were used to analyze the MMU’s effectiveness in concurrent years, comparing metrics while analyzing the purpose of any major shifts from year to year. Patient age-group, race/ethnicity, insurance status, number of visits, services offered, and the clinic’s operating costs are all metrics used to prepare the finalized data. The dashboard is particularly useful to our program since our MMU provides one of the listed costs and clinically effective prevention services, as defined by the National Prevention Program.4
Aside from the aforementioned impact of our MMU to the healthcare system and funders, a particular nonmonetary metric of equal importance to our program is the demographic data collected on the MMU. Marginalized community members are groups that experience discrimination and exclusion because of unequal economic, political, social, and cultural dimensions, including immigration status.5 This includes a vast number of minorities throughout Long Island, many of whom have no desire to bring themselves or family members to a healthcare facility due to fear of mistreatment and discrimination. Yet, over time, many of these populations have turned to our MMU for not only their preventive screenings but as their sole point of contact in the medical community. This is because our MMU employs a staff as diverse as the population in which they screen, has team members who speak multiple languages, and whose primary focus is to put the patient at ease while being a resource for all questions that they may have. Due to allowing only 1 patient on the mobile unit at a time, the MMU has become a safe space of individualized attention for each person who enters. The patient who once faced multiple barriers to healthcare is now in a safe, comfortable, clean environment with 3 professionals who can communicate clearly, and whose sole focus is to care for this patient. The gratitude of each patient is proved through survey card comments, the warm embraces shared with the staff, and the rate of return among the patient population.
Results
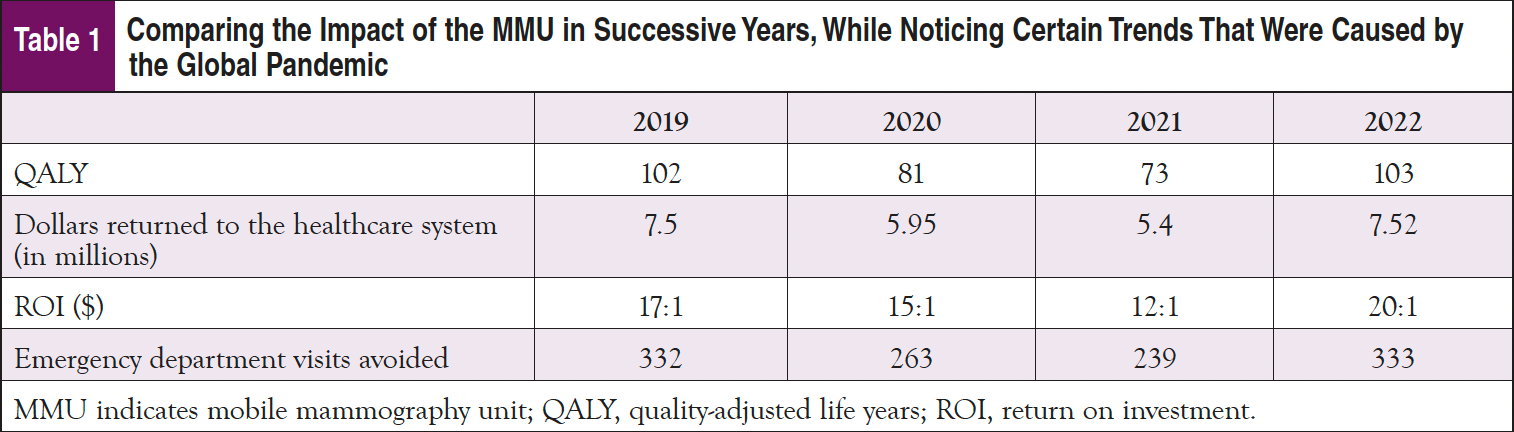
The MMU program impacts the QALY, which is a value of health outcomes and medical interventions offered at the MHC. QALY is a unit of measurement often used in cost–benefit analysis as a prediction of both quality and duration of life after a medical intervention such as a screening mammogram. The calculated data for Stony Brook’s MMU are as follows: QALY was 102 in 2019, 81 in 2020, 73 in 2021, and 103 in 2022 (Table 1). The money saved from prevention was as follows: $7.5M in 2019, $5.95M in 2020, $5.4M in 2021, and $7.52M in 2022. This helps to understand the MMU’s impact on the health of our community through delivered prevention services, as well as what can be done better to increase the trends in successive years.
The system impact of the program is based on the number of unnecessary emergency department visits avoided due to the nature of the preventive screening measures taken by the MMU. This is because of the multiple barriers that exist for underserved women in America, such as lack of transportation, anonymity concerns, and the inability to speak English, among others. These barriers deter certain populations from adhering to screening guidelines, including mammography. Oftentimes it will take physical changes to the breast for a woman to be concerned enough to face her fears and walk into a facility for medical treatment. By that time, the disease has progressed to a later stage than if she were to receive a screening mammogram earlier in the process, and the patient turns to the emergency department as a medical home since she is not under the care of any medical practitioner. Preventable healthcare spending in the emergency department costs billions of wasted dollars annually in the United States, with each emergency department visit averaging over $1000. According to the Healthcare Cost and Utilization Project, aggregate emergency department costs are higher for females, who account for 56% of total emergency department visits, with half of the visits for patients from the lowest income communities.6 Mobile clinics provide accessible care at a more affordable cost to the healthcare system than emergency department visits.7
Stony Brook’s MMU is tagged as a necessary intervention, promoting mammography for the marginalized women who visit the emergency department for nonurgent care.7 This has allowed the program to alleviate local emergency departments by the following number of visits per year: 332 in 2019, 263 in 2020, 239 in 2021, and 333 in 2022. This has collectively avoided nearly $1.2M in costs on local hospitals, all of which are resources saved that can be reinvested into the community (Table 1).
The calculation of ROI proves the bottom-line impact of our MMU. This determines the business case, proving whether our program is able to save money for the healthcare system. The calculated ROI shows how each dollar invested into our program provides downstream savings, demonstrating the cost efficiency of this MMU to community funders and leaders. Stony Brook’s MHC’s ROI ($) is as follows: 17:1 in 2019, 15:1 in 2020, 12:1 in 2021, and 20:1 in 2022 (Table 1).
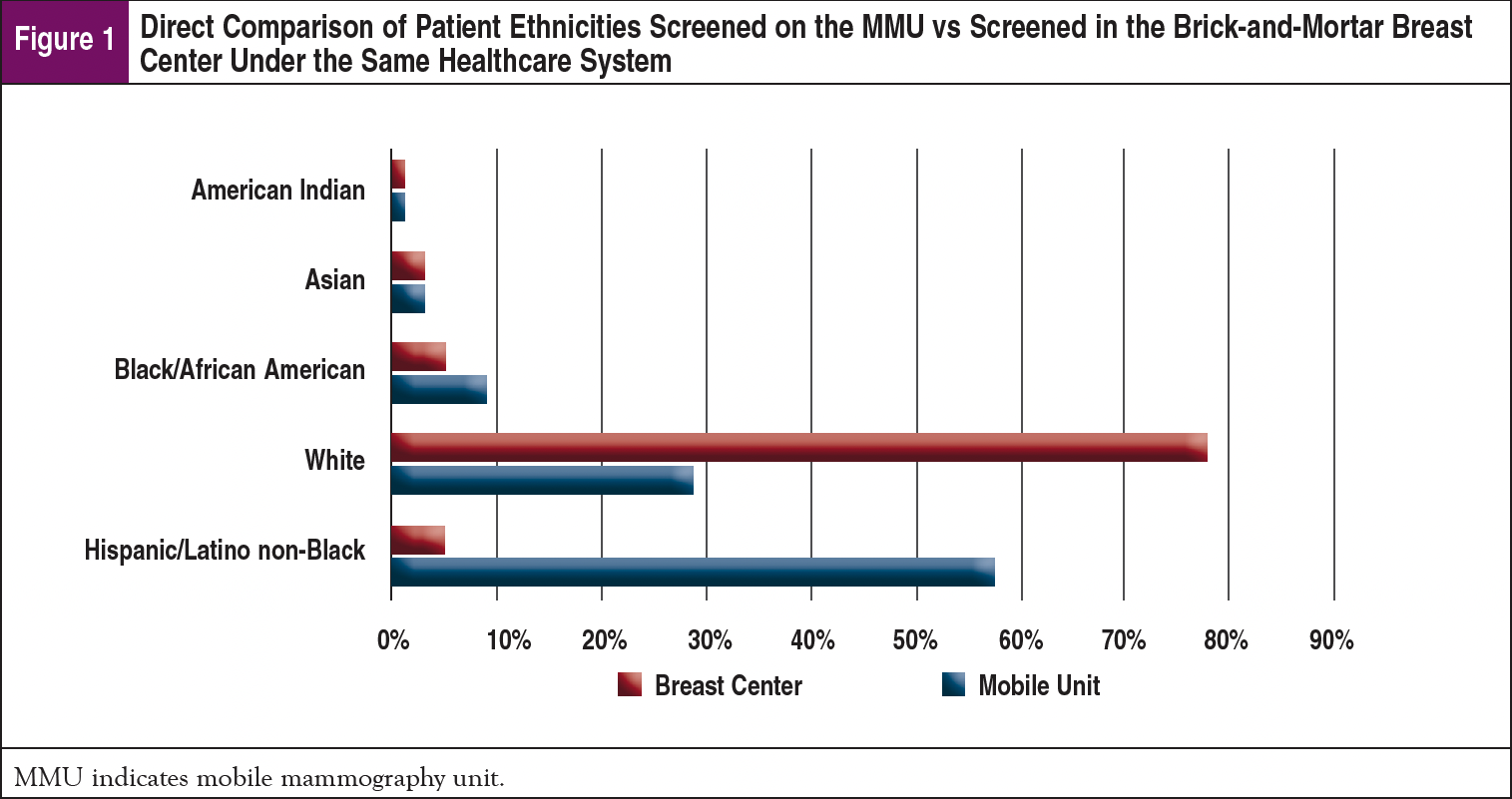
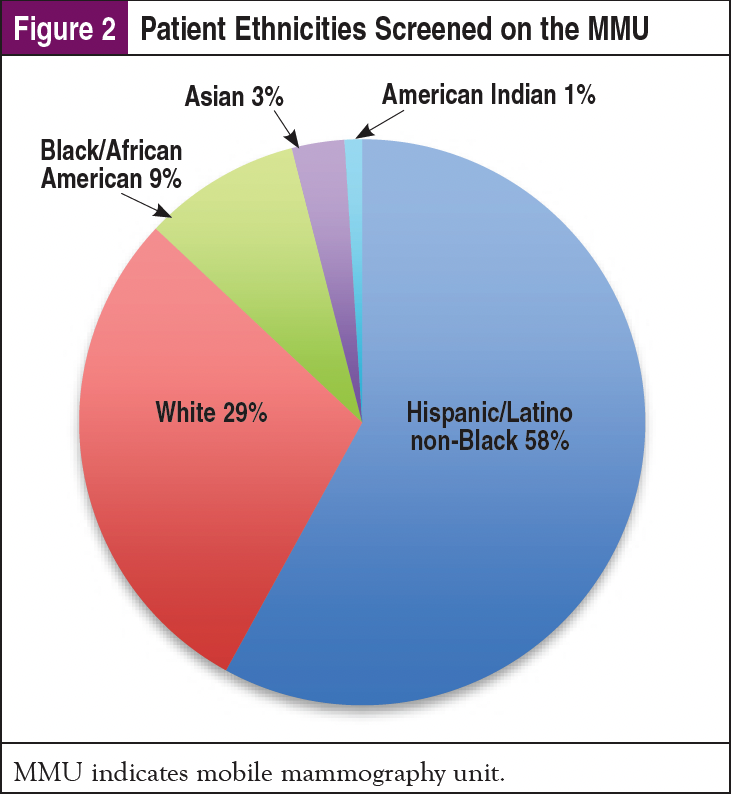
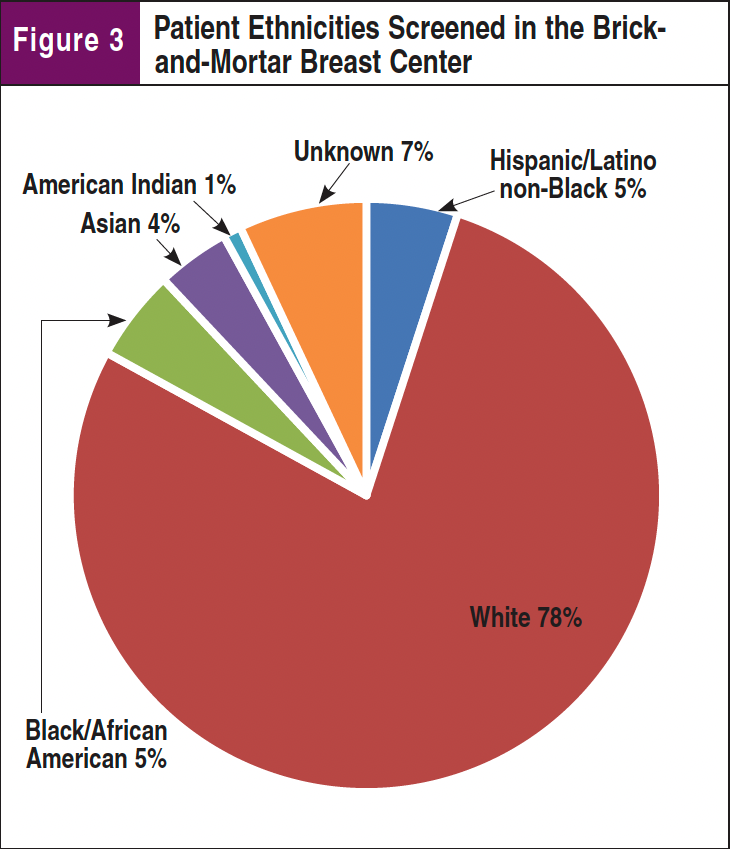
The nonmonetary impact of the MMU is shown through the patient population screened, as 71% are classified as minorities: 58% Hispanic/Latino, 9% Black/African American, 3% Asian, and 1% American Indian. A direct comparison was made to the patient population screened at the brick-and-mortar breast center within our same healthcare system, screening a minority population of just 15%. A comparative analysis is shown in Figure 1, with each facility shown separately in Figures 2 and 3. This proves that the MMU is able to physically address the needs of many populations that are unable to be reached by brick-and-mortar healthcare facilities.
Discussion and Navigation
Calculating the impact of a program not only proves the current state of affairs but can also be used to determine the future direction of the program by analyzing successive years of data. The calculations of QALY, money saved, ROI, and avoided emergency department visits are all impressive stand-alone statistics, but they offer a story that will hopefully be unmatched for the considerable future. The decrease in all numbers from 2019 to 2020 is caused by the sudden shutdown of the MMU due to the COVID-19 pandemic. This saw the QALY drop from 102 to 81 for a calendar year, with almost a 70-person decrease in avoided emergency department visits. The numbers continued to fall as 2020 became 2021, with the pandemic continuing to disrupt everyday life. Once community screening events were allowed to return, new safety measures needed to be implemented, including new training for the MMU staff, new health questions for the patients, and a new protocol added to ensure the safest operations for this program moving forward, all of which still exist today. With the doors now open, hesitancy still remains, but it is imperative that the Long Island population returns to their regularly scheduled cancer screenings. Now more than ever, dependency on MHCs exists for nearly every medical specialty, with increased access being at the forefront of the world today. 2022 proved that our MMU program has returned to normal, even superseding 2019 as the most successful year to date.
The strength of the program comes from the individualized care each patient receives from our staff, starting with the initial phone call, down to the final report, and beyond. The pride is in the patient navigation. For a normal screening mammogram of Breast Imaging-Reporting and Data System (BI-RADS) 1 or 2, the patient and her doctor on record are both sent letters explaining the results, with the patient receiving an additional letter in layman’s terms.With a BI-RADS 0 result, the patient receives a personal phone call from the MMU staff, regardless of insurance status. This is crucial in patient-centered care because questions can be answered regarding the patient’s next steps, with help being offered immediately to ease the burden on the patient. For the insured patient, she is able to attend any facility that accepts her insurance for a diagnostic follow-up appointment, as the patient is not pressured to seek care at any particular facility. In an effort to provide continuity of care, the MMU staff closely monitors each patient’s case. This offers the opportunity to build a relationship as well as identify individual needs of the patient throughout the diagnostic process.
According to the US Census Bureau, the overall percentage of adults 18 to 64 years of age in Suffolk and Nassau counties without health insurance is 10%.8 On the MMU, over 55% of the women screened have no health insurance, which is indicative of the barriers faced in the neighborhoods served. The MMU staff enrolls all uninsured patients into Cancer Services Program (CSP), a state-funded program that allows qualified individuals to benefit from no-cost cancer screenings, including clinical breast exams, Pap tests for cervical cancer screening, and fecal immunochemical tests for colon cancer. CSP also covers the cost for necessary diagnostic testing and biopsy. Patients diagnosed with a cancer are enrolled in Medicaid or another eligible insurance to cover all incurring costs. Nonresidents are enrolled in emergency Medicaid.
Once the patient is enrolled into CSP, she gains the guidance of a knowledgeable staff member to spearhead all future appointments and treatment options. Once an uninsured BI-RADS 0 report is finalized, the MMU staff contacts the patient to inform her of the results and explains that she will be contacted by the CSP staff who will help her book a diagnostic appointment at a facility closest to her home. The patient is now under the care of the MMU and CSP staff, who are following the patient until the case is closed. If an uninsured patient does not have a physician to provide a prescription for her diagnostic exams or biopsy, one is provided for her from the MMU program, staying true to helping eliminate barriers that decrease access to care.
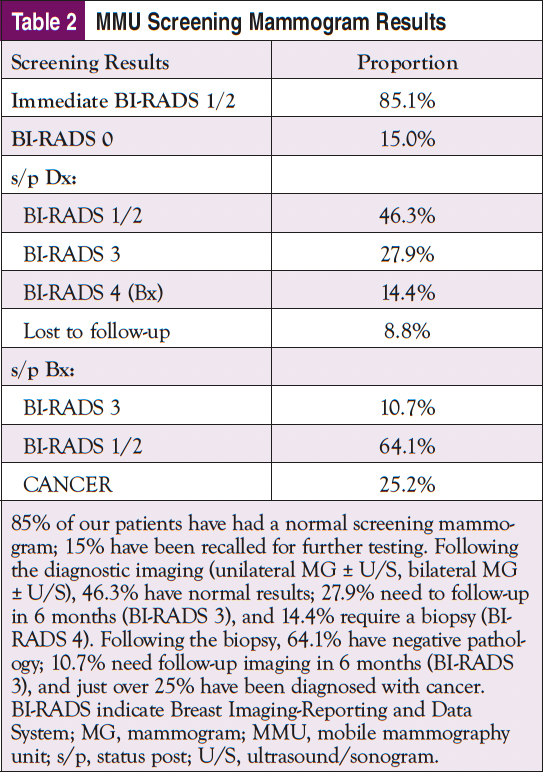
To date, over 30 women have been diagnosed with malignancies, many of which were early-detected cancers, after being screened on the MMU. Of these cases, 59% are classified as White, 33% are Hispanic, and 8% African American. The average age of a diagnosed patient on the mobile unit is 60.6 years, with a range of 41 to 86 years; 33% of the patients are uninsured, with all costs covered by CSP. In an attempt to compare the MMU with results from 2 stand-alone facilities under the same healthcare system, recall rates were compared among the 3 programs, all of which have identical rates of 15%. For all MMU screening mammogram results, see Table 2.
Conclusion
Stony Brook Cancer Center remains on the forefront of patient care, removing barriers so its services can benefit each and every community member who seeks medical care. This is evident in its support and sustainment of the already successful Mobile Mammography Program that delivers its preventive cancer screening to all members of society, regardless of the patient’s insurance or immigration status. The MMU continually visits businesses, libraries, churches, and various other community locations, all at no charge to the host site, in order to leave no excuse for women not to be screened. To date, the MMU has screened over 5500 women, many of whom would not have received a mammogram if not for the MMU being parked in their community, as repeatedly stated in patient survey cards. These women are uninsured, lack transportation, do not have a primary care provider, and are busy caring for loved ones. The majority of the women screened on the MMU are of ethnicities not seen within the hospital walls, not for lack of trying, but for the inability of a brick-and-mortar facility to establish personal connections by extending into underserved communities. The MMU provides solutions to these accessibility hurdles, which is why it has such a profound impact within the most needed areas. The MMU will not rest on its laurels, as breakthrough steps have been taken to expand the services to offer more preventive cancer screenings to a larger population within the Long Island communities. Despite the communal impacts, financial questions do remain, as medical administrators nationwide beg the question of the worth and value of the investments of mobile units within their own healthcare systems.
The greater the availability of MHCs in New York and throughout the country, the better the odds are for early detection, thus increasing survival rates of breast cancer. Medicine, like all other businesses in today’s world, needs to tailor services to the client by becoming easily accessible with less wait times. MHCs not only accomplish these goals, they also produce a cost-saving measure to our country’s healthcare system, which currently ranks last overall among 11 high-income countries despite spending the highest proportion of its gross domestic product on healthcare. A main factor for our current ranking: poor access to care.9
QALY and ROI are often used in cost–benefit analysis related to healthcare and treatment options. When deciding on the appropriate level of healthcare spending, it is typical to equate the marginal cost of healthcare to the benefits received. The benefit of mortality reduction, QALY, socioeconomic impact in Long Island communities, and the direct impact on improving our country’s medical standing are many reasons why MMUs and MHCs are here to stay.
It takes time, trust, and quality-level care to make a positive impact within a community, especially for an unknown entity starting an MHC. Stony Brook’s MMU has made its mark throughout Long Island and continues to strive to meet the needs of every individual community member. The impact of the MMU will continue being measured by increasing the diversity among patients screened, decreasing the number of patients relying on the emergency department as primary care, educating community members, and saving lives. The complete list of how this MMU is impactful is long, yet rewarding. MMUs and MHCs are the future of medicine worldwide. Countries such as Grenada, Pakistan, Bangladesh, and Yemen have MHCs to increase the reach of healthcare, which shows the global socioeconomic impact is both necessary and sustainable.
Funding
No funding sources for the article.
References
- Yu SW, Hill C, Ricks ML, et al. The scope and impact of mobile health clinics in the United States: a literature review. Int J Equity Health. 2017; 16:178.
- American Cancer Society. Key Statistics for Breast Cancer. www.cancer.org/cancer/breast-cancer/about/how-common-is-breast-cancer.html#:~:text=Lifetime%20chance%20of%20getting%20breast,will%20never%20have%20the%20disease. 2023.
- Centers for Disease Control and Prevention. Cancer Statistics at a Glance. www.cdc.gov/cancer/dataviz. 2020.
- Mobile Healthcare Association. MobileHealthMap.org and the Return on Investment Calculator. https://mobilehca.org/mobile_map.html. 2020.
- The National Collaborating Centre for Determinants of Health. St. Francis Xavier University. https://nccdh.ca/glossary/entry/marginalized-populations. 2022.
- Moore B, Liang L. Costs of emergency department visits in the United States. Healthcare Cost & Utilization Project. www.hcup-us.ahrq.gov/reports/statbriefs/sb268-ED-Costs-2017.jsp. 2020.
- Hatcher-Keller J, Rayens MK, Dignan M, et al. Beliefs regarding mammography screening among women visiting the emergency department for nonurgent care. J Emerg Nurs. 2014;40:e27-e35.
- US Census Bureau. QuickFacts. Nassau County, New York; Suffolk County, New York. www.census.gov/quickfacts/fact/table/nassaucountynewyork, suffolkcountynewyork/HCN010212. 2021.
- Frellick M. U.S. Health System Ranks Last Among 11 High-Income Countries. WebMD Health News. www.webmd.com/health-insurance/news/20210804/us-health-system-ranks-last-among-11-high-income-countries. 2021.



