Tools that help to characterize patient acuity have been used in healthcare for decades and have proved successful as a means of determining staffing needs, improving patient care, and controlling costs.1 Acuity tools can be incorporated into oncology patient navigation programs to support and enhance the effectiveness of navigators through patient-centric evidence-based methods that may have the potential to decrease the overall cost of care.
Objective
The aim of this scoping review is to provide an evidence base that will aid in the development of an oncology patient navigation–specific acuity tool.
Methods
Search Strategy
We utilized the scoping review method2 to research and analyze articles related to patient acuity in an oncology setting published in the past 10 years. This method was chosen to broadly examine the key concepts of acuity, including definition, tools, and factors related to measurement. To develop an overview of existing evidence from a navigation standpoint, the review addressed the following research questions to reveal particular supporting attributes of acuity:
Question 1. What are the definitions of acuity, acuity tool, acuity system, barriers to care, and distress?
Question 2. How can barriers to care be categorized?
Question 3. Is there a relationship between barriers to care and acuity?
Question 4. Is there a relationship between distress and acuity?
Question 5. What acuity tools already exist?
Question 6. How can a patient acuity score relate to factors such as productivity, return on investment (ROI), staffing/caseload, effectiveness, and time management?
Question 7. Is there any support in the literature to demonstrate that any of the Academy of Oncology Nurse & Patient Navigators (AONN+) Standardized Metrics are patient acuity measures?
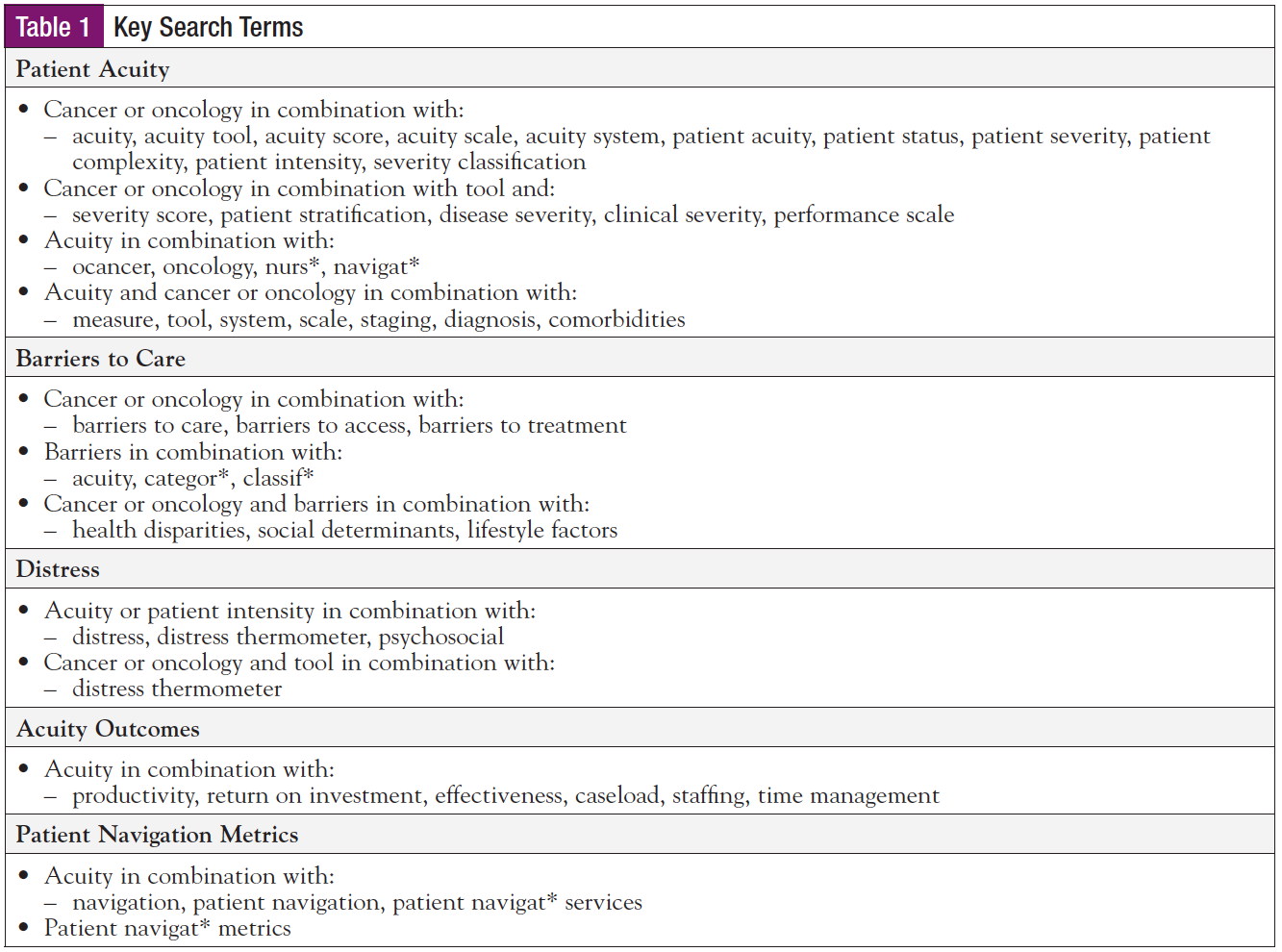
PubMed, MEDLINE (Ovid), and CINAHL databases were searched for literature published between January 1, 2008, and December 25, 2018, using the search terms shown in Table 1. In some cases (eg, definitions, existing acuity tools, factors related to acuity), we included relevant articles published outside of the dates covered by the search. To expand the number of results, we performed hand searches of reference lists for additional articles of relevance. Articles were limited to studies that focused on or were conducted in humans and were published in English.
Data Extraction
The PRISMA model was used to evaluate the articles based on the 7 selected questions.3 Included articles were classified by evidence type and sample size and reviewed for relevant study findings and information. We determined the quality level of included articles based on how well they helped the research questions along with their limitations.
Results
Study Characteristics
The search criteria and limits described above yielded 1711 articles. After titles and abstracts were screened for relevance, 199 full-text articles were reviewed and 105 articles were identified for inclusion in the literature review (Figure). Nineteen (18.1%) of 105 articles addressed multiple research questions.
1. Definitions of Acuity, Acuity Tool, Acuity System, Barriers to Care, and Distress
Seventeen (16.2%) of 105 articles evaluated the definitions of acuity, acuity tool, acuity system, barriers to care, and distress. Two articles outside the dates covered by the search were included because they contributed differentiation between caseload versus workload.4,5 Acuity was defined in 6 articles; however, there is no universal definition for acuity. In 3 articles, a basic definition of acuity was discussed as being the amount of time spent caring for a patient.6-8 Brennan and Daly8 clarified the concept of acuity and touched upon the need to separate acuity from productivity. The authors proposed the following definition of acuity: “a measure of the severity of illness of the patient and the intensity of nursing care that patient requires.”
More complex definitions of acuity were found in the other 3 articles—these incorporate its subsequent effect on workload or case management4,9 or its ability to capture functional and health limitations.10 Two of the articles defined acuity tool/system/scale as systems for quantifying patient severity/acuity to determine caregiving staffing.5,11 Barriers to care, although discussed in several articles included in the review, was only formally defined in 1 article as being “associated with screening, late presentation to care, and lack of treatment, which in turn result in poor health outcomes and health disparities.”12 Eight of the articles defined distress, which was generally well characterized, as a multifactorial unpleasant emotion that may affect one’s ability to cope or manage disease.13-20 Barry and colleagues13 further stated that distress may be experienced with or without a psychiatric syndrome and “can affect a patient’s ability to cope with and manage disease which, in turn, may affect health outcomes.”
Huber and Craig4 encouraged the selection of valid tools and emphasized the need for case management to be “front loaded,” with most of the effort in the beginning of treatment; this level of effort is usually not required to be maintained over time. The front-loaded concept is demonstrated by the navigators’ experience with their patients and supports the idea of acuity. The authors also discussed “acuity differential,” which reflects the outcome of reduction in complexity of core case management factors due to case manager interventions. Reduction in complexity, and thus acuity, corresponds directly to reductions in client symptoms, inappropriate case environment, and ineffective provider use.4
2. Categorization of Barriers to Care
Thirty-one (29.5%) of 105 articles evaluated the categorization of barriers to care. Boehmer21 provides 4 categories related to barriers to care: (1) patient-level barriers, (2) patient-physician relationship, (3) provider characteristics, and (4) system factors. Similarly, many articles presented 3 major distinct categories of barriers to care: patient-related, provider-related, and system-related.22-25 These categories of barriers align with the National Comprehensive Cancer Network Distress Thermometer, which incorporates practical problems, family problems, and emotional problems in the determination of a problem list to measure distress.18 Carrillo and colleagues12 categorized barriers to healthcare access as structural, financial, and cognitive, discussed their interplay, and included evidence-based examples of health outcomes associated with each type of barrier. The authors noted that these barriers lead to decreased prevention, late presentation, and decreased care. In the discussion of barriers to care by Guadagnolo and colleagues,26 factors contributing to health disparities were identified as: (1) patient-related (ie, mistrust, low health literacy, socioeconomic status), (2) physician-related (ie, lack of cultural competency), and (3) healthcare system–related (ie, funding status). In another article, barriers were classified as either financial or nonfinancial.27
Some articles provided further subcategorization of barriers (eg, dividing patient-related issues into psychosocial issues and communication issues28 or into communication and emotional barriers29). Other articles identified physical/geographic and logistical/transportation issues as a separate major category.30-35 Esparza36 categorized barriers into 7 groups: (1) geographic (rural or inner city health professional shortage area and lack of capacity), (2) cultural (patient’s and provider’s beliefs and behaviors toward one another, disease, or the medical system), (3) socioeconomic (insurance, inability to pay for services, lower education), (4) system/organizational (long wait times, limited hours, not access friendly), (5) linguistic and communication, (6) social (child care issues, lack of support system), and (7) racism and provider bias. Other articles also categorized barriers into more than 5 groups,37-41 but these additional distinctions may be more appropriate as subgroups of the larger 3 categories discussed above. Korber and colleagues38 listed barriers and enhancers to breast cancer treatment according to the following themes: (1) education and information (which have a critical role), (2) symptom management, (3) support, (4) treatment to meet individual needs, (5) importance of teamwork, (6) resource assistance, (7) coordination of care, (8) role definition, and (9) survivorship.
Other articles did not categorize barriers but instead described specific types of barriers, gave additional perspectives, or provided other interesting findings. Studies of minorities described several specific barriers to care, including difficulty coordinating services or providing therapeutic interventions,42 belief in alternative therapy,43 and issues related to privacy/trust.44,45 In a similar manner, other articles gave perspectives that focused exclusively on financial barriers46 and barriers to care from the navigator’s standpoint.47 Additional studies discussed differences in barriers to care among married and unmarried patients,48 barriers that are common in newly diagnosed patients,49 and variables that account for racial differences in time until treatment.50
3. Relationship Between Barriers to Care and Acuity
Seven (6.7%) of 105 articles evaluated the relationship between barriers to care and acuity. Patients with low acuity were found to need less help with services such as education, care coordination, travel, and follow-up.51 Unsurprisingly, the total number of barriers to care was found to predict increased navigation time39,52 and time to resolution.23,39 More specifically, barriers such as being unmarried and unemployed were associated with increased navigation assistance.49 Carroll and colleagues52 analyzed the time needed for managing common barriers to cancer treatment and found that each additional barrier resulted in a 16% increase in navigator time. This finding supports the concept that barriers do need to be weighted as to the acuity, with the greater the number, the greater the resulting acuity. As such, the development of an acuity tool should also address the need to measure barriers objectively using different weights for individual barriers versus relying on subjective measures.
Lin and colleagues53 analyzed factors that impact a patient navigator’s time and noted that some barriers (financial, transportation, and fear/feelings about cancer) required more time, but the amount of navigator time spent per patient was consistent. This finding supports the idea that barriers do not need to be weighted in an acuity tool. The type of barrier did not have much effect on timeliness of care. Therefore, the authors argued that navigation services should be directed to patients with the most need—those facing barriers and delays. This supports the use of acuity to drive the actions of the navigator.
In a systematic review of conceptual frameworks to inform medical complexity, Zullig and colleagues10 stated that “contextual factors, including interpersonal, organization, and community factors, may drive complexity for patients and moderate the association between complexity and outcomes.” The authors noted the potential interaction between contextual factors and cultural and language barriers, which may influence healthcare quality.
4. Relationship Between Distress and Acuity
Fourteen (13.3%) of 105 articles evaluated the relationship between distress and acuity. Two studies found that emotional distress was strongly associated with compromised performance status in cancer patients.54,55 However, in an adjusted analysis, Barry and colleagues13 found that even low-acuity patients, especially those who were unemployed or disabled, are at risk for distress. Johnson and colleagues15 noted that younger patients may be more vulnerable to distress due to added developmental stress (eg, starting a family, completing education, postponing life goals). Kim and colleagues54 had similar findings that showed the effects of emotional distress on performance decline were increased in younger patients (<45 years) compared with older patients (>65 years).
Examples of major sources of distress for oncology patients include practical, family, emotional, spiritual, and physical problems56 such as pain, balance/mobility issues, and fatigue.57 There is evidence in the literature to suggest that distressed patients tax the healthcare system and utilize services at a higher rate than nondistressed patients.15 However, somewhat surprisingly, a more recent study also found that patients with more severe melanomas required significantly less psycho-oncologic support than those with less severe melanomas.58
Distress levels seem to stem from personality factors such as resilience and trait anxiety, and both Harding14 and VanHoose and colleagues59 found that trait anxiety/worry was the strongest predictor of distress. Fortunately, patients have been found to report fewer symptoms of distress after just 3 or 4 visits with a navigator.60
Warmenhoven and colleagues61 found that depression in palliative care patients is associated with poor outcomes in the palliation of physical symptoms, treatment adherence, and prognosis. De La Cruz and colleagues31 examined the impact of depression on the intensity of patient navigation. Due to higher utilization of healthcare services generally needed for depression, the authors reported that this condition could require additional navigation support to improve outcomes. Although linked to distress, depression was not found to change navigation time in women.30
Evidence also suggests that a higher cancer stage or more functional impairment is associated with higher spousal distress and therefore poorer work productivity.62 Lastly, studies of different distress measures have found that scores on the Behavioral Health Status Index and the Distress Thermometer are highly correlated63; however, distress scales also seem to be highly correlated with physical symptoms burden,61 suggesting that current tools may not actually be good measures of psychological distress.
5. Existing Acuity Tools
Twenty-two (21.0%) of 105 articles evaluated existing acuity tools. Three articles were published before 2008 and were outside the dates covered by the search. Shaha and Bush5 stressed the value of classification to be “most valid and reliable when its main or sole purpose is to describe the relative intensity of patients.” In 2006, Balstad and Springer64 appeared to be the first to indicate the need for a tool that measures patient acuity in the hospital nursing case management setting and the importance of capturing the variability that exists within patient demands in nursing care. Huber and Craig4 introduced the concept of the outcome of patient management (navigation) with the greater impact on patients with large acuity differential.
Since then, several oncology acuity tools have been reported, including:
- Mitchell Cancer Institute’s oncology nurse navigation acuity tool65
- Billings Clinic’s patient navigation acuity scale66
- Oncology Acuity Tool67
- Acuity Scale for Oncology Outpatient Infusion Room68
- Cleveland Clinic Cancer Center’s Medical
- Oncology Acuity of Care Rating System69
- Lehigh Valley Health Network’s acuity scale70
- Patient Navigator Acuity Tool71
- Acuity-based staffing tool for chemotherapy
- infusion department72
- Warren Grant Magnuson Clinical Center’s patient intensity tool73
In their acuity-based staffing tool, Vortherms and colleagues72 provided a worksheet for assignment of patient acuity points, specifying acuity criterion and predetermined maximum acuity points.
In addition, the following nononcology-specific tools have been reported:
- Patient Acuity Case Management Evaluation Tool4,64
- BluCuity Scale74
- Caseload Intensity Tool75
- Patient Classification System76
- Kilgore Heart Failure Case Management Acuity Tool77
- Permanente Online Interactive Network Tool78
- Intermountain Health Care’s acuity tool5
- Association of UK University Hospitals’ tool79
- Patient Centred Assessment Method80
6. Factors Related to Acuity
Thirty-one (29.5%) of 105 articles evaluated factors related to acuity such as productivity, ROI, staffing/caseload, effectiveness, and time management. One article outside the dates covered by the search contributed concepts of outcomes that are related to changes case managers make in their clients’ care. Huber and Craig4 developed groundwork showing that acuity differentials had a more direct relationship with actual care management activities than did the outcome measures such as ROI, hours billed, case life, and savings. Typically, as the number of barriers to care increases for a patient, so does the patient’s acuity score.81 Both barriers and acuity tend to be positively correlated with navigation time,81 suggesting that high-acuity patients used more resources per patient than low- or medium-acuity patients.65 Patient severity or condition instability has also been associated with the need for more intensive therapies, monitoring, and interventions.67 This evidence suggests that determining patient acuity is the best way to identify optimal patient caseloads for navigators, and that navigators who have patients with a higher acuity level should ideally have a lesser volume of patients.82
According to the American Nurses Association, an unanticipated outcome of implementing a patient classification and acuity system is the multidisciplinary collaboration involved and the opportunities resulting from this process.11 Chapman and colleagues83 underscore the importance of developing an acuity tool for community nursing in the context of its vital role in helping patients remain independent and manage their long-term conditions in conjunction with person-centered, preventive, and coordinated care. Although staffing models that consider a patient’s condition, severity, or acuity require evaluation of these factors throughout the day to be implemented,84 acuity-based systems can, in the long run, help hospitals use existing staff more efficiently.69,85,86 One example of a way to estimate workload is to multiply the volume of tumor by the patient’s acuity level.66
Several important factors need to be considered when determining nurse caseload, including a patient’s physical care requirements, health educational needs, psychosocial needs, and social support.87,88 Johnson and colleagues15 as well as Kim and colleagues54 noted that younger individuals’ distress is high due to family issues, whereas older individuals’ distress is due to decline in mobility. Nurse competency can also make a difference when it comes to staff assignment decisions.89 Currently, there are quite a few classification-based nurse staffing tools for caseload described in the literature.
Baldwin and Jones65 describe 11 factors of the Mitchell Cancer Institute Oncology Nurse Navigation Acuity Tool that influence acuity: (1) staging at diagnosis; (2) receiving multiple treatment modalities; (3) type of chemotherapy (multiagent vs single agent vs oral agents); (4) treatment status (new vs active treatment); (5) Eastern Cooperative Oncology Group performance status; (6) comorbidities; (7) hospitalizations; (8) colostomy, ileostomy, tracheostomy, feeding tube; (9) noncompliance with treatment; (10) family support; and (11) Patient Health Questionnaire 2/9 depression screening.
Mascarenhas and colleagues90 examined the correlation between caseload and acuity to determine if there were potential factors affecting productivity in oncology nurse navigation. The authors observed that head and neck and genitourinary patients presented the highest average acuity with the lowest caseload.90 Additionally, Willhite81 found that barriers and acuity scores correlated with navigation time, whereas distress scores did not show this correlation. O’Keeffe91 elaborated on the psychosocial component of patient-related factors affecting nurse workload in terms of nursing tasks related to monitoring and intervention correlating with mental disabilities, end-of-life care, palliative care, and including personal and family dynamics. Lastly, in an analysis of resource use and Medicare costs during lay navigation for geriatric patients with cancer, Rocque and colleagues92 found that supportive care interventions decrease acuity.
7. AONN+ Standardized Metrics and Patient Acuity Measures
Seven (6.7%) of 105 articles helped to evaluate the level of support in the literature to demonstrate whether any of the AONN+ Standardized Metrics are patient acuity measures. The AONN+ Standardized Metrics include 35 evidence-based oncology metrics used to measure the impact of patient navigation programs based on patient experience, clinical outcomes, and ROI.93
The ultimate goal of cancer navigation programs is to provide high-quality care with improved clinical outcomes and a high ROI.93 Metrics are used to evaluate the success of a navigation program and can include assessments of patient experience, clinical outcomes, and business performance.94 Additionally, treatment adherence, barriers to treatment, and patient satisfaction with care and navigation services are also important patient-related outcome measures for navigation services.95 Research suggests that patient navigation metric domains include measures of quality of life, satisfaction with care, social support, distress, and caregiver burden.90 Palos and Hare96 discuss navigation metrics to measure patient and/or caregiver outcomes that were agreed upon at the American Cancer Society’s National Leadership Summit. Patient navigation metric domains were: (1) quality of life, (2) satisfaction with care, (3) social support, (4) distress, and (5) caregiver burden.
The 35 metrics of patient navigation have only recently been identified, and more research needs to be done to evaluate if and how they relate to patient acuity. Nevertheless, previous studies of patient navigation programs have found that a more advanced stage of cancer at initial diagnosis predicted shorter times to consultation97 and that physical symptoms, psychological distress, and depression symptoms are associated with longer hospital stays, whereas physical and anxiety symptoms are associated with a higher likelihood for readmission within 90 days.98 Lastly, it has also been found that health centers with higher proportions of poor patients had smaller caseload sizes, suggesting that poorer patients generate a higher workload for doctors, most likely due to their more significant comorbidity profile.99
Discussion
Limitations
As described in Table 2, the included articles presented several limitations for the scoping review. These limitations need to be thoroughly considered in the development of an acuity tool that can maximize the effectiveness and ROI of oncology patient navigation programs.
Key Findings
In summary, our database search strategy yielded 1711 records from which 199 full-text articles were reviewed and narrowed down to 105 relevant articles for inclusion in this scoping review. Findings from our review and analysis of relevant articles indicate a high level of variability and complexity in how acuity and its related factors are defined and determined. There is a lack of consensus on the definition of acuity, and no standard categorization of barriers to care exists. The relationships between barriers to care and acuity and between distress and acuity have not been clearly established. Existing acuity tools present additional shortcomings in their application to an oncology patient navigation-specific tool. The current literature also fails to provide sufficient support to demonstrate whether any of the AONN+ Standardized Metrics are patient acuity measures.
Implications for Practice
The learning outcomes from this scoping review will help to inform the development of an oncology patient navigation-specific acuity tool. When finalized, the acuity tool will be used to help oncology navigators characterize the intensity of patient navigation workload, aid in the allocation of resources, and measure the effectiveness of navigation on patient outcomes. The acuity tool will support and enhance oncology navigators’ effectiveness through patient-centric evidence-based methods that may potentially decrease the overall cost of care.
Conclusions
The importance of acuity tools and their potential to improve patient outcomes are well recognized. Nevertheless, the results of this scoping review demonstrate a continuing need for additional research to better understand how oncology navigation acuity is defined and determined. Further study is also required to evaluate how AONN+ Standardized Metrics perform as patient acuity measures. Addressing these gaps will facilitate the development of an acuity tool to optimize the effectiveness of oncology patient navigator programs.
Acknowledgments
AONN+ gratefully acknowledges Astellas US, LLC, for its collaboration on the Oncology Navigation Acuity Initiative. The Acuity Tool may be used to help oncology navigators characterize the intensity of patient navigation workload, aid in the allocation of resources, and measure the effectiveness of navigation on patient outcomes. This initiative is intended to support and enhance oncology navigators’ effectiveness through patient-centric evidence-based methods that may have the potential to decrease the overall cost of care. The authors would also like to acknowledge the Acuity Committee members for their expertise, dedication, and time on this very important project: Cheryl Bellomo, MSN, RN, OCN, ONN-CG; Nicole Erb; Barbara Hale, MSW, LCSW; Rita Kristy, MS; Rani Khetarpal; Wendy Latash, PhD; Nicole Messier, BSN, RN, OCN; Colleen Sullivan-Moore, RN, MS; and Lianna Willhite, BSN, RN, ONN-CG, CBCN.
Disclosures
Rita Kristy, MS, and Wendy Latash, PhD, are employees of Astellas US, LLC.
References
- O’Keeffe M. Acuity-adjusted staffing: a proven strategy to optimize patient care. American Nurse Today. 2016;11(3):28-34.
- Peters M, Godfrey C, McInerney P, et al. The Joanna Briggs Institute Reviewers’ Manual 2015: Methodology for JBI Scoping Reviews. Adelaide, SA Australia: The Joanna Briggs Institute; 2015.
- Liberati A, Altman DG, Tetzlaff J, et al. The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate health care interventions: explanation and elaboration. PLoS Med. 2009;6:e1000100.
- Huber DL, Craig K. Acuity and case management: a healthy dose of outcomes, part I. Prof Case Manag. 2007;12:132-144.
- Shaha SH, Bush C. Fixing acuity: a professional approach to patient classification and staffing. Nurs Econ. 1996;14:346-356.
- Zimmermann C, Burman D, Bandukwala S, et al. Nurse and physician inter-rater agreement of three performance status measures in palliative care outpatients. Support Care Cancer. 2010;18:609-616.
- Alghamdi MG. Nursing workload: a concept analysis. J Nurs Manag. 2016;24:449-457.
- Brennan CW, Daly BJ. Patient acuity: a concept analysis. J Adv Nurs. 2009;65:1114-1126.
- Brennan CW, Daly BJ. Methodological challenges of validating a clinical decision-making tool in the practice environment. West J Nurs Res. 2015;37:536-545.
- Zullig LL, Whitson HE, Hastings SN, et al. A systematic review of conceptual frameworks of medical complexity and new model development. J Gen Intern Med. 2016;31:329-337.
- American Nurses Association. Defining Staffing: Workforce Management. Patient Classification and Acuity Systems. The Request for Proposal Process. www.nursingworld.org/~497e37/globalassets/practiceandpolicy/work-environment/nurse-staffing/website-staffing-and-acuity-systems-pdf-final_2017.pdf.
- Carrillo JE, Carrillo VA, Perez HR, et al. Defining and targeting health care access barriers. J Health Care Poor Underserved. 2011;22:562-575.
- Barry V, Lynch ME, Tran DQ, et al. Distress in patients with bleeding disorders: a single institutional cross-sectional study. Haemophilia. 2015;21:e456-e464.
- Harding MM. Incidence of distress and associated factors in women undergoing breast diagnostic evaluation. West J Nurs Res. 2014;36:475-494.
- Johnson RL, Larson C, Black LL, et al. Significance of nonphysical predictors of distress in cancer survivors. Clin J Oncol Nurs. 2016; 20:E112-E117.
- Ma X, Zhang J, Zhong W, et al. The diagnostic role of a short screening tool—the distress thermometer: a meta-analysis. Support Care Cancer. 2014;22:1741-1755.
- National Comprehensive Cancer Network. NCCN Clinical Practice Guidelines in Oncology (NCCN Guidelines. Distress Management. Version 2.2013. 2013.
- National Comprehensive Cancer Network. NCCN Guidelines for Patients. Distress. Version 1.2017. www.nccn.org/patients/guidelines/distress/index.html#462017. 2017.
- National Institutes of Health. National Cancer Institute. NCI Dictionary of Cancer Terms. Distress. www.cancer.gov/publications/dictionaries/cancer-terms.
- Vitek L, Rosenzweig MQ, Stollings S. Distress in patients with cancer: definition, assessment, and suggested interventions. Clin J Oncol Nurs. 2007;11:413-418.
- Boehmer U. LGBT populations’ barriers to cancer care. Semin Oncol Nurs. 2018;34:21-29.
- Bourdeanu L, Luu T, Baker N, et al. Barriers to treatment in patients with locally advanced breast cancer. J Natl Compr Canc Netw. 2013;11: 1193-1198.
- Katz ML, Young GS, Reiter PL, et al. Barriers reported among patients with breast and cervical abnormalities in the patient navigation research program: impact on timely care. Womens Health Issues. 2014;24:e155-e162.
- Murphy MM, Tseng JF, Shah SA. Disparities in cancer care: an operative perspective. Surgery. 2010;147:733-737.
- Post DM, McAlearney AS, Young GS, et al. Effects of patient navigation on patient satisfaction outcomes. J Cancer Educ. 2015;30:728-735.
- Guadagnolo BA, Cina K, Helbig P, et al. Medical mistrust and less satisfaction with health care among Native Americans presenting for cancer treatment. J Health Care Poor Underserved. 2009;20:210-226.
- Campbell C, Craig J, Eggert J, Bailey-Dorton C. Implementing and measuring the impact of patient navigation at a comprehensive community cancer center. Oncol Nurs Forum. 2010;37:61-68.
- Becze E. Patient and nursing aspects of oncology navigation. ONS Connect. 2011;26:14-15.
- Freeman HP. The history, principles, and future of patient navigation: commentary. Semin Oncol Nurs. 2013;29:72-75.
- Chambers SK, Hyde MK. Underserved groups and barriers to cancer care. Eur J Cancer Care (Engl). 2015;24:1-3.
- De La Cruz II, Freund KM, Battaglia TA, et al. Impact of depression on the intensity of patient navigation for women with abnormal cancer screenings. J Health Care Poor Underserved. 2014;25:383-395.
- Grimes C, Dankovchik J, Cahn M, Warren-Mears V. American Indian and Alaska Native cancer patients’ perceptions of a culturally specific patient navigator program. J Prim Prev. 2017;38:121-135.
- Itty TL, Hodge FS, Martinez F. Shared and unshared barriers to cancer symptom management among urban and rural American Indians. J Rural Health. 2014;30:206-213.
- Lim JW. Barriers to cancer care, perceived social support, and patient navigation services for Korean breast cancer patients. Soc Work Health Care. 2015;54:47-64.
- Madore S, Kilbourn K, Valverde P, et al. Feasibility of a psychosocial and patient navigation intervention to improve access to treatment among underserved breast cancer patients. Support Care Cancer. 2014;22:2085-2093.
- Esparza A. Patient navigation and the American Cancer Society. Semin Oncol Nurs. 2013;29:91-96.
- Goss E, Lopez AM, Brown CL, et al. American Society of Clinical Oncology policy statement: disparities in cancer care. J Clin Oncol. 2009;27:2881-2885.
- Korber SF, Padula C, Gray J, Powell M. A breast navigator program: barriers, enhancers, and nursing interventions. Oncol Nurs Forum. 2011;38:44-50.
- Ramachandran A, Snyder FR, Katz ML, et al. Barriers to health care contribute to delays in follow-up among women with abnormal cancer screening: data from the Patient Navigation Research Program. Cancer. 2015;121:4016-4024.
- Tejeda S, Darnell JS, Cho YI, et al. Patient barriers to follow-up care for breast and cervical cancer abnormalities. J Womens Health (Larchmt). 2013;22:507-517.
- Walsh J, Harrison JD, Young JM, et al. What are the current barriers to effective cancer care coordination? A qualitative study. BMC Health Serv Res. 2010;10:132.
- Palomino H, Peacher D, Ko E, et al. Barriers and challenges of cancer patients and their experience with patient navigators in the rural US/Mexico border region. J Cancer Educ. 2017;32:112-118.
- Pati S, Hussain MA, Chauhan AS, et al. Patient navigation pathway and barriers to treatment seeking in cancer in India: a qualitative inquiry. Cancer Epidemiol. 2013;37:973-978.
- Sawchuk CN, Van Dyke E, Omidpanah A, et al. Caregiving among American Indians and Alaska Natives with cancer. Support Care Cancer. 2015;23:1607-1614.
- Sprague Martinez L, Freeman ER, Winkfield KM. Perceptions of cancer care and clinical trials in the black community: implications for care coordination between oncology and primary care teams. Oncologist. 2017;22:1094-1101.
- Thomson MD, Siminoff LA. Finding medical care for colorectal cancer symptoms: experiences among those facing financial barriers. Health Educ Behav. 2015;42:46-54.
- Pratt-Chapman M, Simon MA, Patterson AK, et al. Survivorship navigation outcome measures: a report from the ACS patient navigation working group on survivorship navigation. Cancer. 2011;117(15 Suppl):3575-3584.
- Alamanda VK, Song Y, Holt GE. Effect of marital status on treatment and survival of extremity soft tissue sarcoma. Ann Oncol. 2014;25:725-729.
- Hendren S, Chin N, Fisher S, et al. Patients’ barriers to receipt of cancer care, and factors associated with needing more assistance from a patient navigator. J Natl Med Assoc. 2011;103:701-710.
- Jones LA, Ferrans CE, Polite BN, et al. Examining racial disparities in colon cancer clinical delay in the Colon Cancer Patterns of Care in Chicago study. Ann Epidemiol. 2017;27:731-738.
- Allison AL, Ishihara-Wong DD, Domingo JB, et al. Helping cancer patients across the care continuum: the navigation program at the Queen’s Medical Center. Hawaii J Med Public Health. 2013;72:116-121.
- Carroll JK, Winters PC, Purnell JQ, et al. Do navigators’ estimates of navigation intensity predict navigation time for cancer care? J Cancer Educ. 2011;26:761-766.
- Lin CJ, Schwaderer KA, Morgenlander KH, et al. Factors associated with patient navigators’ time spent on reducing barriers to cancer treatment. J Natl Med Assoc. 2008;100:1290-1297.
- Kim JH, Yoon S, Won WY, et al. Age-specific influences of emotional distress on performance status in cancer patients. Psychooncology. 2013;22:2220-2226.
- Rocque GB, Williams CP, Jones MI, et al. Healthcare utilization, Medicare spending, and sources of patient distress identified during implementation of a lay navigation program for older patients with breast cancer. Breast Cancer Res Treat. 2018;167:215-223.
- Tonsing KN, Vungkhanching M. Assessing psychological distress in cancer patients: the use of distress thermometer in an outpatient cancer/hematology treatment center. Soc Work Health Care. 2018;57:126-136.
- Rocque GB, Taylor RA, Acemgil A, et al. Guiding lay navigation in geriatric patients with cancer using a distress assessment tool. J Natl Compr Canc Netw. 2016;14:407-414.
- Nolte S, van der Mei SH, Strehl-Schwarz K, et al. Comparison of patient-reported need of psycho-oncologic support and the doctor’s perspective: how do they relate to disease severity in melanoma patients? Psychooncology. 2016;25:1271-1277.
- VanHoose L, Black LL, Doty K, et al. An analysis of the distress thermometer problem list and distress in patients with cancer. Support Care Cancer. 2015;23:1225-1232.
- Swanson J, Koch L. The role of the oncology nurse navigator in distress management of adult inpatients with cancer: a retrospective study. Oncol Nurs Forum. 2010;37:69-76.
- Warmenhoven F, van Weel C, Vissers K, Prins J. Screening instruments for depression in advanced cancer patients: what do we actually measure? Pain Pract. 2013;13:467-475.
- Manne SL, Siegel S, Heckman CJ, Kashy DA. Psychological distress as a mediator of the association between disease severity and occupational functioning among employed spouses of women recently diagnosed with breast cancer. Psychooncology. 2015;24:1560-1568.
- Cutillo A, O’Hea E, Person S, et al. The distress thermometer: cutoff points and clinical use. Oncol Nurs Forum. 2017;44:329-336.
- Balstad A, Springer P. Quantifying case management workloads: development of the PACE tool. Lippincotts Case Manag. 2006;11:291-302; quiz 303-304.
- Baldwin D, Jones M. Developing an acuity tool to optimize nurse navigation caseloads. Oncology Issues. 2018;33(2):17-25.
- Blaseg K. Patient navigation at Billings Clinic: an NCI Community Cancer Centers Program (NCCCP) pilot site. www.accc-cancer.org/docs/projects/resources/pdf/patientnavigation-guide/s15.pdf?sfvrsn=875c3b1 0_0. 2009.
- Brennan CW, Daly BJ, Dawson NV, et al. The oncology acuity tool: a reliable, valid method for measuring patient acuity for nurse assignment decisions. J Nurs Meas. 2012;20:155-185.
- DeLisle J. Designing an acuity tool for an ambulatory oncology setting. Clin J Oncol Nurs. 2009;13:45-50.
- Hawley E, Carter NG. An acuity rating system for infusion center nurse staffing. Oncology Issues. 2009;24(6):34-37.
- Roman R, Beaupre L. Development and utilization of an acuity scale for oncology patient navigation. Journal of Oncology Navigation & Survivorship. Abstract. www.jons-online.com/issues/2014/august-2014-vol-5-no-4/1277-category-iv-original-research-on-navigation-programs-august-2014.
- Sullivan-Moore C, Cook C. Patient Navigator Acuity Tool. National Consortium of Breast Centers. http://files.ctctcdn.com/b59f4183201/ 350b2d96-b1a0-44e9-a585-76207345dbbb.pdf. 2015.
- Vortherms J, Spoden B, Wilcken J. From evidence to practice: developing an outpatient acuity-based staffing model. Clin J Oncol Nurs. 2015;19:332-337.
- West S, Sherer M. ISO: The “right” nurse staffing model. Oncology Issues. 2009;24(6):26-30.
- Craig K, Flaherty-Quemere A. Implementing an automated acuity tool for scoring case management cases and caseloads at Blue Cross Blue Shield of Massachusetts. Prof Case Manag. 2009;14:185-191.
- Collister B, Slauenwhite CA, Fraser KD, et al. Measuring home care caseloads: development of the Caseload Intensity Tool. Home Health Care Management & Practice. 2014;26:239-249.
- Harper K, McCully C. Acuity systems dialogue and patient classification system essentials. Nurs Adm Q. 2007;31:284-299.
- Kilgore MD. An acuity tool for heart failure case management: quantifying workload, service utilization, and disease severity. Prof Case Manag. 2018;23:130-138.
- Potts B, Adams R, Spadin M. Sustaining primary care practice: a model to calculate disease burden and adjust panel size. Perm J. 2011;15:53-56.
- Smith J, Forde V, Goodman M, et al. How to keep score of acuity and dependency. Nurs Manag (Harrow). 2009;16:14, 16-19.
- Yoshida S, Matsushima M, Wakabayashi H, et al. Validity and reliability of the Patient Centred Assessment Method for patient complexity and relationship with hospital length of stay: a prospective cohort study. BMJ Open. 2017;7:e016175.
- Willhite L. Navigation acuity. Journal of Oncology Navigation & Survivorship. 2018;9(11):473. Abstract.
- Catholic Health Initiatives. Navigation Program Resource Guide: Best Practices for Patient Navigation Programs. https://mdpnn.files.wordpress.com/2013/04/chi-navigation-program-resource-guide-_final-012013_.pdf. 2013.
- Chapman H, Kilner M, Matthews R, et al. Developing a caseload classification tool for community nursing. Br J Community Nurs. 2017;22: 192-196.
- American Nurses Association. Optimal Nurse Staffing to Improve Quality of Care and Patient Outcomes: Executive Summary. https://cdn.ymaws.com/www.anamass.org/resource/resmgr/docs/NurseStaffingWhitePaper.pdf. 2015.
- Huber DL, Craig K. Acuity and case management: a healthy dose of outcomes, part III. Prof Case Manag. 2007;12:254-271.
- Liang B, Turkcan A. Acuity-based nurse assignment and patient scheduling in oncology clinics. Health Care Manag Sci. 2016;19:207-226.
- Brady AM, Byrne G, Horan P, et al. Reliability and validity of the CCNCS: a dependency workload measurement system. J Clin Nurs. 2008;17:1351-1360.
- Martin-Misener R, Kilpatrick K, Donald F, et al. Nurse practitioner caseload in primary health care: scoping review. Int J Nurs Stud. 2016;62:170-182.
- Young J, Lee M, Sands LP, McComb S. Nursing activities and factors influential to nurse staffing decision-making. Journal of Hospital Administration. 2015;4(4):24-31.
- Mascarenhas D, Passwater C, Koutlas J, et al. Oncology nurse navigation: examining a correlation between caseload and acuity. Oncology Nursing Society Annual Congress. 2018. Washington, DC. https://ons.confex.com/ons/2018/meetingapp.cgi/Paper/2622.
- O’Keeffe M. Practical steps for applying acuity-based staffing. American Nurse Today. 2016;11(9):30-34.
- Rocque GB, Pisu M, Jackson BE, et al. Resource use and Medicare costs during lay navigation for geriatric patients with cancer. JAMA Oncol. 2017;3:817-825.
- Strusowski T, Johnston D. AONN+ evidence-based oncology navigation metrics crosswalk with national oncology standards and indicators. Journal of Oncology Navigation & Survivorship. 2018;9(6):214-221.
- Sein E, Johnston D, Strusowski T, Bellomo C. Measuring the impact navigation has on patient care by supporting the multidisciplinary team. In: Shockney LD, ed. Team-Based Oncology Care: The Pivotal Role of Oncology Navigation. Cham, Switzerland: Springer International Publishing; 2018.
- Fiscella K, Ransom S, Jean-Pierre P, et al. Patient-reported outcome measures suitable to assessment of patient navigation. Cancer. 2011;117(15 Suppl):3603-3617.
- Palos GR, Hare M. Patients, family caregivers, and patient navigators: a partnership approach. Cancer. 2011;117(15 Suppl):3592-3602.
- Basu M, Linebarger J, Gabram SG, et al. The effect of nurse navigation on timeliness of breast cancer care at an academic comprehensive cancer center. Cancer. 2013;119:2524-2531.
- Nipp RD, El-Jawahri A, Moran SM, et al. The relationship between physical and psychological symptoms and health care utilization in hospitalized patients with advanced cancer. Cancer. 2017;123:4720-4727.
- Muldoon L, Rayner J, Dahrouge S. Patient poverty and workload in primary care: study of prescription drug benefit recipients in community health centres. Can Fam Physician. 2013;59:384-390.
- Craig K, Huber DL. Acuity and case management: a healthy dose of outcomes, part II. Prof Case Manag. 2007;12:199-212.
- Bagshaw SM, Opgenorth D, Potestio M, et al. Healthcare provider perceptions of causes and consequences of ICU capacity strain in a large publicly funded integrated health region: a qualitative study. Crit Care Med. 2017;45:e347-e356.
- Good MJ, Hurley P, Woo KM, et al. Assessing clinical trial-associated workload in community-based research programs using the ASCO Clinical Trial Workload Assessment Tool. J Oncol Pract. 2016;12:e536-e547.
- Kraljic S, Zuvic M, Desa K, et al. Evaluation of nurses’ workload in intensive care unit of a tertiary care university hospital in relation to the patients’ severity of illness: a prospective study. Int J Nurs Stud. 2017; 76:100-105.
- Fasoli DR, Fincke BG, Haddock KS. Going beyond patient classification systems to create an evidence-based staffing methodology. J Nurs Adm. 2011;41:434-439.
- Jennings BM. Patient Acuity. In: Hughes RG, ed. Patient Safety and Quality: An Evidence-Based Handbook for Nurses. Rockville, MD: Agency for Healthcare Research and Quality; March 2008.
- Tuna R, Baykal U, Turkmen E, Yildirim A. Planning for the size of the nursing staff at an outpatient chemotherapy unit. Clin J Oncol Nurs. 2015;19:E115-E120.
- Choi J, Choi JE, Fucile JM. Power up your staffing model with patient acuity. Nurs Manage. 2011;42:40-43.
- High B. Preliminary data on patient acuity scores used as drivers of navigation activity and as a measurement of navigation effectiveness. Journal of Oncology Navigation & Survivorship. 2018;9(11):475-476. Abstract.
- Cunningham JJ. New system to manage nurses’ workloads: optimizing patient care at Walter Reed. Defense AT&L. 2018;Jan-Feb:22-26.
- Sullivan-Moore C, Everett K, Grieg M, Lopez J. To explore benefits of patient navigator tool to measure job responsibilities. Journal of Oncology Navigation & Survivorship. 2018;9(11):468. Abstract.