The Norma F. Pfriem Breast Care Center (NPBCC) is a comprehensive breast care center, providing screening, diagnosis, treatment, outreach, and supportive services. The center serves Connecticut’s southern Fairfield County, including the low-income community of Bridgeport, a city of more than 139,000 residents, with over 21% living in poverty. Bridgeport is almost 70% minority, split nearly evenly between Hispanics (33.5%) and African Americans (34.8%).1 About 43% of residents speak a language other than English at home.1
Connecticut has the second highest rate of new breast cancer cases in the nation and the twelfth highest death rate in the nation (with higher death rates for African American women).2 Nearly one-third of breast cancers in Connecticut are detected at later stages, after some metastasis has occurred.2
Within the NPBCC’s service areas, the statistics are even more troubling. The city of Bridgeport is characterized by high stage IV breast cancer diagnoses, high breast cancer incidence, and above-average breast cancer mortality.3 In addition, Bridgeport has one of the highest risks for death from breast cancer in the state (30.1 per 100,000, well above the state average of 23.9).4
For the last 10 years, the Breast Care Center’s community-based outreach program has helped low-income and medically underserved women understand the importance of screening to detect breast cancer at an early stage. The program has also taught women how to access free mammograms and other screening and diagnostic procedures (at the NPBCC and elsewhere) and where to find support and counseling services in their local community.
The NPBCC provides the largest outreach program of its kind in the area, reaching over 2500 women each year. Nurse educators participate in programs at churches, places of employment, community centers and agencies, clinics, health fairs and other neighborhood fairs, community colleges, and senior housing.
A COMMUNITY AT RISK
Several risk factors converge in Bridgeport to create a community at increased risk of breast cancer. Lack of adequate health insurance is common. In Connecticut, Hispanics are 5.4 times more likely—and blacks 2.7 times more likely— than whites not to have health insurance.5 This leaves 40% of Connecticut’s Hispanic community uninsured.6 The uninsured and Medicaid recipients are more likely to be diagnosed with cancer at a later stage compared to those with health insurance.2 People from lower social classes are also less likely to receive cancer screenings, and their survival rates are lower, even when they have healthcare coverage.2
Health disparities also play a part. African American women across all age groups are more likely to die from breast cancer.7 This disparity, now at 37%, continues to grow, according to a recent report from the American Cancer Society. With the African American population at over 30%, the impact in Bridgeport is enormous. Finally is the question of sheer numbers. The Latino population is growing in Bridgeport as it is across the nation, where it is expected to triple by 2050. With that growth will come a rise in the number of Latinas with breast cancer, according to Lydia Buki, PhD, a professor of community health at the University of Illinois, who has studied incidence and mortality rates for breast and other cancers among Latinas.8
Breast cancer, she notes, is the most common cancer afflicting Latinas in the United States, and the 5-year survivorship rate for Latinas is lower than for non- Latina whites.8 Latinos are more likely than non- Latino whites to present with larger tumors or at more advanced stages of disease.8 Further, researchers from the Arizona Cancer Center and MD Anderson Cancer Center have found that breast cancer appears to be occurring at an earlier age among Hispanics, something we have observed at the NPBCC.9
Raising awareness is critical to serving this growing community and detecting breast cancer early, when it is more treatable. “[The issue] is women knowing the importance [of cancer screening], and at the same time being able to access information and screening services,” according to Dr Buki.8
CHANGING TACTICS
While the NPBCC has been successful in reaching many underserved women through its outreach program, over the years it became clear there were some women—the very poorest, without English, distrustful of the healthcare system— who wouldn’t come to a health fair or other outreach program or follow up on a referral form, even under the best of circumstances. We saw a need to reach more deeply and aggressively into the community.
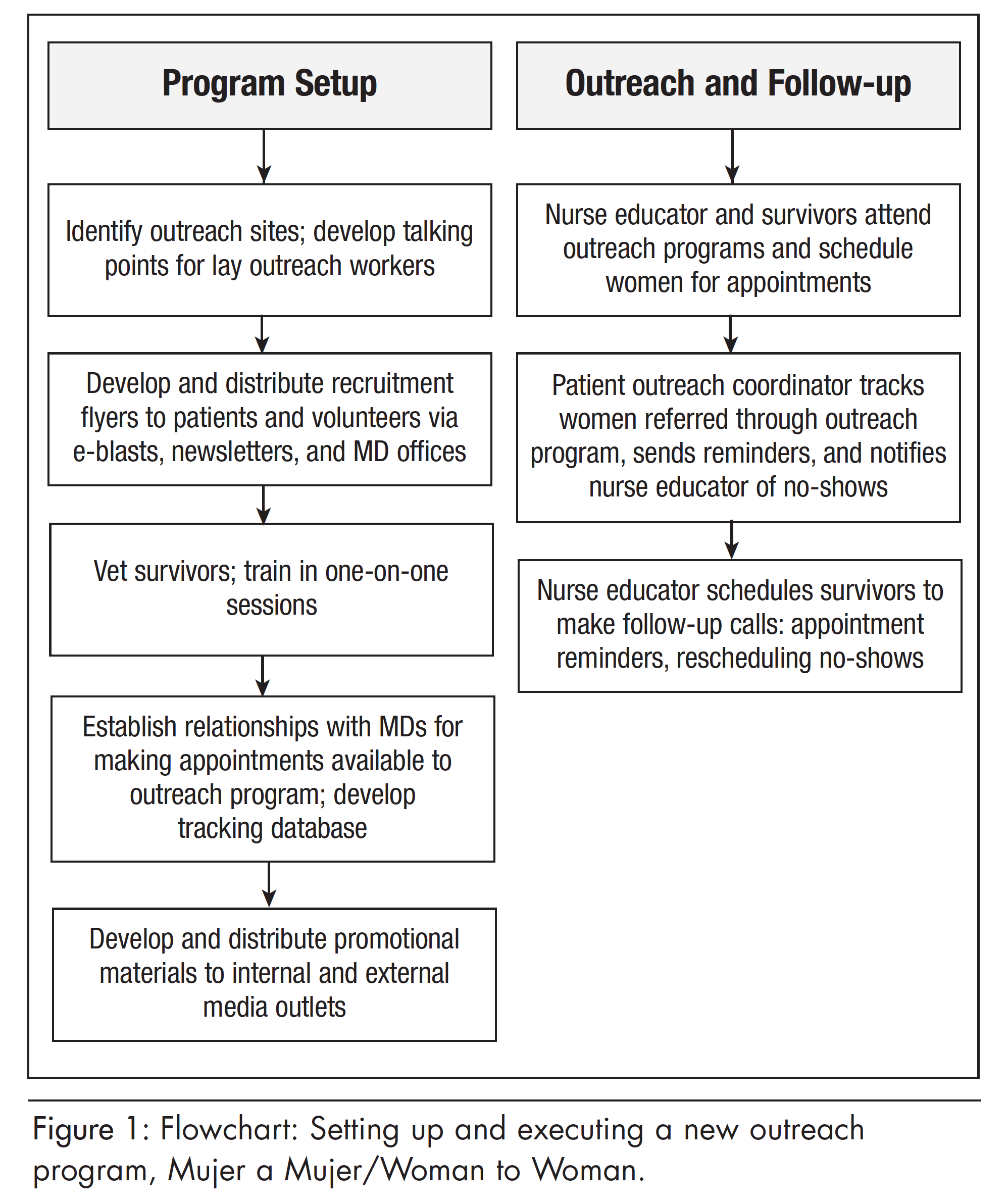
This paper will describe how we developed a new outreach program to connect with our most isolated clients using evidence-based outreach methods in a unique venue. Mujer a Mujer/ Woman to Woman trains bilingual cancer survivors as volunteer lay outreach workers to navigate women into screening. After the initial success of the bilingual outreach effort, the program became a regular fixture at a weekly food pantry to reach women in a medically underserved neighborhood. This paper will outline the process for setting up and executing the program (Figure 1) and establishing a presence at a unique venue to target the neediest. Initial results and program benefits will also be discussed, as well as lessons learned and plans for enhancing and expanding the program.
MUJER A MUJER/WOMAN TO WOMAN
In 2009, with a grant from the Avon Breast Care Foundation, the Breast Care Center began a new program, Mujer a Mujer/Woman to Woman. As part of the program, volunteer bilingual breast cancer survivors accompanied nurse educators at outreach programs. There was evidence to support making this change. Studies indicate that peer role models are effective in helping Latinas navigate the healthcare system to obtain exams.8,10 They are trusted sources of information, speak the same language, and know the culture. By discussing cancer, a topic not normally broached in traditional Latino culture, role models help to break down barriers to screening.
We scheduled community workshops at existing venues while adding other more creative settings, such as job training programs, parent groups, and outreach programs for the homeless, to create a multisite program tailored to the community, an approach that has been shown to increase participation in screening among Latinas.11 Initially, we identified breast cancer survivors from our existing pool of patients and volunteers and recruited some of them to join our nurse educators at our outreach programs.
Later, we created a flyer, in English and Spanish, to distribute to patients (in person and via e-mail) for recruitment purposes. Volunteers were offered a $50/day stipend plus $15/day for transportation. While the response was good, many respondents were not bilingual, lacked flexible schedules, or were looking for regular employment. In the end, we built our pool slowly, contacting women among our volunteers and patients who appeared to have the skills and flexibility to succeed as lay outreach workers.
The nurse educator wrote talking points, trained survivors individually as outreach workers, and attended outreach programs with survivors. To the public, there was no apparent difference between the professional and lay outreach worker, but the nurse could observe and listen and step in as necessary. Eventually survivors were able to attend outreach programs on their own.
The nurse secured a list of available appointment times from doctors at our clinic and used it to schedule women who expressed an interest. Later, the nurse negotiated the ability to call into the office for more time slots. Teaching materials included breast self-exam shower cards and patient education sheets. We created a program database to track clients and English/Spanish referral forms to distribute at events. The forms were coded by venue, so we could track referrals from the program events.
The foundation required us to track demographic information as well, using an anonymous client intake form (CIF). We promoted the program through our newsletter, patient e-mail list, ads in local newspapers—including Spanish-language papers—press releases, and The Norma F. Pfriem Breast Care Center’s Senior Nurse Navigator-Educator Sally Cascella (center) worked with Deacon Donald Foust (left), the administrator of Holy Rosary Church, to implement the outreach program. Web-based community calendars maintained by local media outlets, which resulted in several radio interviews during the morning news shows about the outreach program and breast health in general.
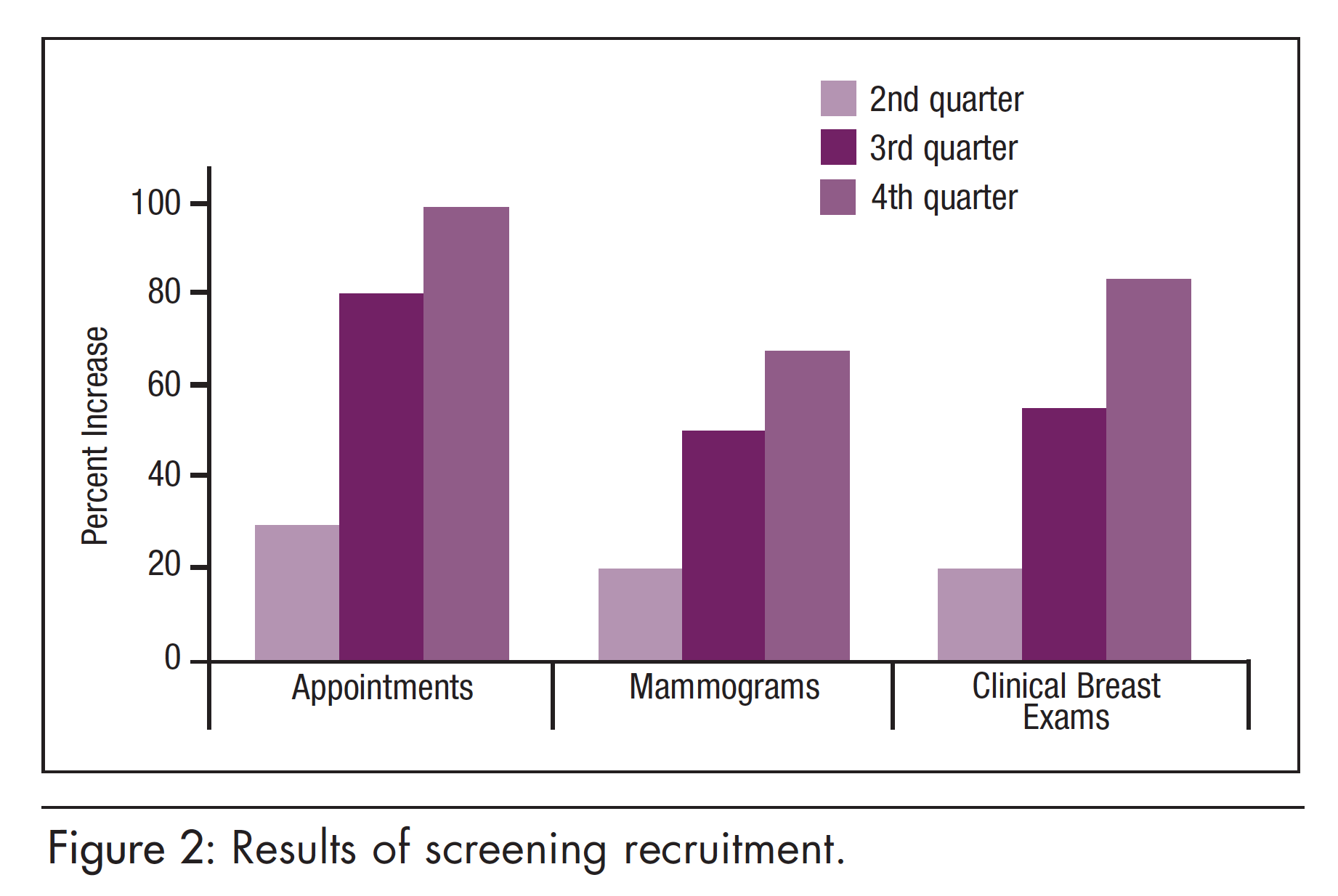
It quickly became clear that while the number of women we referred for appointments was increasing, only a small percentage were following up on their own. To increase participation, we began scheduling appointments while we engaged women in conversation at our outreach events rather than giving them the option of calling us. Staff began taking appointments with them, and this made a significant difference. Women were also offered a $15 cash card to a local grocery store if they scheduled an appointment, and we developed a contact sheet to accompany the CIFs so we could follow up with the women. Later, we gained the ability to call in for alternate appointment dates and times for women who couldn’t make available slots. Scheduled and completed appointments increased each quarter—mammograms increased by 36% and clinical breast exams by 37% from the second to the third quarter, and by 34% and 59%, respectively, from the third to the fourth quarter (Figure 2).
The no-show rate remained high and needed to be addressed. It had become clear that many women were scheduling appointments simply to get the grocery store cash card but were not following through. We changed our process; clients would receive a grocery store card only if they came in for their appointment. With many women below the poverty level, the cards proved to be a powerful incentive, much more so than other items we had tried in the past such as free cosmetics and jewelry, and use of the cards resulted in increased compliance. We also shifted follow- up to our volunteer breast cancer survivors because of their language skills.
Survivors called women before their appointments and followed up if they didn’t show. Although transportation within our urban location, including the availability of free rides through Medicaid, did not appear to be a factor preventing women from keeping their appointments, keeping in touch was often challenging. Because of their financial situations, our low-income clients move often. Many do not have phone service or lose phone service when their finances change. However, with the combination of our increased calling and the grocery store cards as incentives, many more women were completing their appointments. By the fourth quarter, our no-show rate had decreased by 23%.
Despite challenges in the beginning, by the end of the year we had developed an outreach program that navigated women into screening at the annual rate we had set for ourselves of 150.
FINDING THE NEEDIEST
Targeting the neediest for early detection required us to be creative. One neighborhood with a high incidence of late-stage diagnosis called out for our attention. The central/east area of Bridgeport is a low-income, medically underserved area designated as a primary care health professional shortage area.12 The population is primarily Hispanic. As in other areas of Bridgeport, women have difficulty navigating the healthcare system because of language and cultural barriers. As a result, many have not seen a doctor in years, nor are they likely to venture outside the neighborhood for healthcare. Many are without insurance because of a lack of awareness or misconceptions about public insurance. These were women with the greatest need, yet they were the least likely to come to an outreach program. And no outreach workers had gone to them.
A UNIQUE VENUE
With the help of a local church, the Holy Rosary Church in Bridgeport, we set up shop at their food pantry, believing we had a better chance of reaching women where they lived and at institutions they were sure to frequent. About 70 women from our target population came to the food pantry each week, including some who were homeless. Deacon Donald Foust, the church administrator, was an enthusiastic supporter. He explained, “By providing access to these important services, I believe we have the potential to save lives in a population that is in dire need of pre-ventive care.”
RESULTS
The program took place monthly, and we spoke to 35 women at our first event. After that, outreach workers spoke with 30 to 40 women each month. Women were scheduled for and completed appointments at a rate similar to our other outreach programs. About 30% were scheduled for mammograms, for many their first, and about 25% completed their appointments. Women with abnormal results received advanced diagnostic services. Women were tracked and followed at the Breast Care Center.
We also helped women without regular healthcare connect with a doctor. Patients met with a financial advocate who helped them access their benefits, including the Connecticut Breast and Cervical Cancer Early Detection Program and Medicaid. Spanish speakers were referred to a bilingual social worker.
The program has already saved lives. One 47- year-old woman, homeless and mentally ill, who had never had a mammogram, met with a nurse educator and a bilingual breast cancer survivor and signed up for a free mammogram. She was seen at the Breast Care Center’s clinic at Bridgeport Hospital and later learned she had been diagnosed with breast cancer. Now she is receiving treatment through the Breast Care Center without having to worry about medical bills or insurance. For this woman, the grocery store cards were a very meaningful incentive and key to getting her to complete her first and subsequent appointments. Although maintaining contact has been challenging, we continue to work with her through her treatment.
BRIDGING BARRIERS
Women overall were receptive to the breast cancer survivors as outreach workers. They were more likely to talk about breast health and share experiences with someone who had been through the breast cancer experience and who spoke their language, an important factor for many women we encountered. Many of their anxieties were lessened when they met these survivors and understood that breast cancer could be overcome.
Alicia, one of the bilingual breast cancer survivors who accompanied our outreach workers, reported that many of the women she encountered were surprised to find someone who could speak with them in Spanish. She also reported that many women had no idea when or how to examine themselves for breast cancer. Alicia was very open with women about her breast cancer journey. When they learned that her cancer was found during a routine mammogram, they understood the importance of an annual mammogram. It gave them hope when they met a survivor who was doing well and had returned to her life as it was before breast cancer.
Survivors and clients also bonded as women. At the East Side Senior Center in Bridgeport, Alicia met a 50-year-old woman who had not had a mammogram in 2 years. Alicia shared her story, and the conversation shifted to how, as women, they put others before themselves. The woman said she was inspired to make (and keep) her appointment and do something for herself.
During these conversations, there is also the opportunity for women to learn more about breast cancer, such as identifying risk factors they weren’t aware of. One woman with a family history of breast cancer came to a community health fair for a completely different issue, but when she saw our breast cancer survivor handing out information, made an appointment for a breast exam and mammogram. She said she had never thought about the importance of getting a baseline mammogram and being monitored at her age (she was in her late 30s) despite her family history. The results of her exam were fine, and she is now aware that she needs to be watched more closely and come in annually for exams.
The program also provides survivors with a way to channel their passion for helping other women with breast cancer. “I am thankful that I had the people who helped me through my [breast cancer] journey during treatment,” said one survivor. “So now, as a survivor, I can make a difference by helping women in the community.”
CHALLENGES
One of the main challenges of the program is recruiting survivors who are excited to volunteer and can articulate the exam process. Despite the $50/day stipend plus $15/day for transportation, we had to move aggressively to recruit survivors. As noted above, we sent an e-mail blast to our patient list and placed English and Spanish announcements in our newsletter and in the Bridgeport Hospital employee newsletter. Some women who expressed an interest had difficulty meeting their obligations when they were scheduled for programs, while others would have required a great deal of training, more than our lean staff had time for.
Others were looking for a job with regular hours rather than irregular events that took place at different times, and on differ - ent days of the week, including weekends. Occasionally, a bilingual social worker from our partner organization CancerCare attended some of our programs. Ideally, a pool of volunteers with a variety of schedules would create more flexibility and provide backup volunteers when someone’s schedule changed at work or at home. Because our nurse educators split their time with their duties as nurse navigators, the program would also benefit from a person dedicated solely to education who could also train survivors as volunteers.
LOOKING FORWARD
Because we see many of the same women at the food pantry each month, we are now trying to reach out to women whom we don’t see by providing men from the community with a packet of information. Our hope is that it will reach the adult women in their family. The packet contains an informational pamphlet, a bracelet with our name, and other items. These small tokens are meaningful to individuals who have so little. Women can learn about the center and contact us through the church. In the future, we see replicating the program at other food banks on a monthly basis. We also continue to experiment with new venues.
Once the program was established, we were able to attract additional grant funding for expenses such as grocery store debit cards, stipends for survivors, and teaching materials. We will continue to explore new grant opportunities as the program grows.
REFERENCS
- US Census Bureau. American Community Survey, 2005-09. http://www.census.gov/acs/www/data_documentation/2009 _5yr_data/. Accessed April 8, 2012.
- Connecticut Cancer Partnership. Connecticut Comp rehensive Cancer Control Plan, 2005-08. Hartford, CT: Connecticut Cancer Partnership; 2005.
- Connecticut Affiliate of Susan G. Komen for the Cure. Community Report, 2009. Hartford, CT: Connecticut Affiliate of Susan G. Komen for the Cure; 2010.
- Connecticut Department of Public Health. Cancer Incidence in Connecticut Towns, 2000-2003. Hartford, CT: Connecticut Department of Public Health; 2006.
- Connecticut Department of Public Health. Connecticut Health Disparities Project. The 2009 Connecticut Health Disparities Report. Hartford, CT: Connecticut Department of Public Health; 2009.
- Latino Policy Institute. A Profile of Latino Health in Connecticut. Hartford, CT: Hispanic Health Council; 2006.
- Centers for Disease Control and Prevention. CDC health disparities and inequalities report—United States 2011. MMWR Morb Mortal Wkly Rep. 2011;60(suppl):1-116.
- Buki LP, Selem M. Cancer screening and survivorship in Latino populations: a primer for psychologists. In: Villarruel FA, Carlo G, Grau JM, et al, eds. Handbook of U.S. Latino Psychology. Thousand Oaks, CA: Sage Publications Inc; 2009:363-368.
- Avon Foundation for Women. Breast cancer rates questioned in Latina population. http://www.avonfoundation.org/press-room/breast-cancer-rates-questioned-in-latina-population.html. Accessed July 25, 2011.
- Saad-Harfouche FG, Jandorf L, Gage E, et al. Esperanza y Vida: training lay health advisors and cancer survivors to promote breast and cervical cancer screening in Latinas. J Community Health. 2011;36:219-227.
- Sudarsan NR, Jandorf L, Erwin DO. Multi-site implementation of health education programs for Latinas. J Community Health. 2011;36:193-203.
- Connecticut Department of Public Health. Federal shortage designation information, CT towns. http://www.ct.gov/dph/lib/dph/practitioner_licensing_and_investigations/plis/jvis a/designatedareas.pdf. Accessed July 25, 2011.




