As the field of oncology nurse navigation continues to expand, standardization of the orientation process is necessary. “To move the field forward, explication of navigator tasks is necessary to inform the development of programs, job descriptions, training, evaluation, certification standards, and reimbursement mechanisms.”1 The orientation/onboarding process for oncology nurse navigation is neither standardized nor well understood across the industry. According to Dellasega and colleagues,2 orientation to the work environment can reduce attrition, shape early job satisfaction, and help to set a nurse’s attitude toward the employer and role—even among experienced nurses. To be an oncology nurse navigator (ONN), most employers require some type of experience, whether in oncology or as a nurse in general. Orientation therefore should focus less on being a first-time nurse and more on the role itself. This being said, mentoring and orienting are essential pieces of the process. “A good orientation is key for your new navigator’s success.”3
Orientation is usually specific to the employer and considers the type of role and the type of employee.4 As Colduvell5 notes, nursing is a very detail-oriented position, and thus a new nursing role can be especially overwhelming if not prepared well. Colduvell stresses the importance of organization. Human Resources, benefits, and employer expectations will be excluded, as this research will focus more specifically on orientation to the role. The Joint Commission6 requires that job-specific training occurs but does not define exactly what that entails for each facility. It does state that competency is measured by a combination of observable and measurable knowledge and skills. Evidenced-based orientation guidelines for the role of ONN are difficult to find in the literature.
At Sarah Cannon, the Cancer Institute of HCA Healthcare, onboarding and orientation are key components to the success of the ONN. Many tools are utilized in program development. The role is supported by educators, administrative leadership, and physician-led programming. It is important to measure the effectiveness of organizational efforts during and after any significant shifts in programmatic development, such as the addition of new facilities.
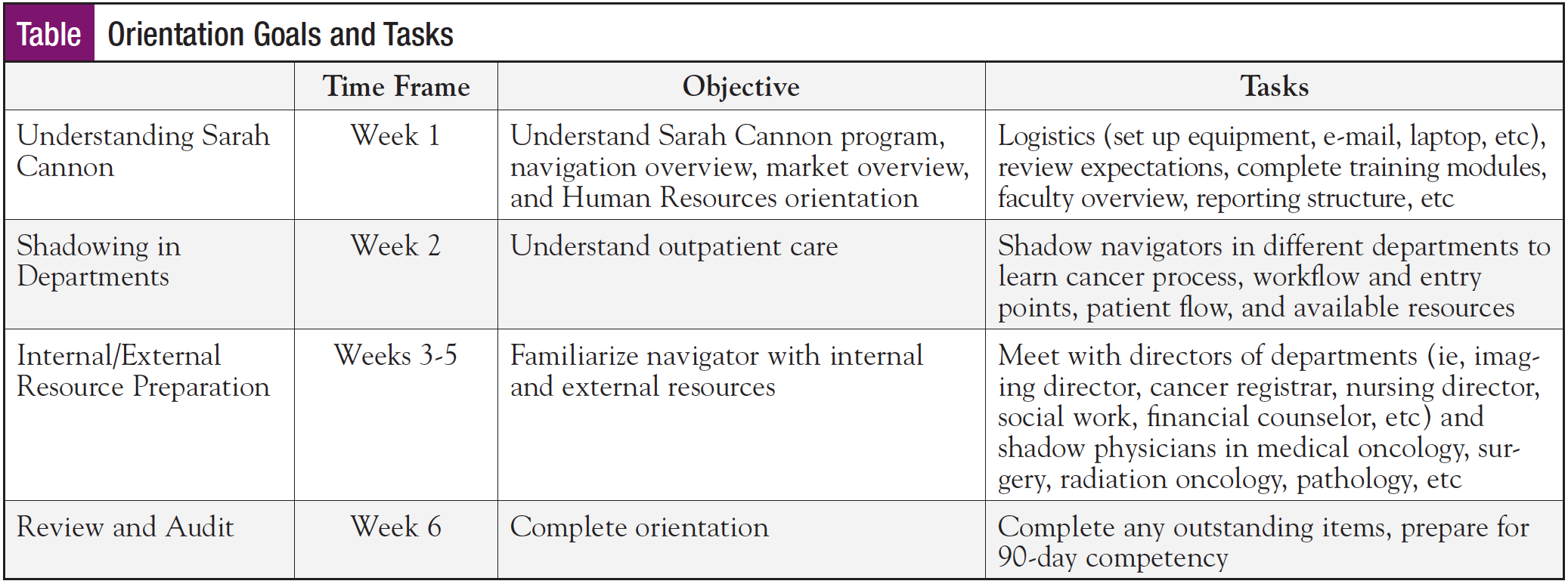
Sarah Cannon provides Division Directors of Navigation with a toolkit that consists of orientation “how-tos” for onboarding new navigators as well as a refresher training for existing navigators. This toolkit is consistent across our network to help standardize the onboarding process. We have found this to be helpful when navigators are filling in for other colleagues across markets. Our director’s toolkit includes an onboarding checklist, job description, competencies, weekly templates, competency tests, and mentor/preceptor checklists (Table).
As part of the onboarding process, navigators are given a competency test for their knowledge of the tumor site that they will be navigating. This allows the director as well as the navigator to know where more training is needed, whether it is hands-on in the clinic with the physicians or didactic. The test is an online link outside our educational tool. There is no pass/fail score; it only evaluates their knowledge base.
Because of the large size of our organization, a voluntary self-reported survey was performed to obtain information on the standardized onboarding at every level of the network. New navigators who are onboarding to our company have access to similar tools during their orientation while the individual’s timeline fluctuates. The navigators in this grouping are all actively employed registered nurses with a focused population of oncology patients. The benefits of using this sample population are the volume of navigators, volume of facilities, and the consistency of metrics and outcomes related to the success of the navigation.
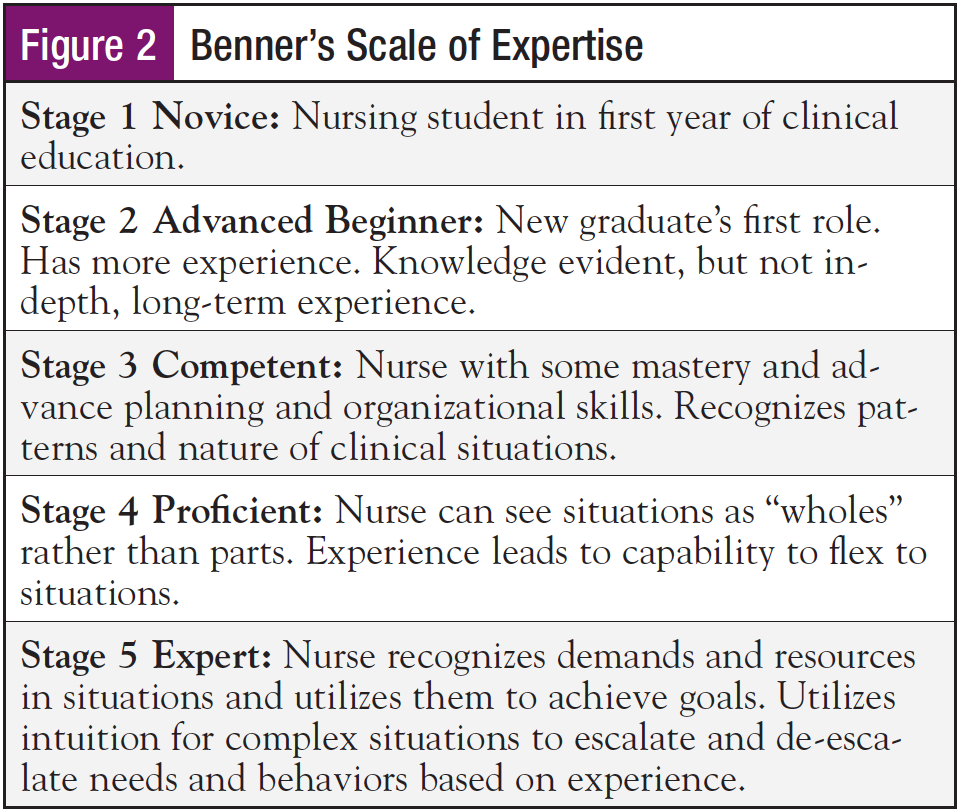
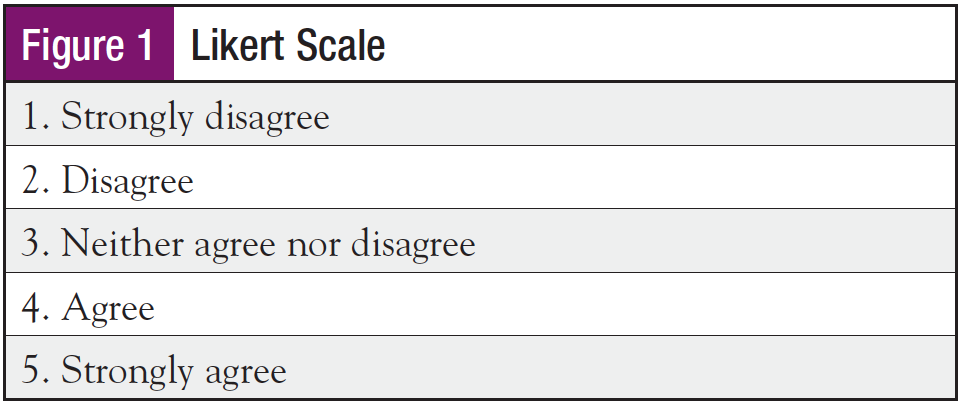
Responses to the survey were blinded. Questions were offered in multiple choice format and open response survey. The Likert scale (Figure 1) was utilized when appropriate, and Benner’s Scale of Expertise (Figure 2) was used to self-report nursing proficiency in the survey. The scales were explained in detail in the introduction to the survey. Over a 7-day period, 79 oncology navigators from across the nation were queried. Questions pertained to level of navigator expertise, length of time in nursing, time in role, and orientation-based questions.
Results from the study revealed a total of 57 navigators (56 women, 1 man) from 9 states responded. Representation from all age groups was well distributed: 25 to 34 years, 23%; 35 to 44 years, 25%; 45 to 54 years, 20%, and 55 to 64 years, 30%. More than 75% have been nurses for over 10 years, with more than 60% having over 5 years of oncology experience. Sixty percent have been an ONN for more than 2 years. On several dimensions measured by the Benner level, self-reported responses were similar, with approximately 25% competent, approximately 45% proficient, and 25% reporting as expert. Average length of orientation/onboarding was more than 4 weeks for 65%. Fifty percent of the total surveyed reported this length of time was appropriate. Orientation strategies utilized were 8% online, 78% shadowing, 53% textbooks, 69% videos/Webex, and 47% navigation staff meetings.
Overwhelmingly, the study revealed satisfaction with the onboarding process with education and tools utilized during the process, but it did show more shadowing time was a request with 69% disease-specific, 58% with mentor, 50% with physicians, and 46% with other navigators. The request for increased shadowing time was shared with leadership and is implemented at the division leadership level.
In conclusion, the current orientation/onboarding process of those responding to this survey indicates that the process is successful in training competent, proficient, and expert ONNs. The navigators reported continued use of provided materials, education provided, and tools received. Ongoing education is part of the routine working environment, with continuing education provided frequently and often after the orientation period has concluded. However, one aspect of the survey did show additional time in specific modalities of shadowing would be beneficial. This validates the current process used by this enterprise that is orchestrated by the education department and navigation leaders.
References
- Braun KL, Kagawa-Singer M, Holden AE, et al. Cancer patient navigator tasks across the cancer care continuum. J Health Care Poor Underserved. 2012;23:398-413.
- Dellasega C, Gabbay R, Durdock K, Martinez-King N. An exploratory study of the orientation needs of experienced nurses. J Contin Educ Nurs. 2009;40:311-316.
- Strusowski T. Creating a Navigator Orientation Checklist. Association of Community Cancer Centers. http://mynetwork.accc-cancer.org/blogs/acccbuzz-blog/2016/11/29/creating-a-navigator-orientation-checklist. Accessed December 14, 2018.
- McMullen L, Christensen D, Haylock PJ, et al. 2017 Oncology Nurse Navigator Core Competencies. Oncology Nursing Society. www.ons.org/sites/default/files/2017-05/2017_Oncology_Nurse_Navigator_Competencies.pdf. Accessed December 14, 2018.
- Colduvell K. Nursing Orientation: 10 Tips To Get The Most Out Of Your Time. Nurse.org. https://nurse.org/articles/nursing-orientation-tips. 2017. Accessed December 14, 2018.
- The Joint Commission. Orientation Standards. www.jointcommission.org/standards_information/jcfaqdetails.aspx?StandardsFaqId=897&ProgramId=46. Accessed December 14, 2018.
- Benner P. From Novice to Expert. Nursing Theory. http://nursing-theory.org/theories-and-models/from-novice-to-expert.php. 2016. Accessed December 14, 2018.