Background: Disparities in breast cancer outcomes among underserved ethnic minority women are well established. Adverse social determinants of health create barriers to optimal breast cancer treatment, such as access to treatment, missed appointments, and delays in treatment. Interventions to promote better access to recommended treatment are critically needed.
Objective: To create and implement a dedicated pilot program to minimize barriers to care and increase referrals and access to resources for medically underserved women with breast cancer.
Methods: A program was designed that included a dedicated oncologist, bilingual nurse coordinator, social worker, and a newly created community cancer care navigator. Partnerships with community agencies and a legal assistance association were established. Funding was secured to support a 2-year pilot program.
Results: A total of 101 underserved women with breast cancer participated. The average age was 57.3 years, 54.8% were ethnic minorities, 45.5% had government insurance, 6% had no insurance, and English was a second language or not spoken for 13.9%. There were 120 referrals primarily for nonmedical needs (48.3% financial, 3.3% housing, 17.5% legal issues, 20.8% transportation).
Discussion: The complex needs of underserved women with breast cancer were confirmed and require innovative approaches to decrease modifiable factors that contribute to disparate outcomes.
Conclusion: A dedicated program for an underserved population was successful in minimizing barriers to receiving optimal breast cancer care. A community cancer care navigator role was essential as a liaison with partners in the community.
Biologic factors, genetics, histologic features, and estrogen and progesterone receptors are known to contribute to patient outcomes.1-4 In addition, adverse social determinants of health create significant barriers to care access, resources, and optimal breast cancer treatment.5,6 Black and Hispanic women with breast cancer have greater psychosocial, support, financial, and overall needs,7-9 often resulting in missed appointments, delayed appointments, fewer treatment options, less likelihood of receiving recommended treatment, and worse outcomes.5,7,10 Patient navigation has been an approach to address nonmedical barriers for underserved cancer patients, including but not limited to finances, transportation, lack of childcare, insurance, unmet informational needs, employment, and housing,11-13 with demonstrated improvements in unmet needs, adherence to treatment, and receiving recommended therapy.11,14,15 Evidence also suggests that screening for legal issues is important for vulnerable populations,13,16 and oncology-legal partnerships offer a critical linkage to address and resolve issues that can facilitate optimal receipt of care.16,17
There is a need for oncology to address barriers to cancer care, especially in those communities with greater numbers of ethnic minorities and underserved populations with reported increased unmet needs.8 In the State of Connecticut, Hispanics and blacks account for 14.2% and 10.4% of the population, respectively,18 whereas in the greater New Haven area, blacks account for 35% and Hispanics 27% of the population and have lower household incomes, higher percentage receiving food stamps, and more non-English–speaking persons. Based on the population data and the experience of providers in the clinical breast cancer setting, an urgent need was identified to address underserved women with breast cancer.
Objective
To create and implement a dedicated pilot program to minimize barriers to care and increase referral and access to resources for medically underserved women with breast cancer. The purpose was to assess feasibility of the program and referrals to access resources for women with breast cancer who were enrolled.
Methods
An assessment was conducted on the services currently provided by nursing, social work, and supportive care resources at the Smilow Cancer Hospital at Yale New Haven Hospital community campus site. While these provider and clinical resources were available, they were primarily hospital-based with significant identified barriers to time and expertise to address the complexity of factors associated with underserved populations. The primary goal was to provide coordinated comprehensive and high-quality patient-centered care that would integrate community resources and partnership with New Haven Legal Assistance Associates (NHLAA). To achieve this goal, collaboration was established with ambulatory administration of Yale New Haven Hospital, the nursing manager for the Yale Cancer Center Breast Cancer Program, and the Yale School of Nursing to support grant applications for funding and development of resources. Two grant applications were submitted (Avon Foundation for Women and the Connecticut Health and Educational Facilities Authority) for the proposed pilot program and were awarded ($110,000). Funding supported the newly created role of a community cancer care navigator (32 hours a week), a dedicated nurse coordinator (1 day a week), a dedicated social worker (1 day a month), an administrative coordinator (one-half day a week), as well as development of informational materials and funds to support patient needs, such as transportation and food insecurity.
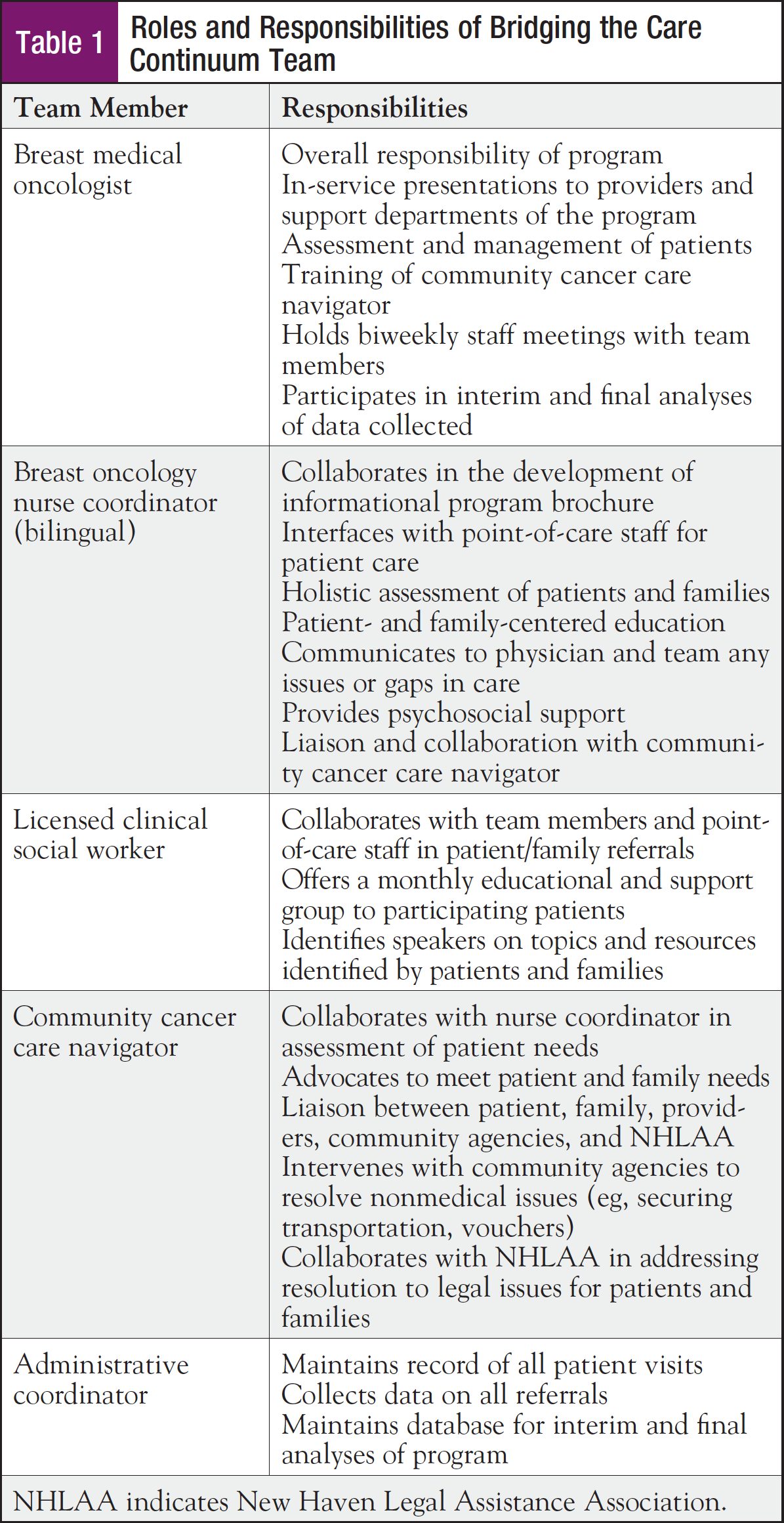
Members of the team were identified to include a breast medical oncologist, a nurse coordinator, a community cancer navigator, a social worker, and an administrative staff coordinator. Members of the team had an established working relationship, unified commitment to the underserved population in the area, and previous research collaborations. Together, these factors strongly supported the collaborative development and implementation of the program. The roles and responsibilities of the primary program team members are detailed in Table 1. The bilingual community cancer care navigator was recruited and trained by the breast medical oncologist and the NHLAA and oriented to the goals of the program. As an experienced patient navigator in the health system, the expanded role and community outreach was easily adapted for the target population and community where these women lived.
Results
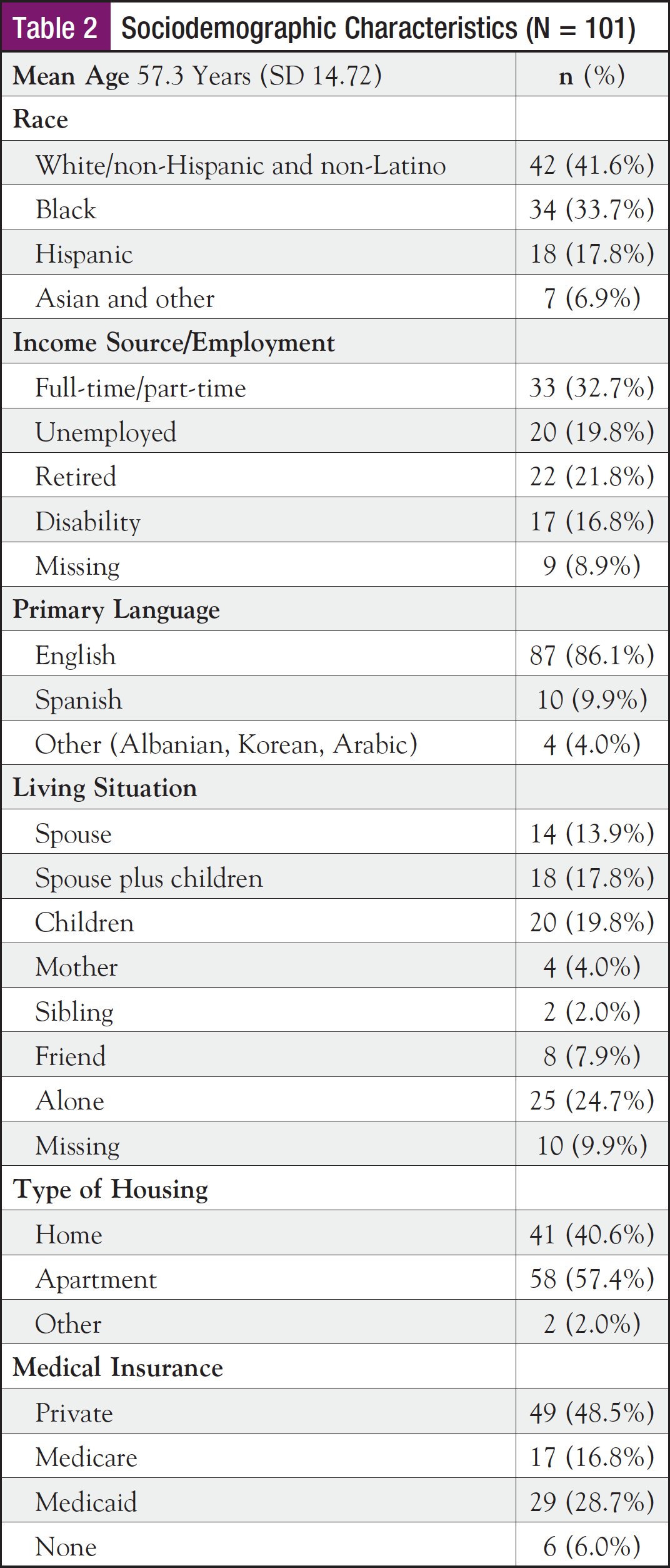
A total of 101 women with breast cancer participated in the program, Bridging the Care Continuum, designed for the vulnerable and underserved breast cancer population. The sociodemographic characteristics are detailed in Table 2. The average age of program participants was 57.3 years (range, 27-97 years); the majority were nonwhite; about two-thirds were unemployed, retired, or disabled; slightly more than half had no insurance or government insurance; and the majority (86%) spoke English. Chemotherapy or combined chemotherapy plus endocrine therapy was the most common treatment, and the majority had metastatic breast cancer. There were 31 medical referrals, with 75% of those to palliative care or hospice.
This group of women with breast cancer reported multiple unmet needs, and 120 referrals were made for nonmedical reasons (Table 3). Among the 58 referrals for financial issues, 60% were $50 gift cards primarily for food or clothing. Other financial issues reported were need for help with utility bills, mortgage, medical bills, copays, general living expenses, and limitations of a fixed income. The referrals to the NHLAA included employment, housing court, marriage/family issues, Family Medical Leave Act, and disability issues. Transportation was predominantly the need to get to clinic and hospital appointments, and vouchers for taxis were issued to approximately one-quarter of the women.
Discussion
The findings of this pilot program for an identified group of vulnerable breast cancer patients confirmed the evidence in the literature on risk factors and unmet needs; specifically, fewer than half had private medical insurance,7,10,14 and adverse survival outcomes have been reported for women with breast cancer who have Medicaid or no insurance.19 There were significant financial needs related to food, transportation, out-of-pocket medical costs, and nonmedical expenses,6,9,10,20 and there was an explicit need for legal assistance with financial, domestic, and social issues,13,16 as well as a variety of psychosocial issues9,11 that were assessed and managed by the team social worker. There was strong evidence of the contribution of the role of the community cancer care navigator as a liaison to community resources and to the legal partnership. In addition to the perceived value by the team, this dedicated navigator role went beyond the scope of the traditional hospital- or clinic-based support providers. Navigators have been shown to assist with screening, provide support and continuity, refer to appropriate resources to resolve issues, decrease barriers to receiving care, and avoid complications.12,14,15,17,21 Addressing unmet needs and barriers to care and identifying resources to underserved populations can minimize or prevent missed appointments, delays in treatment, no-show appointments, urgent visits, and emergency department visits.7,11,15 If interventions such as this pilot program are implemented, there is the opportunity to alter adverse outcomes, such as unfavorable therapeutic response and decreased disease-free and overall survival, and improve optimal receipt of recommended therapies and patient-perceived quality of survival.3,5,17
Although the findings of this pilot program demonstrated receptiveness of patients, feasibility of implementation, evidence of preliminary success in improving access to breast cancer care (ie, transportation support to visits), and decreasing barriers by referral to medical and nonmedical resources, there are significant limitations. The program was not designed as a research study in which you would collect data on missed appointments, delays in treatment, or quality of perceived care and be able to demonstrate an advantage to the program compared with usual care. In 1 study that tested an intervention to decrease no-show appointments with telephone calls by a navigator over a period of 5 months, there was a difference between the intervention and control groups.15 There is currently a randomized controlled trial comparing a patient navigator with a patient navigator plus legal partner. The outcomes of interest are timely treatment, quality of care, and patient-centered outcomes (needs, satisfaction). Some preliminary findings on recruitment with sociodemographic characteristics on those accrued to date have been reported,17 but this trial remains in the recruitment and data collection phases. Further research is needed to generate a body of evidence for translation to clinical practice for agencies and organizations that would support the value of dedicated navigators, partners, and providers to patient outcomes.
Conclusion
Creating and implementing a dedicated program for underserved women with breast cancer provided support to address barriers to care and initiated referrals to resources, thus increasing access to those resources and promoted continuity of care for these vulnerable women and their families. The complexity of issues and the unmet needs of an underserved population were validated. The partnership with a legal assistance organization was valuable and resulted in resolution of several social, employment, housing, disability, and other issues that required professional intervention. The community cancer care navigator demonstrated the need for the role that transcended the scope of the traditional social worker that is available to outpatient cancer settings. That role was supported by the grant funds, and one challenge is the sustainability of support for such roles with only pilot program data. Research is needed to confirm and test the value of the pilot program and the role of a community cancer care navigator. Data from such research could provide support for funding and sustainability of the role within cancer care settings. It is critical for providers, organizations, and the community to address the complexity of social and environmental factors of populations known to be at risk for poorer outcomes and develop goals and interventions to promote optimal patient outcomes and better quality of life.20,22
Acknowledgments
Funding from Avon Foundation for Women and the Connecticut Health and Educational Facilities Authority. For administrative support: Teren Basel and Patricia DeWitt, Office of Development of Yale New Haven Hospital, and New Haven Legal Assistance Association.
References
- American Cancer Society. Facts & Figures for African Americans 2019-2021. Atlanta, GA: American Cancer Society; 2019.
- American Cancer Society. Facts & Figures for Hispanic/Latinos 2018-2020. Atlanta, GA: American Cancer Society; 2018.
- Saparano JA, Wang M, Zhao F, et al. Race and hormone receptor–positive breast cancer outcomes in a randomized chemotherapy trial. J Natl Cancer Inst. 2012;104:406-414.
- Vicini F, Jones P, Rivers A, et al. Differences in disease presentation, management techniques, treatment outcome, and toxicities in African-American women with early stage breast cancer treated with breast-conserving therapy. Cancer. 2010;116:3485-3492.
- Morris GJ, Naidu S, Topham AK, et al. Differences in breast carcinoma characteristics in newly diagnosed African-American and Caucasian patients: a single-institution compilation compared with the National Cancer Institute’s Surveillance, Epidemiology, and End Results database. Cancer. 2007;110:876-884.
- Spencer JC, Samuel CA, Rosenstein DL, et al. Oncology navigators’ perceptions of cancer-related financial burden and financial assistance resources. Support Care Cancer. 2018;26:1315-1321.
- Sabatino SA, Coates RJ, Uhler RJ, et al. Health insurance coverage and cost barriers to needed medical care among U.S. adult cancer survivors age <65 years. Cancer. 2006;106:2466-2475.
- Knobf MT, Ferruci L, Cartmel B, et al. Needs assessment of cancer survivors in Connecticut. J Cancer Surviv. 2011;6:1-10.
- Moadel AB, Morgan C, Dutcher J. Psychosocial needs assessment among an underserved, ethnically diverse cancer population. Cancer. 2007;109(2 suppl):446-454.
- Darby K, Davis C, Likes W, Bell J. Exploring the financial impact of breast cancer for African American medically underserved women: a qualitative study. J Health Care Poor Underserved. 2009;20:721-728.
- Madore S, Kilbourn K, Valverder P, et al. Feasibility of a psychosocial and patient navigation intervention to improve access to treatment among underserved breast cancer patients. Support Care Cancer. 2014;22:2085-2093.
- Gentry S. Navigation and breast cancer standard of care. Journal of Oncology Navigation & Survivorship. 2020;11(1):14-19.
- Friedlander Cole C. Breast cancer navigation: finding solutions for the most vulnerable during a health crisis. Journal of Oncology Navigation & Survivorship. 2020;11(3):84-86.
- Ko NY, Darnwell JS, Calhoun E, et al. Can patient navigation improve receipt of recommended breast cancer care? Evidence from the National Patient Navigation Research Program. J Clin Oncol. 2014;32:2758-2764.
- Percac-Lima S, Cronin PR, Ryan DP, et al. Patient navigation based on predictive modeling decreases no-show rates in cancer care. Cancer. 2015;121:1662-1670.
- Retkin R, Antoniadis D, Pepitone DF, Duval D. Legal services: a necessary component of patient navigation. Semin Oncol Nurs. 2013;29:149-155.
- Ko NY, Bak S, Gunn C, et al. An innovation in patient navigation: background, methods, and measures. Journal of Oncology Navigation & Survivorship. 2019;10(6):218-226.
- Statistical Atlas. Race and Ethnicity in Connecticut. https://statistica latlas.com/state/Connecticut/Race-and-Ethnicity. Accessed March 9, 2020.
- Unger JM, Blanke CD, LeBlanc M, et al. Association of patient demographic characteristics and insurance status with survival in cancer randomized clinical trials with positive findings. JAMA Netw Open. 2020;3:e203542.
- Hastert TA, McDougall JA, Strayhorn SM, et al. Social needs and health-related quality of life among African American cancer survivors: results from the Detroit Research on Cancer Survivors study. Cancer. 2021;127:467-475.
- Freund KM, Battaglia TA, Calhoun E, et al. National Cancer Institute Patient Navigation Research Program: methods, protocol, and measures. Cancer. 2008;113:3391-3399.
- Hassmiller SB, Kuehnert P. Building a culture of health to attain the sustainable development goals. Nurs Outlook. 2020;68:129-133.