With a malignancy like lung cancer, early detection can quite literally mean the difference between life and death. Despite this, lung cancer screening and incidental pulmonary nodule (IPN) management are still sorely lacking in the United States, according to Kim Parham, BSN, RN, CB-BN, vice president, Strategic Partnerships and Clinical Liaison, Thynk Health, and Shawn Perkins, BSN, RN, OCN, a thoracic services nurse navigator at Cone Health Cancer Center at Alamance Regional.
At the 2022 AONN+ Midyear Conference in Austin, TX, Mr Perkins and Ms Parham discussed the importance of early detection and pulmonary nodule management in lung cancer and emphasized the crucial role of the navigator in establishing programs that bring these vital services to the people that need them most.1
Lung Cancer Statistics
Lung cancer is one of the most common cancers diagnosed—and the most common cause of cancer death—in the United States. The overall 5-year relative survival rate for lung cancer is relatively low compared with some other cancers: 22% (18% for men and 25% for women), with 26% for non–small-cell lung cancer and 7% for small-cell lung cancer.2
However, the 5-year survival rate is about 60% for lung cancers diagnosed at a localized stage, but less than one-quarter of lung cancers are found at this early stage. According to Mr Perkins, this underlines the need for implementing comprehensive screening programs and raising awareness about not only the importance—but the absolute necessity—of pulmonary nodule programs in lung cancer. Navigators play a crucial role in this effort.
Prior to 2015, screening efforts for lung cancer were mostly patient-paid and largely unsuccessful, but since then, navigators have played a pivotal role in expanding community outreach for screening and prevention efforts.
“You have to market to your public, because a lot of people don’t know about lung screening, just like most people aren’t aware of nurse navigation,” said Mr Perkins. “Lung screening has been covered by the Centers for Medicare & Medicaid Services since 2015, and many people have still never heard of it.”
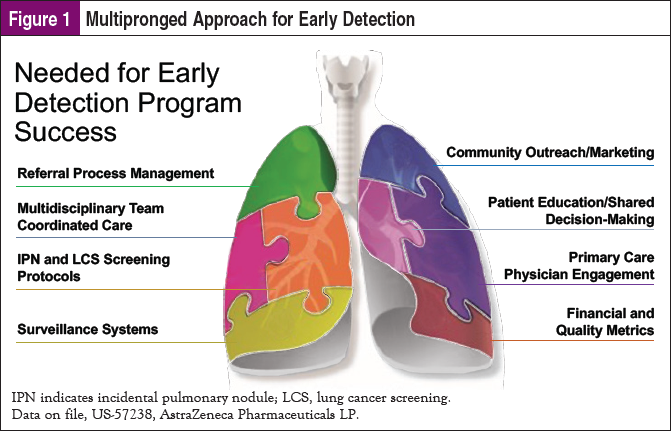
Setting up an early detection program requires a multipronged approach (Figure 1). Among the many logistical components needed are:
- A dedicated referral process (to ensure the right patients are coming in for lung screening)
- A multidisciplinary team
- IPN and lung cancer screening protocols (knowing how to handle results and successfully move the patient through the continuum)
- Surveillance systems (managing large volumes of patients, making sure no patient slips through the cracks)
- Community outreach/marketing
- Patient education/shared decision- making
- Engagement and support from primary care providers (PCPs)
- Tracking of financial and quality metrics
Navigation can address each of these components while prioritizing patient advocacy, education, and support. In their pivotal role in moving the patient through the cancer care continuum, navigators have become instrumental members of the multidisciplinary team.
“When you put all of these pieces together, you get a good program that delivers comprehensive early detection for lung cancer,” he said.
Entry Points for Early Lung Cancer Detection
Patients have 2 entry points for early lung cancer detection: abnormal screening results and IPN findings. “Screening and incidental pulmonary nodule programs are 2 very separate but complementary systems,” he explained.
Lung cancer screening involves eligibility requirements: a patient must be of a certain age, with a certain smoking history. IPN programs, on the other hand, have no eligibility requirements; IPN findings are detected on imaging/tests/scans that are performed for an unrelated reason (hence the term “incidental”).
“It doesn’t matter if you ever smoked; if you have an IPN finding, we need to follow it,” Mr Perkins noted, adding that about 10% to 20% of lung cancer is diagnosed in nonsmokers.3
“With up to 20% of patients being diagnosed with lung cancer who have no tobacco history, making sure we have an IPN identification and follow-up is crucial,” said Ms Parham. “Many of these patients are women and, in many cases, younger. In fact, nonsmoking lung cancer would be within the top 10 of cancer incidence and mortality by itself.”
But just because some patients might be a bit younger and healthier, it doesn’t mean they’re not in need of navigation. “I worked with several young patients who were athletes, and many of these patients have unique educational needs and barriers,” she said. “One young athletic male patient of mine who was just diagnosed with lung cancer was able to bank his sperm before starting treatment.”
Mr Perkins echoed this point, bringing up a patient of his who was diagnosed with stage IV adenocarcinoma of the lung 10 years ago at the age of 48 years. “He was a never smoker with no other risk factors,” he noted. “He was a tennis pro, and he continues to coach to this day while receiving maintenance treatment.”
The American College of Radiology requires lung screening results to be reported as a Lung-RADS (Reporting and Data System) score; these numerical scores represent “incomplete,” “negative,” “benign,” “probably benign,” “suspicious,” “very suspicious,” and “other” findings.4 According to the organization, Lung-RADS is a quality assurance tool designed to standardize lung cancer screening CT reporting and management recommendations, to reduce confusion in lung cancer screening CT interpretations, and to facilitate outcome monitoring. Navigators should familiarize themselves with the Lung-RADS classification system, as they play a key role in helping patients to understand the different categories of findings, as well as the next steps for management. “Results for IPN findings should be reported following Fleischner Society guidelines. Like Lung-RADS, this allows for consistent recommendations based on factors such as individual risk factors, nodule size, number, consistency (solid, part solid, or ground glass), increase in size, and location” as stated by Mr Perkins.
According to Mr Perkins, the navigator role is even more crucial when findings are classified as 4A and above; at this point, the navigator should involve the patient’s PCP and entire multidisciplinary team in their management. In addition to narrowing down the best path forward in explaining suspicious findings, this practice enhances timeliness of care and ensures consistent follow-up.5
“You want to tell the patient honestly that there’s something suspicious, but you don’t want them up all night worrying for the next 3 months while awaiting their recommended follow-up CT scan,” he said. “It’s a delicate thing to manage, like many things that navigators deal with.”
Coverage determination for lung cancer screening can be a gray area depending on a person’s insurance plan, age (ie, too young for Medicare or too old to fit within the screening requirements), and other factors, “so navigators should be best friends with the person getting authorizations and approvals; these people are so important to helping us navigate coverage,” he added. Navigators should also network and familiarize themselves with additional financial assistance options for patients, such as grants or charitable funding.
Barriers to Establishing Screening and IPN Programs
The workflow for an IPN is different from that of a lung cancer screening finding. According to Ms Parham, a lung nodule is classified as anything under 3 centimeters, but as they are often measured in millimeters, they can be easily overlooked. After it’s found, a radiologist will identify and properly document the IPN, classifying it as low-risk or high-risk, per the Fleischner Society guidelines. The ordering provider then receives the results and communicates their significance to the patient and PCP, and appropriate follow-up care is scheduled, or the patient is enrolled in a nodule management program, she explained.
However, this process does not always go smoothly. Certain barriers are unique to either lung cancer screening or IPN programs, but some overlap.
With screening, hurdles such as lack of opportunity/access, myths/stigma, and adherence often stand in the way, while barriers unique to IPN findings include patient lack of a PCP/lack of PCP awareness, as well as a lack of or inconsistent reporting. But through consistent patient education, care coordination, assessing patients for barriers to care, and offering resources to address those identified barriers, navigators can clear these hurdles, especially when dealing with a patient’s PCP and multiple health systems.5
Barriers that can be found with both lung cancer screening and IPN programs include inconsistency of radiology reporting, PCP knowledge (or lack thereof) of findings, stigma, anxiety (or “scanxiety”), poor tracking of patients, health equity issues (missing the uninsured/underinsured patients), and financial barriers (annual scans may be covered, but diagnostic scans may not) (Figure 2).
Mr Perkins emphasized the importance of screening adherence to detecting nodule growth. “Our national rates of adherence are low,” he said. “But rates of adherence are higher with a centralized navigation program—around 70%—compared with 40% with a decentralized program.”
He also pointed out the importance of acquiring an accurate smoking history, as people sometimes unintentionally provide an inaccurate history. “When you ask a 70-year-old how many years he’s been smoking, he might say 30 years, even if he started when he was 20,” Mr Perkins noted. “We all want to think we’re younger than we are, and we also want to minimize our history.” Patients also might minimize the number of cigarettes they smoke, so it’s important for navigators to use language that will elicit truthful answers: ie, “How old were you when you first started smoking?” rather than, “How many years have you been smoking?”
Lung Cancer Screening Programs: Keys to Success
According to Mr Perkins, successful lung cancer screening programs have a number of characteristics:
Clinical Expertise—“The Navigator Is the Glue”
“You need the expertise to manage the questions that are going to come up from your patients,” he said. “When you call them to verify their eligibility for screening, they’re going to want to know why they need to have this done.”
They might ask questions like: “Does the doctor suspect I have lung cancer and isn’t telling me?” or “What's going to happen if have it?” PCPs may also appreciate the navigator’s guidance on sharing results with patients, he added.
Infrastructure
“So many programs rush into screening before developing the necessary infrastructure, and that results in some growing pains,” he said. Gaining support from physician champions (typically pulmonologists or thoracic surgeons), PCPs, and administrators first, then developing processes (ie, tracking patients, handling results, insurance issues, etc), are important first steps in building a program.
Care Coordination, Data Management, Identification, and Tracking
“These are so important to efficiently handling abnormal findings, navigating patients, and keeping them moving forward,” he said, adding that navigators will inevitably be dealing with multiple specialties (pulmonary, thoracic, radiology, pathology, etc), and they are often responsible for facilitating communication between all of them.
Metrics
To continue lung cancer screening efforts, programs have to be able to demonstrate their benefit—both in terms of patient outcomes as well as financially.
According to Ms Parham, 2 specific business models can help burgeoning early detection programs to justify their impact and demonstrate financial benefit for the health system: the National Lung Cancer Roundtable LungPLAN and the GO2 Foundation business model.
Biomarker Testing and Survivorship
Once diagnosed, a patient with lung cancer will typically undergo surgery, radiation therapy, or systemic therapy, depending on the stage. But with the use of biomarker testing, lung cancer treatment becomes much more personalized to the individual patient. Many of the key biomarkers that play a role in lung cancer (eg, EGFR, ALK, BRAF, ROS1, NTRK, MET, RET, PD-L1, and KRAS) now have correlating FDA-approved targeted treatments.6
“Your role as a navigator is so important to assuring appropriate testing,” said Ms Parham. “If you’re working in the early detection realm, keep up with the NCCN [National Comprehensive Cancer Network] guidelines, because they’re changing.”
The NCCN guidelines now include separate adjuvant and neoadjuvant therapy recommendations for early-stage lung cancer6,7; it’s crucial that navigators stay abreast of these changes to ensure that the appropriate tests are provided to the appropriate patients, she noted. Navigators also play an important role in facilitating turnaround time for tissue testing, providing education to patients on the importance of testing, and solving financial issues associated with biomarker testing, she said, adding that some insurance plans only cover limited biomarker testing, while some will cover the entirety of next-generation sequencing.
According to Ms Parham, navigators can find numerous online webinars, while AONN+ local navigator networks provide educational opportunities for navigators to keep up to date with new medications and indications (including new targeted treatments). “With many neoadjuvant and adjuvant indications being recommended, it’s important to look frequently at the NCCN guidelines—either by app or on the website—and have them available during multidisciplinary tumor board discussions,” she said. “Being the patient voice within tumor board discussions is so important, and that starts with knowing the most up-to-date recommendations.”
Mr Perkins agreed, adding: “with the speed of healthcare advances, it has never been more vital that navigators stay current with changing guidelines. With the barrage of new information coming out daily, our PCPs struggle to keep up, and often it is up to nurse navigators to educate them. Staying up to date is one of the best ways we can advocate for our patients to receive the best care and outcomes.”
Perhaps most importantly, more lung cancers found at early stages translates to more lung cancer survivors.
“You’re going to have more and more patients diagnosed at stage I and II,” said Ms Parham. “So now is the prime time to ramp up your survivorship programs for patients with lung cancer; you’re always going to be the advocates for your patients to have better outcomes and better quality of life.”
Acknowledgment
The Journal of Oncology Navigation & Survivorship gratefully acknowledges the contributions of Ms Parham and Mr Perkins in the creation and review of this article.
References
- Parham K, Perkins S. Importance of Early Detection in Lung Cancer: Elevating the Navigator’s Role. Academy of Oncology Nurse & Patient Navigators (AONN+) 2022 Midyear Conference, Austin, TX. Presented May 13, 2022.
- American Cancer Society. Cancer Facts & Figures 2022. www.cancer.org/research/cancer-facts-statistics/all-cancer-facts-figures/cancer-facts-figures-2022.html. Accessed May 2, 2022.
- Centers for Disease Control and Prevention. Lung Cancer Among People Who Never Smoked. www.cdc.gov/cancer/lung/nonsmokers/index.htm. Accessed May 2, 2022.
- American College of Radiology. Lung-RADS Version 1.1. www.acr.org/-/media/ACR/Files/RADS/Lung-RADS/LungRADSAssessmentCatego riesv1-1.pdf. Accessed May 2, 2022.
- Collar N, O’Neill B, Parham K, et al. Identifying best practices and gaps in early-stage lung cancer: from screening and early detection through resectable disease treatment. Journal of Oncology Navigation & Survivorship. www.jons-online.com/component/mams/?view=article&artid=4384.
- National Comprehensive Cancer Network. NCCN Clinical Practice Guidelines in Oncology (NCCN Guidelines). Non–Small Cell Lung Cancer. Version 3.2022. nscl.pdf (nccn.org). Page NSCL-J.
- National Comprehensive Cancer Network. NCCN Clinical Practice Guidelines in Oncology (NCCN Guidelines). Small Cell Lung Cancer. Version 2.2022. www.nccn.org/guidelines/guidelines-detail?category=1&id=1462.
This activity is supported by an independent educational grant from AstraZeneca LP.