It is widely accepted that patient navigation is a necessary component of any quality comprehensive cancer center.1-7 There have been, and continue to be, advances in radiology and diagnostics, improved surgical techniques, new chemotherapies and immunotherapies, applied genomic and precision medicine, and innovations in radiation therapy. Treatments are now more effective, more complex, more expensive, and more individualized. This has led to a need for significant coordination of services and care.
The oncology nurse navigator (ONN) model was developed to identify and minimize barriers to cancer screening, diagnosis, and treatment, and to coordinate care and follow-up throughout the cancer care continuum.8-10 While many cancer accreditation programs, hospitals, clinics, and patients recognize the benefits of patient navigation, measuring the value added by ONNs has been challenging. After reviewing nationwide studies of the American healthcare system and its general fragmentation, the American College of Surgeons Commission on Cancer upgraded its accreditation standards starting in 2012 to require a focus on patient-centered care.3,11,12 By 2015, a patient navigation program became a requirement for accreditation. In addition, Standard 2.2 of the National Accreditation Program for Breast Centers requires that “A patient navigation process is in place to guide the patient with a breast abnormality through provided and referred services.”4 In the ongoing effort to deliver value-based care, organizations are striving to identify a set of metrics that can capture the impact of patient navigation on patient outcomes and quality of care.13-16
Escalating costs, advancing technology, informed consumerism, scientific developments, an aging population, and a higher demand for quality care and patient satisfaction are all external dynamics challenging today’s healthcare delivery system.5,17 A strategy for balancing these forces is essential as customer expectations continually expand despite the demand for controlling or cutting costs as a major value-added feature of service.
In 2017, an interdisciplinary team at the DeCesaris Cancer Institute (DCI) at Anne Arundel Medical Center (AAMC), Annapolis, MD, convened to participate in a week-long kaizen or Rapid Improvement Event (RIE). Kaizen, a process improvement method usually occurring over the course of 2 to 5 days, is the focused analysis of the small, manageable elements of a problem with rapid implementation of a solution by a team of stakeholders with ongoing, real-time reassessment.18,19 This method attempts to eliminate nonvalue-added actions or activities within a specific process, thereby creating a more efficient and effective cost-containment process (high quality-low cost). Managers, physicians, providers, information systems analysts, nurses, and support personnel from the DCI participated in the event alongside the ONNs.
Value-added activities, as defined in a nursing time study, are patient-centered actions that directly benefit the patient, meeting or exceeding patient expectations.17 There is a distinction made between value-added (direct patient benefit), essential tasks required to deliver patient care (necessary but do not directly benefit the patient), and nonvalue-added activities (do not benefit the patient and are unnecessary). For example, value-added tasks include patient assessment, teaching, and communications; essential tasks consist of documentation, data entry, and coordination of ancillary services; nonvalued-added tasks involve time on call-waiting, delay in receiving return calls or paperwork, locating equipment, and lunch breaks.17
ONN functions may be categorized into 2 domains: instrumental/logistical, which suggests technical competence (essential tasks), and interpersonal/educational, which reflects the patient-navigator relationship and ONN expertise (value-added).20,21 If this indeed is the overall function of ONNs, then the majority of their duties and responsibilities is incorporated into the value-added and essential tasks categories.
The Hospital Consumer Assessment of Healthcare Providers and Systems survey measures data associated with the patient’s perception of their healthcare experience.22 Medicare reimbursement, at least in part now, is tied to this patient satisfaction. Care coordination, reinforcement of adherence to the treatment plan, and patient engagement, 3 major activities of the ONN, are found to be associated with patient satisfaction and outcomes.9,23,24 Consequently, a focus on providing ONN services that enhance these activities may prove beneficial to not only the patient experience, but also to clinical outcomes and the organization’s bottom line.
In today’s multifaceted oncology care environment, even with shared electronic medical records (EMRs), it is difficult for specialists to communicate, and the human dimension is lost when care is not adequately personalized; the attempts at efficiency perhaps serve system rather than patient. Patient navigation is a key strategy to overcome these issues and enhance the quality of cancer care delivery resulting in efficient care coordination and improved outcomes for patients.5-7,25-29
Registered nurses in the navigator role are best suited for this task and are able to apply the nursing process (assessment, diagnosis, planning, implementation, evaluation) to the individual patient’s evolving needs, clinical situation, and response to therapies.8,30 The skill set of ONNs allows them to meet the patient at any point in their treatment timeline and address barriers that may impede timeliness to care and/or result in less than optimal clinical outcomes and patient experiences.30,31
A critical component to understanding the ONN role is the concept of bidimensional accountability; the ONN works on behalf of the patient within a healthcare system.30,31 In reconciling these 2 domains, the unique role of the ONN influences positive patient outcomes (patient satisfaction, timeliness of care, decreased patient anxiety, decreased lengths of stay, and reduced treatment delays)16,32,33 and promotes positive system outcomes (interdisciplinary communication, patient retention, and downstream revenues).30-32,34
The potential benefits of a well-designed patient navigation system have been well described (Table 1).8,11,16,35-37 Despite these conjectured benefits, there continues to be a paucity of data on ONN effectiveness or even agreement on the best metrics. In an attempt to standardize ONN metrics, the Academy of Oncology Nurse & Patient Navigators (AONN+) embarked on an initiative to identify evidence-based oncology navigation metrics.38 AONN+ subsequently developed 35 metrics to measure the influence of navigation on the 3 key areas: patient experience, clinical outcomes, and return on investment.26 Currently, utilization of these metrics or establishment of benchmarks for patient navigation is very limited.
While many hospitals and clinics recognize the benefits of patient navigation, the role and functions of the ONN are inconsistent.39 In 2013-2017, the Oncology Nursing Society (ONS) identified a framework for the ONN role and reorganized the Oncology Nurse Navigator Core Competencies for Practice to include coordination of care, communication, patient education, and professional roles. The ONS added and defined the role of the Expert ONN as a “professional registered nurse with oncology-specific clinical knowledge and critical thinking and decision-making skills who offers individualized assistance to patients, families, and caregivers to help overcome healthcare system barriers.”30
Objectives
In 2016, ONNs at the DCI at AAMC recognized the need to better clarify the impact of their role on the patient experience, patient outcomes, and return on investment.
The objectives for this initiative were to:
- Define the mission of the AAMC Oncology Navigation Program and the ONN role
- Establish annual ONN core competencies evaluation through case study presentations30,40
- Standardize the ONN referral process
- Develop and standardize navigators’ documentation
- Quantify ONNs’ work in removing barriers to care, identifying patient acuity, and tracking patient volumes and ONN interventions
- Monitor ONN metrics electronically
Methods and Results
Mission Statement and Role Definition
The RIE team defined the program’s mission and ONNs’ role within the organization. The goal was to differentiate the ONN role from other case managers, nononcology nurse navigators, treating nurses, and lay navigators in our health system and the community. The team developed the following:
- AAMC ONN Program Mission Statement:
The Oncology Nurse Navigator Program is established to provide individualized, comprehensive, and compassionate patient and family-focused care, and to eliminate barriers to quality healthcare through evidence-based interventions. - Definition of ONN Role:
“The AAMC Oncology Nurse Navigator is a professional registered nurse with oncology-specific knowledge who offers education and resources along with individualized assistance to patients, families, and caregivers to overcome healthcare system barriers, thereby facilitating timely access to comprehensive quality care from diagnosis through all phases of the cancer experience.”
ONN Role and Core Competencies
The nursing process is vital to the success of navigation in light of increasingly complex oncology care plans.30 The ONN applies the nursing process while taking into account patient preferences, cultural/ethnic backgrounds, health literacy, and work/life priorities. Nursing evaluation occurs throughout the patient-navigator relationship, and evaluation by a certified ONN has been found to result in better outcomes and patient compliance.16,25
Prior to the completion of the analysis incorporated in the RIE effort, the ONNs were frequently performing non-navigation (clerical) duties along with navigation functions as they were known to “get things done.” Indeed, a medical oncologist on the RIE team stated, “The nurse navigators do the job so well, they have become victims of their own success.” The RIE team engaged in observational time studies resulting in reallocation of clerical duties. These duties included obtaining authorization for diagnostic scans, assisting patients with tertiary referral appointments, and gathering external medical records. The result was that the ONNs could now serve more patients and focus on the functions identified in the nationally recognized ONS Core Competencies.30
Using the ONS Core Competencies for Practice, each ONN now presents a case study annually to demonstrate incorporation of these core competencies into their professional practice. Peers, providers, administrators, and interested hospital staff attend the presentations for discussion, evaluation, and feedback.
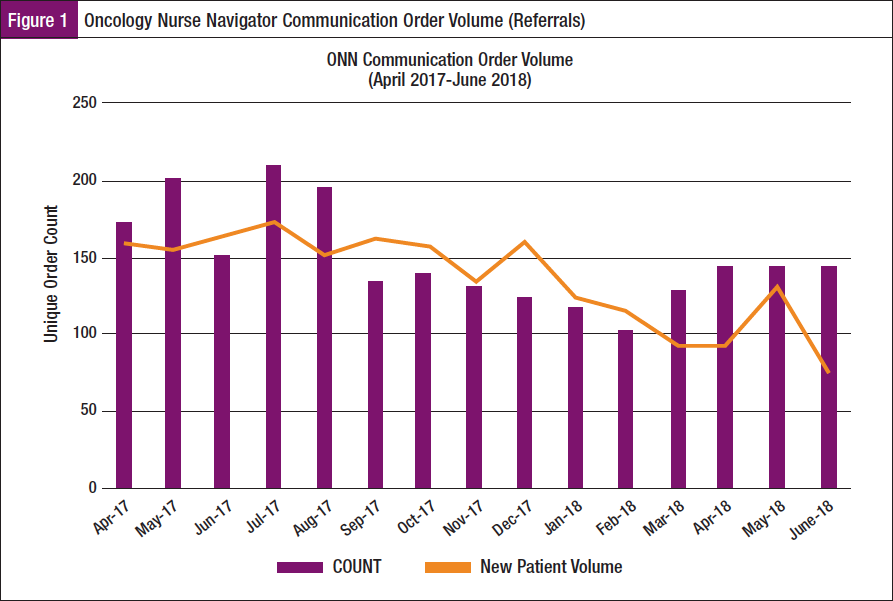
An ONN referral process in the EMR was created to simplify the process for requesting ONN support for patients. The referral process identifies new patients and patients whose acuity increases, requiring reassessment along the care continuum. This is an improvement from the previous haphazard process of e-mail, telephone, or verbal hallway referrals. The ONN Communication Order populates an EMR work queue that ONNs check daily. The ONNs then perform chart reviews and contact and/or meet the patient to assess needs and barriers to care and initiate the patient-navigator relationship. This referral process better captures patients who may have been missed previously or whose acuity level has increased. Metrics for referral volume are now reportable (Figure 1). Overall, the ONN referrals follow the trend line of new patient volume. Months in which referral count exceeds new patient volume indicates not only new patient referrals but also established patients who may now require new or additional ONN support.
ONN Value-Added (Barriers, Acuity, Interventions)
Our metrics (percentage of barriers addressed, acuity level, and interventions) measure the ONNs’ functions and influence on timeliness to care (mitigating barriers to care) and the coordination of anticipatory care to avert increasing acuity levels (improved patient outcomes).
To capture these data, the team created a standardized ONN note within the EMR in which to document nursing process, barriers identified and addressed, patient acuity rating, and interventions (“touches”). This template now includes discrete fields with drop-down menus that make documentation more efficient and consistent and also allow for extraction of data for reporting purposes. The standardized EMR note is used for newly referred oncology patients at the initiation of the patient-navigator relationship. A follow-up template note exists for ongoing coordination of care along the care continuum.
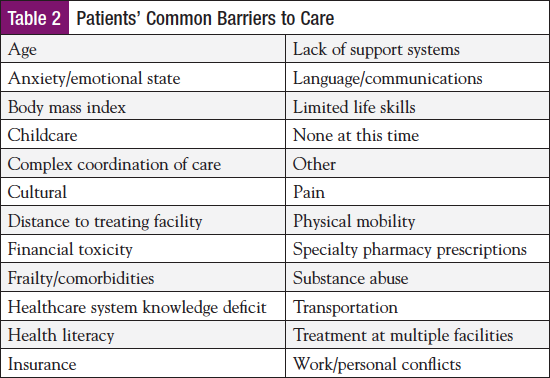
Identifying and addressing patients’ barriers to care and implementing actions to minimize obstacles that stand between the patient and the required treatment is one of the most important roles of the ONN.41 There are several barriers that are commonly observed among patients, although there are differences for each patient within the barrier categories. For example, the transportation barrier for one patient may be securing a ride to an appointment. For another, it is assistance with paying car insurance so that he/she may drive to a medical visit. The team compiled a list of common barriers within the ONN note (Table 2). During the period from April 2017 through August 2018, the top 3 barriers identified included complex coordination of care (27.1%), anxiety/emotional state (21.4%), and health literacy (13%).
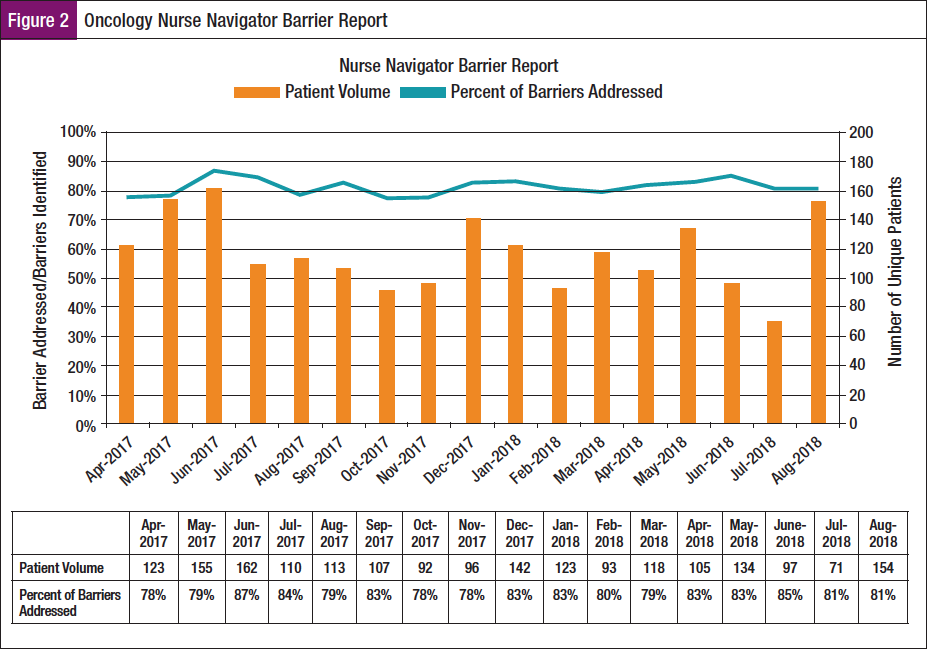
If barriers faced by an individual negatively influence the time it takes to get to treatment, it is surmised that addressing these barriers expedites the process.29 By having barriers identified and addressed in discrete fields, the percentage of barriers addressed can be calculated and used as a metric for value-added by the ONN (Figure 2). Since collecting these data, ONNs have remarkably maintained a barrier mitigation rate of 81%. This value will not achieve 100%, because some barriers cannot be removed (eg, age).
Patient acuity is widely recognized as a factor when considering nursing caseload.42 To delineate caseload further, the ONN team identifies a patient acuity rating at the initiation of the patient-navigator relationship. The RIE team developed an acuity tool based on the number of patient barriers the ONN identifies during the nursing assessment (Table 3).
Within the note, the ONN assigns a patient’s acuity level (Figure 3). For the indicated period, overall data reveal that 61% of the new patient volume had an acuity level of 3 to 4, indicating higher navigation needs; 22% had an acuity level of 2, and 17%, once assessed, had no significant navigation needs. Although a patient is determined to have an acuity rating of level 1 (no navigation needs), the ONN must first perform an assessment of the patient to determine this, hence, work performed (value-added productivity). When the monthly percentage of patients’ acuity assessed exceeds 100%, the ONNs have not only assessed new patients but have reassessed patients already on the cancer care continuum—perhaps referred as having developed additional barriers to care, declining performance status, or other issues that may hinder optimal patient outcomes.
Electronic reporting of ONN interventions (or “patient touches”) was developed as a means to document value-added (direct benefit to patient) and essential tasks (necessary to deliver care) performed by the ONNs. The terms “patient touch,” “intervention,” and “work unit” are used interchangeably and represent 1 ONN note in the EMR.
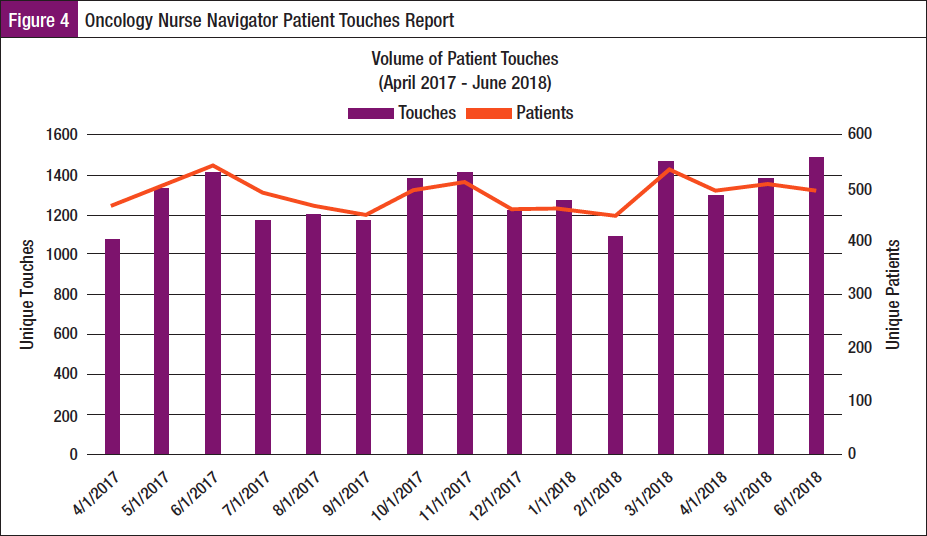
Patient touches include face-to-face encounters, telephone calls, result and progress notes, patient and family teaching, electronic patient portal communications, orders, imaging and pathology results discussions, referrals, etc (Figure 4). Between April 2017 and June 2018, there were 19,345 ONN work units for 3903 unique patients (average of 5 touches per patient). Hence, each of the 6 navigators averaged 651 patients with 3255 interventions per navigator during this period. This number perhaps underreports, because documenting a note often encompasses multiple interventions within 1 note. Consider that not every patient required ongoing navigation depending on acuity level, while higher acuity patients required more intense navigation services.
Discussion
Achieving widespread utilization of the EMR ONN referral process within the organization has been challenging. The premise behind the ONN referral is to engage staff to identify patients needing navigator support. If the ONN is unaware of the patient, critical assessment and referrals to supportive resources remain untapped. When this occurs, there are risks of unmet patient needs, improper sequencing of diagnostic scheduling and inappropriate testing resulting in treatment delay, increased distress, added costs, and potentially poorer outcomes.
Documentation of changing acuity levels as patients proceed through the oncology continuum poses some difficulty. The acuity of each patient is subject to change throughout the cancer experience. The ONN needs the ability to demonstrate the acuity of the patient caseload at any given time. There is also the consideration that, perhaps, each type of barrier should be weighted in determining an acuity level.
Timeliness to treatment is often used as a metric for effective patient navigation, although appropriate time to treatment for different cancers varies. For example, a patient with imaging that is suspicious for lymphoma may require a biopsy and treatment within days, whereas a patient with a finding suspicious for ovarian cancer will require time for workup and surgical planning, with diagnosis and treatment beginning simultaneously with surgery. Other delays may be due to patient factors such as a desire for second opinions or genetic testing. The expertise of the ONN is essential for the clinical decision-making required to tailor the navigation plan based on each patient’s type of cancer.
Conclusion
Identifying metrics that directly measure value-added by ONNs has been an ongoing challenge for this specialty. Improvements in the processes of ONN referrals, delegation of nonclinical tasks, use of documentation templates, and evaluation of integrating core competencies into practice allow for more efficient and effective ONN utilization. Incorporating patients’ acuity level rather than just patient volume not only aids in evaluating navigators’ caseloads but also lends itself to focus resources on high-risk patients. Identifying barrier mitigation rates and ONN interventions are metrics for analyzing the impact of ONN interpersonal skills/expertise (value-added) and technical competence (essential tasks) on the patient experience. Further, it is surmised that mitigating barriers to care reduces time to treatment, improves compliance to treatment plan, and ultimately affects clinical outcomes. Converting downstream referrals to revenue dollars may be a promising metric for ONNs’ impact on business performance. Lack of comparable benchmarking to other navigation programs also limits the interpretation of these metrics.
Standardization of care has proven benefits; however, patients want a personal touch, not assembly-line care. Each individual is different, will have different reactions to the diagnosis, different responses to treatment, and certainly different needs along the continuum of care. Unlike other types of patient navigation, the cancer continuum of care is a nonlinear journey. The ONN guides patients through their cancer experience and assists them along the detours that occur with, through, and beyond cancer.
This initiative was an initial step in developing metrics and analyzing ONNs’ role in value-based care. It is recognized that ongoing research, refinement, and benchmarking of metrics for patient navigation must continue to demonstrate the direct value-added by oncology nurse navigation to the patient experience, volume of emergency department visits, readmission rates, end-of-life care, clinical outcomes, and business performance.
References
- Freund KM, Battaglia TA, Calhoun E, et al. National Cancer Institute Patient Navigation: Research Program: methods, protocol, and measures. Cancer. 2008;113:3391-3399.
- Paskett ED, Harrop JP, Wells KJ. Patient navigation: an update on the state of the science. CA Cancer J Clin. 2011;61:237-249.
- American College of Surgeons. Commission on Cancer. Cancer Program Standards 2016 Edition. www.facs.org/quality-programs/cancer/coc/2016-standards. Accessed May 31, 2018.
- American College of Surgeons. National Accreditation Program for Breast Centers. Standards Manual 2018 Edition. https://accreditation.facs.org/accreditationdocuments/NAPBC/Portal%20Resources/2018NAPBCStandardsManual.pdf. Accessed May 31, 2018.
- Winckworth-Prejsnar K, McCanney J, Schatz AA, et al. Policy challenges and opportunities to address changing paradigms in cancer care delivery. J Natl Compr Canc Netw. 2019;17:424-431.
- Alison LM. Oncology nurse navigators: putting the “value” in value-based payment models. Am J Manag Care. 2018;24(5 Spec No.):SP128-SP129.
- Gonzalo JD, Haidet P, Papp KK, et al. Educating for the 21st-century health care system: an interdependent framework of basic, clinical, and systems sciences. Acad Med. 2017;92:35-39.
- Oncology Nursing Society. Oncology nurse navigation role and qualifications. Oncol Nurs Forum. 2015;42:447-448.
- Riley S, Riley C. The role of patient navigation in improving the value of oncology care. Journal of Clinical Pathways. 2016;2:41-47.
- Freeman HP, Rodriguez RL. The history and principles of patient navigation. Cancer. 2011;117(15 Suppl):3539-3542.
- Wilcox B, Bruce SD. Patient navigation: a “win-win” for all involved. Oncol Nurs Forum. 2010;37:21-25.
- Horner K, Ludman EJ, McCorkle R, et al. An oncology nurse navigator program designed to eliminate gaps in early cancer care. Clin J Oncol Nurs. 2013;17:43-48.
- Esparza A, Calhoun E. Measuring the impact and potential of patient navigation. Cancer. 2011;117(15 Suppl):3537-3538.
- Freund KM, Battaglia TA, Calhoun E, et al. Impact of patient navigation on timely cancer care: the Patient Navigation Research Program. J Natl Cancer Inst. 2014;106:dju115.
- Guadagnolo BA, Dohan D, Raich P. Metrics for evaluating patient navigation during cancer diagnosis and treatment. Cancer. 2011;117(15 Suppl):3563-3572.
- Lee T, Ko I, Lee I, et al. Effects of nurse navigation on health outcomes of cancer patients. Cancer Nurs. 2011;34:376-384.
- Upenieks VV, Akhavan J, Kotlerman J. Value-added care: a paradigm shift in patient care delivery. Nurs Econ. 2008;26:294-300; quiz 301.
- Branco D, Wicks AM, Visich JK. Using quality tools and methodologies to improve a hospital’s quality position. Hosp Top. 2017;95:10-17.
- Knechtges P, Decker MC. Application of kaizen methodology to foster departmental engagement in quality improvement. J Am Coll Radiol. 2014;11(12 Pt A):1126-1130.
- Carle AC, Jean-Pierre P, Winters P, et al. Psychometric evaluation of the patient satisfaction with logistical aspects of navigation (PSN-L) scale using item response theory. Med Care. 2014;52:354-361.
- Jean-Pierre P, Fiscella K, Winters PC, et al. Psychometric development and reliability analysis of a patient satisfaction with interpersonal relationship with navigator measure: a multi-site patient navigation research program study. Psychooncology. 2012;21:986-992.
- Hospital Consumer Assessment of Healthcare Providers and Systems. CAHPS Hospital Survey. www.hcahpsonline.org. Accessed June 3, 2019.
- Manary MP, Boulding W, Staelin R, Glickman SW. The patient experience and health outcomes. N Engl J Med. 2013;368:201-203.
- Campbell C, Craig J, Eggert J, Bailey-Dorton C. Implementing and measuring the impact of patient navigation at a comprehensive community cancer center. Oncol Nurs Forum. 2010;37:61-68.
- Crane-Okada R. Evaluation and outcome measures in patient navigation. Semin Oncol Nurs. 2013;29:128-140.
- Strusowski T, Sein E, Johnston D, et al. Standardized evidence-based oncology navigation metrics for all models. Journal of Oncology Navigation & Survivorship. 2017;8(5):220-237.
- Chen LM, Ayanian JZ. Care continuity and care continuation: what counts? JAMA Intern Med. 2014;174:749-759.
- Institute of Medicine. Levit LA, Balogh EP, Nass SJ, Ganz PA, eds. Delivering High-Quality Cancer Care: Charting a New Course for a System in Crisis. Washington, DC: National Academies Press; 2013.
- Walsh J, Young JM, Harrison JD, et al. What is important in cancer care coordination? A qualitative investigation. Eur J Cancer Care (Engl). 2011;20:220-227.
- Oncology Nursing Society. 2017 Oncology Nurse Navigator Core Competencies. www.ons.org/sites/default/files/2017-05/2017_Oncology_Nurse_Navigator_Competencies.pdf.
- Oncology Nursing Society. Oncology Nurse Navigator Core Competencies. 2013. www.ons.org/sites/default/files/ONNCompetencies_rev.pdf.
- Desimini EM, Kennedy JA, Helsley MF, et al. Making the case for nurse navigators: benefits, outcomes, and return on investment. Oncology Issues. 2011;26(5):26-33.
- Korber S, Padula C, Gray J, Powell M. A breast navigator program: barriers, enhancers, and nursing interventions. Oncol Nurs Forum. 2011;38:44-50.
- Fillion L, Cook S, Veillette A, et al. Professional navigation framework: elaboration and validation in a Canadian context [online exclusive]. Oncol Nurs Forum. 2012;39:E58-E69.
- Gilbert JE, Green E, Lankshear S, et al. Nurses as patient navigators in cancer diagnosis: review, consultation and model design. Eur J Cancer Care (Engl). 2011;20:228-236.
- What You Need to Know About the 2015 Standards. Journal of Oncology Navigation & Survivorship. www.jons-online.com/issues/2014/October-2014-vol-5-no-5. 2014. Accessed October 21, 2018.
- Battaglia TA, Burhansstipanov L, Murrell SS, et al. Assessing the impact of patient navigation: prevention and early detection metrics. Cancer. 2011;117(15 Suppl):3553-3564.
- Academy of Oncology Nurse & Patient Navigators. Standardized Metrics Source Document. https://aonnonline.org/images/articles/standardized_metrics/Metrics-Source-Document.pdf. Accessed April 11, 2019.
- Brown CG, Cantril C, McMullen L, et al. Oncology nurse navigator role delineation study: an Oncology Nursing Society report. Clin J Oncol Nurs. 2012;16:581-585.
- American College of Surgeons. Commission on Cancer. Cancer Program Standards (2016 Edition). Ensuring Patient-Centered Care. Version 1.2. www.facs.org/quality-programs/cancer/coc/2016-standards. Accessed May 31, 2019.
- Oncology Nursing Society. Role of the oncology nurse navigator throughout the cancer trajectory. Oncol Nurs Forum. 2018;45:283.
- Baldwin D, Jones, M. Developing an acuity tool to optimize nurse navigation caseloads. Oncology Issues. 2018;33(2):17-25.